Case Report, Clin Dermatol Res J Vol: 7 Issue: 1
Pseudo Hernia: A Case Report of Post Therapeutic Post Herpes Zoster Motor Neuron Disease
Mohammad Aslam, Maikal Kujur*, Mohammad Nafees Ahamad, Sadiq Hussain and Mohammad Atif Ansari
Department of Surgery, Jawaharlal Nehru Medical College and Hospital, Aligarh Muslim University, Aligarh, Uttar Pradesh, India
*Corresponding Author:Maikal Kujur
Department of Surgery, Jawaharlal Nehru Medical College and Hospital, Aligarh Muslim University, Aligarh, Uttar Pradesh, India
E-mail:maikal4kujur@gmail.com
Received date: 02 December, 2021, Manuscript No.CDRJ-22-52486
Editor assigned date: 06 December, 2021, PreQC No. CDRJ-22-52486 (PQ);
Reviewed date: 20 December, 2021, QC No.CDRJ-22-52486;
Revised date: 27 December, 2021, Manuscript No. CDRJ-22-52486 (R);
Published date: 03 January, 2022, DOI:10.4172/2576-1439.1000177
Citation: Aslam M, Kujur M, Ahamad MN, Hussain S, Ansari MA (2022) Pseudo Hernia: A Case Report of Post Therapeutic Post Herpes Zoster Motor Neuron Disease. Clin Dermatol Res J 7:1.
Abstract
Introduction: Pseudo hernia is defined as bulging of the abdominal wall that is not caused by structural defects rather, frequently due to muscle paralysis. Pseudo-hernia/Phantom-hernia due to herpes zoster is also known as abdominal wall postherpetic pseudo- hernia, herpes zoster-induced abdominal paresis and segmental roster abdominal paresis. Approximately 5% of patients with herpes zoster experience motor complications such as facial palsy, ramsay hunt syndrome, ogilvie’s syndrome or segmental paresis of the limbs. Pseudo hernia due to herpes zoster is also a rare motor complication of herpes zoster and occurs in approximately 0.17% of cases. Elderly and immuno compromised patients are at higher risk of developing motor deficits due to herpes zoster. Motor deficits usually occur in the same or adjacent levels as to where the virus is infected. Generally, abdominal bulging due to herpes zoster is asymptomatic, but when the visceral nerve is involved in the gastrointestinal tracts, colonic pseudo-obstruction and constipation-associated symptoms can concur.
Case report: A 60-year-old male presented to surgery OPD of Jawaharlal Nehru Medical College, Aligarh Muslim University for expansile left-sided flank swelling and discomfort for 2 months. He was admitted with a clinical impression of a left lumbar hernia. Abdominal ultrasonography didn't reveal any abdominal wall defect. Detailed history revealed severe burning pain and vesicles along the left T9-10 dermatome 3 months back. A diagnosis of herpes zoster was made and the patient was given famciclovir for a week. Following which skin lesions improved, though chronic left-sided flank discomfort and mild burning pain remained and bulge appeared after 1 month of treatment. A final diagnosis of Pseudo hernia, the complication of herpes zoster was then made and the patient was kept under close observation. He was tolerating a normal diet. His pain had subsided and was discharged in satisfactory condition. He has been on regular follow up since then.
Conclusion: Pseudo hernia due to herpes zoster usually shows a good prognosis, with self-regression after a few months. In most reported cases, symptoms resolve without treatment between 3 and 12 months after onset. Surgeons should be very aware of both contamination and such unusual presentations.
Keywords: Orofacial acute herpes zoster
Keywords
Phantom-hernia; Pseudo-hernia; Lumbar-hernia; Herpes zoster; Ramsay Hunt Syndrome (Herpes zoster Trigeminal Neuralgia); Ogilvie’s Syndrome; Postherpetic Neuralgia (PHN); Herpes zoster ophthalmicus; Herpes zoster oticus, Orofacial acute herpes zoster (shingles)
Introduction
A hernia is the bulging of part of the contents of the abdominal cavity through a weakness in the abdominal wall [1]. While a pseudo hernia is an abdominal wall bulge that may be mistaken for a hernia but lacks the findings of the abdominal wall that characterizes a hernia. A phantom hernia is a term used to describe bulging usually on either side of the abdomen due to weakness or paralysis of muscle due to neuronal dysfunction. Pseudo-hernia due to herpes zoster is also known as abdominal wall postherpetic pseudo-hernia, herpes zoster-induced abdominal paresis and segmental roster abdominal paresis [2]. Thus, the natural history and treatment of this condition differ from those of a hernia. This is a case report of a pseudo hernia/phantom hernia due to herpes zoster (shingles) induced motor neuron complication [3].
Case Study
A 60-year-old male presented to the Dermatology OPD of Jawaharlal Nehru Medical College, Aligarh Muslim University for left-sided flank severe burning pain and vesicles along the left T9-10 dermatome for 1 day, 2 months back [4-6]. A diagnosis of herpes zoster was made and the patient was given famciclovir for a week. Following which skin lesions improved, though chronic left-sided flank discomfort and mild burning pain remained and bulge appeared after 1 month of treatment (Figures 1 and 2).

Figure 1: Anterior view of patient abdomen with Valsalva.
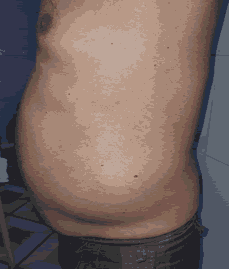
Figure 2: Left lateral view of patient abdomen with Valsalva.
Abdominal ultrasonography didn't reveal any abdominal wall defect. Without a specific cause for his abdominal herniation, the patient was advised to visit the general surgery OPD for further evaluation.
Physical Examination
He was a well build old male with the following vitals:
Pulse rate: 84/minute;
Blood pressure: 134/88 mm of Hg;
Respiratory rate: 18/minute;
Temperature: 99.2 °F;
Oxygen saturation: 100% on room air;
General examination and systemic examination were within normal limits. Upon a per-abdominal examination, we noticed a soft lump in his left mid-abdomen on the left side, just above the level of the umbilicus [7-11]. The lump was expansive with respiration and cough. The abdominal muscle tone was reduced on the left flank. Abdominal ultrasonography was conducted to evaluate the possibility of abdominal hernia, but it doesn’t show signs of hernia. His blood investigations were within normal limits. The bowel sounds were normal.
Management
Pseudo hernia associated with herpes zoster was then diagnosed, and the patient was kept under close observation. He has advised a waistband for strengthening abdominal muscle as a conservative treatment for pseudo hernia. The patient was tolerating a normal diet. His pain had subsided and was without any untoward incident. He has been on regular follow up since then.
Discussion and Conclusion
Herpes zoster usually occurs from viral multiplication and spreads within the dorsal root ganglia (the sensory axons), causing severe pain and postherpetic neuralgia among its main complications. However, motor complications can occur when the virus attacks the ventral root (motor axons). Approximately 5% of patients with herpes zoster experience motor complications such as facial palsy, Ramsay Hunt syndrome, Ogilvie’s syndrome or segmental paresis of the limbs. Pseudo Hernia due to herpes zoster is also a rare motor complication of herpes zoster and occurs in approximately 0.17% of cases. A pseudo hernia is defined as bulging of the abdominal wall that is not caused by structural defects, collection of fluid, or a mass but, rather, muscle paralysis. Elderly and immuno compromised patients are at higher risk of developing motor deficits due to herpes zoster. Motor deficits usually occur in the same or adjacent levels as to where the virus is infected. Generally, abdominal bulging due to herpes zoster is asymptomatic, but when the visceral nerve is involved in the gastrointestinal tracts, colonic pseudo-obstruction and constipation-associated symptoms can concur. A few hypotheses have been made to explain the pathogenesis of visceral involvement. The first is the direct invasion of varicella-zoster virus in the intrinsic intestinal autonomic nervous system. Another hypothesis is that the vesicular eruption can cause visceral peritoneal inflammation, thus causing pain or constipation in the gastrointestinal tract. The final explanation is the involvement of autonomic ganglion caused by the infection of the ventral horn of the spinal cord. A diagnosis of pseudo hernia due to herpes zoster is based on clinical suspicion with previous or present history of herpes zoster and abdominal-wall bulging that is not associated with a structural defect. For evaluation, EMG can be used to detect any nerve-conduction abnormality in the abdominal wall muscles.
Pseudo hernia due to herpes zoster usually shows a good prognosis, with self-regression after a few months. In most reported cases, symptoms resolve without treatment between 3 and 12 months after onset. Surgeons should be very aware of both contamination and such unusual presentations.
Consent
Well informed and written consent had been taken from the patient in his language.
Ethical Clearance
Ethical clearance has been taken from the institutional ethical committee.
References
- Yagi Y, Matono T, Nakamura K, Imura H (2018) Postherpetic abdominal pseudohernia: A diagnostic pitfall. J Gen Fam Med 19: 36-37. [Crossref], [Google Scholar] [Indexed]
- Yoo J, Koo T, Park E, Jo M, Kim MS, et al., (2019) Abdominal pseudohernia caused by herpes zoster: 3 case reports and a review of the literature. JAAD Case Rep 5: 729-732. [Crossref], [Google Scholar], [Indexed]
- Ohno S, Togawa Y, Chiku T, Sano W (2016) Postherpetic pseudohernia: Delayed onset of paresis of abdominal muscles due to herpes zoster causing an ipsilateral abdominal bulge. BMJ Case Rep 2016. [Crossref], [Google Scholar], [Indexed]
- Nair P, Pariath K (2018) Abdominal wall herniation after herpes zoster. Indian Dermatol Online J 9: 278. [Crossref], [Google scholar]
- https://www.cdc.gov/shingles/hcp/clinical-overview.html.
- Gross G (2006) Herpes zoster. In: Recent Aspects of Diagnosis and Control. Karger 26: 20-36.
- Masood I, Majid Z, Rind W, Zia A, Riaz H et al. (2015) Herpes zoster-induced Ogilvie’s syndrome. Case Rep Surg 2015: 563659. [Crossref];[Google Scholar];[Indexed]
- Zaladonis AG, Applebaum D, Hsu S (2021) Painful abdominal outpouching in an adult male. Cureu 13: e12416. [Crossref], [Goggle scholar]
- Lee JY, Sunwoo JS, Kwon KY, Lee KB, Ahn MY et al. (2019) Postherpetic pseudohernia: Lesion localization using thoracic spine magnetic resonance imaging. J Clin Neurol 15: 262-4. [Crossref], [Google Scholar]
- Yu YH, Lin Y, Sun PJ (2019) Segmental zoster abdominal paresis mimicking an abdominal hernia: A case report and literature review. Medicine Baltimore 98: e15037. [Cross ref], [Google Scholar]
- Riopelle A, Kim D, Dayal A (2020) Spontaneous resolution of abdominal pseudohernia after herpes zoster. Am J Med 133: e102-3. [Crossref] [Google Scholar]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 

