Case Report, Clin Dermatol Res J Vol: 2 Issue: 2
A Vascular Surgeon Should Know What Eritema AB IGNE IS: Case Report
Emine Şeyma Denli yalvac*, Mustafa Aldag, Cemal Kocaaslan and Ebuzer Aydin
Department of Cardiovascular Surgery, Faculty of Medicine, Medeniyet University, Istanbul, Turkey
*Corresponding Author : Emine Seyma Denli Yalvac
Department of Cardiovascular Surgery, Faculty of Medicine, Medeniyet University, Istanbul, Turkey
Tel: 9050570000
E-mail: drseymadenli@yahoo.com
Received: August 01, 2017 Accepted: August 16, 2017 Published: August 22, 2017
Citation: Yalvac ESD, Aldag M, Kocaaslan C, Aydin E (2017) A Vascular Surgeon Should Know What Eritema AB IGNE IS: Case Report . Clin Dermatol Res J 2:2.
Abstract
Erythema Ab IGNE (EAI) has been characterized as asymptomaticlocalized area of reticulated erythema and hyperpigmentation due to chronic and prolonged exposure to heat at relative lower temperatures. Patients with EAI think that the disease is caused by circulatory disorder. Therefore, these patients are frequently referred to the vascular surgery polyclinic. The diagnosis of this disease can be made with a simple physical examination and anamnesis. The treatment is to get away from the exposure of the
agent. Although EAI is common and the treatment is very easy, the diagnosis can be challenging for vascular surgeons due to the lack of familiarity. So in this article, a 29-year-old male with EAI has been presented to remind the vascular surgeon of this disease in context of current literature information.
Keywords: Erythema Ab IGNE; Heater; Vascular surgeon
Introduction
Erythema Ab IGNE (EAI) is a heat-dependent dermatosis due to the frequent use of electronic devices and close contact to heaters [1]. Temperature changes between 43-47 °C may cause Erythema Ab IGNE. When electronic devices and heat exposure are introduced repetitively in contact with the body and damag the superficial blood vessels, the lesion turns into permanent, non-blanchable reddishbrown hyperpigmentation and hemosiderin accumulation causes reticular distribution [2,3]. EAI is easy to diagnose based on amnesis. Since histopathological findings are usually non-specific, skin biopsies are recommended to exclude other differential diagnoses such as cutaneous vasculitis. It is usually asymptomatic, but patients may have skin burning, fever or itching complaints. Initial treatment for EAI involves stopping the contact to heat source and electronic devices. If healing is achieved, the pigmentation abnormality may disappear very quickly. When lesions are visually irritating, topical retinoid with or without topical steroids and 5-fluorouracil cream can be used [4]. Although EAI carries a favorable prognosis, due to which squamous cell carcinoma and Merkel cell carcinoma can arise within lesions of EAI [5,6]. In this article we present a case of heat deviceinduced EAI in a 29-year-old male with current literature.
Case Report
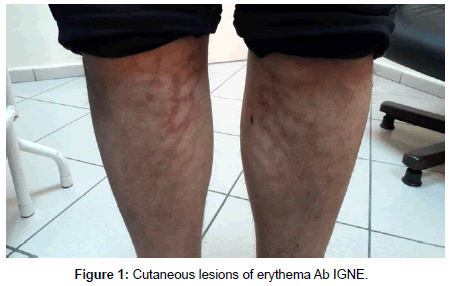
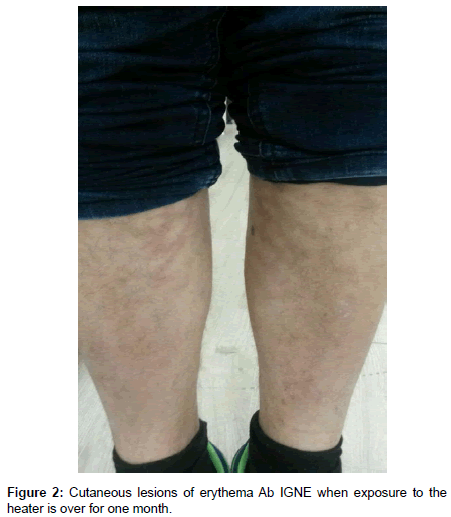
A 29-year-old male was admitted to the clinic complaining redbrown rashes below knees (Figure 1). Similar lesions were not found elsewhere in the body. His vascular examination was normal. After detailed anamnesis, he explained that he had close contact with heater in recent months to warm up to normalize his body temperature. EAI was diagnosed so he was recommended to stay away from heaters without medical treatment. He was informed that the existing stains on him may disappear spontaneously. A skin biopsy was not required. At a month’s follow-up, a noticeable improvement in the patient’s skin was observed (Figure 2).
Discussion
EAI is associated to excessive exposure to heat due to electronic devices or heaters. It is important to know the anamnesis of heat exposure through a detailed questioning. Patients may notice late because lesions are developing slowly. Most of the EAI cases triggered by the use of the heater occur in the lower knee regions. It is enough to move away from the heat source in order for the lesion to disappear spontaneously [7]. If exposure to heat continues, the lesions can become permanent [8]. Patients usually think that this is a vascular disease. For this reason, patients come to vascular surgery centers. A vascular surgeon makes sure patients with EAI. All heaters should not contact our body for a long time. EAI is avoidable. Patients applying for evaluation of lesions in the lower knee regions should be asked whether they have use heater or not in the past.
Conflict of Interests
The authors have no conflict of interests regarding this work.
References
- Levinbook WS, Mallett J, Grant-Kels JM (2007) Laptop computer–Associated erythema Ab IGNE. Cutis 80: 319-320.
- Riahi RR, Cohen PR (2012) Laptop-induced erythema Ab IGNE: Report and review of literature. Dermatol Online J 18: 5.
- Botten D, Langley RG, Webb A (2010) Academic branding: erythema ab iğne and use of laptop computers. CMAJ 182: E857
- Poustinchian BR, Pohlman DJ (2010) Erythema Ab IGNE. J Am Osteopath Assoc 112: 808
- Wharton JB, Sheehan DJ, Lesher JL (2008) Squamous cell carcinoma in situ arising in the setting of erythema Ab IGNE. J Drugs Dermatol 7: 488-489.
- Hewitt JB, Sherif A, Kerr KM, Stankler L (1993) Merkel cell and squamous cell carsinomas arising in erythema Ab IGNE. Br J Dermatology1993; 128: 591-592.
- Dvoretzky I, Silverman NR (1991) Reticular erythema of the lower back. Erythema Ab IGNE. Arch Dermatol 127: 405-409.
- Finlayson GR, Sams WM, Smith JG (1966) Erythema Ab IGNE: a histopathological study. J Invest Dermatol 46: 104-108.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi