Case Report, Clin Oncol Case Rep Vol: 5 Issue: 1
Primary Squamous Cell Carcinoma of the Liver
Paul Guzik*, Andrew Gdowski, Christopher Kim, Amanda Rivera-Begeman, Hannah Kay, Declan Fleming, and Gail Eckhardt
Gastroenterology Fellow Physician, Loma Linda University, Los Angeles, USA
*Corresponding Author:
Paul Guzik
Gastroenterology Fellow Physician
Loma Linda University, Los Angeles, USA
E-mail: paul.r.guzik@gmail.com
Received: August 30, 2021, Manuscript No: COCR-21-8005;
Editor assigned: September 02, 2021, PreQC No: P-8005;
Reviewed: October 03, 2021, QC No: Q-8005;
Revised: December 22, 2021, Manuscript No: R-6219;
Published: January 10, 2022, DOI: 10.4172/cocr.5(1).212
Citation: Guzik P, Gdowski A, Kim C, Rivera-Begeman A, Kay H, et al. (2022) Primary Squamous Cell Carcinoma of the Liver. Clin Oncol Case Rep 5:1
Abstract
Primary Squamous Cell Carcinoma (SCC) of the liver is a very rare diagnosis with limited reported cases in the current literature. The prognosis is extremely poor with few patients surviving after 12 months, irrespective of treatment. Here, we report a case of hepatic primary squamous cell carcinoma.
Keywords: Liver cancer; Oncology; Cancer; Hepatic cancer; Rare malignancy; Rare cancer; Primary squamous cell carcinoma of the liver
Case Report
A 60-year old woman presented to our hospital with ongoing abdominal pain and anorexia. She was evaluated one month prior at an outside hospital where she was diagnosed with poorly differentiated SCC by liver biopsy. A palpable, tender abdominal mass in her right upper quadrant was noted on exam. Her liver function tests comprised of an alkaline phosphatase (ALP) 188 u/L (upper limit of normal range (ULN) 121 u/L), aspartate transferase (AST) 71 u/L (ULN 34 u/L), and alanine transferase (ALT) 86 u/L (ULN 60 u/L). Total bilirubin was within normal range. Tumor markers revealed an elevated Carbohydrate Antigen (CA) 19-9 of 56.7 U/mL (ULN 3 U/mL) and CA-125 of 77.7 U/mL (ULN 35 U/mL). Alpha-Fetoprotein (AFP), Carcinoembryonic Antigen (CEA) and CA 15-3 were all within normal limits. Computed tomography (CT) scan of her abdomen revealed a 17 cm necrotic liver mass with mild intrahepatic biliary dilatation and a 1.4 cm left periaortic lymph node (Figure 1). Repeat liver biopsy revealed large areas of invasive SCC in solid nests and interconnecting cores with areas of necrosis (Figure 2). A metastatic cancer workup was negative for a primary tumor outside of the liver.
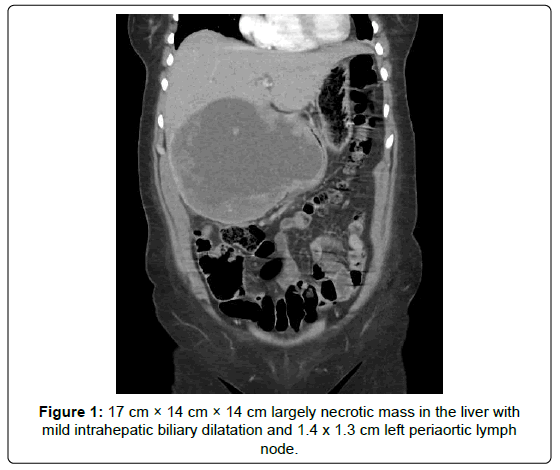
Figure 1: 17 cm × 14 cm × 14 cm largely necrotic mass in the liver with mild intrahepatic biliary dilatation and 1.4 × 1.3 cm left periaortic lymph node.
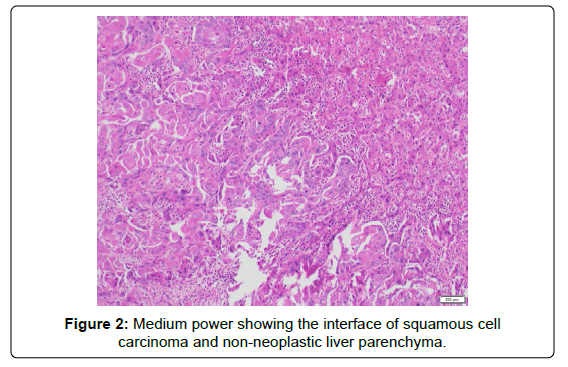
Figure 2: Medium power showing the interface of squamous cell carcinoma and non-neoplastic liver parenchyma.
She underwent a right hepatectomy with resection of the common hepatic and common bile ducts as well as porta hepatis lymph nodes. The distal stomach and duodenum, a segment of the transverse colon, and a portion of the abdominal wall adjacent to the mass were also resected (Figure 3, Figure 4). Pathologic evaluation revealed moderately differentiated SCC of the liver with direct extension into the abdominal wall, stomach and colon. There was evidence of lymphovascular invasion as one of five resected peri-hepatic lymph nodes were positive for metastatic malignancy. All resected surgical margins were free of malignancy. One month after hospital discharge, a PET scan revealed multifocal hypermetabolic metastatic liver lesions with hypermetabolic peritoneal metastases and ascites. She was started on palliative chemotherapy with carboplatin and paclitaxel but unfortunately passed away six months after her initial diagnosis.
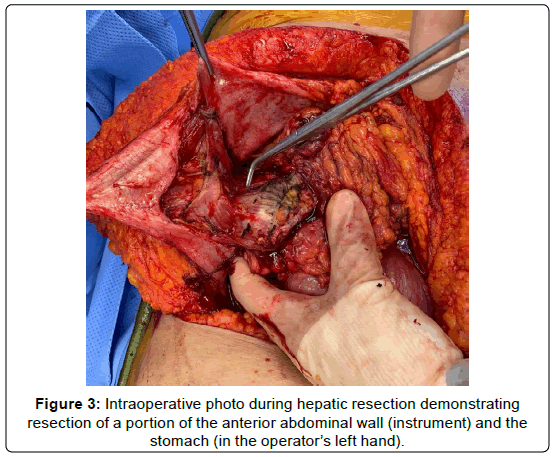
Figure 3: Intraoperative photo during hepatic resection demonstrating resection of a portion of the anterior abdominal wall (instrument) and the stomach (in the operator's left hand).
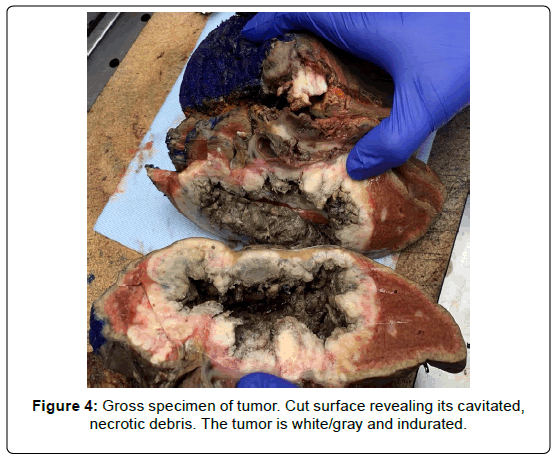
Figure 4: Gross specimen of tumor. Cut surface revealing its cavitated, necrotic debris. The tumor is white/gray and indurated.
Discussion
The pathogenesis of primary SCC of the liver is not completely understood. It is postulated that hepatic cysts undergo a metaplasia- dysplasia transformation progressing from benign to malignant [1,2]. It is also suggested that inflammation in the biliary tract, possibly from stones or infection, may be the inciting step in the development of primary SCC [2]. Additional associations with liver cirrhosis and Caroli’s disease (a rare congenital liver disorder characterized by cystic dilation of intrahepatic bile ducts and renal cysts) have been proposed [3,4]. This patient did not have known cirrhosis, Caroli’s disease, biliary stones or hepatic cysts. In patients with localized disease, primary management should be aimed towards margin-negative surgical resection of the tumor. Patients who undergo surgical resection have a longer overall survival than those who do not (17 vs. 5 months) [1]. Due to the rare nature of this condition, there are no standardized guidelines to direct adjuvant therapy. The presence of nodal metastatic disease may be considered to be an indicator of higher risk for the development of systemic metastasis, and thus a platinum-based chemotherapy regimen was started. Other treatment modalities that have been reported for patients with SCC of the liver include systemic chemotherapy with 5-fluorouracil (FU), hepatic artery infusion chemotherapy, and radiation therapy [1,5].
References
- Zhang XF, Du ZQ, Liu XM, Lv Y (2015) Primary squamous cell carcinoma of liver: Case series and review of literatures. Medicine (Baltimore) 94: e868.
- Nakajima T, Kondo Y (1990) A clinicopathologic study of intrahepatic cholangiocarcinoma containing a component of squamous cell carcinoma. Cancer 65: 1401-1404.
- Spaggiari M, Di Benedetto F, Ballarin R, Losi L, Cautero N, et al. (2011) Primary squamous cell carcinoma of the liver associated with Caroli's disease: A case report. Onkologie 34: 193-195.
- Kaji R, Sasaki N, Tateishi I, Nagata E, Okabe Y, et al. (2003) A case report of primary hepatic squamous cell carcinoma that remarkably responded to low dose arterial injection of anti-cancer drugs. Kurume Med J 50: 71-75.
- Takahashi H, Hayakawa H, Tanaka M, Okamura K, Kosaka A, et al. (1997) Primary adenosquamous carcinoma of liver resected by right trisegmentectomy: Report of a case and review of the literature. J Gastroenterol 32: 843-847.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 