Case Report, Biomater Med Appl Vol: 2 Issue: 2
A New Titanium System to Help Spinal Surgeon
Iñaki Arrotegui*
Department of Neurosurgery, Hospital General Universitario de Valencia, Valencia-Spain
*Corresponding Author : Dr. Iñaki Arrotegui
Department of Neurosurgery, Hospital General Universitario de Valencia, Valencia-Spain
Tel: 00-34-627492961
E-mail: athbio@yahoo.es
Received: April 05, 2018 Accepted: May 22, 2018 Published: May 28, 2018
Citation: Arrotegui I (2018) A New Titanium System to Help Spinal Surgeon. Biomater Med Appl 2:2. doi: 10.4172/2577-0268.1000116
Abstract
We made a brief review on the indications of lumbar arthrodesis throughout its evolution during the last years, as well as the use of a new system that facilitates the closing time of the system that favors the decrease of the surgery time.
Keywords: Biomaterials; Implants
Introduction
By performing a level arthrodesis of the lumbar region allows us to restore stability or correct the alignment of the vertebrae in cases where there is an alteration, either by degenerative, congenital or traumatic processes [1]. The realization of this fixation will be carried out by placing transpedicular screws, which are inserted into the vertebrae through the pedicle (portion that connects the anterior part (body) and the posterior part (arch) of the vertebra). This route allows you to obtain a good anchor point to achieve the desired correction
In other cases intersomatic boxes will be associated, a kind of wedges that are placed between the vertebrae. These will allow another point of support, while providing greater stability to the column. Although these are the most frequent methods that exist many others, such as interspinous devices, screws for lateral masses, laminar screws, among others. It consists of the fastening of two or more vertebrae by fusion (welding) of your bone [2].
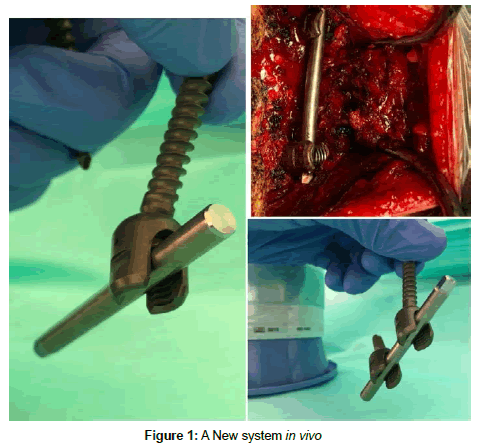
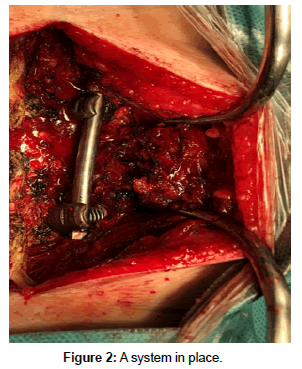
It is a surgical option in cases of spinal instability, isthmic and/ or degenerative spondylolisthesis, facet arthropathy, postoperative instability, disc hernia recurrence and degenerative scoliosis. The common denominator of many of these conditions is the segmental instability of the spine, defined as the loss or reduction of the mechanical integrity of a mobile segment of the spine, manifested by pain or neurological symptoms when loads are applied. The main objective of spinal lumbar arthrodesis is to minimize or eliminate mobility by increasing the load capacity of the injured mobile segment. With this new arthrodesis system as shown in the Figure 1, the bar is placed and is perfectly subject, without any restriction, with the lordosis perfectly preserved. Likewise, the head of the screw allows the positioning of the fixing nut in a simple way, decreasing the closing time of the system (Figure 2).
History
From the beginning of the last century, these interventions were carried out, which required the placement of bone grafts from the patient himself at the level of the back of the vertebrae, once the muscles had been carefully removed. The problem was that the patient had to remain in bed for six months in a plaster bed to reduce mobility and thus allow the consolidation (fusion) of the bone grafts. To avoid the long bed period and increase the success rate of bone fusion, in the 60s it started in Europe and especially in France, to place screws in the peduncular level of the vertebrae, which were connected to each other through bars or plates. Over time, the type of screw has evolved (the first ones broke frequently) and the type of bars (now there are no plates and there are elastic bars to allow some mobility). However, the problem remained that to place the screws, the rods and the grafts, large incisions had to be made and devascularization and denervation of large portions of the spinal musculature had to be removed. The postoperative period, it was very heavy and long, largely due to the damage inflicted on the muscles by the surgical approach [3].
In order to reduce the damage to the muscle mass and achieve a faster and more complete recovery, they began to apply minimally invasive methods.
Surgery Techniques
In the spine they have allowed the reduction of the size of the incisions (which already began when the microscope, the endoscope and the percutaneous techniques were introduced with laser or with nucleotomy) and the reduction of the damage to the Para-spinal muscular masses [4]. Among these new techniques, percutaneous Posterolateral lumbar arthrodesis stands out. Through incisions of just over 1 cm for each screw, it is possible to instrument large areas of the spine. The result has been a more rapid recovery, a reduction in the need to transfuse blood, a reduction in hospital admission and costs, and an earlier reincorporation to work.
Technique
Two screws are placed per vertebra to be fused, one on each side of the vertebra, which will later serve as an anchor to the titanium rods that will join one vertebra with the other, avoiding movement while the fusion takes place over several months. In addition, graft previously extracted from the body of the patient, corpse or artificial substitutes of bone that will favor the fusion of the vertebrae may be provided.
Incision in the skin and separation muscles: The entire musculature of the vertebrae is detached. The surface of the bone is lifted or revived by means of a chisel; this will favor that after the contribution of the graft the fusion takes place. The screws are connected to each other with a bar on each side of the vertebra and special hooks. It is screwed by locking the bar to the screws. Graft contribution that will favor the fusion process, in this case it is used extracted from the patient.
Suture of the skin: The neurosurgeon will indicate the fixation of the spine in cases where it is necessary to correct the curvature of the spine (balance), in cases where there is instability of the spine (excessive displacement of one vertebra with respect to the other) or when we anticipate instability secondary to a surgical maneuver, such as surgery for canal stenosis.
Fixation will be the norm in herniated disc surgery in the cervical spine, since it has been shown that simple discectomy involves the appearance of a cervical kyphosis (change of the curvature of the spine) in 5-10 years, which is associated with a clinical deterioration [5].
Benefits of column fixation for the patient, the benefits come from the recovery of the stability of the spine. The lumbar instability initially causes lumbar contractures, and may appear difficulties in ambulation, in the most severe cases, in which there may be a nervous entrapment secondary to this instability. Regarding the alteration of the balance, the situation is similar; when the spine works in an unfavorable alignment it causes an early muscular fatigue that, likewise, ends up causing contractures, fatigue and pain [6]. In cases of advanced discopathy we will need intersomatic boxes to recover the height lost secondary to the discopathy.
Results
A Mayo Clinic study found that the best results were seen in patients with degenerative disc disease, followed by patients with spondylolisthesis and finally patients who had received a prior discectomy [5]. Possible risks of fixation of the spine.
The main risk of lumbar arthrodesis is associated with the neurological injury that can occur when inserting the fusion material (fixation) Transpedicular screw, which contacts the nerve root and a neurological symptoms appears.
That is why neurosurgeons use radiological methods to control the location of the implanted material at all times, whether by X-ray, intraoperative CT or neuronavigation systems. They also have intraoperative monitoring systems to verify the correct location of the system once it is implanted. For them a small current is applied to the fixation and, depending on the response obtained, it will be known how close the system of arthrodesis of the nerve roots is.
Other complications of any surgery, such as infection or hemorrhage, should be considered. To avoid them, antibiotic prophylaxis is established before surgery and careful hemostasis is performed during surgery. Indications to be followed by the patient submitted to the fixation of the spine: After the surgery, whenever possible, early mobilization is established. This initial ambulation must be prudent. The objective during the first month is not to recover muscle tone but to let the muscles heal and avoid complications in the arthrodesis system, which can appear when subjected to excessive tension when it is not yet integrated into the bone. 3 to 4 weeks, a mild rehabilitation treatment will begin, which will normally last a month. During this time, it is advisable to avoid physical efforts, especially the load weights (3 kg) [6].
Once this period has elapsed, it will be important to maintain a good muscle tone, so it is recommended to perform physical activities, avoiding impact (running) and rotation (golf) and, especially, the combination of them (squash). Toning the abdominal and lumbar musculature is of vital importance in patients with lumbar pathology.
The muscles are the cables that support the spine and, the better the tone of the spine, the lower the load that the joints, bones and ligaments must bear.
Conclusion
This new system comes to join the large number of existing, its advantages, the bar is always in lordotic position, and also the rapid closure of the system facilitates a shorter surgical time, so important in post-operative recovery, decreasing the hospital stay.
References
- Aygun H, Cakar A, Huseyinoglu N, Huseyinoglu U, Celik R (2014) Clinical and radiological comparison of posterolateral fusion and posterior interbody fusion techniques for multilevel lumbar spinal stabilization in manual workers. Asian Spine J 8: 571-580.
- Pawar AY, Hughes AP, Sama AA, Girardi FP, Lebl DR, et al. (2015) A comparative study of lateral lumbar interbody fusion and posterior lumbar interbody fusion in degenerative lumbar spondylolisthesis. Asian Spine J 9: 668-674.
- Booth KC, Bridwell KH, Eisenberg BA, Baldus CR, Lenke LG (1999) Minimum 5-year results of degenerative spondylolisthesis treated with decompression and instrumented posterior fusion. Spine 24: 1721-1727.
- Boos N, Marchesi D, Zuber K, Aebi M (1993) Treatment of severe spondylolisthesis by reduction and pedicular fixation a 4-6-year follow-up study. Spine (Phila Pa 1976) 18: 1655-1661.
- Sudprasert W, Choovongkomol K, Piyapromdee U, Leownorasate M (2016) Impact on neurological recovery of transforaminal debridement and interbody fusion versus transpedicular decompression in combination with pedicle screw instrumentation for treating thoracic and lumbar spinal tuberculosis. Asian Spine J 10: 543-552.
- Zhao FD, Yang W, Shan Z (2012) Cage migration after transforaminal lumbar interbody fusion and factors related to it. Orthop Surg 4: 227-232.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi