Research Article, J Addict Behav Ther Rehabil Vol: 9 Issue: 1
Effectiveness of Peak Flow Meter Exercises to Improve Atelectasis after Surgery Involving Sternotomy
Abdul Jalil Khan*, Sairish Sairien, Hina Khattak, Ayesha Razzak, Maryam Azeem and Samina Naz
Physiotherapy Department of Different Hospitals, Kohat, Pakistan
*Corresponding Author : Abdul Jalil Khan
Physiotherapy Department of Different
Hospitals, Kohat, Pakistan
Tel: +923319037749
E-mail: ajk2005_jalil@yahoo.com
Received Date: December 09, 2019; Accepted Date: December 18, 2019; Published Date: December 28, 2019
Citation: Khan AJ, Sairien S, Khattak H, Razzak A, Azeem M, et al. (2019) Effectiveness of Peak Flow Meter Exercises to Improve Atelectasis after Surgery Involving Sternotomy. J Addict Behav Ther Rehabil 9:187. doi:10.37532/jabtr.2020.9(1).187
Abstract
Background: In the current time cardiopulmonary disorders are the most common cause of death and disability among which atelectasis has now become an advanced disease in Pakistan and all over the world. Atelectasis is a condition in which one or more areas of your lungs collapse or don't inflate properly which is appeared with high morbidity and mortality. There appears to be no published data on Peak flow meter exercises and effects of Peak flow meter exercises on atelectasis in Pakistan or in the world. The purpose of this study is the advancement and role of Peak flow meter exercises after atelectasis.
Study Objective: To determine the effectiveness of Peak flow meter exercises on atelectasis.
Methodology: A total of 56 patients were selected post atelectasis with a complaint of absent or decreased air entry in lung bases. All the patients were selected by non-probability convenient sampling and distributed randomly into control (n=28) and experimental (n=28) groups. A well-designed questionnaire was used for the collection of data. The assessment before and after Peak flow meter exercises was done and different variables (auscultation scale, arterial blood gases and dyspnea Borges scale) were noted. General physical therapy protocol was given to all patients but Peak flow meter exercises were added for the experimental group.
Results: Different variables were analyzed and the experimental group shows highly significant (p<0.05) in the improvement of lung sound and x-ray. It was also noted that the Borges Dyspnea scale (p<0.5) and auscultation scale (p<0.05), partial pressure of carbon dioxide (p<0.05) all found highly significant in the experimental group, but the PO2(p>0.5) and SO2(p>0.05) was not found significant due to lack of control on oxygen flow in the patients.
Conclusion: These findings suggest that Peak flow meter exercises are effective to improve lung expansion in atelectasis patients. The improvement of the experimental group was early as compare to the control group. The potential for administration of technique was safe and proved to be very effective for the improvement of atelectasis
Keywords: Atelectasis; Dyspnea borges scale; Peak flow meter exercises
Introduction
In recent times cardiopulmonary diseases are the most common cause of death and disability among which atelectasis has now become an advanced disease in Pakistan and all over the world. Furthermore according to international studies respiratory problems are most leading cause of death and loss of lung volume is noted routinely after atelectasis. Furthermore, atelectasis appears with high morbidity and mortality after surgery involving sternotomy which occurs approximately 7.4 cases-18 cases per one lac population per annually in men and 1.2 cases-6 cases per one lac population per annually in women’s [1].
However, there appears to be no published data on peak flow meter exercises and effects of peak flow meter exercises on atelectasis in Pakistan or in the world. The purpose of this study is the advancement and role of cardiopulmonary physical therapy (peak flow meter exercises) after atelectasis. This led to increased interest for the researchers to investigate the relationship between specific active peak flow meter exercises and the role of intensive care physical therapy. The researcher was also interested in introducing an evidence-based approach in intensive care physical therapy and its role to regain normal lung volume and to overcome the respiratory crisis [2].
As we know that atelectasis is very advanced but a major procedure so it may give rise to multiple complications, some of them are discussed as above. There are different factors which interfere with normal respiratory mechanics due to atelectasis i.e. pain due to sternotomy and air presence in the pleural space which leads to guarded breathing, increased mucus production and decreased mucociliary clearance (post general anesthesia effects) are some of the important causes which affect the gas exchange and promote hypoxia, hypercapnia and tachypnea [3]. In these circumstances, if the patient also develops decrease lung compliance due to air in the lung then it may lead to increase pleural pressure and comprises lung expansion causing further deterioration of the condition.
As we know that in atelectasis there is a decrease the lung compliance, due to which one or more areas of the lungs collapse or don't inflate properly it can also affect the movement of the doom shape of the diaphragm, which is the principal muscle of respiration. It can also affect arterial blood gasses. It can also affect lung volumes and capacities and as whole chest pain is increased and the patient can breathe very hard. So in this way atelectasis severely affects respiratory mechanics and hence it may decrease lung compliance and aids in the severity of condition further [4].
Many studies suggest a relationship between peak flow meter exercises (positive pressures) with atelectasis but the relationship between peak flow meter exercises and atelectasis is not properly determined yet because there is no published data or evidence found on the relationship between peak flow meter exercises and atelectasis. As we know that physiotherapy is becoming a very advance field and it has also many sub-fields among which the pulmonary system is a much-neglected system by the Physiotherapists [5,6].
A peak flow meter is a simple and very low price device which is used for measuring how well the air moves away from your lungs. Measuring your peak flow using this meter is an important part of managing your asthma symptoms and preventing an asthma attack.
Methodology
This study was done on admitted patients of atelectasis at Lady Reading Hospital (LRH) Peshawar Pakistan from August 2015 to January 2016. A total of 56 patients were included in this study as per the inclusion and exclusion criteria. Patients were selected by nonprobability convenient sampling and then distributed randomly into control (n=28) and experimental (n=28) groups.
General physical therapy protocol (mobilization, static walk, breathing exercises and in bed activity) given to both the groups were the same but active peak flow meter exercises were performed only by the experimental group. Different tools were used in this study like auscultation scale of the chest, Arterial Blood Gases (ABGs) and dyspnea Borges scale. All these variables were analyzed by SPSS 20 [7].
After coordination of supervisor, co-supervisor, peer review, intensivist, and national cardiopulmonary Physiotherapists a good structure strategy and questionnaire were prepared and this questionnaire was used to collect the data from the control group and experimental group. As the pre-treatment assessment was done and different variables were noted which includes auscultation scale of the chest, Arterial Blood Gases (ABGs) and dyspnea Borges scale which is also known as modified Borg scale for perceived dyspnea or Shortness of Breath (SOB) [8].
Then general Physical therapy treatment was given to both the groups i.e. control group and experimental group, but 2 hourly 20 active peak flow meter exercises were performed by each patient in the experimental group. The patients in the experimental group were instructed to inhale as much air as they can and then exhale the air through peak flow meter slowly which gives a positive pressure on the lungs to improve the lung compliance and to improve the Arterial Blood Gasses (ABGs) and also to improve the lung volumes and capacities.
Furthermore, an instructor was also there to perform the active peak flow meter exercises in front of the patients in the experimental group. While instructing the patients in the experimental group the instructor instructs them to inhale as much air as they can and then exhale the air through the peak flow meter slowly and gently. The same session was repeated two [2] hourly in the morning and evening shifts. And then progress was noted through questionnaire twice/24 hours. And these protocols were followed for a week. On duty, the medical officer was involved to grade the chest movements by auscultation. While the other 28 patients which were in the control group were following the general physical therapy protocol which includes mobilization, static walk, chest physiotherapy, breathing exercises and in bed activity according to the standard operating procedures as per hospital policy [9,10].
Results
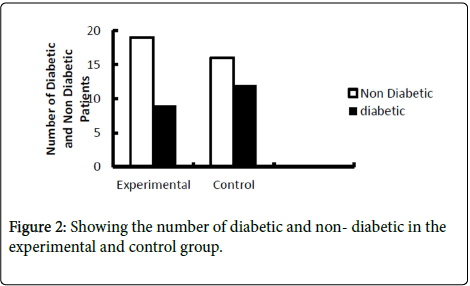
The mean age of the experimental and control group was (53.86 ± 5.104) and (53.25 ± 5.372) years respectively. Patients gender consists 39 male (Experimental 20, Control 19) and 17 females (Experimental 09, Control 08), 18 smokers (8 experimental, 10 control group) 21 with diabetes (09 experimental, 12 control group) as per Pulmonary function scale, on the first day mean was noted 4.00 ± 0 for both experimental and control group but on the third-day post- chest tubes mean for experimental group (1.00) and control group (1.43 ± 0.504) highly significant (p<0.05) which shows the marked difference regarding improvement of pulmonary function test in experimental group.
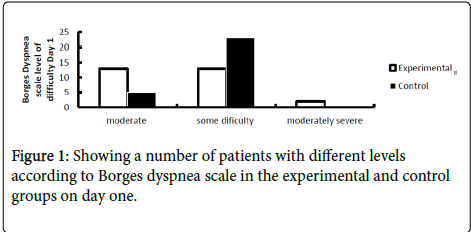
The mean partial pressure of oxygen for experimental group (134.29 ± 15.731) and (122.68 ± 10.267), for control group (124.61 ± 21.808) and (121.36 ± 11.126) on first and third-day post-atelectasis respectively with non-significant (p>0.05) As oxygen flow was not in our control in the study, as well as due to ethical consideration it was compulsory to keep the partial pressure of oxygen up to optimum, so we get non-significant p-value. Borges dyspnea scale mean for experimental group (5.61 ± 0.629) and (1.21 ± 0.738), for control group (5.82 ± 0.390) and (3.18 ± 0.863) on first and third postatelectasis day respectively highly significant (p<0.05) this scale is also showing the better recovery in experimental group and further aid in effectiveness of technique (Figures 1 and 2; Tables 1 and 2).
| Group | Patient Gender | ||
|---|---|---|---|
| Male | Female | Total | |
| Experimental | 20 | 8 | 28 |
| Control | 19 | 9 | 28 |
| Total | 39 | 17 | 56 |
Table 1: Showing the number of males and females in the experimental and control group.
| Group | Borges dyspnea rating day 3 | Total | ||||
|---|---|---|---|---|---|---|
| Nothing at all | Just noticeable | Very slight | Slight | slight moderate | ||
| Experimental | 4 | 15 | 8 | 1 | 0 | 28 |
| Control | 0 | 2 | 2 | 13 | 11 | 28 |
| Total | 4 | 17 | 10 | 14 | 11 | 56 |
Table 2: Showing a number of patients with different levels according to Borges dyspnea scale in the experimental and control group on day three.
Discussion
As up to our knowledge this is the first report to find out the effectiveness of peak flow meter exercises in patients with decreased air entry in lungs post atelectasis in Pakistan. This study was purely for improvement of knowledge; Advancement in physical therapy for Intensive care patients, as well as the researcher, was interested to introduce the evidence-based practice in the felid. But there are multiple studies done to improve lung expansion, it is noted that incentive spirometer and other devices are widely used to improve lung expansion. Different lung expansion exercises are also used to improve lung expansion in atelectasis patients, these researches are done internationally and different techniques were used to overcome and to optimize lung function.
Conclusion
According to this study's peak, flow meter exercises show early improvement in lung expansion. The results of the experimental group show highly significant values for Borges dyspnea scale, pulmonary function test and significant in the partial pressure of oxygen as compare to the control group. Furthermore, these results also suggest the effectiveness and role of peak flow meter exercises to improve lung expansion in post atelectasis patients. And it is also noted that the use of this technique also helps to overcome the respiratory crisis and make the treatment cost-effective. It is noted that this technique is very effective to improve lung expansion thereby to overcome respiratory crisis and cost of treatment but the larger sample size is required to authenticate the technique.
References
- Huddy S, Joyce W, Pepper J (1991) Gastrointestinal complications in 4473 patients who underwent cardiopulmonary bypass surgery. Br J Sur 78: 293-296.
- Cheng D, Karski J, Peniston C, Raveendran G, Asokumar B, et al. (1996) Early tracheal extubation after coronary artery bypass graft surgery reduces costs and improves resource use. A prospective, randomized, controlled trial. Anesthesiology 85: 1300-1110.
- Hanson CA, Ritter AB, Duran W, Lavietes MH (1990) Ascites: Its effect upon static inflation of the respiratory system1-3. Am Rev Respir Dis 142: 39-42.
- Pelosi P, Quintel M, Malbrain M (2007) Effect of intra-abdominal pressure on respiratory mechanics. Acta Clin Belg 62: 78-88.
- Wallin G, Cassuto J, Högström S, Rimbäck G, Faxen A, et al. (1986) Failure of epidural anesthesia to prevent postoperative atelectasis. Anesthesiology 65: 292-297.
- Kroenke K, Lawrence V, Theroux J, Tuley M, Hilsenbeck S (1993) Postoperative complications after thoracic and major abdominal surgery in patients with and without obstructive lung disease. Chest 104: 1445-1451.
- Mackay J, Mensah GA (2004) The atlas of heart disease and stroke. The atlas of heart disease and stroke.
- Murray CJ, Lopez AD (1997) Alternative projections of mortality and disability by cause 1990-2020: Global Burden of Disease Study. The Lancet 349: 1498-1504.
- Must A, Spadano J, Coakley EH, Field AE, Colditz G, et al. (1999) The disease burden associated with overweight and obesity. JAMA 282: 1523-1529.
- Pelosi P, Cereda M, Foti G, Giacomini M, Pesenti A (1995) Alterations of lung and chest wall mechanics in patients with acute lung injury: effects of positive end-expiratory pressure. Am J Resp Crit Care Med 152: 531-537.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi