Short Communication, J Otol Rhino Vol: 12 Issue: 4
Pseudocyst of Pinna-New Method of Surgical Management
Sudhangshu Kumar B1*, Devnath T2, Shailendra Nath B3, Asim S3, and Susmita B4
1Department of ENT, Khulna Medical College and Hospital, Khulna, Bangladesh, India
2Department of Resident Surgeon, Khulna Medical College and Hospital, Khulna, Bangladesh, India
3Department of Medicine, Khulna Medical College and Hospital, Khulna, Bangladesh, India
4Department of MPH Student at Tata Institute of Social Science, Mumbai, India
*Corresponding Author: Sudhangshu Kumar B, Department of ENT, Khulna Medical College and Hospital, Khulna, Bangladesh, India; E-mail: ballavsk@yahoo.com
Received date: 28 December, 2021, Manuscript No. JOR-22-51120; Editor assigned date: 30 December, 2021, PreQC No. JOR-22-51120; Reviewed date: 13 January, 2022, QC No. JOR-22-51120; Revised date: 28 February, 2022, Manuscript No. JOR-22-51120; Published date: 08 March, 2022, DOI: 10.4712/2324-8785.1000434
Citation: Sudhangshu Kumar B, Devnath T, Shailendra Nath B, Asim S, Susmita B (2022) Pseudocyst of Pinna-New Method of Surgical Management. J Otol Rhino 11:4.
Description
Pseudocyst of pinna is not very common problem in ENT practice. This is a benign painless cystic swelling arising in pinna and visible on lateral surface of pinna. No obvious cause of this swelling can be identified. This is an intra-cartilaginous cyst without any epithelial lining. So, the name pseudocyst there is no definite and effective medical treatment for this pseudocyst [1]. There are so many surgical treatments available. We describe a novel minimal surgical technique for this condition. 18 patients 12 male and 6 female ages ranging from 40 -60 years were included in this trial. All patients were selected from my private consultancy between January 1, 2015 to December 31, 2018 [2]. With proper aseptic measure and under local anesthesia very small stab incision given by no 15 BP blade on most dependent part and a ventilation tube made up of plastic tube of a butterfly needle inserted through the stab incision just like grommet insertion on tympanic membrane. Both ends of the plastic tube just heated by gas lighter and pressed on any hard smooth surface so that ends of the tube take a shape of grommet. These patients were followed up over 3 months. 16 patients had successful outcome. We observed complete resolution after 2 weeks [3]. Patients were advised to restrict head bath to avoid water entry through the tube while the tube was in situ. 2 patients develop secondary infection which was controlled by broad spectrum antibiotics and got cured. The new technique of surgical management is very simple, inexpensive, and effective minimal surgical method of management for the pseudocyst of pinna.
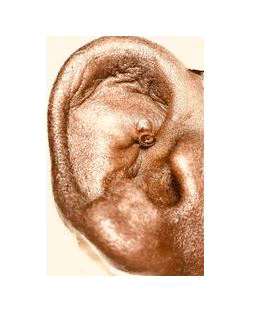
Pseudocyst of pinna is an idiopathic benign painless cystic swelling developed spontaneously on the lateral aspect pinna due to accumulation of fluid. It is an intra-cartilaginous cyst without having any epithelial lining. The common sites of origin cymba concha, scaphoid fossa and triangular fossa of the pinna. These lesions are also named as endochondral pseudocyst, intra cartilaginous cyst and benign idiopathic cystic chondromalacia. Histologically these are intra cartilaginous cyst without having any epithelial lining hence it is called pseudocyst [4]. The fluid inside the cyst is yellow or straw colored serous or viscous fluid containing glucose and protein. The lesions are mostly unilateral(Figure 1).
These are simple lesions sometimes incidentally found by close contact but difficult to manage either by medical or surgical procedure. Hence there are so many modalities of management described in literature [5]. Whatever modality of treatment is applied the aim of treatment includes restoration and preservation of normal appearance of pinna and prevention of recurrence. We describe our experience of management of these comparatively less common simple lesions of pinna by applying our new and minimal surgical technique. Eighteen patients were diagnosed clinically as pseudocyst of pinna in my private consultation clinic between January 2015 to December 2018. The procedure to be done was explained to the patients and their written consent taken for enrolment in the study.
Diagnosis was made by aseptic aspiration of non-purulent straw or yellow color fluid from the cyst. All patients were posted for our minimal invasive new technique of surgical intervention [6]. With all aseptic precaution and under local anesthesia a stab incision given on selected dependent part of the cyst and through that stab instantly made ear grommet type drain tube made up of butterfly needle set inserted. These self-retaining types of drain tubes were kept in situ for two weeks. After two weeks we observed complete resolution of the cyst. Then we removed the drain tube. The patients were followed up once in a month for 3 months to see any recurrence. Twenty-four patients were diagnosed as cases of pseudocyst of pinna from January 2015 to December 2018. The age distribution in our study group ranged from 25 to 45 years. The lesion was seen more in scaphoid fossa followed by triangular fossa and cymba concha. Twenty-one patients had complete resolution within two weeks. Two patients developed secondary infection which was effectively controlled by broad spectrum antibiotics and subsequently cured(Figure 2) [7].
The pseudocyst of pinna is fairly an uncommon problem found among adult and predominantly in males (88.88%) in our study group consistent with other report. The sites of origin are scaphoid fossa, triangular fossa and cymba concha and concha in order of precedence [8]. The predisposing factors and etiology are not known. Its pathogenesis is hypothetical yet. Hormonal factor may play a part for male predominance. Abnormal release of lysosomal enzymes from chondrocytes gives rise to progressive dilatation and formation of intra cartilaginous cavity. One hypothesis explained congenital embryonic dysplasia of the auricular cartilage that leads to formation of pseudocyst [9-11].
Conclusion
There is no single accepted method of treatment for this condition. The various modalities of treatment are close aspiration and pressure bandage, aspiration with buttoning, aspiration and intralesional corticosteroid injection, anterior wall deroofing, incision and curettage of cartilage wall, intralesional sclerosing agents etc. are being practiced. Fibrin glue as a sealing material between the two flaps of cartilage has been reported. Whatever method is applied to treatment there is every chance of recurrence in significant number of cases. Almost in all methods of treatment needs compression dressing which is difficult to provide and maintain. Our new technique of grommet type plastic drain tube insertion through a stab incision does not require any pressure dressing. Moreover, it is simple cost effective and compliant to patient with acceptable outcome.
References
- Choi S, Lam KH, Chan KW, Ghadially FN, Ng As (1984) Endochondral pseudocyst of the auricle in Chinese. Arch Otolaryngol 110: 792-796
- Chen Q, Fei Y, Zho T, Luo D, Wu B, et al. (2001) Research on the immunological cause of auricular pseudocyst. Lin Chuang Er Bi Yan Hou Ke Zhi 15:304-305
- Schulte KW, Neumann NJ, Ruzicka T (2001) Surgical pearl: The close-fitting ear cover cast-a noninvasive treatment for pseudocyst of the ear. J Am Acad Dermatol 44: 2856
- Bhat VS, Shipla, Nitha, KS Ravi (2014) Deroofing of auricular pseudocyst: Our experience. J Clin Diagn Res 8:KC05-7
- Miyamoto H, Okajima M, Takahashi I (2001) Lactate dehydrogenase isoenzymes and intralesional steroid injection therapy for pseudocyst of the auricle. Int J Dermatol 40:380-384.
- Engel D (1966) Pseudocysts of the auricle in Chinese. Arch Otolaryngol 83: 197-202.
- Chang CH, Kuo WR, Lin CH, Wang LF, et al. (2004) Deroofing surgical treatment for pseudocyst of the auricle. J Otolaryngol 33: 177-80.
- Tuncer S, Basterzi Y, Yavuzer R (2003) Reccurrent auricular pseudocyst: a new treatment recommendation with currettage and fibrin glue. Dermatol Surg 29: 1080-1083.
- Rehman A, Sangoo M, Hamid S, Wani A, Khan N (2013) Recurrent pseudocyst pinna: A rational approach to treatment. Int J Sci Res Publ 3:1-4.
- Ramadass T, Ayyaswamy G (2006) Pseudocyst of auricle etiopathogenesis, treatment update and literature review. Indian J Otolaryngol Head Neck Surg 58:156-159.
[Crossref] [Google Scholar] [Indexed]
- Lim CM, Goh YH, Chao SS, Lynee L (2002) Pseudocyst of the auricle. Laryngoscope. 112: 2033-2036
[Crossref] [Google Scholar] [Indexed]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi