Research Article, Jor Vol: 10 Issue: 4
The Importance of Ki-67, Ck-6 and Ck-16 Expression in the Evaluation of the Destructive Effect and Hyper Proliferative Capacity of Cholesteatoma
Taşdemir Aykut1, Gönüldaş Burhanettin1*, Erkılıç Suna2, Tunç Orhan1 and Kanlıkama Muzaffer1
1 Otorhinolaryngology Head and Neck Surgery, Gaziantep University, Gaziantep, Turkey
2 Pathology Department, Gaziantep University, Gaziantep, Turkey
*Corresponding Author: Burhanettin G
Department of Otolaryngology Head and Neck Surgery, Gaziantep, Turkey
Tel: 05059449825
E-mail: drburhanettin83@gmail.com
Received date: March 27, 2021; Accepted date: April 12, 2021; Published date: April 20, 2021
Citation: Aykut T, Burhanettin G , Suna E, Orhan T , Muzaffer K (2021) The Importance of Ki-67, Ck-6 and Ck-16 Expression in the Evaluation of the Destructive Effect and Hyper Proliferative Capacity of Cholesteatoma. J Otol Rhinol 10:4.
Abstract
Objective: Cholesteatoma, with its hyperproliferative feature and destructive pathogenesis, causes bone destruction of the middle ear structures and its surroundings. We aimed to investigate the expression of Ki-67, cytokeratin-6 (CK-6) and cytokeratin-16 (CK-16) in acquired and recurrent cholesteatoma and to correlate them with bone destructive capacity. Materials and Methods: The study was performed as a prospective immunohistochemical study using cholesteatoma tissue (n=45) and external auditory canal skin (n=10) collected during tympanoplasty operation. The findings were recorded considering whether the cholesteatoma was recurrent or not, the extent of cholesteatoma during the operation, ossicular damage and the presence of complications. The patients were divided into 4 groups: Complicated cholesteatoma, recurrent cholesteatoma, uncomplicated cholesteatoma and external auditory canal skin as the control group. Groups were compared in terms of Ki-67 expression level, CK-6 and CK-16 staining patterns. Results: In all groups with cholesteatoma, Ki-67 index was found to be significantly higher than the control group. In addition, the Ki-67 index was found to be significantly higher in the complicated and recurrent cholesteatoma groups compared to the uncomplicated group (p=0.015 and p=0.001, respectively). While CK-6 showed only suprabasal staining on the skin of the external auditory canal, it showed a full-coat staining pattern in cholesteatoma. When the groups with cholesteatoma were compared in terms of CK-16 staining pattern, the only significant result was higher full-thickness staining rates in the recurrent cholesteatoma group compared to the uncomplicated cholesteatoma group (p=0.022) Conclusion: Ki-67 index has been shown to be an important pathological parameter in evaluating the aggressive behavior of cholesteatoma. In addition, our study is the first to show the significant relationship of Ki-67 and CK-16 with recurrent cholesteatomas.
Keywords: Recurrent cholesteatoma; Complicated cholesteatoma; Cytokeratin-6; cytokeratin-16; Ki-67
Introduction
Cholesteatoma is defined as the abnormal presence of keratinized squamous epithelium in the middle ear cavity and other pneumatized areas of the temporal bone. Cholesteatoma, with its hyperproliferative and destructive properties, causes bone destruction of the middle ear structures and its surroundings. The ossicular chain and bone resorption of the otic capsule can cause hearing loss, vestibular dysfunction, facial paralysis and intracranial complications. There is no single cause of osteoporosis in cholesteatomas. Mechanisms such as pressure necrosis, chronic osteomyelitis, resorption with osteoclast, enzymatic reseorption, local pH changes, and vascular proliferation are thought to play a role in cholesteatoma-related bone resorption [1].
Cholesteatomas show similar features regardless of the underlying pathogenesis; hyperproliferation and differentiation with invasion, increased inflammation [2]. Normally there is a balance between cell proliferation and programmed cell death in keratinocytes. This balance is impaired in cholesteatoma and causes an increase in the accumulation of excessively proliferating epithelial keratin [3]. When the epithelium begins to hyperproliferate, the destructive process begins in cholesteatoma. Studies have been conducted on cytokeratin and Ki-67 to show the hyperproliferative properties of cholesteatoma [4,5].
Cholesteatoma, with its hyperproliferative potential, can lead to destruction in surrounding tissues and related complications, and may present with postoperative recurrences. However, complications do not occur in every patient with cholesteatoma. In this study, we aimed to investigate the expression of Ki-67, CK-6 and CK-16 in acquired cholesteatoma and to reveal the relationship of these markers with destruction and recurrence of cholesteatoma.
Materials and Methods
Facts
The study was conducted as a prospective immunohistochemical study by collecting cholesteatoma tissue (n=45) and external auditory canal skin (n=10) during tympanoplasty operation between February 2015 and September 2018. Ethics committee approval was obtained from the patients by providing information about the study.
During the operation, the extent of cholesteatoma, ossicular chain damage and the presence of complications were recorded. Patients with congenital cholesteatoma were not included in the study. In the study, patients were divided into four groups:
Complicated cholesteatoma (n=15): Patients with at least one clinical complication and findings of intraoperative complications.
Recurrent cholesteatoma (n=15): Patients with previous cholesteatoma surgery but recurrence of cholesteatoma.
Uncomplicated cholesteatoma (n=15): Cholesteatoma with one or more ossicular chain destruction but without complications.
Control group (n=10): The group whose external auditory canal epithelium was sampled from patients operated for chronic otitis media without cholesteatoma.
Immunohistochemical Examination and Evaluation
During the operation, tissue samples were taken for the study froups and placed in 10% formulation and sent to the Pathology Department for immunohistochemical analysis. After the samples taken from all groups were embedded in paraffin, 4 micron thick sections were obtained and placed on a poly-l-lysine coated lam. Lames were initially kept in the oven at 370C for 15 minutes, and then immunohistochemical staining was performed with Ki-67, CK-6 and CK-16 dyes on an automatic staining device (Ventana Bench Mark Ultra, SN:316054). After treatment with primary antibody, it was washed in tap water and covered with an ultra-amount. All samples were evaluated under a light microscope by the same pathologist and researcher. The pathologist and investigator were unaware of the clinical condition of the patients and the study groups during the evaluation of the samples, and the study thus gained a double-blind feature. 100 epithelial cells were counted by evaluating the 3 most stained areas at 200 magnifications under light microscopy and the number of positively stained epithelial cells was determined as the percentage of Ki-67 positive cells. CK-6 and CK-16 staining patterns were determined according to the stained epithelial layers (Figure 1).
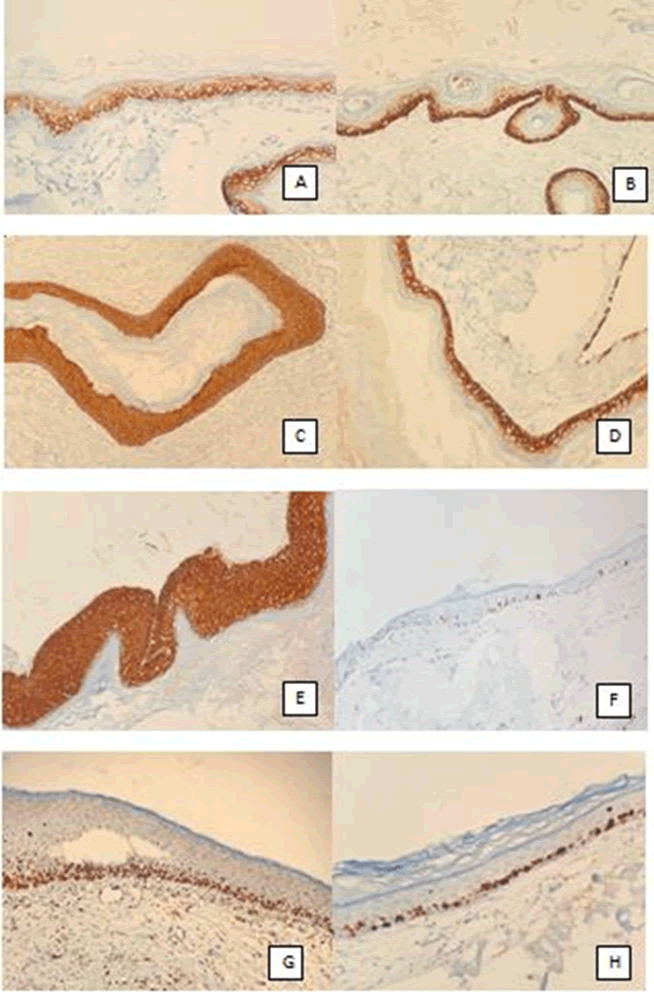
Figure 1: (A) Cholesteatoma and external auditory canal skin immunohistochemical staining. Suprabasal layer staining of the external auditory canal skin with CK-6. (B,C) Outer ear canal skin Basal-suprabasal layer staining with CK-16. (D) Basal strength, suprabasal pale staining. (E) Full coat staining of cholesteatoma with CK-16. (F) Staining of the outer ear canal skin with Ki-67. (G) Staining of recurrent cholesteatoma with Ki-67. (H) Staining of complicated cholesteatoma with Ki-67.
Statistical analysis
The compliance of numerical variables to normal distribution was tested with the Shaphiro-Wilk test. Student's t-test was used to compare variables that fit normal distribution in two groups, and ANOVA and LSD tests were used to compare three groups. Relationships between categorical variables were tested with the Chisquare test. SPSS 22.0 Windows version was used in the analysis. P<0.05 was considered significant.
Results
35 (63.6%) of the patients were male, 20 (36.4%) were female. The average age of the patients included in the study was 33.64 ± 15.61, and their ages ranged from 5-71, and the age distribution by groups was homogeneous.
In the complicated cholesteatoma group, 11 patients had a single complication, and 4 patients had multiple complications. LSSC fistula and facial paralysis were observed in 2 patients, otomastoidevtomy and LSSC fistula in 1 patient (Table 1).
| Complications | Number of cases |
|---|---|
| LSSC Fistula | 8 |
| Automastoidectomy | 4 |
| Fasial paralysis | 4 |
| Menengitis | 1 |
| Temporal Lobe abscess | 1 |
Table 1: Complication secondary to cholesteatoma.
Ki-67 positive staining percentages according to the groups are given in (Table 2). The Ki-67 index was significantly higher in the complicated cholesteatoma group compared to the uncomplicated cholesteatoma and the control group (p=0.015 and p=0.001, respectively). The Ki-67 index was also found to be significantly higher in the recurrent cholesteatoma group compared to the uncomplicated cholesteatoma and the control group (p=0.001 and p=0.001, respectively). The Ki-67 index was also found to be significantly higher in the uncomplicated cholesteatoma group compared to the control group (p=0.003). No significant difference was found between the complicated cholesteatoma and recurrent cholesteatoma group in terms of Ki-67 index (p=0.157)
| Groups | Ki-67 (%) |
|---|---|
| Complicated cholesteatoma(n=15) | 62.53 ± 17.36 |
| Recurrent cholesteatoma (n=15) | 71.20 ± 21.30 |
| Uncomplicated collesteatoma (n=15) | 47.40 ± 13.26 |
| Control group (n=10) | 26.30 ± 9.94 |
| Total (n=55) | 54.18 ± 22.68 |
Table 2: Percentage of Ki-67 positive staining by groups.
17 (37.8%) of the patients who were operated for chronic otitis media with cholesteatoma had canal wall up mastoidectomy and 28 (62.2%) had canal wall down mastoidectomy. The Ki-67 index was found to be significantly higher in patients who underwent cholesteatoma surgery with canal wall down compared to those with canal wall up (p=0.009) (Table 3).
| Groups | Ki-67 (%) |
|---|---|
| Canal wall down (n=28) | 66.25 ± 20.39 |
| Canal wall up (n=17) | 50.70 ± 15.00 |
Table 3: Ki-67 positive staining percentage according to surgical technique.
We found that CK-6 has different staining patterns in cholesteatoma and external auditory canal epithelium. CK-6 only had a suprabasal staining pattern in the external auditory canal epithelium of all patients in the control group. No staining was observed in the basal layer. In all patients with cholesteatoma, CK-6 has a full coat staining pattern.
We observed that all patients in the control group of CK-16 had basal and suprabasal staining patterns in the external auditory canal epithelium, but it showed pale staining in the suprabasal layer. We observed that 31 (68.89%) of the patients with cholesteatoma had full coat staining, and 14 (31.11%) had basal and suprabasal staining patterns.
When he froups with cholesteatoma were compared according to the CK-16 staining patterns, we found the only significant relationship between the recurrent cholesteatoma group and the group with uncomplicated cholesteatoma (p=0.022). When complicated cholesteatoma and recurrent cholesteatoma groups were compared in terms of CK-16 staining pattern, p=0.369; When the complicated cholesteatoma and uncomplicated cholesteatoma groups were compared, we obtained p=0.142 statistical value (Table 4).
| Groups | |||||
|---|---|---|---|---|---|
| Complicated cholesteatoma n (%) |
Recurrent cholesteatoma n (%) |
Uncomplicated cholesteatoma n (%) |
External auditory canal epithelium n (%) |
||
| CK-16 staining pattern | Basal-Suprabasal staining | 4 (26.7%) | 2 (13.3%) | 8 (53.3%) | 10(100%) |
| Full coat staining | 11 (73.3%) | 13 (86.7%) | 7 (46.7%) | 0 (0%) | |
Table 4: CK-16 staining pattern according to the groups.
When the relationship between the CK-16 staining pattern and the Ki-67 index was compared, the Ki-67 index of the full-coat stains was found to be significantly higher than the basal-suprabasal stains (p=0.001) (Table 5).
| Ki-67 (%) | ||
|---|---|---|
| CK-16 | Basal-Suprabasal staining (n=24) | 41.29 ± 20.39 |
| Staining pattern | Full coat staining (n=31) | 64.16 ± 19.26 |
Table 5: Percentage of positive Ki-67 staining according to CK-16 staining pattern.
Discussion
Ki-67 protein is a marker closely related to cellular proliferation. Since this protein is present in all active phases of the cell cycle susch as G1, S, G2 and mitosis, but not in the G0 phase, it is a unique marker in growing and proliferating cells [6]. In previos studies, it wasshown that there is a higher rate of Ki-67 expression in cholesteatoma epithelium compared to normal skin [7-10]. Although there are many literature studies stating that the Ki-67 index is high in cholesteatoma, there are few studies that contradict each other and explain the relationship between Ki-67 index and the destructive behavior of cholesteatoma [11-13]. It can be concluded that the difference in clinical parameters and methodological methods was effective in obtaining different results in these studies. One or more ossicular damage due to chronic inflammation can be seen in patients with chronic otitis media with discharge without cholesteatoma. This situation indicates that one or more ossicular damage is an insufficient parameter in evaluating the aggressiveness of cholesteatoma. Therefore, in our study, we defined cholesteatomas with one or more ossicular chain damage or causing damage in the attic as non-invasive group without complications. According to our experience, we also encounter dehiscences in the facial canal in patients operated for chronic otitis media without cholesteatoma. In an anatomical study conducted by Baxter [14], it was reported that 57% of people had dehiscence in the facial canal at the oval window level. In another study conducted by Moreano et al. [15] on 1000 temporal bones, dehiscence was found in at least one of the facial canals in 56% of the patients. In our study, we based on complications related to cholesteatoma to reveal the invasive character of cholesteatoma. We did not consider facial canal dehiscence alone as a complication. Because facial canal dehiscence alone may be a pre-existing anatomical defect independent of the disease, and accepting it as a complication will lead to a false positive evaluation. Therefore, we considered facial paralysis and facial canal dehiscence in contact with intraoperative cholesteatoma as a clinical complication. Other complications we included in the complicated cholesteatoma group were LSSC fistula, otomastoidectomy, temporal lobe abscess, and meningitis. The high Ki-67 index in cholesteatoma compared to the epithelium of the external auditory canal was consistent with previous studies. In addition, our study provides support that the Ki-67 index is an important pathological parameter in the aggressive behaviour of cholesteatoma. However, there are also factors that limit our study. The most important of these is the period from the onset of cholesteatoma to the emergence of complications. If the patients who are accepted as uncomplicated cholesteatoma are delayed in the diagnosis, it may appear as a complication in the future or does the aggressive behavior of cholesteatoma increase over time? Despite these uncertainties, our study is supported by both previous studies and statistically significant data we obtained.
Although cholesteatoma has been treated surgically, its recurrent nature poses a clinically important problem. Recurrence rates between 5% and 71% have been reported in the literature. The reason for the high difference between rates may be related to type of cholesteatoma, surgical technique, follow-up frequency, postoperative follow-up time and the statistical method applied [16]. In previous studies, no difference was found between recurrent and non-recurrent cholesteatomas at Ki-67 level [17,18]. In our study, contrary to the literature, we found a significantly higher Ki-67 index in recurrent cholesteatomas. We think that the inclusion of more patients in the study and the increase in the sample size and the more detailed grouping of the patients were effective in obtaining results in this way. This study is the first to provide evidence that Ki-67 index may be an important pathological parameter for recurrent cholesteatomas. We can collect recurrent cholesteatomas that develop after surgical treatment of cholesteatomas that develop after surgical treatment of cholesteatoma in two groups as residual and recurrent. Residual cholesteatoma is a cholesteatoma formed by the squamous epithelial tissue remaining in the middle ear. Recurrent cholesteatoma is the recurrence of cholesteatoma despite surgical removal. It is difficult to make a clear statement as to whether these are residual or recurrent cholesteatoma. However, the patients we operated for recurrent cholesteatoma had a canal wall down mastoidectomy in the previous surgery. Based on this, we think that the recurrent cases in our study were mostly recurrent cholesteatoma. Because the possibility of residual canal wall down mastoidectomy is low.
Cytokeratins are one of the most studied markers to reveal the hyperproliferative character of cholesteatoma epitheliumç the distribution of cytokeratins in the epithelium varies according to the cell type, growth, migrationand differentiation stage [19]. Vennix investigated the expression of a group of cytokeratin, including CK-6, CK-16 and CK-17 in cholesteatoma, and revealed different types of staining patterns in cholesteatoma [20]. In our study, we observed that CK-6 showed only suprabasal staining patterns in the epithelium of the external auditory canal, in accordance with the literature. CK-6 expression was not observed in the basal layer. In all patients with cholesteatoma, CK-6 showed a full-coat staining pattern. We found that CK-6 expression, which is a marker associated with hyperproliferation, was increased in cholesteatoma. This result reflects the hyperproliferative behavior of cholesteatoma showed that this marker was not related to the aggressive behavior of cholesteatoma. In our study, CK-16 showed basal-suprabasal staining in the epithelium of the external auditory canal and stained the suprabasal layer pale. We observed that 31 (68.89%) of the patients with cholesteatoma had full-coat staining and 14 (31.11%) had a basal-suprabasal staining pattern. When we compared the relationship between the CK-16 staining pattern and the Ki-67 index, the Ki-67 index of the full-coat stains was found to be significantly higher than the basal-suprabasal stains (p=0.001). We have supported that cholesteatoma has a hyperproliferative character with a positive correlation between the CK-16 staining pattern and the Ki-67 index. When the groups with cholesteatoma were compared in terms of CK-16 staining pattern, the only significant result was a higher rate of full-coat staining patterns in the recurrent cholesteatoma group than the uncomplicated cholesteatoma group (p=0.022). In this study, we provided support proving that CK-16 is a parameter that can be used in the differentiation of recurrent cholesteatomas from non-recurrent cholesteatomas. On the other hand, although the CK-16 staining pattern did not show a statistically significant difference between the complicated cholesteatoma group and the uncomplicated cholesteatoma group, a higher rate of full-thickness staining was observed in the complicated group. Although CK-16 is a hyperproliferative marker, it alone cannot explain the aggressive behavior of cholesteatoma. In our study, we divided the patients operated for cholesteatoma into two groups as surgical technique: Canal wall down and canal wall up. Ki-67 index was found to be significantly higher in patients who underwent cholesteatoma surgery with canal wall down compared to those performed with canal wall up. Although the surgical technique chosen affects the quality of life, this result supports that we make a more accurate surgical technique decision intraoperatively compared to the prevalence of cholesteatoma.
Conclusion
We have shown that Ki-67 index and CK-16 staining pattern are usable parameters in terms of follow-up and prognosis of patients with cholesteatoma. It has been shown that Ki-67 index is an important pathological parameter in evaluating the aggressive behavior of cholesteatoma. In addition, our study is the first study showing the significant relationship of Ki-67 and CK-16 with recurrent cholesteatomas.
References
- Sade J (1987) Treatment of cholesteatoma. Am J Otol 8: 524-533.
- Olszewska E, Wagner M, Bernal-Sprekelsen M, Ebmeyer J, Dazert S, et al. (2004) Etiopathogenesis of cholesteatoma. Eur Arch Otorhinolaryngol 1: 6-24.
- Huisman MA, De Heer E, Grote JJ (2003) Cholesteatoma epithelium is characterized by increased expression of Ki-67, p53 and p21, with minimal apopitosis. Acta Otolaryngol 123: 377-82.
- J. Bujía, Sudhoff H, Holly A, Hildmann H, Kastenbauer E, et al. (1996) Immunohistochemical detection of proliferating cell nuclear antigen middle ear cholesteatoma. Eur Arch Otorhinolaryngol 253: 21-4.
- Olszewska E, Lautermann J, Koc C, Schwaab M, Dezert, et al. ( 2005) Cytokeratin expression pattern in congenital and acquired pediatric cholesteatoma. Eur Arch Otorhinolaryngol 262: 731-36.
- Oijen MG, Medema RH, Slootweg PJ, Rijksen G (1998) Positivity of the proliferation marker Ki-67 in noncycling cells. Am J Clin Pathol 110: 24–31.
- Bujia J, Holly A, Sudhoff H, Antoli-Candela F, Tapia MG, et al. (1996) Identification of proliferating keratinocytes in middle ear cholesteatoma using the monoclonal antibody Ki-67. ORL J Otorhinolaryngol Relat Spec 58: 23-6.
- Olszewska E, Chodynicki S, Chyczewski L, Rogowski M (2006) Some markers of proliferative activity in cholesteatoma epithelium in adults. Med Sci Monit 12: 337-40.
- Olszewska E, Chodynicki S, Chyczewski L, Rogowski M (2006) Some markers of proliferative activity in cholesteatoma epithelium in adults. Med Sci Monit 12: 337-40.
- Chae SW, Song JJ, Suh HK, Jung HH, Lim HH, et al. (2000) Expression patterns of p27kip1 and ki-67 in cholesteatoma epitelium. Laryngoscope 110:1898-1901.
- Sudhoff H, Bujia J, Fisseler-Eckhoff A, Schulz-Flake C, Holly A, et al. (1995) Expression of the cell cycle related antijen (MIB-1) in cholesteatoma and auditory meatal skin. Laryngoscope 105: 1227-1231.
- Chae SW, Song JJ, Suh HK, Jung HH, Lim HH, et al. (2000) Expression patterns of p27kip1 and ki-67 in cholesteatoma epitelium. Laryngoscope 110:1898-1901
- Hamed MA, Nakata S (2017) Cytokeratin 13, Cytokeratin 17, and Ki-67 expression in human acquired cholesteatoma and their correlation with its destructive capacity. lin Exp Otorhinolaryngol 10: 213-220.
- Baxter A (1971) Dehiscence of the Fallopian canal. An anatomical study. J Laryngol Otol 85: 587-94.
- Mallet Y, Nouwen J, Lecomte-Houcke M, Desaulty A (2003) Aggressiveness and quantification of epithelial proliferation of middle ear cholesteatoma by MIB1. Laryngoscope 113: 328-331
- Akdoğan V, Yılmaz I, Canpolat T, Ozluoglu LN (2013) Role of langerhans cells, Ki-67 protein and apoptosis in acquired cholesteatoma: prospective clinical study. J Laryngol Otol 127: 252–259
- Choufani G, Mahillon V, Decaestecker C, et al. (1999) Determination of the levels of expression of sarcolectin and calcyclin and of the percentages of apoptotic but not proliferating cells to enable distinction between recurrent and nonrecurrent cholesteatoma. Laryngoscope 109: 1825–1831.
- Şanlı A, Tezer İ, Paksoy M, Aydın S, Hardal Ü, et al. (2007) Tekrarlayan kolesteatomlu olgularda Ki-67 ekspresyonunun değerlendirilmesi. Kulak Burun Bogaz Ihtis Derg 17: 65-69
- Olszewska E, Sudhoff H (2007) Comparative cytokeratin distribution patterns in cholesteatoma epithelium. Histol Histopathol 22: 37-42.
- Vennix PP, Kuijpers W, Peters TA, Tonnaer EL, Ramaekers FC, et al. ( 1996) Keratinocyte differentiation in acquired cholesteatoma and perforated tympanic membranes. Arch Otolaryngol Head Neck Surg Aug 122: 825-832.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi