Case Report, Clin Oncol Case Rep Vol: 2 Issue: 1
Primary Renal Angiosarcoma with Cutaneous Metastasis to the Skin
Jessica Connor1, Saikrishnaraya Doppalapudi1, Wenlei He2, Michael Benson2, Michael Esposito2 and Mutahar Ahmed2
1Rutgers New Jersey Medical School, New Jersey, USA
2Department of Urology, Hackensack University Medical Center, Hackensack, New Jersey, USA
*Corresponding Author : Jessica Connor
Rutgers New Jersey Medical School, USA
Tel: 2013151536
E-mail: jac700@njms.rutgers.edu
Received: July 24, 2018 Accepted: February 06, 2019 Published: February 13, 2019
Citation: Connor J, Doppalapudi S, He W, Benson M, Esposito M, et al. (2019) Primary Renal Angiosarcoma with Cutaneous Metastasis. Clin Oncol Case Rep 2:1.
Abstract
Angiosarcoma is a rare and rapacious tumor that most frequently arises from the skin and soft tissue. When these tumors do originate from solid organs, the most common sites of origin are the breast, liver, and bone. Angiosarcomas themselves represent approximately 2% of soft tissue sarcomas and of these, less than 1% are primary renal tumors. When angiosarcoma is discovered in the kidney, it almost always represents metastasis from a cutaneous or visceral organ primary tumor and metastasis is not uncommon as these tumors exhibit aggressive behavior. On the rare occasion that an angiosarcoma arises in the kidney, metastasis is likely with up to 45% of cases presenting with metastasis at time of diagnosis. The most common sites of metastasis from the kidney include liver, lungs, and bone with reports of spread to the peritoneum and spleen occurring as well. Myxoid liposarcoma is a rare tumor in the pediatric age group. Improvements in facilities for multi-modal treatment might help to improve outcomes in a limited-resource setting like ours.
Keywords: Angiosarcoma; Tumor; Computed tomography
Introduction
Angiosarcoma is a rare and rapacious tumor that most frequently arises from the skin and soft tissue. When these tumors do originate from solid organs, the most common sites of origin are the breast, liver, and bone [1]. Angiosarcomas themselves represent approximately 2% of soft tissue sarcomas and of these less than 1% are primary renal tumors [2]. When angiosarcoma is discovered in the kidney, it almost always represents metastasis from a cutaneous or visceral organ primary tumor and metastasis is not uncommon as these tumors exhibit aggressive behavior [3]. On the rare occasion that an angiosarcoma arises in the kidney, metastasis is likely with up to 45% of cases presenting with metastasis at time of diagnosis [4]. The most common sites of metastasis from the kidney include liver, lungs, and bone with reports of spread to the peritoneum and spleen occurring as well [4].
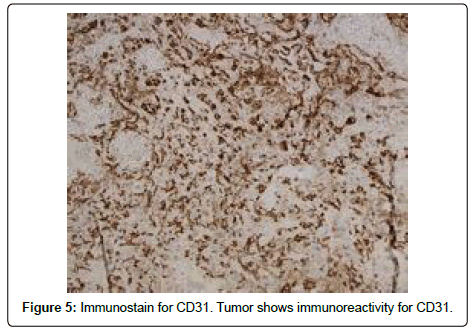
Epidemiologically, primary renal angiosarcoma has often proven to be a white Caucasian male entity [2]. The average age of reported cases is 61 years and there a slight left-sided dominance [4]. Diagnosis is challenging as these tumors present with features similar to those of other renal masses with symptoms such as hematuria, flank pain, abdominal mass, and weight loss [5]. On computed tomography, renal angiosarcomas appear as large necrotic masses, similar in appearance to many renal cell carcinomas [6]. Immunohistochemical analysis and histopathology thus play key roles in definitive diagnosis. CD31, an endothelial cell adhesion molecule is highly specific and sensitive for angiosarcoma [7].
Here we present a case in which the patient was discovered to have both renal and skin involvement at time of presentation. Based on the literature, it is likely that the renal tumor in the context of a scalp angiosarcoma represents metastasis, however after pathological workup, it was discovered that the tumor most likely originated from the kidney or the retroperitoneum.
Case Report
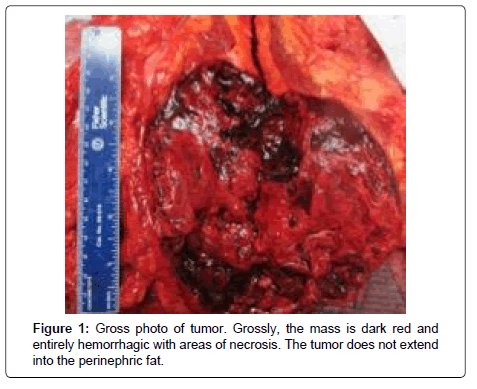
The patient is an 84-year-old male former smoker with history of hypertension and hyperlipidemia who presented with diffuse abdominal pain. Computed tomography scan showed a 16.3 x 13.3 x 16.5 cm mass in the lower pole of the left kidney with areas of central low attenuation consistent with necrosis. In addition, there was concern for involvement of the transversalis musculature. However, there was no pathological lymphadenopathy in the abdomen or pelvis. At the time of exam, he was also discovered to have a “cyst” on the right temporal region which was described by a medical oncologist as a probable angiosarcoma (Figure 1).
A robotic-assisted laparoscopic left radical nephrectomy was performed with no complications. Meticulous dissection was necessary due to the very large size of the mass. Specimen was placed in a large laparoscopic bag and then open extraction was used to remove the intact left kidney, adrenal gland, and a segment of the ureter. Intra-operatively, it was discovered that the tumor did not involve the musculature. A lymph node dissection was not performed since none appeared pathologic. The patient had an uneventful post-operative course and was discharged 2 days later (Figure 2).
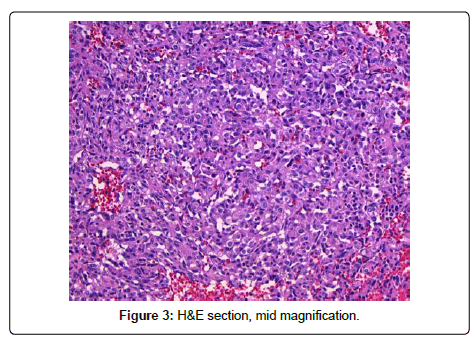
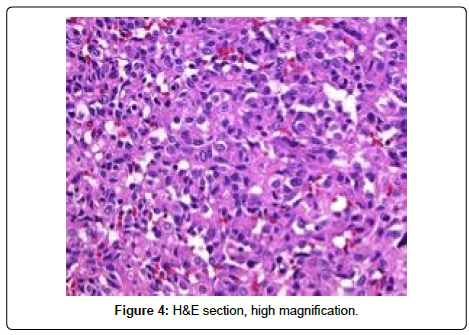
Pathology showed a high grade angiosarcoma with extensive necrosis and hemorrhage. Grossly, the tumor was 14 cm in greatest dimension and primarily located within the perirenal and hilar soft tissue with focal involvement of the lower pole of the kidney. The renal vein and collecting system were not invaded by tumor. The adrenal gland and segment of ureter were negative for tumor involvement (Figure 3). On immunohistochemical analysis, the tumor cells were reactive to CD31, CD34, ERG (expected for angiosarcoma) and caldesmon. In addition, the tumor cells showed weak focal positivity for desmin, and negativity for HMB-45, melan-A, and PAX-8. Congo-red staining was negative for amyloid-type material. The gross and histological pathology suggested that the origin of the tumor was either kidney proper or retroperitoneal soft tissue. Patient had a skin biopsy of the scalp lesion, which showed angiosarcoma (Figure 4).
Post-operative PET scan revealed extensive metastatic disease with metastasis to the lung, liver, and bone. The patient was started on a palliative regimen of taxol and sutent. Formal resection of his temporal region lesion was planned, however not completed due to severe side effects the patient experienced during chemotherapy. Approximately three months after his nephrectomy, the patient presented to the emergency department with shortness of breath. He was found to have worsening metastatic disease with bilateral pleural effusions. His condition declined despite drainage of the effusions and his family decided to proceed with end of life care (Figure 5).
Discussion and Conclusion
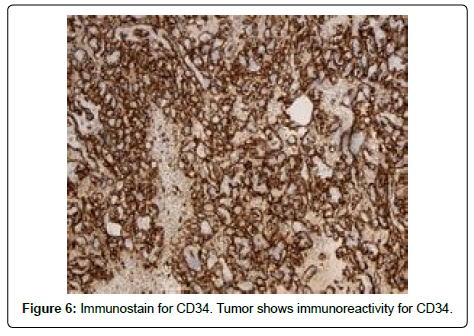
PRA is an extremely rare tumor. Risk factors are not wellestablished but may include renal transplantation and exposure to toxic chemicals including arsenic and vinyl chloride [8]. Due its rarity, there is no well-accepted, well-researched standardized treatment regimen. The majority of the reported cases have been treated with radical nephrectomy. There is no role for partial nephrectomy because it is virtually impossible to distinguish PRAs from renal cell carcinomas without pathological evaluation [9] (Figure 6).
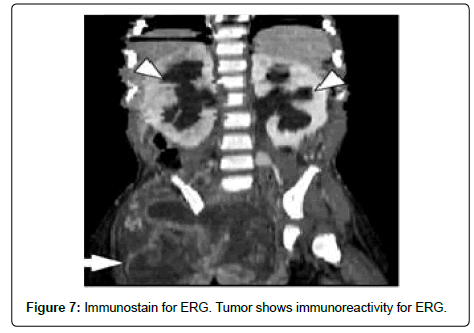
Pathological evaluation of PRA reveals similar findings to primary angiosarcomas from other sites. Microscopic sections show numerous, irregular vascular channels lined by endothelial cells exhibiting varying degrees of pleomorphism, nuclear atypia, multilayering, and mitotic activity. Immunohistochemical studies are generally negative for epithelial markers such as epithelial membrane antigen (EMA) and Cam 5.2 and mostly positive for endothelial markers such as CD31, CD34, and FLI-1 [4] (Figure 7).
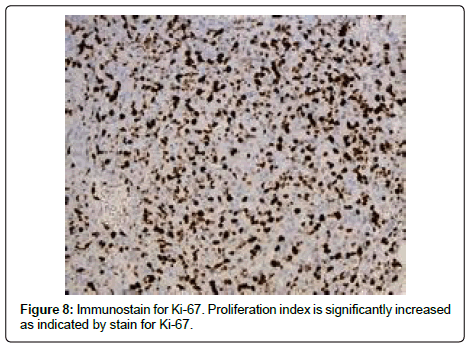
In most cases, radical nephrectomy with adjuvant radiotherapy or chemotherapy is the preferred treatment regimen [3]. Despite optimal therapy, however, local recurrence and distant metastases is common. Prognosis for a patient with PRA is often dictated by the size of the mass at presentation and the presence or absence of metastases [2]. A review by Mark et al. established a size cutoff of 5 cm, with patients presenting with angiosarcomas less than 5 cm having significantly better prognoses [10]. The majority of PRAs, however, present with advanced tumor size; an average of 13 cm at presentation was calculated by Omiyale et al. in a review of 62 cases [4]. In addition, nearly 45% of cases in this review presented with distant metastases [4]. A combination of large tumor size and high likelihood of metastases at presentation contributes to the overall poor prognoses of PRA patients (Figure 8).
PRA is known to spread hematogenously, most commonly to the lungs, liver, and bone. Our case is especially novel, because the skin tumor represented a site of metastasis rather than a primary tumor site Generally, when angiosarcoma is discovered in the kidney, it represents metastasis from a cutaneous or visceral tumor [3]. There has been only one reported case of skin metastasis from PRA in the literature [11].That patient was HIV positive, had significantly suppressed CD4 counts, and died 3 months after diagnosis [11].
PRA is difficult to differentiate from other renal tumors with imaging studies. Consequently, histopathology and immunohistochemistry are paramount for proper diagnosis. There may be a role for CT guided biopsy prior to surgery, but considering the general lack of effective treatment options (most individuals die of the disease despite optimal therapy), a correct preoperative diagnosis unfortunately may not provide any additional benefit to patients.
References
- Lee CH, Park KU, Nah DY, Won KS (2003) Bilateral spontaneous pneumothorax during cytotoxic chemotherapy for angiosarcoma of the scalp: a case report. J Korean Med Sci 18: 277-280.
- Celebi F, Nur PK, Saglam S, Cem BN (2015) Primary renal angiosarcoma with progressive clinical course despite surgical and adjuvant treatment: A case report. Oncol Lett 9: 1937-1939.
- Papadimitriou VD, Stamatiou KN, Takos DM, Adamopoulos VM, Heretis IE, et al. (2009) Angiosarcoma of kidney: A case report and review of literature. Urol J 6: 223-225.
- Omiyale AO (2015) Clinicopathological features of primary angiosarcoma of the kidney: a review of 62 cases. Transl Androl Urol 4: 464-473.
- Fukunaga M (2009) Angiosarcoma of the kidney with minute clear cell carcinomas: a case report. Pathol Res Pract. 205: 347-351.
- Brown CJ, Falck VG, Mac LA (2004) Angiosarcoma of the colon and rectum: report of a case and review of the literature. Dis Colon Rectum 47: 2202-2027.
- Akkad T, Tsankov A, Pelzer A, Peschel R, Bartsch G, et al. (2006) Early diagnosis and straight forward surgery of an asymptomatic primary angiosarcoma of the kidney led to long-term survival. Int J Urol 13: 1112-1114.
- Leggio L, Addolorato G, Abenavoli L, Ferrulli A, Angelo DC, et al. (2006) Primary renal angiosarcoma: a rare malignancy. A case report and review of the literature. Urol Oncol 24: 307-312.
- Zenico T, Saccomanni M, Salomone U, Bercovich E (2011) Primary renal angiosarcoma: case report and review of world literature. Tumori 97: 6-9.
- Mark RJ (1996) Angiosarcoma: A report of 67 Patients and a review of the literature. Cancer 77: 2400-2600
- Adjiman S, Zerbib M, Flam T, Brochard M, Desligneres S, et al. (1990) Genitourinary tumors and HIV-1 infection. Eur Urol 18: 61-63.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi