Research Article, J Neurosci Clin Res Vol: 7 Issue: 1
A Clinical Study of Spinal Dysraphism Cases in Tertialy Care Center, Kakinada, Andhra Pradesh
M Premjit Ray1 and Kodali Sandhya2*
1Professor and HOD, Department of Neurosurgery, Rangaraya Medical College, Kakinada, Andhra Pradesh, India
2Final Year Resident, Department of Neurosurgery, Rangaraya Medical College, Kakinada, Andhra Pradesh, India
*Corresponding author: Kodali Sandhya, Department of Neurosurgery, Rangaraya Medical College, Kakinada, Andhra Pradesh, India
Tel: +919849379789; E-Mail: sykodali@icloud.com
Received date: 07 December, 2021, Manuscript No. JNSCR-22-56927;
Editor assigned date: 09 December, 2021, PreQC No. JNSCR-22-56927(PQ);
Reviewed date: 23 December, 2021, QC No JNSCR-22-56927;
Revised date: 28 December, 2021, Manuscript No. JNSCR-22-56927(R);
Published date: 07 January, 2022, DOI: 10.4172/JNSCR.1000125
Citation: Sandhya K, Premjit Ray M, et al (2022) A Clinical Study of Spinal Dysraphism Cases in Tertialy Care Center, Kakinada, Andhra Pradesh. J Neurosci
Abstract
Background
We encounter cases of spinal dysraphism in our hospital very frequently. There is no documented evidence on the total number of population affected with Spinal Dysraphism available in our area .This prompted us to conduct the clinical study of spinal dysraphism cases in Rangaraya Medical College , Kakinada , Andhra Pradesh.
Introduction
In India, neural tube defects are the most common congential abnormality noted in every corner of the country in all communities. Most of the mothers are primi gravida with poor awareness of preconceptual supplementation. In our country inspite of regular government run programmes of mother & child care, we get to see these cases very often. There is lot of apprehension post birth of an abnormal child in the family.
Materials & Methods: This is a Prospective Longitudinal study. All patients with complaints of spinal dysraphism coming to the department of neurosurgery , GGH ,under Rangaraya medical college kakinada during the period of October 2015- December 2017 were included in the study after taking informed consent from parents/guardians. All patients were analysed as per our study protocol.
Results: A total number of 30 patients have been included in the study. Preconceptual folate usage only in 2 , Prenatal folate usage in all patients ,Premature delivery in 8, Age of presentation was less than 1 month in 46.6% , Female infants more affected , Lumbar region was the most common site of presentation , Total paraplegia in 46.6%, Surgical outcome – 4 had hydrocephalus , 7 had respiratory infections , 12 had wound infection ,5 mothers had one previous abortion, other anomalies detected are Tetralogy of Fallot in one and single kidney cyst in one baby. Conclusion: Spinal dysraphism cases were frequently seen in clinical practice in GGH, kakinada. Majority were from low socioeconomic group of rural background with less awareness of preconceptual folate usage .Mothers with previous miscarriages had NTD in present child birth. Spinal dysraphism management and prognosis depend on early diagnosis and prompt treatment at the earliest.
Keywords: Clinical Study, Spinal Dysraphism, Spina bifida, Anthropology, Etiology
History
Spina bifida or spinal dysraphism have been present as long as man has walked the planet. Anthropology excavations from 200 AD have shown spinal dysraphism findings from Mexico [1] varying degrees of dyraphism of spine have been evident for centuries,as indicated in Ferembachâ??s anthropology report [2] [Figure 1&2].

Figure 1: Anthropology Excavation from Mexico

Figure 2: Illustration of Van Forest.
The first modern record of a child with spina bifida - incomplete closure of the neural tube - is from 1587, documented by dutch physician Peter Van Forest [3], though there is evidence that spina bifida existed in ancient civilizations well before the modern era.
In 1610 Van Forest performed the first recorded surgical resection of the myelomeningocele sac. The first illustrated example of spinal dysraphism appeared in a textbook entitled Observationes Medicae, first published in 1641Anatomic illustrations of spina bifida are first seen in Tulpius [4], described this lesson as â??nervorum propagines tam varie per tumorem dispersas (the prolongations of the nerves scattered in different directions through the tumor).
In the 1700s and 1800s great advancements were made in the understanding of spina bifida, its etiology, and its clinical consequences, spearheaded by Morgagni in 1761. Over a century later, Lebedeff theorized that myelomeningocele is due to a failure of the neural tube to close, and in 1886, von Recklinghausen described the types of spina bifida and the surgical treatments available.
The term spinal dysraphisma (also known as spina bifida, spinal defect, defect of the neural tube, open/cleft spine), was coined by B.W. Lichtenstein in 1940, [5] referring to a pleomorphic group of skin and neuronal disorders
Dutch surgeon and anatomist, Frederik Ruysch (1638-1731), published the first extensive spina bifida series, ten cases, in 1691 The surgical series of spina bifida patients, published by Fraser in 1929, looked at patients operated on between 1898 and 1923, and reported that two thirds were alive at hospital discharge, with 23% still alive at 6 years follow-up.
The major breakthrough in the treatment of children with spina bifida was the development of the ventriculoatrial shunt in the 1950s, ushering in the age of modern shunting and allowing for the treatment of hydrocephalus, which is almost uniformly associated with myelomeningocele.
Introduction
Spina bifida literally means a spine in two parts or open spinea [6] Spinal dysraphism involves a spectrum of congenital anomalies resulting in a defective neural arch through which meninges and/or neural elements herniate leading to a variety of clinical manifestations [7]. They are divided into aperta (visible lesion) and occulta (with no external lesion). Meningocele, myelomeningocele, lipomeningomyelocele, myeloschisis and rachischisis are the usual names associated depending on the pathological findings.
Prevalence
The estimated incidence of spinal dysraphism is about 1 3/1,000 live births [7-9].The prevalence of spinal dysraphism has been on the decline world over in the last few decades due to better nutrition for women, folic acid supplementation, improved antenatal care and high resolution ultrasound for prenatal screening and biochemical markers. High prevalence noted in under developed & developing countries. Low prevalence noted in developed countries [9].
Aims & Objectives
To study the epidemiological pattern of spinal dysraphism in the patients coming to Government General Hospital ,under Rangaraya Medical College , Kakinada.
1) To Study the epidemiological patterns of spinal dysraphism.
2) To evaluate the surgical treatment of spinal dysraphism.
3) To study the post-operative outcome.
Materials & Methods
All Patients with complaints of spinal dysraphism coming to the department of neurosurgery in Government General Hospital under Rangaraya Medical College, Kakinada.
A Prospective Longitudinal study conducted from October 2015 to December 2017, a total of 30 patients were included in the study after taking informed consent from parents/guardians.
Statistical analysis done using Microsoft Excel software and SPSS computer program. Inclusion criteria:
1) Patients with swelling on the back anywhere from cervical to sacral region over the spine
2) Patients with open defect of the spine in midline Exclusion criteria:
â?¢ Patients with other forms of NTD occipital encephalocele
â?¢ Patients with only occult spinal dysraphism scars/discolouration/tuft of hair The following details were noted for all the patients
Detailed clinical examination (Physical and Systemic examination) Imaging MRI Whole Spine, x ray spine, USG abdomen
Surgery Excision & Reconstruction of neural tube & preservation of neural elements.
Results and Discussion
In the 30 patients treated in our hospital [Table 1-6].
Table 1: Age distribution of patients.
Table 2: Sex distribution in various age groups.
Table 3: Wt of babies.
Table 4: Site of presentation of lesion.
Table 5: Degree of paresis / functioning of LL.
Table 6: Folic acid usage.
In India the initial reaction of parents and family on seeing a newborn baby with a swelling in the back over the spine or open defect is a big fear, both for the sustainment of life of the new born and the future life of the baby. This anxiousness and fear immediately seek the help of the nearest available medical personnel irrespective of the place. They are then directed to a qualified neurosurgeon at the earliest from the local centre.
These days prenatal ultra-sonogram is giving information of the existing malformations prior to the delivery. Parents are then counseled for the necessary precautions and for terminations in unavoidable circumstances. With increasing awareness among the common public population, The following studies were used for comparing data & Analysing in our study [10].
There were 30 cases in the present study with age varying from 1 day to 10 yrs of age, with a mean age of 24 days. Its correlating with studies conducted in the Asian subcontinent [Table 7].
Table7: Studies conducted in the Asian subcontinent.
Premature deliveries were present in 8 children and term delivery in 22 children most of the babies weighed between 1500grams to 2500 grams, with most centred at 2000 +/- 200 grams.
In our study in 30 patients, 18 were females and 12 males. Female preponderance was noted in our study. There was male preponderance in few studies. [Table 8].
Table 8: In our study in 30 patients, 18 were females and 12 males. Female preponderance was noted in our study. There was male preponderance in few studies
Swelling in the posterior aspect of spine was the symptom of presentation for all the children. Ruptured swelling was present in 11 children. Out of 11, 8 had continous leak of CSF, 3 children had thick serous discharge from the swelling due to secondary infection. 4 children presented with signs of meningism [Table 9].
Table 9: Swelling in the posterior aspect of spine was the symptom of presentation for all the children.
Clinical presentation to the hospital - more than half of the children presented to hospital immediately within 1 week of child birth. Thereafter there was equal presentation in all age groups till the age of 10 years. [Table 10] [Clinical Photographs]
Table 10: Clinical presentation to the hospital
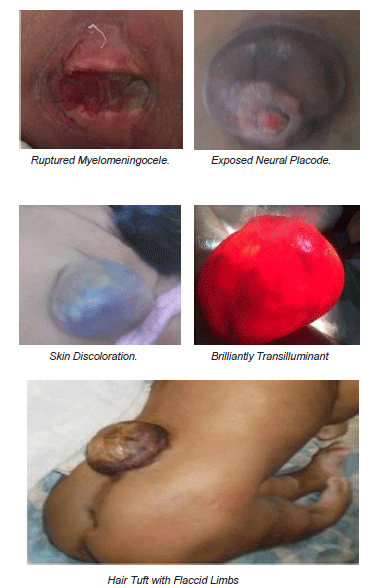
Size of the lesion ranged from 2cm to 12cm with a mean of 6.5cm in length. Width ranged from 1cm to 7.5cm with a mean of 4cm [Table 11].
Table 11: Size of the lesion ranged from 2cm to 12cm with a mean of 6.5cm in length.
Site Of Presentation - lumbar was commonest region, followed by sacral region. Dorsal & cervical regions had less frequency of presentation in our study [Table 12].
Table 12: Site of Presentation
Degree of Lower limb paresis- complete paralysis had no improvement. Children with normal power of lower limbs have not deteriorated in our study [Table 13] [MRI Photographs].
Table 13: Degree of Lower limb paresis- complete paralysis had no improvement.
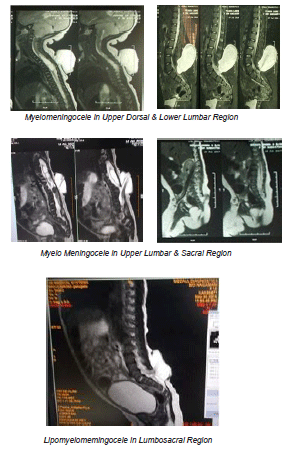
Foot Abnormality - congenital talipus equino varus abnormality was noted in almost all cases of complete lower limb paralysis. Ortho paedician consultation was advised for children in the follow up period.
Bowel Incontinence could not investigated in our centre. We performed anal tone examination with per rectal examination. Features of Patoulous opening with lax sphincter contraction were considered as children with incontinence. Head Circumferenceâ?? average head circumference of the child ranged from 34-38 cms. Children with increased head size with respect to age were evaluated without symptoms of hydrocephalus or raised ICP [Table 14].
Table 14: Average head circumference of the child ranged from 34-38 cms.
Anterior Fontanelle was lax in children without any symptoms. In children with Arnold chiari abnormalites , post-operative hydrocephalus was noted. Anterior fontanelle served as single clinical criteria along with head circumference to monitor the CSF dynamics and diversion after primary surgery for the spinal dysraphism.
Growths of Child / Milestones were delayed in children with total paralysis of lower limbs. Other children could reach milestones as per age. Neck holding, sitting, crawling, standing with support and walking were delayed in some children and completely absent in children with lower limb paresis. [Table 15] [Chart 1], [Intra OP Photos]
Table 15: Growth of Child/ Milestones were delayed in children with total paralysis of lower limbs.
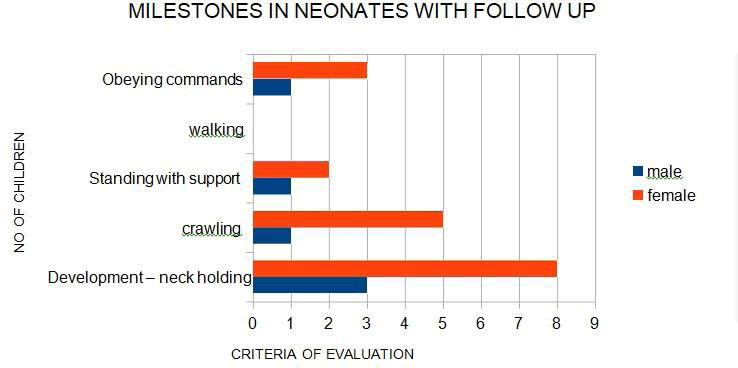
Chart 1: Growth of child/ attainment of milestones
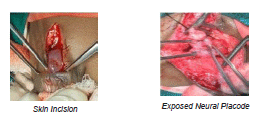
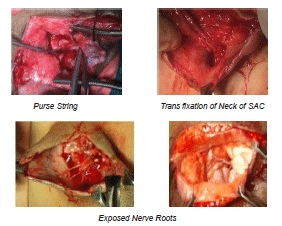
Social smile, recognizing people, holding objects, obeying commands, speech were delayed in few children with Arnold chiari abnormalities. However overall developmental delay was quite evident clinically.
Presence Of Hydrocephalus - 2 children had primary hydrocephalus and were managed with VP shunt prior to surgery for spinal defect. 4 children developed hydrocephalus post operatively within 1 month duration of initial surgery. All children were taken up for CSF diversion procedure - VP shunt. Hydrocephalus was controlled post operatively for all children [Table 16].
Table 16: Presence of Hydrocephalus.
Consanguineous Marriage of their parents was there in 13 children. Commonest noted was 2nd degree relative marriage. 2 couples used contraceptives. Preconceptual folic acid was used by 3 parents only. Twenty eight mothers out of 30 used prenatal supplementation of iron, folic acid & calcium [Table 17].
Table 17: Usage of Preconceptual folic acid.
Family History of NTD was evident in 3 children, 24 fathers had addictions, and 2 mothers had addictions to local alcohol & smoking habits. Commonly seen were parents with 2 children in almost half of the study - with second child affected, 6 couples had 3 children with 3rd child being affected & for 8 couples the affected child was their first child [Table 18].
Table 18: Family History of NTD.
Seventy five percent of our parents were from rural background. Ninty percent of parents from low socioeconomic status group. Twenty eight mothers attended antenatal clinics in all trimesters in our study. Two mothers attended antenatal clinics in the third trimester [Table 19 & 20].
Table 19: Socioeconomic status group.
Table 20: Antenatal clinics in the third trimester.
Age of Mother at Conceiving of the first child â?? the youngest was 16 yr old and 26 being the oldest mother. The average range of age of conceiving the affected child was 19-22 years. Abortions of Mother in Previous Pregnancies were noted in 8 mothers. 2 mothers had bad obstetric history [Table 21] [Chart 2].
Table 21: Abortions of mother in previous pregnancies.
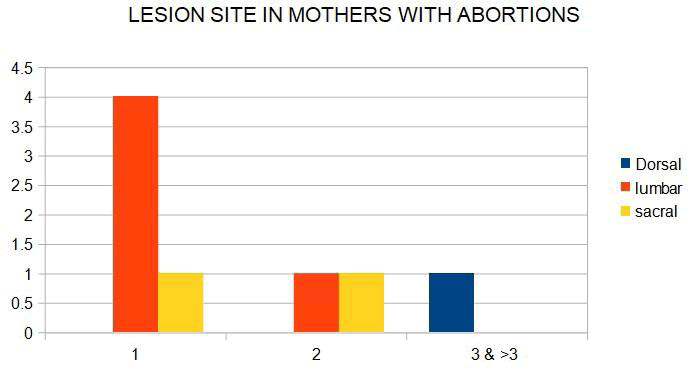
Chart 2: Lesion site in mothers with abortions
Associated Chiari Malformations were noted in almost all patients excepting a few children with sacral lesions [Table 22].
Table 22: Associated Chiari Malformations were noted in almost all patients excepting a few children with sacral lesions.
Other Anomalies detected were tetralogy of fallot and Single kidney cyst in one child each in our investigative follow-up [Table 23]. Picu Period of Stay Pre-Op/Post-Op: children with respiratory infections and low birth weight babies with failure to thrive were nourished in PICU pre operatively for necessary period and then taken up for surgery. Children with poor respiratory compliance were kept on ventilator in post-operative period for required time period. 4 children were shifted to PICU on grounds of aspiration. 6 children developed features of meningism and were treated in PICU till cured [Table 24] [Post OP Scar Pictures].
Table 23: Other anomalies detected were tetralogy of fallot and single kidney cyst in one child each in our investigative follow up.
Table 24: Children with poor respiratory compliance.
Surgical Outcome: all the children with ruptured swellings were treated at the earliest date with fitness of the child [Chart 3]. Wound site infection was the common complication noted. Staphylococcus aureus, pseudomonas & kliebsella were the organisms commonly isolated. Drug sensitivity was present for inj sulbacef, inj piptaz, inj meropenam & inj gentamycin [Table 25].
Table 25: Drug sensitivity was present for inj sulbacef, inj piptaz, inj meropenam & inj gentamycin.
Reconstruction of Flaps was performed with the assistance of our hospital plastic surgery department. Preoperatively the patients were consulted for neccesary intervention. A total of 4 patients out of 30 underwent reconstruction of flaps. There was infection in 2 children, subsided with intravenous antibiotics and local dressing care [Table 26].
Table 26: Reconstruction of flaps was performed with the assistance of our hospital plastic surgery department.
Degree Of Improvement - there was no improvement in cases with total paralysis of the limbs. In 3 children with reflex movements for pain stimulus, there has been one grade improvement of power. Not much significant improvement noted in the power of the lower limbs in the children with paretic limbs [Table 27].
Table 27: Degree of improvement – there was no improvement in cases with total paralysis of the limbs.
Complications attained were wound leak in 7 cases. Subsided in 6 cases with higher antibiotics (inj sulbacef, inj piptaz , inj meropenam) , local wound care & re- repair done in 1 patient. One child presented with recurance of the swelling in the suture site [Table 28].
Table 28: Complications attained were wound leak.
Four children developed hydrocephalus in the post-operative period within one month of surgery for spinal dysraphism. Wound infection in occurred in 12 children. It was very high when compared with other studies. Staphylococcus aureus, pseudomonas & kleibsella were the organisms commonly isolated in the wound swab sent for culture & sensitivity [Table 29].
Table 29: Staphylococcus aureus, pseudomonas & kleibsella were the organisms commonly isolated in the wound swab sent for culture & sensitivity.
Follow Up: 24 children came up for follow up for atleast once and more than half of them were followed up for a period of 3-6 months. 3 deaths occurred. Lost follow up for 3 children after discharge from hospital due to various reasons [Table 30].
Table 30: Follow Up
During follow up most of pre-operative deficits persisted, wound healing was delayed in children with post op infection.. Neurological developmental status and milestones were behind the expected age of development. Most of children could not walk due paresis.
Total Hospital Stay: average stay was about 3 weeks for children from admission to surgery and discharge.
Four children expired in our study due to various reasons. The deaths in other studies were as follows: [Table 31]
Table 31: The deaths in other studies.
Limitations of Study
Small sample size â?? the present study had only 30 patients.
Regional variation (rural set up of our hospital) â?? 80 % of our patients
come from rural background. Poor follow up
Recommendations for Further Study:
Large Sample size
Awareness among public by Anganwadi workers and mid wives Analysis for etiopathogenesis. Folic acid supplementation in preconceptual period has to be encouraged in fertile women.
Conclusion
Spinal dysraphism management and prognosis depend on early diagnosis and prompt treatment at the earliest.
In our study
- The epidemiological prevalence of spinal dysraphism is high in our region in comparison to other studies.
- Ninety percent of our parents were from low socioeconomic group
- Three fourth of our study population was from rural background
- Consanguinity had less role in our study
- Family history of NTD had fewer roles in our study
- All mothers were below 25 years of age
- Mothers with previous miscarriages had children with NTD in present child birth
- Second child of the parents were commonly affected in our study
- All children were taken up for surgery with adequate preparation
- Reconstruction was done for children with inadequate skin flap for closure
- No new neurological deficits were noted in postoperative period
- Two preoperative & two post-operative hydrocephalus were identified and treated
- Infection rate was 40% in our study due to delayed surgery.
- Ninty percent of our patients were followed up and ten percent lost follow up.
References
- Ferembach D (1963) Frequeny of spina bifida occulta in prehistoric human skeletons. Nature 199: 100â??101. [Crossref], [Google Scholar], [Indexed]
- Lichtenstein BW (1940) Spinal Dysraphism: Spina bifida and myelodysplasia. Arch Neuro Psych 44: 792-810. [Crossref], [Google Scholar], [Indexed]
- Harwood-Nash DC, McHugh K (1991) Diastematomyelia in 172 children: the impact of modern neuroradiology. Pediatr Neurosurg 16: 247â??51. [Crossref], [Google Scholar], [Indexed]
- De Jong TP (1993) Peroperative anaphylactic reactions due to latex allergy. Ned Tijdschr Geneeskd. 137: 1934â??1936. [Crossref], [Google Scholar], [Indexed]
- Goodrich JT (2008) A historical review of the surgical treatment of spina bifida. Springer Milan pp. 3-17. [Crossref], [Google Scholar]
- Kumar R, Singh (2003) N:Spinal dysraphism trends in north India. paediatric neurosurgery 38: 133-145. [Crossref], [Google Scholar], [Indexed]
- Samples DC, Tarasiewicz I (2016) Review and Classification of Occult Spinal. Dysraphism and Tethered Cord Syndrome in Children. J Spine 5: 325. [Crossref], [Google Scholar]
- Sidram V, Kumar PCC, Raghavendra B, Sangreshi V (2015) A Prospective Study of Spectrum of Spinal Dysraphisms and its Surgical Outcome. J Spinal Surg 2: 72-77. [Crossref], [Google Scholar]
- Dhingani DD, Boruah DK, Dutta HK, Gogoi RK (2016) Ultrasonography and magnetic resonance imaging evaluation of pediatric spinal anomalies. J Pediatr Neurosci 11:206-212. [Crossref], [Google Scholar], [Indexed]
- Bauer SB, Labib KB, Dieppa RA, Retik AB (1977) Uro-dynamic evaluation of boy with myelodysplasia and incontinence. Urology 10: 354-362. [Crossref], [Google Scholar], [Indexed]
- Kafle P, Sushil K (2017) Spinal dysraphism common entity in neurosurgery. Nepal journal of neurosciences 14: 2-6. [Crossref], [Google Scholar]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi