Case Report, Clin Oncol Case Rep Vol: 3 Issue: 6
Lymphoproliferative Disease in the Pediatric Airway Contributing to Obstructive Sleep Apnea
Harrison Love*, Ryan Mitchell, Anuja Bandyopadhyay and Marissa Bruce
School of Medicine, Indiana University, Indiana
*Corresponding Author:
Harrison Love
School of Medicine, Indiana University
Indiana, United States
E-mail: hllove@iu.edu
Received: August 20, 2020 Accepted: November 02, 2020 Published: November 20, 2020
Citation: Love H (2020) Lymphoproliferative Disease in the Pediatric Airway Contributing to Obstructive Sleep Apnea. Clin Oncol Case Rep 4:1
Abstract
Abstract
This is a case report of an 18-year-old male with a history of lymphoproliferative disease who presented to the otolaryngology-head and neck surgery service with signs and symptoms of Obstructive Sleep Apnea (OSA). The patient had undergone a tonsillectomy and adenoidectomy 12-years prior, but current imaging demonstrated asymmetric tonsils and an enlarged left tonsil. The patient underwent drug-induced-sleep-endoscopy to further investigate the source of obstruction and was found to have obstructive tissue at the supraglottis and base of tongue. The tissue was likely a result of the patient’s lymphoproliferative disease and was a primary contributing factor to the OSA. Clinical suspicion for pharyngeal lymphoid tissue should be high in patients with this disease who are showing clinical signs of OSA.
Keywords: Obstructive sleep apnea; Drug-induced-sleep-endoscopy; DISE; Supraglottoplasty; Lymphoproliferative disease; CVID
Keywords
Obstructive sleep apnea; Drug-induced-sleep-endoscopy; DISE; Supraglottoplasty; Lymphoproliferative disease; CVID
Introduction
Lymphoproliferative disorders represent a broad category of diseases that are all related through the uncontrolled production of lymphocytes. These heterogenous diseases include lymphomas, leukemias, and myelomas, and are most commonly found in immunocompromised individuals who no longer have the ability to regulate lymphocyte growth [1]. This includes patients who are undergoing chemotherapy or organ transplant along with those who have Combined Variable Immunodeficiency (CVID), Severe Combined Immunodeficiency (SCID), and Human Immunodeficiency Virus (HIV), among others.
This diverse cohort of patients can present with unique complications. Dysregulation of their immune system predisposes them to infection and malignancy. However, the unregulated growth of cells can cause localized problems depending on anatomical site. There have been recent cases in the literature that have demonstrated the development of Obstructive Sleep Apnea (OSA) in pediatric patients as a consequence of non-Hodgkin lymphoma, adenotonsillar hypertrophy after liver transplantation, and Epstein-Barr Virus (EBV) tonsillitis [2-4]. This case report offers another instance of OSA following a unique presentation of lymphoproliferative disease in the pharynx and its associated airway obstruction. These cases highlight the importance of airway evaluation and sleep studies in patients with lymphoproliferative disorders and signs and symptoms of obstructive sleep apnea.
Case Report
An 18-year-old male with a past medical history significant for CVID with a mutation of toll-like receptor 9, lymphoproliferative disease, bronchiectasis with chronic hypoxia, Crohn’s disease, asthma, and chronic sinusitis was referred to the otolaryngology-head and neck surgery service by his pulmonologist for investigation of an enlarged left tonsil and signs and symptoms of obstructive sleep apnea, including observed apneas. He reported snoring, significant daytime fatigue and had intermittent witnessed apneic events. During the interview, the patient revealed that he had prior history of adenotonsillectomy (T and A) and lingual tonsillectomy at 6 years of age. On physical exam, he appeared to have grossly asymmetric tonsils, with his left tonsil appearing to occupy nearly 80% of the posterior pharynx. The patient had a BMI of 15.8 and his most recent sleep study in 2010 revealed no significant respiratory abnormalities and only mild sleep disruption. CT neck with contrast, obtained pre-operatively, confirmed the asymmetric enlargement of the left tonsil with interval increase in the size of lymph nodes, which was concerning for a Mucosa-Associated Lymphoid Tissue (MALT) lymphoma. The rest of the exam was unremarkable, and the patient was scheduled for a Drug Induced Sleep Endoscopy (DISE) and adenotonsillectomy to remove obstructing tissue.
Drug Induced Sleep Endoscopy (DISE) was performed, and obstruction was noted at the supraglottis and base of the tongue. Adenotonsillectomy was aborted and patient underwent removal of tissue deposits from the base of tongue and right supraglottis. Pathology report identified florid chronic granulomatous inflammation, which was consistent with benign lesions of lymph nodes and other tissues [5]. He was discharged to home on postoperative day 2, with no respiratory support while awake, and 2 L oxygen via nasal cannula while sleeping to prevent desaturation. He declined postoperative polysomnography (Figure 1).
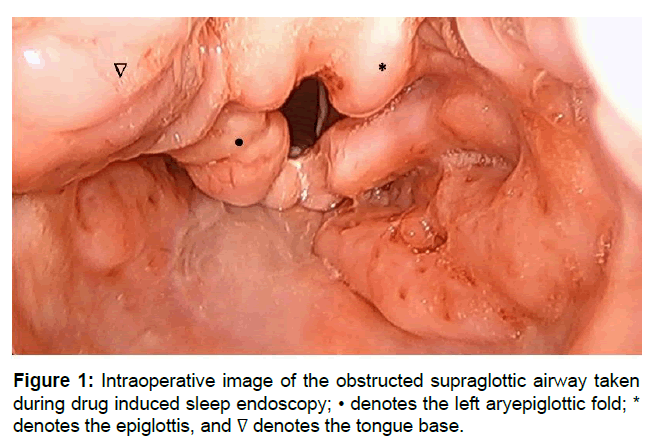
Figure 1: Intraoperative image of the obstructed supraglottic airway taken during drug induced sleep endoscopy; • denotes the left aryepiglottic fold; * denotes the epiglottis, and ∇ denotes the tongue base.
Discussion
This case demonstrated a unique cause for obstructive sleep apnea in the pediatric population. Although lymphatic disease had been shown as a potential cause of airway obstruction [6], this patient was interesting because he had a previous adenotonsillectomy but was evaluated for what appeared to be an asymmetrically enlarged tonsil. This case is similar to one presented in 2017 by Ganesan et al. in which a 14-year-old male had pharyngeal non-Hodgkin lymphoma that was initiating symptoms of obstructive sleep apnea. Although that patient did not have chronic lymphoproliferative disease, he presented to the department of otolaryngology for a pharyngeal mass that was discovered on evaluation of sleep disturbances and daytime somnolence. After being diagnosed, he was treated with chemotherapy and the OSA symptoms were resolved with the resolution of the pharyngeal mass [3].
In a parallel fashion, our patient appeared to have an enlarged left tonsil while being evaluated for newly observed apneas and daytime somnolence. Instead of chemotherapy, our patient was further evaluated with sleep endoscopy. DISE was important in this case because it changed the surgical management from adenotonsillectomy to supraglottoplasty. DISE allowed for the systematic grading of the airway to determine the specific areas for surgical intervention. Without DISE, the patient could have undergone a surgical intervention that would not have corrected his OSA and would have resulted in residual symptoms.
Conclusion
Overall, this case demonstrates that patients with lymphoproliferative disease, snoring, and daytime fatigue should be evaluated for obstructive sleep apnea. Despite a history of previous tonsillectomy, these history and physical findings should prompt clinicians to evaluate for lymphoid regrowth. Clinicians should not be hesitant to use DISE perioperatively to develop a surgical plan. Identification of tonsillar hypertrophy should increase the index of suspicion for pharyngeal lymphoid tissue in patients with lymphoproliferative disease.
References
- Litz CE, Brunning RD (1993) 2 Chronic lymphoproliferative disorders: Classification and diagnosis. Baillieres Clin Haematol 6: 767-783.
- Cheng J (2014) Obstructive sleep apnea (OSA): A complication of acute infectious mononucleosis infection in a child. Int J Pediatr Otorhinolaryngol 78: 561-562.
- Ganesan AP, Jiang W, Kuo DJ, Bhattacharjee R (2017) Obstructive sleep apnoea as a presenting manifestation of non-Hodgkin lymphoma in a child. Lancet Oncol 18: e618.
- Mulla O, Bajaj Y, Knight L (2012) Severe obstructive sleep apnoea due to adenotonsillar hypertrophy after liver transplantation. BMJ Case Rep 2012: bcr2012007059.
- Matsumiya H, Kawata K, Kamekura R (2017) High frequency of Bob1(lo) T follicular helper cells in florid reactive follicular hyperplasia. Immunol Lett 191: 23-30.
- Capdevila OS, Kheirandish-Gozal L, Dayyat E, Gozal D (2008) Pediatric obstructive sleep apnea: complications, management, and long-term outcomes. Proc Am Thorac Soc 5: 274-282.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 