Research Article, J Nephrol Ren Dis Vol: 1 Issue: 1
Renal Osteodystrophy in End Stage Renal Failure Patients on Maintenance Haemodialysis Visiting at Tertiary Care Hospital, Karachi
Javed Altaf Jat*, Poran Kumara and Dileep Kumar
Department of Urology, Liaquat University of Medical and Health Sciences, Jamshoro, Pakistan
*Corresponding Author : Javed Altaf Jat
Department of Urology, Liaquat University of Medical and Health Sciences, Jamshoro, Pakistan
E-mail: javedaltaf115@gmail.com
Received: July 16, 2016 Accepted: December 09, 2016 Published: January 17, 2017
Citation: Jat JA, Kumara P, Kumar D (2017) Renal Osteodystrophy in End Stage Renal Failure Patients on Maintenance Haemodialysis Visiting at Tertiary Care Hospital, Karachi. J Nephrol Ren Dis 1:1.
Abstract
Objective: To determine the frequency of different patterns of renal osteodystrophy in end stage renal failure patients on maintenance haemodialysis visiting at tertiary care Hospital, Karachi.
Methodology: A Cross sectional study was conducted at Nephrology Department, Jinnah Postgraduate Medical Center, Karachi from April to October 2009. Fifty-six (56) patients on maintenance hemodialysis were included through non-probability purposive sampling. Various biochemical parameters of renal osteodystrophy were included in the current study. Serum corrected calcium, phosphate, and alkaline phosphatase and iPTH levels. Chi square test was used to determined frequency of renal osteodystrophy in ESRD patients.
Results: Mean age was 45.85 ± 13.5 years. 34 (61%) were male and 22 (39%) were female. Renal osteodystrophy was found in 89%. The most common type was secondary hyperparathyroidism (Osteitis Fibrosa Cystica) in 32%. Hypophosphatemia was observed in 62% while hypercalcaemia in only 7%. Osteomalacia was common in adolescent age group (66%), Osteitis Fibrosa Cystica (OFC) in adult group (36%) while mixed variety in elder group (50%). Similarly OFC was the most common pattern in both genders.
Conclusion: In the present study it was concluded that the prevalence of renal osteodystrophy was significantly increased. Secondary hyperparathyroidism (Osteitis Fibrosa Cystica) is the most common pattern of ROD followed by mixed osteodystrophy and adynamic bone disease.
Keywords: Renal osteodystrophy; End-stage renal failure; Hemodialysis
Introduction
Evidence suggested that mineral and bone metabolism disorders are associated with increased risk for cardiovascular calcification, morbidity, and mortality [1,2]. Renal Osteodystrophy (ROD) is defined as an alteration of bone morphology in patients with Chronic Kidney Disease (CKD), quantifiable by histomorphometry of bone biopsy [3]. The global incidence of ROD in patients with advanced renal failure and those treated with haemodialysis (HD) is 90 to 100% and this begin to appear when GFR falls <60 ml/min [4,5]. In CKD patients, deficiency of calcitriol leads to secondary hyperparathyroidism [6]. This leads to high turnover bone disease (Osteitis Fibrosa Cystica), short turnover bone disease (Adynamic bone disease and Osteomalacia) and mixed variety (Osteitis Fibrosa Cystica and Osteomalacia) [7]. The most accurate diagnostic test for detecting ROD in patients with CKD is bone biopsy but it is invasive and requires trained personnel for its interpretation thus hampering its use in clinical practice [3]. Together with the measurements of serum calcium, phosphorus, and alkaline phosphatase levels, intact PTH (iPTH) is used to evaluate, diagnose, and guide the treatment of renal osteodystrophy [8]. Serum iPTH levels >300 pg/ml strongly suggest the presence of high-turnover skeletal lesions, whereas values <150 pg/ml are consistent with Adynamic osteodystrophy [5]. A sustained elevation of serum phosphate alone among patients with end stage renal failure is associated with increased mortality [9]. Although extensive research has been done worldwide regarding renal Osteodystrophy and its significant association with high mortality has been established, there is dearth of national data available in Pakistan. We conducted study to determine different patterns of renal Osteodystrophy in patients with end stage renal failure (ESRF) on maintenance haemodialysis; so that appropriate management could be done and preventive strategies could be planned.
Material and Methods
A Cross-sectional study was conducted at Nephrology Department, Jinnah Postgraduate Medical Center Karachi from April 2009 to October 2009. Fifty-six (56) patients were included through non-probability Purposive sampling. All patients with end stage renal failure (ESRF) on maintenance haemodialysis (twice/thrice a week for >3 months) were included and patients with acute on chronic renal failure, history of fractures within 6 months, and history of parathyroidectomy were excluded. ESRF was defined as glomerular filtration rate <15 ml/min (calculated through Formula: 140-Age (years) x weight (Kg)/72 x serum creatinine). Three patterns of Renal Osteodystrophy were taken; high turnover or Osteitis Fibrosa Cystica, low turnover (Adynamic and Osteomalacia) and mixed. High turnover/OFC was defined as serum iPTH >300 pg/ ml, high Alkaline phosphatase (N=80-306 U/l), low or normal corrected serum calcium (N=8.8-10.5 mg/dl) and high serum phosphate (N=3.5—5.5mg/dl). In low turnover adynamic was defined as serum iPTH <150 pg/ml, low to normal alkaline phosphatase, Elevated or normal corrected serum Calcium and variable serum phosphate levels while Osteomalacia was defined as low corrected serum calcium & phosphate levels, serum iPTH ≥150 pg/ml & elevated serum alkaline Phosphatase. Mixed features of high turnover bone disease and Osteomalacia that do not fit into the above criteria were defined as mixed type.
Data collection procedure
All patients who visited at the department of Nephrology, Jinnah Postgraduate Medical Center Karachi were included in the study after inclusion and exclusion criteria. Informed written consent was taken from patients and parents in case of age <18 years (adolescence). Predialysis blood sample was taken to measure serum calcium, albumin, phosphate, alkaline phosphate and iPTH. Diagnosis of renal osteodystrophy was made with the help of criteria used in operational definition. All data was taken by Principal investigator on pretested questionnaire.
Data analysis
The data was analyzed by SPSS: 19. Mean and standard deviation were computed for quantitative variables like age, serum calcium, phosphate, alkaline phosphatase and iPTH. Frequency and percentage were computed for categorical variables (Gender, duration of hemodialysis, types of renal osteodystrophy). Chi square test was used to determine proportion of types of renal osteodystrophy among end stage renal disease patient on hemodialysis. P value of <0.05 was taken as significant.
Results
The study was carried out in 56 patients on maintenance hemodialysis. The mean age of the patients was 45.85 ± SD 13.5 years (range 13-76 years). Out of the 56 patients, 34 (61%) were male and 22 (39%) were female. Mean values of serum calcium, phosphate, alkaline phosphatase and IPTH were 8.77 ± 1.1 mg/dl, 5.9 ± 1.6 mg/dl, 268 ± 156 mg/dl, & 406 ± 368 pg/ml respectively, as shown in Table 1. Out of the 56 patients, 37 (66%) patients were on twice weekly hemodialysis while 19 (34%) on thrice weekly. Sixteen (28.5%) patients had duration of hemodialysis <1 year, 24 (42.8%) had between 1-2 years and 16 (28.5%) had >2 years.
| VARIABLES | MEAN ± SD | MEDIAN | RANGE |
|---|---|---|---|
| Corrected calcium (mg/dl) | 8.77 ± 1.1 | 8.8 | 6.1-10.7 |
| Phosphate (mg/dl) | 5.9 ± 1.6 | 06 | 2.6-8.9 |
| Alkaline phosphatase (mg/dl) | 268 ± 156 | 245 | 63-834 |
| iPTH (pg/ml) | 406 ± 368 | 262 | 25-1263 |
Table 1: Mean of Different Variables (N=56).
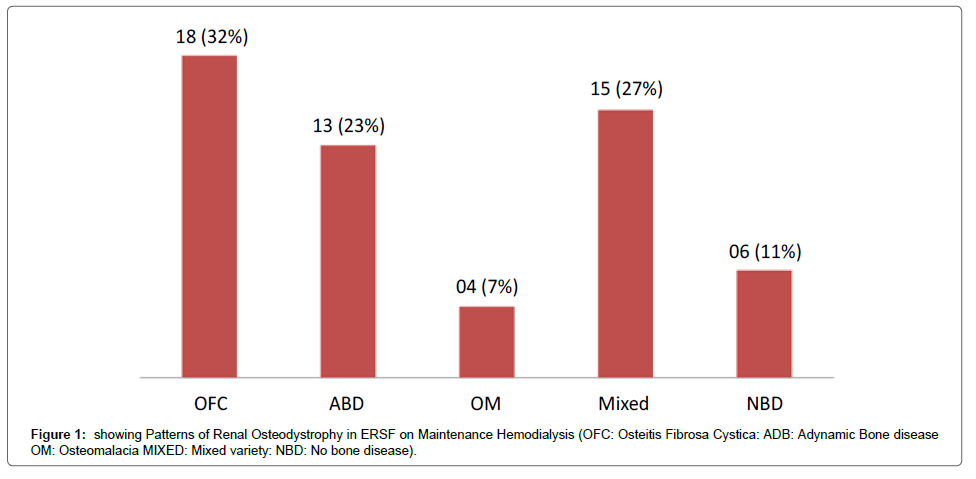
Prevalence of Renal Osteodystrophy in our study was 89.28% (50 patients) while 6 patients (10.7%) had no bone disease. The most common type was secondary hyperparathyroidism (Osteitis Fibrosa Cystica) in 32% of patients followed by mixed 15 (27%) and Adynamic bone disease in 13 (23%) as shown in Figure 1. Proportion of age, gender and duration of hemodialysis in different types of Renal Osteodystrophy is shown in Table 2.
| VARIABLES | OFC | ABD | OM | Mixed | NBD | P value |
|---|---|---|---|---|---|---|
| Age 13—18yrs 19—60yrs >60yrs |
01 (02%) 17 (31%) 00 (00%) |
00 (00%) 11 (20%) 02 (03%) |
02 (03%) 02 (03%) 00 (00%) |
00 (00%) 12 (21%) 03 (05%) |
00 (00%) 05 (10%) 01 (02%) |
0.04 |
| Gender Male Female |
12 (21%) 07 (13%) |
08 (13%) 05 (10%) |
03 (05%) 01 (02%) |
09 (15%) 06 (11%) |
02 (03%) 04 (07%) |
0.02 |
| Duration of hemodialysis <1yr 1-2yrs >2yrs |
06 (11%) 06 (11%) 05 (10%) |
03 (05%) 07 (13%) 03 (05%) |
02 (03%) 01 (02%) 01 (02%) |
02 (03%) 10 (18%) 04 (07%) |
03 (05%) 00 (00%) 03 (05%) |
0.00 |
Table 2: Patterns of Renal Osteodystrophy in ESRF (N=56).
Discussion
About 2/3 of all dialysis patients die within 5 years of beginning of dialysis treatment [10]. In chronic kidney disease the disturbances in mineral and bone metabolism are prevalent and an important cause of morbidity, extra-skeletal calcification and decreased quality of life that have been associated with increased cardiovascular mortality [3]. This study describes the frequency of different types of Renal Osteodystrophy (ROD) in End stage Renal Failure (ESRF) patients on maintenance hemodialysis. In our study about 89% had Renal Osteodystrophy which is higher than the prevalence described in other studies (33-77%) [11-13]. High prevalence due to lower socioeconomic conditions, inadéquates or unrestricted use of phosphate binders, suboptimal dose and short duration of hemodialysis. Recent studies showed that adynamic bone disease is the commonest form of ROD but in our study high turnover bone disease (osteitiis fibrosa cystica) was most common type of ROD among 32% of patients followed by Adynamic bone disease 23% of hemodialysis subjects. This is comparable with the study done by Buargub et al., they reported high prevalence of adynamic bone disease in 27% of hemodialysis patients [4]. A study done by Galea et al. showed similar finding; 45% had high turnover bone disease (iPTH>100 pg/ml) while 42% had low turnover bone disease (iPTH <79.7 pg/ml). The cut off levels for iPTH were low as compare to our study [14]. A considerable percentage of our study patients had Hyperphosphatemia 61%. Retrospective cross-sectional studies suggested that a serum phosphate >6.5 mg/dl is associated with a 27% higher mortality risk compared in patients with serum phosphate level of 2.4-6.5 mg/dl and relative risk increases as serum phosphate level rises.
Conclusion
In the present study it was concluded that the prevalence of renal osteodystrophy was significantly increased. Secondary hyperparathyroidism (Osteitis Fibrosa Cystica) is the most common pattern of ROD followed by mixed osteodystrophy and adynamic bone disease.
Limitation
Our study had few major limitations. We depended completely on plasma PTH levels in our diagnosis of renal bone disease, which although is a good predictor of bone histology but not as accurate as bone biopsy. We did not measure serum 25-OH vitamin D and aluminum levels to exclude the possibility of Osteomalacia or aluminum toxicity.
References
- Ketteler M, Gross ML, Ritz E (2005) Calcification and cardiovascular problems in renal failure. Kidney Int Suppl: S120-S127.
- London GM, Marchais SJ, Guerin AP, Metivier F (2005) Arteriosclerosis, vascular calcifications and cardiovascular disease in uremia. Curr Opin Nephrol Hypertens 14: 525-531.
- Moe S, Drueke T, Cunningham J, Goodman W, Martin K, et al. (2006) Definition, evaluation and classification of renal osteodystrophy: a position statement from Kidney Disease: Improving Global Outcomes (KDIGO) Kidney Int 69: 1945-1953.
- Buargub MA, Nabulsi MF, Shafeh TA (2006) Prevalence and pattern of renal osteodystrophy in chronic hemodialysis patients: a cross sectional study of 103 patients. Saudi J Kidney Dis Transpl 17: 401- 407.
- Hernandez JD, Wesseling K, Salusky IB (2005) Role of parathyroid hormone and therapy with active vitamin D sterols in renal osteodystrophy. Semin Dial 18: 290-295.
- Afifi A (2002) Renal osteodystrophy in developing countries. Artif Organs 26: 767-769.
- Noordzij M, Korevaar JC, Boeschoten EW, Dekker FW, Bos WJ, et al. (2005) The kidney disease outcomes quality initiative (K/DOQI) guideline for bone metabolism and dsease in CKD: association with mortality in dialysis patients. Am J Kidney Dis 46: 925-932.
- Goodman WG (2005) The evolution of assays for parathyroid hormone. Semin Dial 18: 296-301.
- Rodriguez-Benot A, Martin-Malo A, Alvarez-Lara MA, Rodriguez M, Aljama P (2005) Mild hyperphosphatemia and mortality in hemodialysis patients. Am J Kidney Dis 46: 68-77.
- Mohammed IA, Hutchison AJ (2008) Phosphate binding therapy in dialysis patients: focus on lanthanum carbonate. Ther Clin Risk Manag 4: 887-893.
- Poon G (2005) Cinacalcet hydrochloride (Sensipar). Proc (Bayl Univ Med Cent) 18: 181-184.
- Santoso D, Yogiantoro M, Tomino Y (2003) Osteodystrophy in Indonesian haemodialysis patients. Nephrology (Carlton) 8: 261-265.
- Yonova D, Dukova P (2007) Changes of serum bone markers in CAPD and hemodialysis patients. Hippokratia 11: 199-201.
- Galea I, Farrugia E (2005) Biochemical indices of renal osteodystrophy in dialysis patients on the island of Malta. Int Urol Nephrol 37: 335-340.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi