Case Report, Clin Oncol Case Rep Vol: 5 Issue: 5
Cyclophosphamide, Bortezomib and Dexamethasone (CyBordD) for Multiple Extramedullary Plasmacytomas and Bilateral Myelomatous Pleural Effusion
Leilei Teng, Jennifer R Hewlett, and Khalil I Hussein
Department of Medicine, Greenwich Hospital, Yale New Haven Health System, Greenwich, CT, United States
*Corresponding Author: Khalil I Hussein
Department of Medicine, Greenwich
Hospital, Yale New Haven Health System, 5 Perryridge Road, Medical Education,
Greenwich, CT 06830, United States
E-mail: Khalil.Hussein@ynhh.org
Received: January 15, 2022; Manuscript No: COCR-22-51853;
Editor Assigned: January 19, 2022; PreQC Id: COCR-22-51853 (PQ);
Reviewed: March 12, 2022;
QC No: COCR-22-51853 (Q);
Revised: March 18, 2022; Manuscript No: COCR-
22-51853 (R);
Published: May 05, 2022; DOI: 10.4172/cocr.5(5).233
Citation: Teng L, Hewlett JR, Hussein KI (2022) Cyclophosphamide, Bortezomib and Dexamethasone (CyBordD) for Multiple Extramedullary Plasmacytomas and Bilateral Myelomatous Pleural Effusion. Clin Oncol Case Rep 5:5
Abstract
Multiple soft-tissue Extramedullary Plasmacytomas (EMP) and Myelomatous Pleural Effusion (MPE) are two uncommon manifestations of advanced Multiple Myeloma (MM). The presence of both multiple EMP and MPE in the same MM presentation is very rare. We report the case of an 81-year-old woman who presented with dyspnea on exertion and productive cough. Physical exam found bibasilar rales and multiple soft, subcutaneous, mobile lumps on her bilateral upper extremities. Computed Tomography (CT) of her chest with Intravenous (IV) contrast identified a large mantle of soft tissue surrounding the distal thoracic aorta, a second mass involving the anterior right chest wall, and bilateral pleural effusions. Subsequent biopsy of the right chest wall mass revealed plasma cell neoplasm. Pleural fluid cytology was consistent with plasmacytoid/plasmacytic neoplasm. She was started on Cyclophosphamide, Bortezomib and Dexamethasone (CyBorD). Repeat Positron Emission Tomography (PET)-CT after 11 days of treatment demonstrated excellent response with apparent resolution of the posterior mediastinal mass and right anterior chest wall mass, no activity in thoracic spine, and decreased bone activity. Despite improved disease activity, she acutely decompensated due to aspiration pneumonia and septic shock, and she expired one week later. EMP and MPE individually confer poor prognosis, and the presence of both conditions as the initial manifestations of MM may complicate the diagnostic process and suggest more aggressive clinical features. The experience of our patient suggests the potential for favorable outcomes to CyBorD if complications are avoided.
Keywords: Multiple myeloma; Extramedullary plasmacytomas; Myelomatous pleural effusion; PTEN hamartoma tumor syndrome
Introduction
Multiple Myeloma (MM) arises from the malignant transformation of plasma cells. As the plasma cells infiltrate into bone marrow and skeleton, anemia, bone pain, renal insufficiency from light chain deposition, and hypercalcemia often result. Although the proliferation of neoplastic plasma cells is highly dependent on the bone marrow microenvironment, extramedullary involvement can occur in advanced stages of MM in the form of plasma cell leukemia or soft tissue Extramedullary Plasmacytomas (EMP). However, soft tissue EMP presenting as the initial manifestation of MM is very uncommon. The incidence of Extramedullary Plasmacytomas (EMP) at the time of MM diagnosis is between 3%-5% and may indicate a more advanced disease at diagnosis and stromal-independent transition [1,2]. EMP usually develops from either local extension of skeletal masses with thoracic wall as the most common affected region, or hematogenous spread with multiple subcutaneous nodules as the most frequently involved sites [3]. Both mechanisms are demonstrated in our case.
Pleural effusion is not rare in MM, and the reported incidence ranges from 11% to 42.7% [4-6]. Myelomatous Pleural Effusion (MPE), however, is a very uncommon cause of pleural effusion in MM with incidence of only 0.8% to 2.65% [7-10]. MPE is due to plasma cell infiltration of the pleura and tends to occur later in the disease course, but in rare cases including ours, MPE can be the presenting manifestation of MM. The pleural involvement can be the result of direct extension or invasion of a nearby lesion, or rarely, primary pleural plasmacytoma [11].
We describe a very atypical presentation featuring both MPE and multiple EMP at the time of diagnosis. A large chest wall lesion was the most likely cause of the MPE, which had to be differentiated from more common and benign etiologies of pleural effusion in MM such as heart failure, renal failure, or concurrent infection. While the concurrence of both EMP and MPE at diagnosis provided mutual corroboration for a more advanced disease stage of MM, the rarity of the combination clouded the initial clinical presentation and prolonged the diagnostic workup, which we highlight in this report. MPE and EMP individually confer poor prognosis, and the combination portended even worse outcome. However, our case suggests the potential for favorable outcomes in response to Cyclophosphamide, Bortezomib and Dexamethasone (CyBorD). As part of our literature review, we collected 18 previously reported cases with our case as the 19th case of both MPE and multiple EMP, and we discuss lessons to be learned [12-15].
Case Report
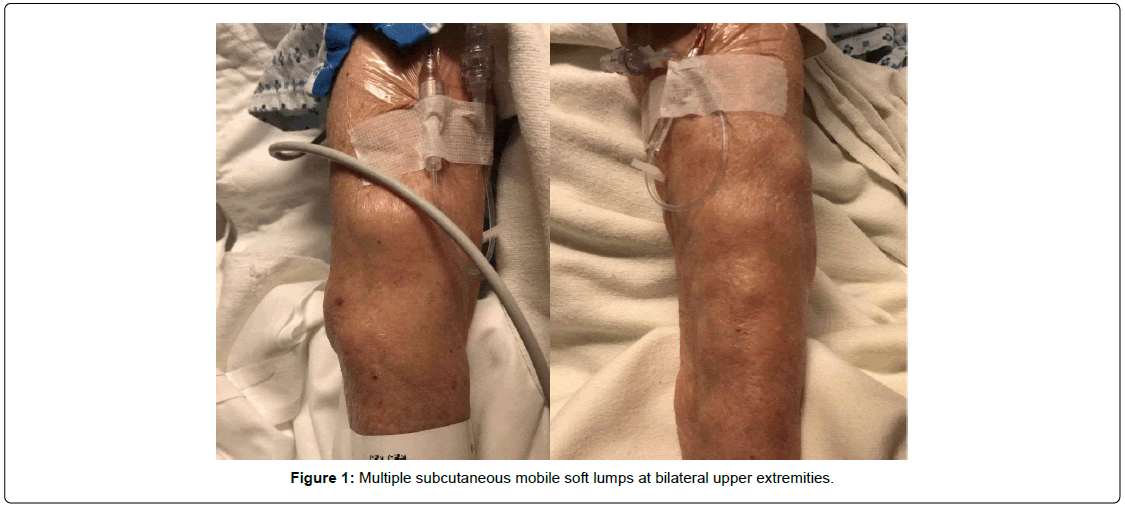
An 81-year-old woman with prior history of surgery to remove symptomatic left cavernous hemangioma 15 years ago in Guatemala complicated by residual dysphasia presented with productive cough and dyspnea on exertion of 4 weeks duration. Initial vital signs were: temperature 97.2°F, heart rate 98 beats per minute, blood pressure 168/76 mmHg, respiratory rate 20 breaths per minute, and oxygen saturation 92% on room air. Physical exam found multiple soft, subcutaneous, and mobile lumps on bilateral upper extremities (Figure 1). Chest auscultation demonstrated bibasilar rales, bilateral end expiratory wheezing, and significantly decreased breath sounds over right lower lung field. Labs revealed serum protein 7.7 g/dL, albumin 3.2 g/dL, Serum Lactate Dehydrogenase (LDH) 152 U/L, corrected calcium 9.9 mg/dL, and negative respiratory virus Polymerase Chain Reaction (PCR). Complete blood cell count with differential, creatinine, liver function tests, lactic acid, troponin I, procalcitonin, pro-BNP, blood cultures, and electrocardiogram were unremarkable. Chest x-ray was notable for cardiomegaly, edema, and bilateral pleural pulmonary effusions.
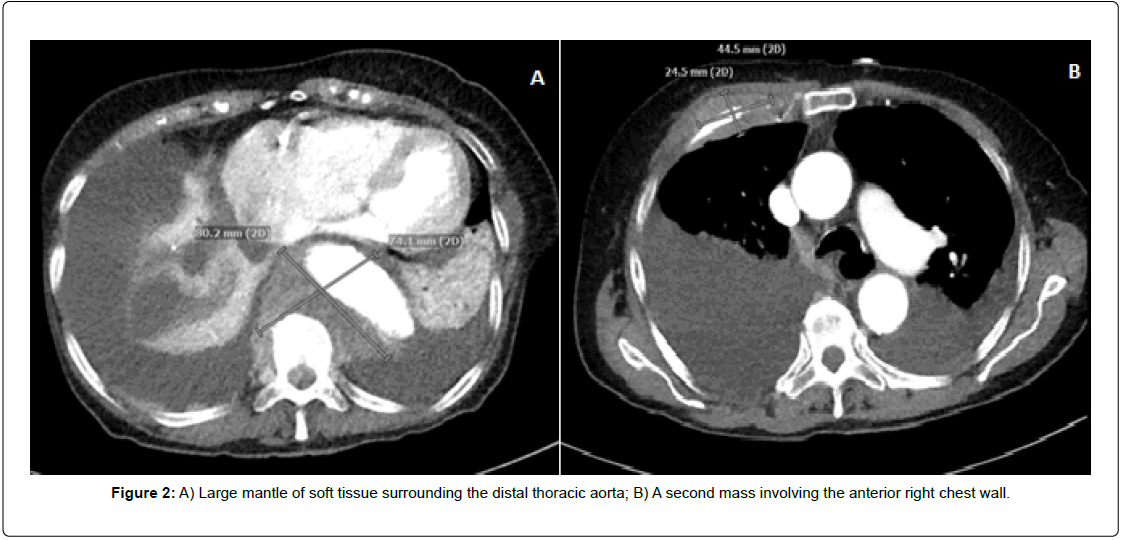
Computed Tomography (CT) of the chest with Intravenous (IV) contrast additionally identified a large mantle of soft tissue surrounding the distal thoracic aorta measuring 8.0 cm × 7.4 cm × 8.5 cm (Figure 2A) that also involved the T10 vertebral body. Also identified was a mass involving the anterior right chest wall measuring 4.5 cm × 2.5 cm × 4.6 cm (Figure 2B). Magnetic Resonance Imaging (MRI) of the brain found non-specific enhancing lesions in the right parietal calvarium. Full-spine MRI found T4 and T10 body enhancement with right epidural extension, abnormal bone marrow signal throughout the spine, and vertebral hemangiomas. Transthoracic echocardiogram was unremarkable.
Thoracentesis drained 1200 mL of serosanguinous fluid with pleural protein 4.9 g/dL, glucose 105 mg/dL, LDH 132 /L, and amylase 23 U/L, consistent with an exudative effusion. Pleural fluid cultures returned negative. Cytology of the fluid was consistent with plasmacytoid/plasmacytic neoplasm andflow cytometry found involvement by an abnormal lymphoplasmacytic population consistent with surface lambda light chain-restriction. In situ hybridization testing of pleural fluid for Human gammaherpesvirus 8 (HHV-8) and Epstein-Barr Virus (EBV) returned negative, which excluded primary effusion lymphoma.
Biopsy of right chest wall mass showed plasma cell neoplasm, and protein and immunoelectrophoresis showed lambda light chainrestricted and positive IgA lambda light chain gammopathy. Serum protein electrophoresis (SPEP) found abnormal band measuring 1.3 g/dL present in the beta region which was further characterized as IgA lambda on concurrent serum immunofixation electrophoresis. Bone Marrow (BM) biopsy and flow cytometry from BM aspirate were unremarkable.
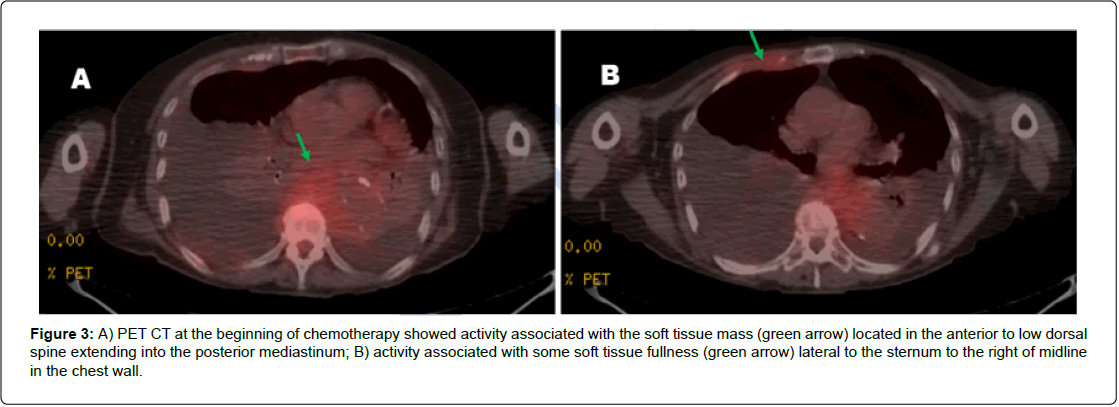
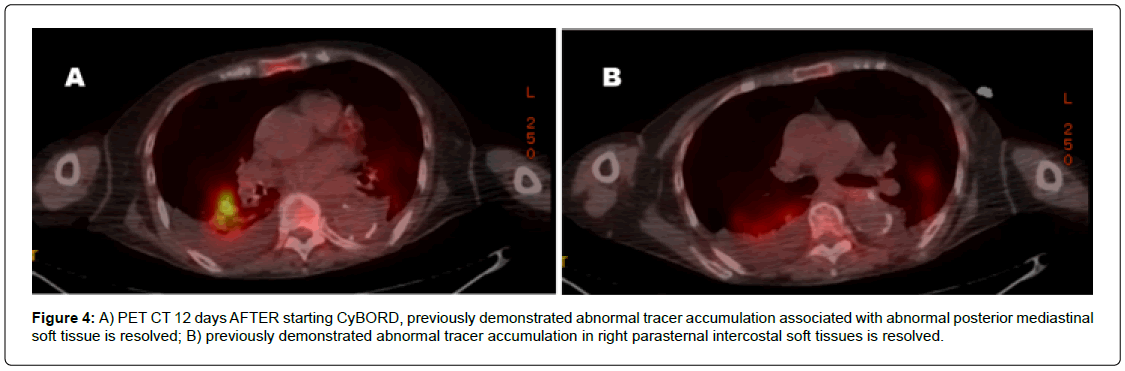
The patient was started on induction chemotherapy with CyBorD. After 12 days, repeat Positron Emission Tomography (PET)- CT showed excellent response in the posterior mediastinal mass (Figure 3A) and right anterior chest wall mass (Figure 3B) no longer noted (Figure 4), no activity in thoracic spine, and decreased bone activity. One week later, she decompensated due to aspiration pneumonia and septic shock, and she expired.
Figure 3: A) PET CT at the beginning of chemotherapy showed activity associated with the soft tissue mass (green arrow) located in the anterior to low dorsal spine extending into the posterior mediastinum; B) activity associated with some soft tissue fullness (green arrow) lateral to the sternum to the right of midline in the chest wall.
Literature review
We performed a literature search in PubMed using search criteria [(Multiple Myeloma) and (pleural effusions) and (extramedullary)], which resulted in 41 publications [16-18]. We selected 10 cases consistent with concurrent EMP and MPE by reading the abstracts. We then performed a broader search by the criteria of [(Myelomatous pleural effusion) and (extramedullary plasmacytoma)], which resulted in 19 articles [19]. We then selected additional 7 cases by comparing with the prior list of 10 and excluding the overlap cases. One more case was found by reading the review articles regarding extramedullary disease in Multiple Myeloma in the past 20 years. We included a total of 19 reports of MPE and multiple EMP, 18 from our literature review plus our case (Table 1).
Table 1: Summary of case reports.
| Age (years) | Sex | Onset in the disease course | EMP sites | MPE laterality | Pathology subtype | Management | Outcomes |
|---|---|---|---|---|---|---|---|
| 62 | Male | At diagnosis | Para-tracheal mass lesion |
Right | Not done | Dexamethasone and lenalidomide | Expired 2 weeks after presentation |
| 68 | Male | After diagnosis, exact time not given | Right thoracic and paravertebral |
Right | IgA Kappa | PE drainage, pleurodesis by bleomycin instillation, local radiation, systemic therapy for MM (pomalidomide +cyclophosphamide+dexamethasone) resulted in resolution of 2 episodes of MPE | Expired 18 months after the first MPE episode |
| 50 | Female | Not available | Ovaries, uterus, pancreas | Right | Not available | At the presence of MPE, 4 courses of the bortezomib+lenalidomide+dexamethasone regimen, partial response was achieved; 2 courses of daratumumab+lenalidomide+dexamethasone (DLd) regimen achieved complete response; followed by autologous peripheral blood stem cell transplantation +additional 4 courses DLd regimen; maintenance therapy containing daratumumab and dose-reduced lenalidomide | Maintained relapse-free survival for two years with maintenance therapy |
| 67 | Female | EMP at 14 years and MPE at 19 after diagnosis | Right chest wall | Right | IgA Kappa | Chemotherapy, autologous hematopoietic stem cell transplantation, and local radiation therapy at the presence of EMP; chemical pleurodesis with talc, local radiotherapy and chemotherapy (pomalidomide–dexamethasone–cyclophosphamide) at the presence of MPE | Achieving clinical remission that lasted 6 months after diagnosis of the MPE. |
| 39 | Female | 4 years after diagnosis | Pericardial, cardiac tamponade | Left | IgA Lambda | 4 cycles of PAD (bortezomib+adriamycin+dexamethasone)+ Zoledronic acid resulted complete remission for 2 years; at the 1st relapse, 4 cycles of Lenalidomide+dexamethasone, loss of response, VCD chemotherapy (bortezomib, cyclophosphamide, and dexamethasone) achieving a second complete remission; reduced-intensity conditioning regimen followed by fully matched sibling hematopoietic stem cell transplantation to consolidate response; at 2nd relapse, 2 cycles of VCD, switched to VBCMP/VBAD chemotherapy (vincristine, carmustine, cyclophosphamide, melphalan, prednisone/vincristine, carmustine, doxorubicin, and high-dose dexamethasone), achieving a third complete remission; at presence of MPE, 18th cycle of carfilzomib+dexamethasone | Remained complete remission 19 months after MPE |
| 68 | Male | 4 months after diagnosis | Left chest wall mass | Bilateral | IgA Kappa | MPE appeared after two cycles of chemotherapy using bortezomib and dexamethasone; required intubation at the presence of MPE | expired 12 hours after extubation for comfort measures only |
| 74 | Female | at diagnosis | Mediastinal mass; right posterior paraspinal mass | Right | IgG Kappa | Hospice | expired within a month of diagnosis |
| 62 | Female | 3 months after diagnosis | Subcutaneous | Right | IgA Kappa | three cycles of thalidomide and dexamethasone induction + local radiation resulted in remission of MM; local radiation leading to complete regression of the subcutaneous nodule; VAD (vincristine, doxorubicin and dexamethasone) started at the presence of MPEsubcutaneous nodules | expired 12 month after the first clinical presentation |
| 52 | Female | 7 years after diagnosis | Abdominal lymphadenopathy; renal mass | Right | IgG Kappa | Thalidomide and dexamethasone resulted In complete remission of MM; thalidomide+zoledronic acid maintenance for 5 years; at 5th year's progression, lenalidomide+dexamethasone+zoledronic acid resulted in partial response; new pelvic lesion, palliative radiotherapy, 3 cycles of VRD (bortezomib+lenalidomide+dexamethasone) regimen followed by VRD maintenance ; at 7th years presence of EMP, 1 cycle of PAD (bortezomib+ doxorubicin+dexamethasone) regimen, followed by metronomic therapy (cyclophosphamide+prednisolone+thalidomide | Expired 3 months after the presence of MPE |
| 53 | Male | At the diagnosis | Bilateral pleural nodules | Bilateral | IgG Kappa | 2 cycles of VTD (bortezomib, dexamethasone and thalidomide) |
By the time of case reported, overall condition of the patient is good (clear time course not given). |
| 65 | Male | At the diagnosis | Anterior mediastinal mass | Bilateral | Lambda light chain restriction | Two courses of induction chemotherapy intravenous (thalidomide+cyclophosphamide + dexamethasone), radiotherapy | Long term outcomes not given |
| 76 | Male | At diagnosis | Bilateral pleural and chest wall masses; extraosseous soft-tissue masses on lumbosacral spine | Bilateral | IgG Lambda | Not reported | Expired 4 weeks after presentation |
| 70 | Male | at diagnosis | Mediastinal mass; numerous pleural-based nodules | Right | IgG Lambda | Velcade, melphalan, and prednisone | Not reported |
| 66 | Female | 1.5 years after diagnosis | Pleural thickening | Right | Igg Kappa | 8 months of CTD (cyclophosphamide+thalidomide+dexamethasone) resulted in remission; at presence of MPE, CVD (Cyclophosphamide+Velcade+Dexamethasone) resulted in good response, no re-accumulate for 3 months; At reoccurrence of MPE, Melphalan+dexamethasone started, and progression was halted. | Progression remained halted by the time of case reported (8 months after presence of MPE). No long term outcomes reported |
| 74 | Male | 3 years after diagnosis | Right chest wall and paravertebral space; subcutaneous mass in abdominal wall; multiple gastric polyps | Bilateral | Igg kappa | Observation for 2 years; 12 courses of monthly melphalan + prednisolone resulted in partially remission; at the progression, daily thalidomide+dexamethasone resulted in good response for 3 months | Expired 8 months after the presence of mpe |
| 63 | Female | 3 years after diagnosis | Pleural thickening | Left | Iga kappa | Four cycles of vad (vincristine+ adriamycin+ dexamethasone) resulted in partial response, followed by maintenance thalidomide; at presence of mpe, vad regimen followed by salvage bortezomib+ dexametazone | Expired 11 months after the presence of mpe |
| 55 | Not available | 7 years after diagnosis | Left thoracic wall | Left | Igg lambda | Plasmapheresis and several courses of chemotherapy, radiotherapy | Not available |
| 51 | Female | 4 years after diagnosis | Subcutaneous, abdominal cavity | Right | Igg kappa | Repeated courses of melphalan+prednisolone resulted in remission for 4 years; one course of vcap (vincristine+cyclophosphamide+adriamycin+prednisolone) at the presence of subcutaneous lesion; at progression, alpha-interferon+ mod (mitoxantrone, vincristine, dexamethasone) followed by intrapleural adriamycin, methotrexate + leucovorin, and intraperitoneal of α-interferon | Expired 3 weeks after the appearance of pleural effusions |
| 81 | Female | At diagnosis | Subcutaneous, right chest wall | Right | Lambda light chain restriction | CyBorD (cyclophosphamide + bortezomib + dexamethasone) for 12 days | Expired within 1 month after initial presence of MPE due to aspiration event |
Discussion
Clinical characteristics
Multiple Myeloma (MM) is typically confined to the bone marrow and skeleton. EMP is an uncommon initial manifestation of MM, while MPE is an even rarer form of extramedullary disease. A decade ago, the incidence of EMP was reported to range from 7%-18% in newly diagnosed MM and 6%-20% later in the disease course [20]. Although our screening and diagnostic means have become more widely available, the incidence has not increased. The most recently observed incidence was reported as 3%-5% at time of initial MM diagnosis [21-25]. In a recent observational retrospective study [26], incidence of MPE at relapse of MM was found to be more common than at initial clinical presentation. In our literature review, concurrent soft tissue EMP and MPE at the initial diagnosis of MM were found in only 7 out of 19 cases while the remaining 12 cases developed concurrent presentation of those disease manifestations at relapse.
The majority of EMPs (68%-85%) observed at diagnosis were soft-tissue masses adjacent to bone lesions [3]. In the 19 cases we reviewed, chest wall masses (7 out of 19) were the most common, and paravertebral involvement (4 out of 19) is the second common sites of EMPs. This also suggests that local growth from focal bone lesions remains the most likely mechanism of EMPs. In our case, a large EMP surrounding the distal thoracic aorta had involved the nearby vertebral body, and the epidural lesions appeared to be extraosseous in origin. Extraosseous myeloma is a rare cause of spinal cord compression; most spinal cord compression in MM is related to pathological fracture of the involved vertebral body or extension of a vertebral body myeloma lesion [27]. In prior analysis of EMPs with invasion of the spinal canal, most patients (19 out of 36) were observed to have thoracic spinal cord involvement, similar to our case [28].
Prior studies have suggested that direct plasma cell infiltration of the pleura is the mechanism of MPE development, and patients with adjacent chest wall or pulmonary lesions more commonly develop MPE. Of the cases of MPE we reviewed, the majority (78.9%, 15/19) followed this pattern: chest wall (7/19), mediastinal (3/19), pleural thickening (2/19), para-tracheal (1/19), and pericardial (1/19). Like pleural effusions from other etiologies, our review suggested MPEs have a right-sided preponderance in the setting of concurrent soft tissues EMPs. The number in our selected cases are 11 on the right side, 5 bilateral, and 4 on the left side. This is consistent with one prior observational study [26], but differed from another study reporting left side more commonly involved than right [7]. The reason for this tendency remains unclear.
Although MPE has been reported to be associated with IgG kappa [26] or IgA subtype [7], we have not seen very concentrated distribution in subtypes, with 6 IgG kappa and 6 IgA (1 lambda, 5 kappa) in the 19 cases.
Diagnosis and differentials
EMPs can be found at diagnosis or at relapse of MM with screening by imaging modalities like PET-CT and MRI. Serum Protein Electrophoresis (SPEP) with immunofixation and quantitation of immunoglobulins and serum light chains can also be helpful. The key part of diagnosis is to confirm the presence of malignant plasma cells based on both cytology and immunohistochemistry in the biopsy of EMPs tissues. Thoracentesis followed by pleural fluid studies are essential to diagnose suspected MPE.
In a recent retrospective study of MM patients with pleural effusions, MPE was found in as high as 38.2% of patients [6]. The true rate can be even higher given not all patients undergo appropriate diagnostic evaluation with thoracentesis and biopsy. In our case, the pleural fluid flow cytometry found involvement by an abnormal lymphoplasmacytic population consistent with surface lambda light chain-restriction. A rare differential diagnosis which was considered was Primary Effusion Lymphoma (PEL). All patients with PEL have HHV-8 infection and many have EBV infection. Therefore, in situ hybridization testing of pleural fluid for HHV-8 and EBV are needed to exclude the possibility of PEL. In areas with high prevalence of Tuberculosis (TB), possible etiology of pleural effusions also includes reactive pleural effusion to TB. It has been previously reported that localized extramedullary plasma cell proliferation can be a transient reactive process to pulmonary TB, which subsides when the underlying TB is treated [29].
In our case, the BM pathology and flow cytometry were both negative for plasma cell neoplasm. This can be due to patchy myeloma involvement as noted on PET-CT, which is seen in approximately 4% of MM patients [30]. In this case, there was diagnostic suspicion for underlying genetic syndrome such as PTEN hamartoma tumor syndrome due to hemangiomas in brain and spine, lipomas, and hematologic malignancy, but genetic testing was not performed prior to our patient’s passing.
Treatment
Extramedullary Disease (EMD) was reported to be resistant to conventional treatments but responded well to regimens containing novel drugs such as bortezomib. In a recent review [1], an approach to EMD in newly diagnosed MM is suggested for elderly patients with age greater than 65 years with CyBorD as an initial induction therapy followed by lenalidomide-bortezomib-dexamethasone (RVd) regimen, and then high-dose chemotherapy and autologous stem cell transplant can be considered based on the response. As observed in the 19 cases with concurrent EMPs and MPE over the past three decades, treatment has always been a challenge with no consistent results or trends. However, considering MPE is a rare form of EMPs, the observed benefit still favors the trial of CyBorD as an initial therapy. In our case, patient showed excellent radiographical response to only one cycle of CyBorD prior to her unexpected passing.
Prognosis
MPE confers very poor prognosis with a median time of death of 4 months from onset of the pleural effusions [7]. In a case series of 19 patients with MPE, seven expired within 3 months after initial diagnosis of MPEs, and 2 more expired within 12 months of MPE diagnosis. Among cases with reported cause of death (9 out of 19), most were attributed to direct progression of MM (7/9). In our case, the patient passed due to complications from an aspiration event, which is not a typical sign of MM progression. In a prior observational study of 23 MM patients with MPE, respiratory failure and cardiac tamponade were the two most common causes of death [31].
Conclusion
This data along with our case suggest that patients with MPE may be more likely to deteriorate from pulmonary and/or cardiogenic events rather than the more commonly known complications of MM such as infection or renal failure.
References
- Jagosky MH, Usmani SZ (2020) Extramedullary disease in multiple myeloma. Curr Hematol Malig Rep 15: 62-71.
Google Scholar Cross Ref - Gagelmann N, Eikema DJ, Iacobelli S, Koster L, Nahi H, et al. (2018) Impact of extramedullary disease in patients with newly diagnosed multiple myeloma undergoing autologous stem cell transplantation: A study from the chronic malignancies working party of the EBMT. Haematologica 103: 890-897.
Google Scholar Cross Ref - Bladé J, Fernández de Larrea C, Rosiñol L, Cibeira MT, Jiménez R, et al. (2011) Soft-tissue plasmacytomas in multiple myeloma: incidence, mechanisms of extramedullary spread, and treatment approach. J Clin Oncol 29: 3805-3812.
Google Scholar Cross Ref - Wang Z, Xia G, Lan L, Liu F, Wang Y, et al. (2016) Pleural effusion in multiple myeloma. Intern Med 55: 339-345.
Google Scholar Cross Ref - Byun JM, Kim KH, Choi IS, Park JH, Kim JS (2017) Pleural effusion in multiple myeloma: Characteristics and practice patterns. Acta Haematol 138: 69-76.
Google Scholar Cross Ref - Kang Y, Hou ZL, Yang GZ, Wang XJ, Chen WM (2021) Clinical characteristics and risk factors for pleural effusion in patients with multiple myeloma. Int J Gen Med 14: 649-657.
Google Scholar Cross Ref - Kamble R, Wilson CS, Fassas A, Desikan R, Siegel DS (2005) Malignant pleural effusion of multiple myeloma: Prognostic factors and outcome. Leuk Lymphoma 46: 1137-1142.
Google Scholar Cross Ref - Hussain A, Khurana U, Vijayverghia G, Khurana AK, Goyal A (2021) Cytologic and flowcytometric findings in a case of myelomatous pleural effusion: A rare and ominous presentation of multiple myeloma. Diagn Cytopathol 50: E59-E62
Google Scholar Cross Ref - Martín-Moro F, Roncancio A, Benito A, Talavera M, Villarrubia J (2020) Myelomatous pleural effusion with plasmablastic morphology and high genetic complexity as isolated extramedullary relapse. Ann Hematol 99: 2705-2706.
Google Scholar Cross Ref - Wada A, Yasumura S, Kajikawa S, Murakami J, Sato T (2020) Successful treatment of myelomatous pleural effusion with daratumumab administration before autologous peripheral stem cell transplantation. Rinsho Ketsueki 61: 879-884.
Google Scholar Cross Ref - Velasco-Álvarez D, Gorospe-Sarasúa L, Fra-Fernández S, Blanchard MJ (2019) Extramedullary multiple myeloma with pleural involvement: A rare clinical entity. Arch Bronconeumol (Engl Ed) 55: 333-334.
Google Scholar Cross Ref - Español I, Romera M, Gutiérrez‐Meca MD, del Carmen García M, et al. (2017) Carfilzomib and dexamethasone for extramedullary myeloma with pleuropericardial involvement. Clin Case Rep 5: 1258-1260.
Google Scholar Cross Ref - Asiamah R, Mukkamalla SK, Sahai T, Zhou XP, Han E, et al. (2017) Bilateral myelomatous pleural effusion in a patient with IgA kappa multiple myeloma. Cureus 9: e1238.
Google Scholar Cross Ref - Williams G, Kadaria D, Sodhi A (2016) Concurrent myelomatous pleural effusion and extramedullary mediastinal involvement as an initial manifestation of multiple myeloma. Am J Case Rep 17: 472-475.
Google Scholar - Saidane O, Slouma M, Haouet S, Abdelmoula L (2015) Cutaneous and pleural involvement in a patient with multiple myeloma. BMJ Case Rep 2015.
Google Scholar Cross Ref - Arora P, Gupta SK, Mallik N, Mittal R, Sharma OD (2016) Flow cytometry in diagnosis of myelomatous pleural effusion: A case report. Indian J Hematol Blood Transfus 32(Suppl 1): 138-142.
Google Scholar Cross Ref - Zhang LL, Li YY, Hu CP, Yang HP (2014) Myelomatous pleural effusion as an initial sign of multiple myeloma-A case report and review of literature. J Thorac Dis 6: E152-E159.
Google Scholar Cross Ref - Ok SJ, Kim IS, Lee EY, Kang JE, Lee SM (2014) A case of salivary-type amylase-producing multiple myeloma presenting as mediastinal plasmacytoma and myelomatous pleural effusion. Ann Lab Med 34: 463-465.
Google Scholar - Suwatanapongched T, Pornsuriyasak P, Kanoksil W, Morasert T, Virayavanich W (2014) A 76-year-old man with anemia, bone pain, and progressive dyspnea. Diagnosis: Bilateral myelomatous pleural effusions with extramedullary plasmacytomas. Chest 145; 913-918.
Google Scholar Cross Ref - Raci-Wetherbe E, Dincer HE (2012) IgG myeloma presenting as a large mediastinal mass and pleural effusion. J Bronchology Interv Pulmonol 19: 65-67.
Google Scholar Cross Ref - Miller J, Alton PA (2012) Myelomatous pleural effusion-A case report. Respir Med Case Rep 5: 59-61.
Google Scholar Cross Ref - Nakazato T, Suzuki K, Mihara A, Sanada Y, Kakimoto T (2009) Refractory plasmablastic type myeloma with multiple extramedullary plasmacytomas and massive myelomatous effusion: Remarkable response with a combination of thalidomide and dexamethasone. Intern Med 48: 1827-1832.
Google Scholar Cross Ref - Balleari E, Carbone RG, Grosso M, Ghio R (2008) A pleural effusion due to extramedullary pleural plasmacytoma: A case report. Intern Emerg Med 3: 289-291.
Google Scholar Cross Ref - Yamakawa T, Nagoshi H, Takahashi A, Fukumura R, Takahashi S (1995) Acquired amylase production induced by radiotherapy in a myeloma patient. Rinsho Ketsueki 36: 1175-1181.
Google Scholar - Matsumoto A, Nagata K, Hamaguchi H, Taki K (1993) Solitary bone plasmacytoma terminally developed myeloma with multiple extramedullary lesions and myelomatous pleural effusion and ascites. Int J Hematol 59: 59-65.
Google Scholar - Yanamandra U, Deo P, Sahu KK, Nampoothiri RV, Gupta N (2019) Clinicopathological profile of myelomatous pleural effusion: Single-center real-world experience and review of literature. Clin Lymphoma Myeloma Leuk 19: 183-189.
Google Scholar Cross Ref - Ha KY, Kim YH, Kim HW (2013) Multiple myeloma and epidural spinal cord compression : Case presentation and a spine surgeon's perspective. J Korean Neurosurg Soc 54: 151-154.
Google Scholar Cross Ref - Zhang J, Zhong Y (2015) Clinical analysis of 36 multiple myeloma patients with extramedullary plasmacytoma invasion of the spinal canal. Hematol Oncol 33: 75-79.
Google Scholar Cross Ref - Soliman DS, Ali M, Akikki S, Ibrahim F, El-Omari H, et al. (2020) Transient pleural fluid infiltration by clonal plasma cells associated with pulmonary tuberculosis. Case Rep Oncol 13: 883-891.
Google Scholar Cross Ref - Kyle RA, Gertz MA, Witzig TE, Lust JA, Lacy MQ, et al. (2003) Review of 1027 patients with newly diagnosed multiple myeloma. Mayo Clin Proc 78: 21-33.
Google Scholar Cross Ref - Zhong Y, Zhang J, Wang H (2015) Myelomatous pleural effusion involvement in 23 patients with multiple myeloma: A single-center clinical analysis. Thorac Cancer 6: 359-362.
Google Scholar Cross Ref
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi