Case Report, Clin Oncol Case Rep Vol: 5 Issue: 4
Case Report: Steven Johnson Syndrome/Toxic Epidermal Necrolysis (SJS/TEN) in a Patient with Carcinoma Breast Complicated By Sars-Cov2, Covid-19
Ashok Kumar1*, Manish Kumar2, Bhanu Pratap1, and Nihanty Das2
1Department of Radiation Oncology, Army Hospital (R&R), Delhi Cantonment, New Delhi, India
2Department of Medical Oncology, Army Hospital (R&R), Delhi Cantonment, New Delhi, India
*Corresponding Author: Ashok Kumar
Department of Radiation Oncology, Army Hospital (R&R), Delhi Cantonment, New Delhi, India
E-mail: ashokchand75@rediffmail.com
Received: March 16, 2022; Manuscript No: COCR-22-57432;
Editor Assigned: March 18, 2022; PreQC Id: COCR-22-57432(PQ)
Reviewed: April 05, 2022; QC No: COCR-22-57432(Q);
Revised: April 07, 2022; Manuscript No: COCR-22- 57432(R);
Published: April 15, 2022; DOI: 10.4172/cocr.5(4).228
Citation: Kumar A, Kumar M, Pratap B, Das N. (2022) Case Report: Steven Johnson Syndrome/Toxic Epidermal Necrolysis (SJS/TEN) in a Patient with Carcinoma Breast Complicated By Sars-Cov-2, Covid-19. Clin Oncol Case Rep 5:4
Abstract
Toxic epidermal necrolysis (TEN) and Stevens-Johnson syndrome (SJS) present with extensive epidermal detachment of the skin and mucous membranes as well as systemic involvement. Drug hypersensitivity is the major culprit for TEN/SJS and viral infections such as COVID-19 might also induce SJS/TEN. Drug eruptions are often clinically indistinguishable from viral infections. Here we present a case who reported with SJS/TEN syndrome after taking medications for COVID-19. She was a 70 yr old lady diagnosed and being treated carcinoma breast. She contracted COVID-19 infection and her treatment had to be withheld . She took medications for COVID-19 and later developed SJS/TEN syndrome with pruritic maculopapular rashes involving entire body.
Keywords: Covid-19 , SJS/TEN syndrome, Carcinoma breast
Introduction
Toxic Epidermal Necrolysis (TEN) and Stevens-Johnson Syndrome (SJS) present with extensive epidermal detachment of the skin and mucous membranes as well as systemic involvement [1]. Drug hypersensitivity is the major culprit for SJS/TEN. Other causes of SJS/TEN are mycoplasma pneumonia infection, vaccinations, acute graft-vs-host disease and Systemic Lupus Erythematosus (SLE). Most commonly drugs implicated are lamotrigine, carbamazepine, allopurinol, sulphonamides, and nevirapine. Risk factors also include HIV/AIDS and prior studies have reported a rare primary presentation of SLE as SJS/TEN, which is defined as a new clinical entity (SJS/TENlike lupus erythematosus). Viral infections such as COVID-19 might also induce SJS [2,3].
Most common presentation of SJS are fever, sore throat and fatigue and also include burning of eyes for 2 to 3 days. Patients may also experience burning pain of their skin at the start of the disease. Ulceration of mucous membranes in mouth and genital areas also appear within days of presentation [4]. Rashes on face, trunk, arms and legs and soles of feet are also present. Drug eruptions are often clinically indistinguishable from viral infections. Although there is no meticulous guidelines for treating SJS/TEN like LE, IVIg has been reported as an efficient treatment. We report an unusual case of SJS/ TEN syndrome post covid infection.
Case Presentation
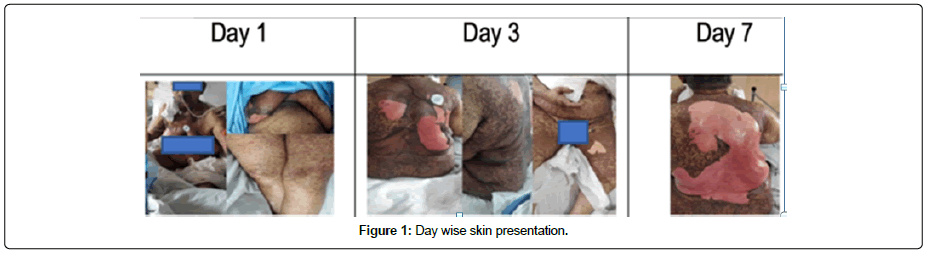
70 years old lady, case of Carcinoma Right Breast (Optd) cT2N0M0, Post BCS, hormone positive with comorbidity of Hypertension presented in Aug 2020 with painless lump in right breast and was treated with neoadjuvant chemotherapy (in view of COVID 19 pandemic and risk of infection patient and relatives did not want to come for daily radiotherapy treatment to the hospital and hence chose to take neo-adjuvant chemotherapy) and breast conserving surgery and was presently on adjuvant radiation. During the course of radiotherapy she presented with fever and cough and was tested positive for COVID-19. She took online consultation and was advised Tab Defcort 6 mg BD, Tab Doxycycline 100 mg BD, Tab Montelukast +Fexofenadine HS, Tab Ecosprin 75 mg, Tab Pantoprazole 40 mg OD, Tab Ivermectin 12 mg OD, Tab VIT-C 500 mg OD, Tab Zinc 50 mg BD and Tab Dolo 650 mg SOS. She took these medications for five days following which she developed skin lesion along-with difficulty in swallowing. She was diagnosed as a case of adverse drug reaction and was given Tab Loratidine 10 mg OD, Tab Allegra 120 mg OD, Clotrimazole mouth paint LA, Tab Fluconazole 150 mg Once daily. Her symptoms continued to progress with increase of maculopapular rashes all over the body with mucosal erosions in mouth. She reported to the hospital after eleven days with complaints of fever, difficulty in swallowing, mouth ulcers, poor oral intake, red raised painful lesions all over the body which progressed to form blisters along with peeling of skin. On evaluation she was in ECOG PS-2, conscious, oriented. GCS-E4V5M6. Dermatological examination was suggestive of diffuse maculo-papular erythematous dusky red, tender rash involving whole body with peeling at B/L infra mammary areas (BSA-5%-8%), Nikolsky sign positive, involvement of oral mucosa in the form of crusted erosions and ulceration ,involvement of B/L conjunctiva in the form of erosions. Total body surface area involved was almost 70% (Figure 1). Her SCORTEN was evaluated using age, malignancy, pulse rate, body surface area peeling, blood sugar random, Sr bicarbonate levels and BUN, the final value came to 04 (Table 1). On the basis of evaluation and history the most likely culprit drug considered was either doxycycline or ivermectin since all other drugs were ruled out as cause for SJS/TEN. Due to the COVID-19 epidemic, no skin biopsies were taken. However, the clinical manifestations were highly compelling for SJS/ TEN. She was started on IV Fluids, IV IG (@2 gm/kg) at the dose of 80 g on day 1 and 60 gm on day 2 and 3 and IV Antibiotics. However, her condition continued to deteriorate and she developed tachypnoea and tachycardia and was shifted to ICU. Her haematological profile was suggestive of sepsis along with super-added infections. After a week of admission in the hospital and due to respiratory fatigue patient was prophylactically intubated and was placed on ionotropic support and amidarone infusion, Inj Hydrocortisone and low molecular weight heparin. In spite of best possible efforts of the entire critical care team she finally succumbed to her illness after 23 days of contracting COVID-19 infection.
Table 1. Calculation of severity of illness score for toxic epidermal necrolysis (SCORTEN) in our patient.
| Risk factor | Score | Patient score | |
|---|---|---|---|
| 0 | 1 | ||
| Age | <40 yrs. | >40 yrs. | 1 |
| Associated malignancy | No | Yes | 1 |
| Heart rate (beats / min) | <120 | >120 | 1 |
| Serum urea (mg/dl)(mmol/L) | <28(10) | >28(10) | 0 |
| Detached / compromised body surface area | <10% | >10% | 1 |
| Sr Bicarbonate levels (mEq/L) | >20 | <20 | 0 |
| Sr Glucose (mg/dl) (mmol/L) | <250(14) | >250(14) | 0 |
| Total | 4 | ||
Discussion
The international outbreak of respiratory illness SARS-COV2, Coronavirus 2019 (COVID-19) began in December 2019 and was declared as pandemic in the 51st World Health Organization Status Report on 11 March 2020 [5]. COVID-19 is caused by SARSCoV- 2 and can be a potentially fatal disease [6]. The most common symptoms are fever, cough, and fatigue, followed by dyspnea and diarrhea [7]. Lymphopenia, elevation of Creatinine Kinase (CK), Lactate Dehydrogenase (LDH) are also frequently observed. The lung involvement is frequently that of an interstitial pneumonia [8]. Presently, there is no effective cure for COVID- 19 and several drugs often in combination have been used.
The SJS is a rare immune complex-mediated hypersensitivity disorder with incidence of 1-2 cases/1,000,000 annually and is generally described as vesiculobullous erythema multiforme of the skin, mouth, eyes, and genitals [9]. Medications appear to be the most common cause of SJS [10]. SJS can be preceded by a prodrome of fever, malaise, sore throat, nausea, vomiting, arthralgias, and myalgias followed by conjunctivitis, in addition to bullae on the skin and mucosal membranes of the mouth, nares, pharynx, esophagus, urethra, genital and anal regions [10]. SJS/TEN presents as a delayed reaction occurring after 4-28 days from drug exposure, therefore it is of paramount importance to acquire precise retrospective pharmacological information preceding the onset of skin manifestations.
COVID-19 is an emerging disease that currently has no specific treatment, and the treatments are purely supportive. The drugs as mentioned for the management of Covid-19 have recently shown adverse reactions of which SJS/TEN syndrome has been also been reported. Of the above chloroquine has been implicated in drug eruptions leading to SJS/TEN syndrome. There is a desperate need to identify effective treatments for COVID-19 and most drugs currently explored in this pandemic are repurposed antiviral and immunomodulatory drugs. Adverse drug reactions, when encountered, add an additional level of complexity to the management of patients with COVID-19.
Conclusion
In our patient the most common offending drug could have been either doxycycline or ivermectin, however, it cannot be said with certainty. Also due to the pandemic the skin biopsy was difficult to be taken and despite all the available management strategies for SJS/TEN patient was lost due to superadded infections and postcovid complications associated with multiple lesions all over the body including oral ulcerations. In conclusion, skin and mucosal susceptibility to drugs may be increased in patients with COVID-19. It is possible that the risk of developing SJS is significantly increased in this category of patients as they might have a lowered capacity to detoxify reactive intermediate drug metabolites.
References
- Caproni M, Torchia D, Schincaglia E, Volpi W, Frezzolini A, et al. (2006) Expression of cytokines and chemokine receptors in the cutaneous lesions of erythema multiforme and Stevens-Johnson syndrome/toxic epidermal necrolysis. B J Dermatol 155: 722-728.
Google Scholar Cross Ref - Wollina U, Karadağ AS, Rowland‐Payne C, Chiriac A, and Lotti T (2020) Cutaneous signs in COVID‐19 patients: a review. Dermatol Therapy 33: 13549.
Google Scholar Cross Ref - De Giorgi V, Recalcati S, Jia Z, Chong W, Ding R, et al. (2020) Cutaneous manifestations related to coronavirus disease 2019 (COVID-19): A prospective study from China and Italy. J Am Acad Dermatol 83: 674-675.
Google Scholar Cross Ref - Hötzenecker W, Prins C, French LE. Erythema Multiforme, Stevens–Johnson Syndrome, and Toxic Epidermal Necrolysis. In: Bolognia JL, ed. Dermatology. 4th edn. Elsevier Limited, 2019: 332–47.
- Zu ZY, Jiang MD, Xu PP, Chen W, Ni QQ, et al. (2020) Coronavirus disease 2019 (COVID-19): A perspective from China. Radiology 296: 15-25.
Google Scholar Cross Ref - Rothan HA, Byrareddy SN (2020) The epidemiology and pathogenesis of coronavirus disease (COVID-19) outbreak. J Autoimmun 109: 102433.
Google Scholar Cross Ref - Huang C, Yeming W, Xingwang L, Lili R, Jianping Z, et al. (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395: 497-506.
Google Scholar Cross Ref - Stebbing J, Phelan A, Griffin I, Tucker C, Oechsle O, et al. (2020) COVID-19: combining antiviral and anti-inflammatory treatments. Lancet Infec Dis 20: 400-402.
Google Scholar Cross Ref - Wong KC, Kennedy PJ, Lee S (1999) Clinical manifestations and outcomes in 17 cases of Stevens- Johnson syndrome and toxic epidermal necrolysis. Australas J Dermatol 40: 131-134.
Google Scholar Cross Ref - Wolkenstein P, Revuz J (1995) Drug-induced severe skin reactions. Incidence, management and prevention. Drug Saf 13: 56-68.
Google Scholar Cross Ref
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi