Research Article, J Spine Neurosurg Vol: 7 Issue: 4
Protection of Paravertebral Muscles and Short Segment Stabilization in Surgical Treatment of Thoracic and Lumbar Compression Fractures
Sukru Oral1*, Atilla Yilmaz1, Ahmet Kucuk2, Halil Ulutabanca2 and Ahmet Selcuklu2
1Department of Neurosurgery, Mustafa Kemal University, Turkey
2Department of Neurosurgery, Erciyes University Medical Faculty, Turkey
*Corresponding Author : Sukru Oral
Department of Neurosurgery, Mustafa Kemal University, Tayfur Ata Sökmen Medical Faculty, Serinyol, Antakya, 31040, Hatay, Turkey
Tel: +90 5072335288
E-mail: sukruor@yahoo.com
Received: September 09, 2018 Accepted: September 20, 2018 Published: September 27, 2018
Citation: Oral S, Yilmaz A, Kucuk A, Ulutabanca H, Selcuklu A (2018) Protection of Paravertebral Muscles and Short Segment Stabilization in Surgical Treatment of Thoracic and Lumbar Compression Fractures. J Spine Neurosurg 7:4. doi: 10.4172/2325-9701.1000306
Abstract
Objective: In this study, patients with thoracolumbar and lumbar fracture fractures were treated with preservation of the paravertebral muscles, unfused posterior short-segment pedicle instrumentation technique. Methods: Between the years 2009-2015, 24 patients were applied short-segment posterior instrumentation surgery for thoracolumbar and lumbar compression fractures in our clinic included in the study. On radiological evaluation, loss of height in spinal anterior corpus (LHSAC) and local angle of kyphosis (LAK) were used. In the operation, the thoracolumbar fascia opened linearly, fascia was excised laterally and finger-dislocated between the multifidus and longissimus muscles. The transversal processes of vertebrates and manufactured objects were found. The transpedicular screws were placed with the C-arm. Results: The mean local angle of kyphosis measured preoperatively was 11.03 degrees and this angle 7.24 degrees at the end of the first year. Before the operation, loss of height in the spinal anterior corpus (LHSAC) was determined as 27.21% on average. At the end of the 1st year, the mean LHSAC was measured as 22.83%. Mean duration of the operation was 103.75 min and mean blood loss was 123.12 ml. Conclusion: In this surgical procedure, preservation of the paravertebral muscles contributes to vertebral column stabilization in cases of short segment instrumentation. For this reason, short segment instrumentation in thoracic and lumbar locations provides a significant kyphotic improvement in patients with compression fractures.
Keywords: Short segment; Paravertebral muscles; Compression fracture
Introduction
Fractures and injuries in the thoracolumbar (T11-L2) area are the most common pathologies in spinal injuries. They constitute 20% of all spinal traumas, and 4-42% of these cases have neurological damage [1]. Lower lumbar location (L3-L5) fractures are less common, and it’s usually shaped a burst fracture [2]. Nowadays, many conservative and surgical methods are applied for thoracolumbar and lumbar location fractures. In the treatment of these fractures, the aim is to provide neurological and mechanical stability [3]. There are many different views and classifications about the selection of surgical methods. For surgical methods, techniques including with fusion and non-fusion posterior, anterior and combined instrumentation are used recently [4]. Posterior short-segment pedicle instrumentation is a widely used method for the treatment of instability, emerging after thoracolumbar and lumbar location fractures [5]. Multifidus muscles in the paravertebral location are responsible for spinal extension, rotation and stabilization. These muscles spread to three joint segments and work to stabilize joints at each segment level. In addition, these muscles reduce degeneration of joints. Unfortunately, these muscles are sometimes damaged during trauma, often during surgical dissection. In this study, patients with thoracolumbar and lumbar fracture fractures were treated with preservation of the paravertebral muscles, unfused posterior short-segment pedicle instrumentation technique, and postoperative clinical and radiological results are stated.
Material and Methods
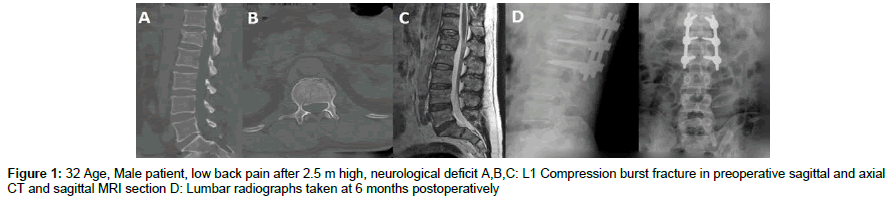
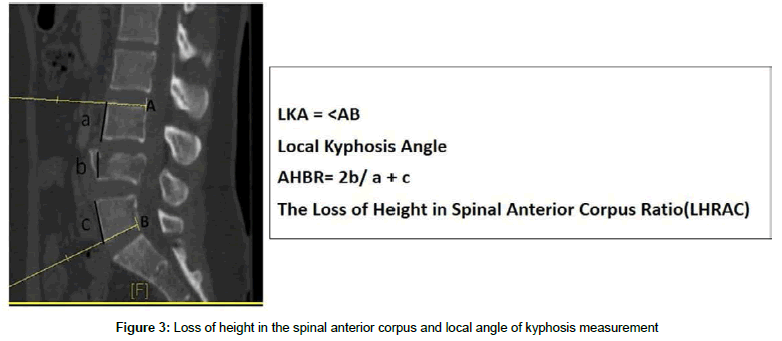
Between the years 2009-2015, 24 patients were applied shortsegment posterior instrumentation surgery for thoracolumbar and lumbar compression fractures in our clinic (Erciyes University Medical Faculty, Neurosurgery Department) were evaluated. We collected information of patient demographics (age and sex), operation time and blood loss (Table 1). Their clinical and radiological results were followed at certain time intervals. The neurological status of the cases was evaluated by Frankel Classification. Patients with Frankel E were taken to study. Preoperative evaluation of the patients was done with CT (Computer Tomography) and MRI (Magnetic Resonance Imaging). X-ray and CT were used at the postoperative 6th month and 1st year controls of the patients (Figure 1 and Figure 2). Patients without additional problems were mobilized with a lumbosacral or thoracolumbar corset in the postoperative early period (8-24 hours). And patients were provided to have been using corsets for 8-12 weeks. On radiological evaluation, loss of height in spinal anterior corpus (LHSAC) and local angle of kyphosis (LAK) were used. LHSAC was calculated by Keene method (Figure 3). LAK was measured by calculating the angle between the parallel line drawn on the upper end plate of the stable vertebrae above the broken vertebrae and the parallel lines drawn on the lower vertebrae (Figure 3).
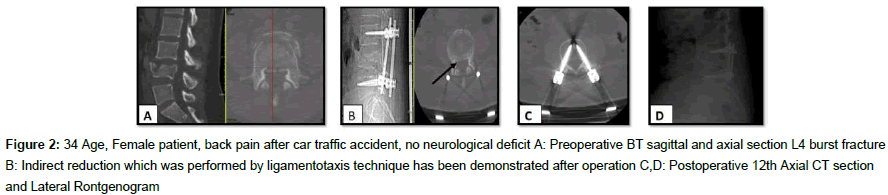
Figure 2: 34 Age, Female patient, back pain after car traffic accident, no neurological deficit A: Preoperative BT sagittal and axial section L4 burst fracture B: Indirect reduction which was performed by ligamentotaxis technique has been demonstrated after operation C,D: Postoperative 12th Axial CT section and Lateral Rontgenogram
| Age | Sex | Level of fracture | Frankel Score | LAK Preop. | LAK Postop. | Blood Loss (ml) | LHSAC Preop.(%) | LHSAC Postop.(%) | Operation Time (Min) |
|---|---|---|---|---|---|---|---|---|---|
| 58 | K | L2 | E | 6,92 | 0,77 | 110 | 34 | 27 | 105 |
| 40 | K | L4 | E | 14,16 | 6,05 | 145 | 25 | 17 | 95 |
| 63 | K | T12 | E | 22,42 | 17,85 | 125 | 43 | 34 | 90 |
| 26 | E | T12 | E | 24,71 | 18,56 | 105 | 25 | 40 | 110 |
| 51 | K | L2 | E | 0,81 | 2,76 | 165 | 18 | 22 | 120 |
| 34 | K | L1 | E | 14,26 | 7,24 | 150 | 19 | 20 | 85 |
| 35 | E | L2 | E | 5,64 | 1,21 | 120 | 11 | 16 | 90 |
| 41 | K | T12 | E | 24,79 | 19,94 | 110 | 35 | 20 | 90 |
| 44 | E | T12 | E | 21,34 | 10,47 | 135 | 37 | 35 | 95 |
| 38 | E | L2 | E | 17,25 | 5,67 | 130 | 20 | 20 | 105 |
| 27 | K | T12 | E | 23,4 | 16,23 | 125 | 45 | 16 | 110 |
| 36 | E | L3 | E | 7,64 | 2,52 | 115 | 33 | 24 | 85 |
| 29 | E | L1 | E | 13,8 | 8,21 | 110 | 22 | 18 | 90 |
| 34 | K | L4 | E | 12,18 | 6,45 | 100 | 33 | 24 | 95 |
| 56 | K | L2 | E | 5,87 | 1,76 | 105 | 18 | 17 | 90 |
| 46 | E | L2 | E | 1,77 | 2,32 | 120 | 20 | 15 | 90 |
| 32 | E | T12 | E | 12,95 | 7,21 | 145 | 34 | 20 | 105 |
| 16 | E | L2 | E | 6,87 | 4,55 | 120 | 23 | 19 | 100 |
| 53 | K | L2 | E | 4,57 | 1,33 | 125 | 18 | 10 | 130 |
| 52 | K | L1 | E | 0,08 | 9,92 | 120 | 10 | 24 | 110 |
| 34 | E | L2 | E | 10,02 | 8,92 | 105 | 37 | 30 | 125 |
| 58 | E | L2 | E | 3,84 | 2,26 | 160 | 35 | 40 | 150 |
| 32 | E | L1 | E | 4,24 | 3,16 | 110 | 28 | 20 | 130 |
| 50 | E | T12 | E | 5,34 | 8,48 | 100 | 30 | 20 | 95 |
Table 1: Information of patient demographics (age and sex), operation time and blood loss.
Surgical technique
All the patients underwent surgery in prone position under general anesthesia. While the prone position was given, head part was supported with special cushions in the form of bagels as eyes and nose is free and open, thorax and pelvis upper part is supported by rolls and pillows. Elastic bandages were used to prevent venous ponding in the lower extremities. 1 hour before the operation, the patients are routinely treated with 25 mg/kg of prophylactic or max. 2 gr. of intravenous cefazolin was applied. The incision was made of a middle line of the broken vertebra covering a top and a bottom. The thoracolumbar fascia opened bilaterally linearly. Fascia was excised laterally and finger-dislocated between the multifidus and longissimus muscles. The transversal processes of vertebrates and manufactured objects were found. The transpedicular screws were placed with the C-arm. The rods were fixed, paying attention to lordosis and kyphosis (Figure 4). Ligamentotaxis was performed and the reduction was provided. Since the paravertebral muscles were protected, transverse connection and fusion were not put. Then the fascias, subcutaneous and skin were closed appropriately.
Statistical method
Whether the distribution of the groups was normal or not was determined by using the Shapiro-Wilk-W test for parametric tests. In addition to this test, normalization of the distributions was examined by using the SPSS program. Obtained continuous data were given as an average. For intergroup analysis, the Paired-T test was used. The obtained value of “p”<0.05 was accepted as statistical significance level. SPSS Statistics 22.0 program was used for the statistical calculations.
Discussion
The mean LAK measured preoperatively was 11.03 degrees and this angle 7.24 degrees at the end of the first year. This improvement in the mean local angle of kyphosis with 3.79 degrees was found to be statistically significant (p=0.01). Before the operation, LHSAC was determined as 27.21% on average. At the end of the 1st year, the mean LHSAC was measured as 22.83%. This height loss seen in the Anterior Body Height Ratio (ABHR) was statistically significant (p=0.03) (Table 2). Mean duration of the operation was 103.75 min and mean blood loss was 123.12 ml (Table 1).
| n | Mean (%) | Standart Deviation | Mean of change | P Değeri | |
|---|---|---|---|---|---|
| Preoperative LKA | 24 | 11,0363 | 7,86162 | 3,79 | P=0.01 |
| Postoperative LKA | 24 | 7,2433 | 5,78102 | ||
| Preoperative LHSAC | 24 | 27,21 | %9,523 | %4,38 | P=0.03 |
| Postoperatie LHSAC | 24 | 22,83 | %7,828 | ||
| LKA: | Local Angle of Kyphosis | ||||
| LHRAC: | Loss of Height in Spinal Anterior Corpus | ||||
Table 2: Changes in LAK and LHSAC before and after surgery
Thoracolumbar (T10-L2), traumatic fractures of the spine are the most common fractures of the spinal column [6]. The thoracolumbar burst fracture may be caused by a failure of the anterior vertebral body against this force when the vertebral body is subjected to significant axial, and possibly flexural, forces [7]. These injuries can be treated in different ways by evaluating the clinical status and radiographic findings of the cases. Conservative and surgical methods can be used in the treatment. Neurological deficits and spinal instability are the most important factors in determining the need for surgery. However, in the conservative treatment of thoracolumbar burst fractures, corset use and limited mobilization reduce the need for surgical intervention and the morbidity that the surgical will create. Therefore, the choice of surgical or conservative treatment for the treatment of thoracolumbar burst fractures and the efficiency of these methods are still controversial, especially in non-neurological deficit cases [8]. However, the general opinion is that surgical treatment is necessary for cases without neurological deficit when 50% and above the canal pressure, and 25° and above kyphotic angulation is found [9]. The aim of surgical treatment of thoracolumbar burst fractures is to provide a rigid stabilization of the spinal canal and nerve roots to get decompression, neurological recovery, and restoration, ease of nursing care, early ambulance and rehabilitation. Furthermore, the surgical treatment limits the number of posttraumatic progressive deformities and vertebrae moving segments [10]. Approach to thoracolumbar burst fractures and their stabilization choice of surgical technique has long been a matter of debate. Among the surgical approaches for thoracolumbar fractures, posterior short segment pedicle instrumentation is one of the most commonly used techniques due to the availability of 3-column stabilization [11]. Markel and colleagues compared short segment fixation with long segment instrumentation and fusion in the treatment of some thoracolumbar burst fractures and showed that short segment fixation gave more successful results [12]. Similarly, Parker and colleagues reported that the most successful way of in thoracolumbar burst fractures is short segment transpedicular stabilization [5]. However, nowadays debate is whether short segment transpedicular stabilization is still an appropriate method. We also performed short segment transpedicular instrumentation to our cases. Advanced surgical techniques and implants with spinal surgery, give satisfactory results. Surgical treatment provides immediate spinal stability and more reliable sagittal alignment, vertebra height is maintained, and canal pressure is removed. Alvine et al. [13] reported that in patients with paraplegic and unstable fractures, indirect decompression is as effective as direct decompression. Similarly, Gertzbein et al. [14] reported that with ligamentotaxis the incidence of canal stenosis was reduced from 54% to 40%, especially in patients who were treated in the first 4 days. In our study, we also performed ligamentotaxis on all of our cases and we achieved the reduction by indirect decompression. In their study comparing short and long segment stabilization in thoracolumbar burst fractures of Tezeren and Kuru, found a 55% ratio 10-degree loss of correction in sagittal alignment in the short-segment instrumentation group, but they reported that there was no such loss of correction in long segment stabilization structures [15]. In our study, there was no loss of local kyphosis at the end of the first year in our patients, and an average improvement of 3.79 degrees was observed. And our results supported the knowledge of the literature. Spinal fusion has always been a part of the stabilization procedure. Theoretically, unless spinal fusion was used, the stabilization surgeon might be less successful. However, Sanderson and colleagues achieved satisfactory results in the short-segment fusion-free stabilization of thoracolumbar burst fractures and they noted that posterior or posterolateral fusion in short segment stabilization is unnecessary [16]. Wang and colleagues compared two groups having thoracolumbar burst fractures by using fusion and non-fusion in their study. They reported that there was no significant difference in loss of kyphotic angle between the two groups. In addition, in the same study, the anterior vertebral body height loss was measured between 3.6% and 8.3% [17]. In our study, the loss of height anterior vertebrae was measured as 4.38% at the end of the first year. In addition, our patients had not been given any fusion since the paravertebral muscles were protected. In our sagittal series, no loss of cornea was observed. Our findings were consistent with the literature. This idea is supported in recent years [9,18,19]. Therefore, we think that fusions made with various grafts are not needed in cases of thoracolumbar burst fractures. In addition, costs and infections caused by graft use can be reduced. In the traditional treatment of thoracolumbar burst fractures, muscle dissection and retraction are performed. Multifidus muscles are separated from the laminae, longissimus and iliolumbar muscles by adhesions to the facet joints, either by cutting with surgical scissors or by coagulating with electrocautery. Patients with this type of surgery have waist and back pain complaints postoperatively. Unlike other paraspinal muscles, the multifidus muscles can be easily injured during surgery because they are only underwent by the medial branches of the dorsal ramus [10]. In many studies, minimally invasive techniques have been shown to have less paraspinal muscle atrophy. Therefore, in minimally invasive approaches, atrophy of paravertebral muscles are prevented, intraoperative bleeding is decreased, the drainage system is not needed and pain is less in the postoperative period [20]. Multifidus muscles provide lateral flexion, extension and rotation movements of the vertebral column. They are also responsible for the stabilization of the vertebral column. In our study, the multifidus muscles were preserved during the surgical procedure and intraoperative bleeding was minimal and no drainage system was needed. So, we didn’t use monoaxial pedicle screw. Because, you will appreciate that It is very difficult to place the rod system in this technique. But, we know that monoaxial pedicle screw exhibited more stability in flexion and extension than the polyaxial pedicle screw in in short-segment fixation.
In our method, transpedicular instruments were placed between the paravertebral muscles by making a single linear incision in the middle hump in the thoracic or lumbar location. In other minimally invasive methods mentioned in the literature, two paramedian skin incisions or in the percutaneous method, a separate incision was made for each instrument [9,21,22]. Therefore, our technique can be implemented more easily and quickly than other minimally invasive techniques.
Conclusion
In this study, for the first time, we demonstrated the technique of short segment transpedicular instrument placement in compression fractures with a single surgical incision made in the dorsal midline. This technique may be preferred in terms of reduced intraoperative bleeding in surgery, short operative time, postoperative hospital stay, and not using fusion, in appropriate cases. In addition, in this surgical procedure, preservation of the paravertebral muscles contributes to vertebral column stabilization in cases of short segment instrumentation. For this reason, short segment instrumentation in thoracic and lumbar locations provides a significant kyphotic improvement in patients with compression fractures.
References
- Esses SI, Botsford DJ, Kostuik JP (1990) Evaluation of surgical treatment for burst fractures. Spine 15: 667-673.
- Sansur CA, Shaffrey CI (2010) Diagnosis and Management of Low Lumbar Burst Fractures. Seminars in Spine Surgery 22: 33-37.
- Benson DR, Burkus JK, Montesano PX, Sutherland TB, McLain RF (1992) Unstable thoracolumbar and lumbar burst fractures treated with the AO fixateur interne. J Spinal Disord 5: 335-343.
- Dai LY, Jiang SD, Wang XY, Jiang LS (2007) A review of the management of thoracolumbar burst fractures. Surg Neurol 67: 221-231.
- Parker JW, Lane JR, Karaikovic EE, Gaines RW (2000) Successful short-segment instrumentation and fusion for thoracolumbar spine fractures: a consecutive 41/2-year series. Spine 25: 1157-1170.
- Wood KB, Li W, Lebl DR, Ploumis A (2014) Management of thoracolumbar spine fractures. Spine J 14: 145-164.
- Briem D, Lehmann W, Ruecker AH, Windolf J, Rueger JM, et al. (2004) Factors influencing the quality of life after burst fractures of the thoracolumbar transition. Arch Orthop Trauma Surg 124: 461-468.
- Rajasekaran S (2010) Thoracolumbar burst fractures without neurological deficit: the role for conservative treatment. Eur Spine J 1: S40-7.
- Lee JK, Jang JW, Kim TW, Kim TS, Kim SH, et al. (2013) Percutaneous short-segment pedicle screw placement without fusion in the treatment of thoracolumbar burst fractures: is it effective?: comparative study with open short-segment pedicle screw fixation with posterolateral fusion. Acta Neurochir (Wien) 155: 2305-2312.
- Hu ZJ, Fang XQ, Fan SW (2014) Iatrogenic injury to the erector spinae during posterior lumbar spine surgery: underlying an atomical considerations, preventable root causes, and surgical tips and tricks. Eur J Orthop Surg Traumatol 24: 127-135.
- Siebenga J, Leferink VJ, Segers MJ, Elzinga MJ, Bakker FC, et al. Treatment of traumatic thoracolumbar spine fractures: a multicenter prospective randomized study of operative versus nonsurgical treatment. Spine 31: 2881-2890.
- Markel DC, Graziano GP (1995) A comparison study of treatment of thoracolumbar fractures using the ACE Posterior Segmental Fixator and Cotrel-Dubousset instrumentation. Orthopedics 18: 679-686.
- Alvine GF, Swain JM, Asher MA, Burton DC (2004) Treatment of thoracolumbar burst fractures with variable screw placement or Isola instrumentation and arthrodesis: case series and literature review. J Spinal Disord Tech 17: 251-264.
- Gertzbein SD, Crowe PJ, Fazl M, Schwartz M, Rowed D (1992) Canal clearance in burst fractures using the AO internal fixator. Spine 17: 558-560.
- Tezeren G, Kuru I (2005) Posterior fixation of thoracolumbar burst fracture: short-segment pedicle fixation versus long-segment instrumentation. J Spinal Disord Tech 18: 485-488.
- Sanderson PL, Fraser RD, Hall DJ, Cain CM, Osti OL, et al. (1999) Short segment fixation of thoracolumbar burst fractures without fusion. Eur Spine J 8: 495-500.
- Wang ST, Ma HL, Liu CL, Yu WK, Chang MC, et al. (2006) Is fusion necessary for surgically treated burst fractures of the thoracolumbar and lumbar spine?: a prospective, randomized study. Spine 31: 2646-2652.
- Jindal N, Sankhala SS, Bachhal V (2012) The role of fusion in the management of burst fractures of the thoracolumbar spine treated by short segment pedicle screw fixation: a prospective randomised trial. J Bone Joint Surg Br 94: 1101-1106.
- Hwang JU, Hur JW, Lee JW, Kwon KY, Lee HK (2012) Cmparison of posterior fixation alone and supplementation with posterolateral fusion in thoracolumbar burst fractures. J Korean Neurosurg Soc 52: 346-352.
- Kim CW (2010) Scientific basis of minimally invasive spine surgery: prevention of multifidus muscle injury during posterior lumbar surgery. Spine 35: S281-286.
- Hoh DJ, Wang MY, Ritland SL (2010) Anatomic features of the paramedian muscle-splitting approaches to the lumbar spine. Neurosurgery 66: 13-24.
- Wiltse LL, Spencer CW (1988) New uses and refinements of the paraspinal approach to the lumbar spine. Spine 13: 696-706.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi