Research Article, Int J Ment Health Psychiatry Vol: 5 Issue: 1
Prescription Pattern of Second Generation Antipsychotics and Outcomes of Patients with Schizophrenia in an Indian Hospital
Mathew VK1*, Sam KG2, Samuel B3 and Das AK4
1Department of Pharmacy Practice, Krupanidhi College of Pharmacy, Bangalore, India
2Department of Pharmacy Practice, College of Pharmacy, Gulf Medical University, Ajman, UAE
3Department of Pharmacy Practice, RR College of Pharmacy, Bangalore, India
4Krupanidhi College of Pharmacy, Bangalore, India
*Corresponding Author : Mathew VK
Assistant Professor, Department of Pharmacy Practice, Krupanidhi College of Pharmacy, 12/1, Chikka Bellandur, Carmelaram Post, Varthur Hobli, off Sarjapur Road, Bangalore-560035, India
Tel: 09901614102
E-mail: mathewvino@gmail.com
Received: June 19, 2019 Accepted: July 24, 2019 Published: July 30, 2019
Citation: Mathew VK, Sam KG, Samuel B, Das AK (2019) Prescription Pattern of Second Generation Antipsychotics and Outcomes of Patients with Schizophrenia in an Indian Hospital. Int J Ment Health Psychiatry 5:1.
Abstract
An observational study was carried out to assess the clinical characteristics of patients with schizophrenia and the treatment pattern of the disease in a tertiary care hospital of south India. A retrospective evaluation of the prescription pattern of second generation antipsychotics and the clinical outcome of patients diagnosed with Schizophrenia in a tertiary care Indian hospital. The influence of patient demographics like age, sex, family history, type of schizophrenia and treatment on the outcome of patient at the time of discharge and length of hospital stay were also evaluated. Among a total of 139 schizophrenic patients, majority were males 81 (58.27%) and the average age was 34.4 ± 11.9 y. A predominance of male patients below 40 years and females above 40 y were observed. Paranoid schizophrenia was the major subclass (63.3%). Paranoid schizophrenia was the most prevalent subclass. Second generation antipsychotics were the major class (93.5%) used, among which tablet olanzapine was prescribed maximum (54.7%). Inj. haloperidol was the major (15.8%) first generation antipsychotic used. Anxiolytics (57.5%) and anticholinergics (56.8%) were the major adjuvant drugs used. The average hospitalization period was 12.4 ± 8.4 days and majority (92.1%) improved at discharge. An overall male predominance of schizophrenia among male population, especially more in age group below 40 y and the female domination above 40 y of age was observed. Second generation antipsychotics were the major class of treatment provided among which olanzapine received maximum prescriptions. Haloperidol was the major drug used among first generation antipsychotics. For the management of schizoaffective disorders, mood stabilizers like lithium, anxiolytics like lorazepam, antidepressants like fluoxetine and sertraline were commonly prescribed. Anticholinergic like benzhexol was prescribed for controlling the extrapyramidal side effects of antipsychotics. The increasing trend of prescribing second generation antipsychotics reflect the efficacy and safety profile as compared to first generation antipsychotics. The present study revealed an increasing trend of Paranoid schizophrenia and the use of second generation antipsychotics improved outcomes like hospitalization period and clinical status at discharge.
Keywords: Schizophrenia; Second Generation Antipsychotics; Prescription Pattern; Clinical outcome
Introduction
Schizophrenia is a chronic and debilitating psychiatric illness, characterized by diminished cognitive functions, emotional disabilities, disturbed relationship and altered decisions making [1]. It represents a heterogeneous syndrome of disorganized and bizarre thoughts, delusions, hallucinations, inappropriate affect and impaired psychosocial functioning [2].
Prevalence studies of schizophrenia in India report rates of between 1.5 per 1000 and 2.5 per 1000. There appears to be no consistent difference between rural and urban areas in the frequency of the illness, and no clear pockets of high or low prevalence. Incidence studies are few, with estimates of an annual incidence of 0.35-0.38 per 1000 in urban populations and 0.44 per 1000 in the rural population [3-5].
Several guidelines exist for rational prescription for schizophrenia, including an Indian guideline. Nevertheless, prescribing in real-world settings often differs from suggested guidelines. High-dose antipsychotic use is not supported by evidence of clinical efficacy and is linked to adverse effects, including risk of sudden death. Anticholinergic agents alleviate neuroleptic-induced extrapyramidal side-effects, but have adverse cognitive effects, alter absorption of other oral medications and have abuse potential. Short-term, as-required use prevents extrapyramidal side-effects in the vast majority of patients, but routine use is nonetheless commonplace.
The rising trend toward polypharmacy in schizophrenia care, which is not supported by current guideline recommendations, warrants critical appraisal [6]. Polypharmacy may also increase the risk of adverse effects, drug interactions, noncompliance, and medication errors. Polypharmacy, is strongly discouraged in treatment guidelines, but typically found in 25% of out-patient attendees [7]. In recent years, the arrival of atypical antipsychotics for treating patients with schizophrenia has received considerable attention. Given the severe side effects associated with many of the older antipsychotics, the introduction of atypicals, which appear to produce far fewer extrapyramidal side effects and show properties associated with reduced negative symptoms, has been greeted enthusiastically by psychiatrists and consumers [8].
Haloperidol was the most frequently prescribed antipsychotic agent in the 1980s and early 1990s. Clozapine was just beginning to be used for treatment-resistant patients during this period. In the mid-1990s, newer atypical antipsychotics such as risperidone (1993) and olanzapine (1996) were introduced for the treatment of schizophrenia [9]. A study by Wang et al. in the year 2000 suggested that atypicals made up more than 50 percent of the antipsychotic medication market based up on a recent review of clinical trial evidence, participants in a National Institute of Mental Health workgroup concluded that atypicals were more effective than traditional antipsychotics and should be considered as the first line of treatment for patients with schizophrenia and the share of expenditures for drugs for mental health is increasing [10]. It is therefore essential that psychotropic medication patterns of schizophrenia patients in public sector programs be monitored to ensure equity and appropriateness of treatment [11]. It is essential to monitor the psychotropic medication patterns of schizophrenia patients to ensure equity and appropriateness of treatment. Thus there is a need to study the distribution pattern of schizophrenia and surveillance of treatment pattern in order to gain an insight into current prescribing practice.
Methodology
The study was a prospective medical record review conducted at the Department of Psychiatry at Kasturba Hospital, Manipal, a 1472 bed hospital. Following a standard protocol all the 139 schizophrenic Patients admitted in Psychiatry ward during the period from August 2006 to May 2007 with a diagnosis of schizophrenia were included in the study. A written informed consent in local language (Kannada and Malayalam) and English was obtained from the patient or care providers. The Cases of schizophrenia were identified and data on treatment pattern were collected from medical records to study the pharmacotherapeutic drug treatment pattern. Demography of the patients like age, sex, family history, ICD–10 sub class, outcome as clinical status of patient at the time of discharge and length of hospital stay were also studied. This study systemically explored the trends in schizophrenia and the pharmacological treatment in a tertiary care hospital. This is a naturalistic observational study, which provides drug utilization data in the context of real-world clinical practice. Such data are likely to represent the evidences of effectiveness during day-to-day practice than randomized trials.
Results
Demographic profile
A total of 139 schizophrenic patients were enrolled in the study. As shown in Table 1 most of the patients were males 81(58.27%) patients and 58 (41.73%) patients were females. The male to female ratio was found to be 1.46: 1. The average age among the patients was 34.44 ± 11.94 years. Age distribution showed that higher numbers of patients belonged to the age group 21-30 y 60 patients (43.17%) In the present study it was observed that majority of the males belonged to the lower age group of less than 40 y while females dominated in higher age group of more than 40 y. Out of 139 patients 82 (58.99%) patients were unmarried and 57 (41.01%) patients were married.
| Age Group (in years) | Number of patients | Percentage (%) |
|---|---|---|
| <20 | 18 | 12.95% |
| 21-30 | 60 | 43.17% |
| 31-40 | 30 | 21.58% |
| 41-50 | 16 | 11.51% |
| 51-60 | 12 | 8.63% |
| 61-70 | 2 | 1.44% |
| >70 | 1 | 0.72% |
| Gender wise distribution | ||
| Males | 81 | 58.27% |
| Females | 58 | 41.73% |
| Marital Status | ||
| Married | 57 | 41.01% |
| Single | 82 | 58.99% |
Table 1: Sociodemographic profile of study sample (n=139).
Family history of psychiatric disorder
As shown in Table 2 out of 139 patients family history was available for 49 patients only. Out of 49 patients 42 patients (85.71%) were having family history of psychiatric disorder. In this 33 patients (67.35%) were having family history of 1 degree relative and 9 patients (18.37%) were having family history of 2 degree relative.
| Family history | Percentage (%) | |
|---|---|---|
| Family History Available | 49 | |
| No family history | 7 | 14.29% |
| Family history Present | 42 | 85.71% |
| 1 degree relative | 33 | 67.35% |
| 2 degree relative | 9 | 18.37% |
Table 2: Family history of psychiatric disorder.
Diagnostic distribution (ICD – 10)
As shown in Table 3, the ICD-10 sub class wise classification of schizophrenia has shown that paranoid schizophrenia (F20.0) was the most prominent diagnosis 88 (63.3%) patients and the least patients diagnosed was in the sub type post schizophrenic depression (F20.4) and other schizophrenia (F20.8) only one patient. There were no patients for diagnosis Simple Schizophrenia (F20.6).
| ICD Code | ICD-10 Sub class | Total no of patients | Percentage (%) |
|---|---|---|---|
| F20.0 | Paranoid Schizophrenia | 88 | 63.30% |
| F20.1 | Hebephrenic Schizophrenia | 2 | 1.44% |
| F20.2 | Catatonic Schizophrenia | 9 | 6.47% |
| F20.3 | Undifferentiated Schizophrenia | 30 | 21.58% |
| F20.5 | Residual Schizophrenia | 4 | 2.88% |
| F20.8 | Other Schizophrenia | 1 | 0.72% |
| F20.9 | Unspecified Schizophrenia | 4 | 2.88% |
| F20.4 | Post Schizophrenic Depression | 1 | 0.72% |
| F20.6 | Simple Schizophrenia | 0 | 0.00% |
| N=139 | |||
Table 3: Diagnostic Distribution (ICD 10).
The average length of hospital stay for all the 139 patients was 12.37 ± 8.4 days with a minimum period of one day to a maximum of 46 days. Distribution of patients according to the Outcome at discharge shown that majority of the patients were ‘Improved’, 128 (92.09%) patients. 10 (7.19%) patients were unchanged during the time of discharge and one patient recovered at the time of discharge.
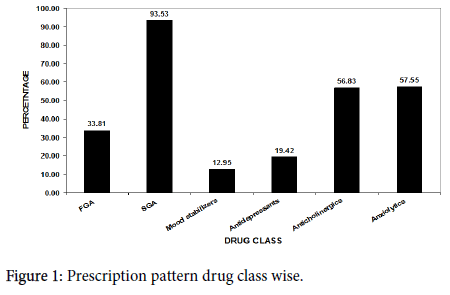
Prescription pattern drug class wise
As is evident from Figure 1 second generation antipsychotics receives maximum prescriptions 130 (93.53%) patients. Anticholinergics and anxiolytics were the drug class which was prescribed next after second generation antipsychotics 79 (56.83%) patients and 80 (57.55%) patients respectively. First generation antipsychotics were prescribed for 47 (33.81%) patients. Antidepressants were prescribed for 27 (19.42%) patients. Mood stabilizers received the least prescription 18 (12.95%) patients.
Prescription pattern for second generation antipsychotics
Second generation antipsychotics were the drug class which was prescribed maximum. As shown in Table 4 among the second generation antipsychotics olanzapine was prescribed maximum 76 (54.68%) patients after which tab risperidone was prescribed mostly in 60 (43.17%) patients. Tab sertindole was prescribed minimum in 2 (1.44%) patients. Clozapine was prescribed for 16.55% of patients.
| S. No. | Drug | No. of prescriptions | Percentage% |
|---|---|---|---|
| 1 | T. Olanzapine | 76 | 54.68% |
| 2 | T. Risperidone | 60 | 43.17% |
| 3 | T. Clozapine | 23 | 16.55% |
| 4 | T. Aripiprazole | 10 | 7.19% |
| 5 | Inj. Olanzapine | 6 | 4.32% |
| 6 | T. Quetiapine | 4 | 2.88% |
| 7 | T. Ziprasidone | 6 | 4.32% |
| 8 | T. Sertindole | 2 | 1.44% |
Table 4: Prescription pattern for second generation antipsychotics.
Prescription pattern for first generation antipsychotics
First generation antipsychotics were prescribed next to second generation antipsychotics. As shown in Table 5 tab haloperidol was prescribed maximum 22 (15.83%) patients after that inj haloperidol was prescribed mostly 22 (7.19%) patients. Tab pimozide was prescribed minimum only one patient.
| S. No. | Drug | No of prescriptions | Percentage% |
|---|---|---|---|
| 1 | Inj. Haloperidol | 22 | 15.83% |
| 2 | T. Haloperidol | 10 | 7.19% |
| 3 | Inj. Zuclopenthixol | 16 | 11.51% |
| 4 | T. Chlorpromazine | 7 | 5.04% |
| 5 | Inj. Fluphenazine | 6 | 4.32% |
| 6 | T. Trifluoperazine | 3 | 2.16% |
| 7 | T. Pimozide | 1 | 0.72% |
Table 5: Prescription pattern for first generation antipsychotics.
Prescription pattern for mood stabilizers
As shown in Table 6 among mood stabilizers lithium was prescribed maximum, for 6 (4.32%) patients and topiramate was prescribed minimum (1.44%).
| S. No. | Drug | No of prescriptions | Percentage% |
|---|---|---|---|
| 1 | T. Lithium | 6 | 4.32% |
| 2 | T. Carbamazepine | 4 | 2.88% |
| 3 | T. Phenytoin | 5 | 3.60% |
| 4 | T. Sod valproate | 3 | 2.16% |
| 5 | T. Topiramate | 2 | 1.44% |
Table 6: Prescription pattern for mood stabilizers.
Prescription pattern for antidepressants
As shown in Table 7 among antidepressants tab fluoxetine and tab setraline was prescribed maximum both 7 (5.04%) patients. tab velnlafaxine, tab dosulepin, tab mirtazapine, tab bupropion and tab seligilin was prescribed minimum 1 (0.72%).
| S. No. | Drug | No of prescriptions | Percentage% |
|---|---|---|---|
| 1 | T. Fluoxetine | 7 | 5.04% |
| 2 | T. Sertraline | 7 | 5.04% |
| 3 | T. Venlafaxine | 1 | 0.72% |
| 4 | T. Amitriptyline | 4 | 2.88% |
| 5 | T. Dosulepin | 1 | 0.72% |
| 6 | T. Citalopram | 2 | 1.44% |
| 7 | T. Escitalopram | 5 | 3.60% |
| 8 | T. Mirtazapine | 1 | 0.72% |
| 9 | T. Bupropion | 1 | 0.72% |
| 10 | T. Seligilin | 1 | 0.72% |
Table 7: Prescription pattern for antidepressants.
Prescription pattern for anticholinergics
As shown in Table 8 among anticholinergics tab benzhexol was prescribed maximum in 78 (56.12%) patients after that inj promethazine was prescribed mostly for 12 (8.63%) patients. tab metaclopromide and tab procyclidine was prescribed minimum one patient.
| S. No. | Drug | No of prescriptions | Percentage% |
|---|---|---|---|
| 1 | T. Benzhexol | 78 | 56.12% |
| 2 | T. Triheixphenidyl | 4 | 2.88% |
| 3 | Inj. Promethazine | 12 | 8.63% |
| 4 | T. Metoclopramide | 1 | 0.72% |
| 5 | T. Procyclidine | 1 | 0.72% |
Table 8: Prescription pattern for anticholinergics.
Prescription pattern for anxiolytics
As shown in Table 9 among anxiolytics tab lorazepam was prescribed maximum 68 (48.92%) patients. tab flurazepam and tab alprazolam was prescribed minimum only one patient.
| S. No. | Drug | No of prescriptions | Percentage% |
|---|---|---|---|
| 1 | T. Lorazepam | 68 | 48.92% |
| 2 | Inj. Lorazepam | 16 | 11.51% |
| 3 | T. Clonazepam | 13 | 9.30% |
| 4 | T. Diazepam | 2 | 1.44% |
| 5 | Inj. Diazepam | 6 | 4.32% |
| 6 | T. Zolpidem | 11 | 7.91% |
| 7 | T. Nitrazepam | 7 | 5.04% |
| 8 | T. Flurazepam | 1 | 0.72% |
| 9 | T. Alprazolam | 1 | 0.72% |
Table 9: Prescription pattern for anxiolytics.
Discussion
This study systemically explored the trends in schizophrenia and the pharmacological treatment in a tertiary care hospital. This is a naturalistic study, which provides data in the context of real-world practice. Therefore, such data are likely to be more representative of day-to-day practice than randomized trials. The gender wise distribution showed that males predominantly had schizophrenia with 59.41% males and 40.59% females. This observation is similar to a study by Dutta et al. carried out in the year 2003 in Uttaranchal, India and Andor et al. study in the year 2003 in Switzerland. The male to female ratio was found to be 1.46: 1 but a study conducted by Padmavathi et al. in Chennai showed a male: female ratio of 1.06: 1 in the year 1986 [3,12,13].
The average age among the patients was 34.44 ± 11.94 y, which is similar to other Indian studies by Chaudhary et al. in the year 2004 in Assam and Padmavathi et al. study in Che Age distribution showed that higher numbers of patients belonged to the age group 21-30 y as supported by Welham et al. in the year 1991 in Australia [3,14,15].
In the present study it was observed that majority of the males belonged to the lower age group of less than 40 y while females dominated in higher age group of more than 40 y, similar to a study by Welham et al. which revealed a female predominance in the 40-50 age group [15]. However studies in USA by WU EQ et al. revealed that majority of males belonged to 46-55 year age group and females belonged to 56-65 age group [1].
Majority of the patients 58.99% were unmarried which is similar to studies by mallinger et al. New York and Rosenheck et al. whereas study in USA by Ren et al. in the year 1999 showed a higher percentage of unmarried patients (76.3%) [16-18]. Previous reports suggest that the percentage of schizophrenic patients, who get married, is usually lower than normal individuals or those with other psychiatric disorders. The low marital rates may be attributed to the poor premorbid adjustment impairing the development of relationships, social and occupational disability arising due to the illness, besides the clinical symptoms and early age of onset [19-22]. An association between mental illness and marital problems has been documented by Indian studies too. However a study from India reported that 70% of their first episode patients were married and 80% of the marriages were intact on follow up for up to 10 y [23-25].
Family history of psychiatric disorder were reported in 85.71% of patients, in which 67.35% involved first degree relative and 18.37% involved second degree relatives. Studies by Thaker et al. showed an existence of psychiatric disorders in relatives of schizophrenic patients. Although the risk of developing schizophrenia is 0.6% to 1.9% in the general population, this increases to approximately 10% if a first degree relative has the illness and to 3% if a second degree relative has the illness [26]. If both parents have schizophrenia, the risk of producing a schizophrenic offspring increases to approximately 40%. Twin studies in dizygotic twins reported that the risk of the second twin developing schizophrenia, if one twin has the illness is between 12% and 14%. However, in monozygotic twins the risk increases to 48%. A search for genetic linkage in schizophrenia has been difficult and any genetic etiologies in schizophrenia are likely to be heterogeneous, but present with similar phenotypes. Potential loci have been identified on chromosome 6, 8, 13, and 22 [2].
Paranoid schizophrenia was the most prominent diagnosis among all sub classes. This is similar to studies by Dutta et al. in Uttaranchal India and Burns et al. in United Kingdom [12,27]. Paranoid schizophrenia was the most common subclass under the age of 70 y, after which unspecified schizophrenia predominated.
The average length of hospital stay for all the 139 patients was 12.37±8.4 days with a minimum period of one day to a maximum of 46 days. Assessment of outcome at discharge showed that majority of the patients 128 (92.09%) improved at the time of discharge. There was no statistical significant association between gender, age and subtype of schizophrenia with the hospitalization period of the patients.
The prescribing practice of antipsychotics in this tertiary care hospital was similar to the pattern of antipsychotics prescription universally indicating that most of the prescriptions were for second generation antipsychotics (SGA), either singly or in combination with other antipsychotic medications [28]. A study conducted by Essock. in USA between the period of 1998 to 1999 has shown a decrease in prescription pattern of first generation antipsychotics (FGA) from 43% in 1998 to 34% in 1999 where as the SGAs increased from 57% to 67% between 1998 to 1999 supporting observation of increased SGAs prescriptions in the present study (93.53%) [28]. Similar studies by Andor et al. in the year 2003 in Switzerland had shown a higher prescription rate of SGAs. A study by Clark et al. showed an increase in prescription of SGA from 43% in 1995 to 70% in 1999 [13,29].
The present study is in accordance with the current trend of SGA prescription which was expected.
Study conducted by Weissman et al. at Veteran’s Healthcare Administration, New York had shown prescriptions for SGAs increased from one–third of antipsychotic prescriptions for patients with schizophrenia to more than one half of the prescription in 2000 [30]. Our findings of higher prescription rates of SGAs are similar to the recommendations made by current treatment guidelines in which SGAs are the first choice in the treatment of schizophrenia. Study by Andor et al. showed that 31.4% of patients received FGAs which is also similar to the present study in which 33.81% patients were prescribed FGAs. Study conducted by Weissman et al. show a rapid decrease in prescription of FGAs from 61% to 44% between the years 1988 and 2000 [13,30].
Antidepressants were prescribed for 19.42% of patients which was similar to study by Andor et al. in the year 2003 in Switzerland which shows 22.2% of prescriptions among schizophrenic patients, contradictory results are reported by Clark et al. study which shows an increased in usage of antidepressants among schizophrenic patients from 18.5% in 1995 to 35.6% in 1999 and Acquaviva et al. in the year 2002 in France showed 51.1% antidepressant prescriptions which was higher than that observed in the present study [13,29,31]. The reason for the decrease in antidepressant prescriptions may be due to greater effectiveness of SGA on depressive symptoms.
Mood stabilizers were least prescribed for 12.95% patients similar to a study by Andor et al. which showed that 10.9% of prescriptions for mood stabilizers [13]. This was in contrast to Acquaviva et al. study in the year 2002 which showed that 19.4% prescriptions for mood stabilizers [31]. The decrease in rate of prescription of mood stabilizers may be due to increase usage of SGAs which seems to be more effective than FGAs in controlling aggression and mood [32].
Among mood stabilizers lithium was prescribed maximum, for 4.32% patients. Lithium does not enhance antipsychotic effect, but may improve labile affect and agitated behavior in selected patients. However a recent meta-analysis showed that the effect of lithium as an augmentation agent seems to be inconclusive [2].
The study conducted by Covell et al. in USA from 1996 to 1998 and Ren et al. USA showed that olanzapine received the maximum prescriptions [18,33]. Acquaviva et al. in the year 2002 showed that 28.6% of prescriptions were provided for olanzapine [31]. However in the present study 54.68% of patients received olanzapine. This may be due to the increase in the prescription of SGAs. The study by Acquaviva et al. showed that risperidone received 11% of prescriptions while in the present study; risperidone prescription was more (43.17%) [31]. A study conducted by Essock [28] in USA between 1998 and 1999 showed that among SGAs risperidone was prescribed maximum (23%) in 1988 which increased to 27% in 1999. Prescription of olanzapine increased from 18% in 1998 to 27% in 1999 but the growth of prescriptions for olanzapine was 5% compared to 4% for risperidone, thus showing a favorable trend for olanzapine which is seen in our study. Research studies have shown that olanzapine may have greater efficacy than risperidone among patients with chronic schizophrenia [34,35].
Clozapine was prescribed for 16.55% of patients. Study conducted by Weissman et al. and Essock [30]. The study of Essock SM had shown a decrease in the prescription of clozapine, this may be because of safety concerns and the need for white blood cell monitoring, it is generally recommended by TIMA antipsychotic algorithm (2003) that patients be tried on two new SGAs as monotherapy before proceeding to a trial of clozapine [28].
Among FGA tab haloperidol was prescribed maximum 22 (15.83%) patients similar to study by Acquaviva et al. [31] in the year 2002 France and study by Fourier et al. in the year 1996 in France [36]. Haloperidol is a potent antipsychotic drug but has a high propensity to cause adverse effects. Where there is no treatment option, use of haloperidol to counter the damaging and potentially dangerous consequences of untreated schizophrenia is justified. However, where a choice of drug is available, clinicians may wish to prescribe an alternative antipsychotic with less likelihood of adverse effects such as Parkinsonism, akathisia and acute dystonias [37].
Acquaviva et al. study in the year 2002 in France showed 32.9% prescriptions for anticholinergics which were less than our study but a study by Fourrier et al. in the year 1996 in France shows 86.1% prescription for anticholinergics and Ungavari et al. in the year 1996 study in Hong Kong shows 61.8% which were higher than our study [31,36,38]. Study by Fourrier et al. showed 52.3% prescriptions for anxiolytics which was comparable to our study [36]. Anticholinergics are routinely used to treat extrapyramidal symptoms that may occur in most patients’ receiving neuroleptic treatment.
Benzodiazepines are used for a variety of purposes in schizophrenia including anxiety, agitation, disruptive behaviour, motor disturbances and sometimes also for the augmentation of antipsychotic therapy to alleviate positive symptoms. Addition of a benzodiazepine to an antipsychotic may be as acceptable as antipsychotic monotherapy for people with schizophrenia. The effectiveness of benzodiazepines to calm acutely ill patients early in treatment has been documented [39]. Among anxiolytics tab lorazepam was prescribed maximum (48.92%) similar to study by Magliano et al. in Italy during the year 1998 [40].
Conclusion
An observational study was carried out to assess the clinical characteristics of schizophrenia and the treatment pattern of the disease in a tertiary care hospital of south India. An overall male predominance of schizophrenia among male population, especially more in age group below 40 years and the female domination above 40 years of age was observed. Paranoid schizophrenia was the most prevalent subclass. Second generation antipsychotics were the major class of treatment provided among which olanzapine received maximum prescriptions. Haloperidol was the major drug used among first generation antipsychotics. For the management of schizoaffective disorders, mood stabilizers like lithium, anxiolytics like lorazepam, antidepressants like fluoxetine and sertraline were commonly prescribed. Anticholinergic like benzhexol was prescribed for controlling the extrapyramidal side effects of antipsychotics. The increasing trend of prescribing second generation antipsychotics reflect the efficacy and safety profile as compared to first generation antipsychotics.
References
- WU EQ, Shi L, Birnbaum H, Hudson T (2006) Annual prevalence of diagnosed schizophrenia in the USA: A claims data analysis approach. Psychol Med 36: 1535-1540.
- Crismon ML, Buckley PF (2005) Schizophrenia. In: Pharmacotherapy a pathophysiology approach. Dipiro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey LM (eds) Mc Graw Hill (6th edn) USA. pp: 1209-1234.
- Padmavati R, Rajkumar S, Srinivasan TN (1998) Schizophrenic patients who were never treated: A study in an Indian urban community. Psychol Med 28: 1113-117.
- Sethi BB, Gupta SC, Mahendru RK, Kumari P (1974) Mental health and urban life: A study of 850 families. Br J Psychiatry 124: 243-246.
- Nandi DN, Mukherjee SP, Boral GC, Ajmany S (1980) Socio-economic status and mental morbidity in certain tribes and castes in India: A cross-cultural study. Br J Psychiatry 136: 73-85.
- Janssen BB, Weinmann S, Berger M, Gaebel W (2004) Validation of polypharmacy process measures in inpatient schizophrenia care. Schizoph Bull 30: 1023-1033.
- Stahl S (2000) Neuroscientific basis and practical applications. Essential Psychopharmacology (2nd edn) Cambridge University Press, New York. p: 601.
- Siris SG (2000) Depression in schizophrenia: Perspective in the era of "atypical" antipsychotic agents. Am J Psychiatry 157: 1379-1389.
- Olfson M, Marcus S, Pincus H, et al. (1998) Antidepressant prescribing practices of outpatient psychiatrists. Arch Gen Psychiatry 55: 310-316.
- Wang PS, Joyce CW, Terri T, Pincus HA (2000) Recent patterns and predictors of antipsychotic medication regimens used to treat schizophrenia and other psychotic disorders. Schizophr Bull 26: 451-457.
- Dawkins K, Lieberman JA, Lebowitz BD, Hsiao JK (1999) Antipsychotics: Past and Future National Institute of Mental Health Division of Services and Intervention Workshop, July 14, 1998. Schizophr Bull 25: 395-405.
- Dutta SB, Dhasmana DC, Bhardwaj R (2005) Psychotropic drug utilization pattern among patients with schizophrenia. Indian J Psychiatry 47: 243-244.
- Andor E, Peter M, Hess L, Valterio C (2005) Antipsychotic use in patients with schizophrenia treated in private psychiatry. Swiss Med Wkly 135: 109-115.
- Chaudhary PK, Deka K, Chetai D (2006) Disability associated with mental disorders. Indian J Psychiatry 48: 95-101.
- Welham JL, Thomis RJ, McGrath JJ (2004) Age at first registration for affective psychosis and schizophrenia. Schizophr Bull 30: 849-853.
- Malinger JB, Fisher SG, Brown T, Lamberti JS (2006) Racial disparities in the use of second-generation antipsychotics for the treatment of schizophrenia. Psychiatr Serv 57: 133-136.
- Rosenheck R, Stroup S, Keefe RS, McEvoy J, Swartz M, et al. (2005) Measuring outcome priorities and preferences in people with schizophrenia. British J Psychiatry 187: 529-536
- Ren XS, Kazis LE, Lee AF, Hamed A, Huang YH, et al. (2002) Patient characteristics and prescription pattern of atypical antipsychotics among patients with Schizophrenia. J Clin Pharm Ther 27: 441-451.
- Ritsner M, Sherina O, Ginath Y (1992) Genetic epidemiological study of schizophrenia: Reproductive behaviour. Acta Psychiatr Scand 85: 423-429.
- Lane A, Byrne M, Mulvany F, Kinsella A, Waddington JL, et al. (1995) Reproductive behaviour in schizophrenia relative to other mental disorders: Evidence for increased fertility in men despite reduced marital rate. Acta Psychiatr Scand 91: 222-2528.
- Nanko S, Moridaira J (1993) Reproductive rate in schizophrenic outpatients. Acta Psychiatr Scand 87: 400-404.
- Odegaard O (1980) Fertility of psychiatric first admissions in Norway 1936-1975. Acta Psychiatr Scand 62: 212-220.
- Thara R, Srinivasan TN (1997) Marriage and gender in schizophrenia. Indian J Psychiatry 39: 64-69.
- Thara R, Padmavathi R, Lakshmi A, Karagavalli P (2005) Family education in schizophrenia: A comparison of two approaches. Indian J Psychiatry 47: 218-221.
- Ponnudurai R, Jayakar J, Sekaran BWCS (2006) Assessment of mortality and marital status of schizophrenic patients over a period of 13 years. Indian J Psychiatry 48: 84-87.
- Thakr G, Admi H, Moran M, Lahti A (1993) Psychiatric illnesses in families of subjects with schizophrenia: Spectrum personality disorders: High morbidity risks for unspecified functional psychosis and schizophrenia. Am J Psychiatry 150: 66-71.
- Burns T, Christova L, Cooper S, Harrison G, McKendrick J et al. (2006) Maintenance antipsychotic medication pattern in outpatients Schizophrenia patients: a naturalistic cohort study. Acta Psychiatr Scand 113: 126-134.
- Essock SM (2002) Antipsychotic prescribing practices. Schizophr Bull 28: 1-4.
- Clark RE, Bartels SJ, Mellman TA, Peacock WJ (2002) Recent trends in antipsychotic combination therapy of schizophrenia and schizoaffective disorders: Implications for state mental health policy. Schizophr Bull 28: 75-84.
- Weissman EM (2002) Antipsychotic prescribing practices in the Veterans Healthcare Administration: New York metropolitan region. Schizophr Bull 28: 31-42.
- Acquaviva E, Gansquet L, Falissard B (2005) Psychotropic combination in schizophrenia. Eur J Clin Pharmacol 61: 855-861.
- Barak Y, Mireck I, Knobler HY, Natan Z, Aizenberg D (2004) Suicidality and second generation anytipsychotics in schizophrenia patients: A case-controlled retrospective study during a 5-year period. Psychopharmacol 175: 215-219.
- Covell NH, Jackson CT, Evans AC, Essock SM (2002) Antipsychotic prescribing practices in Connecticut's public mental health system: Rates of changing medications and prescribing styles. Schizophr Bull 28:17-29.
- Volavka J, Czobor P, Sheitman B, Lindenmayer JP, Citrome L, et al. (2002) Clozapine, olanzapine, risperidone, and haloperidol in the treatment of patients with chronic schizophrenia and schizoaffective disorder. Am J Psychiatry 159: 255-262.
- Opolka JL, Rascati KL, Brown CM, Gibson PJ (2004) Ethnicity and prescription patterns for haloperidol, risperidone, and olanzapine. Psychiatr Serv 55: 151-156.
- Fourrier A, Gasquet I, Allicar MP, Bouhassira M, Lépineet JP, et al. (2000) Pattern of neuroleptic drug prescription: A national cross sectional survey of a random sample of French psychiatrists. Br J Clin Pharmacol 49: 80-86.
- Joy CB, Adams CE, Lawrie SM (2001) Haloperidol versus placebo for schizophrenia. Cochrane Database Syst Rev 2.
- Ungavari GS, Chung YG, Chee YK, Fungâ€ÂShing N, Kwong TW, et al. (2002) The pharmacological treatment of Schizophrenia in Chinese patients: A comparison of prescription pattern between 1996 and 1999. Br J Clin Pharmacol 54: 437-444.
- Volz A, Khorsand V, Gillies D, Leucht S (2007) Benzodiazepines for schizophrenia. Cochrane Database Syst Rev 1.
- Magliano L, Fiorillo A, Guarneri M, Marasco C, De Rosa C, et al. (2004) Prescription of psychotropic drugs to patients with schizophrenia: An Italian national survey. Eur J Clin Pharmacol 60: 513-522
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi