Research Article, J Sleep Disor Treat Care Vol: 7 Issue: 2
Modified Transcendental Meditation Intervention for Nurses via an Application User Group Accessed on Smartphones: Effects of Anxiety and Depression on Sleep Quality
Ru-Wen Liao1*, Chin-Min Huang2, Pei-Shan Hung2, Jing-Wan Luan3 and Yi-Chyan Chen4
1MSN, RN, Vice Director, Department of Nursing, Taipei Tzu Chi Hospital, Buddhist Tzu Chi Medical Foundation, Graduated school of National Taipei University of Nursing and Health Sciences, Taiwan
2MSN, RN, Head Nurse, Department of Nursing, Taipei Tzu Chi Hospital, Buddhist Tzu Chi Medical Foundation, Taiwan
3RN, Master Student, Department of Nursing, Taipei Medical University Shuang Ho Hospital, National Taipei University of Nursing and Health Sciences, Taiwan
4MD, PhD, Director, Department of Psychiatry, Taipei Tzu Chi Hospital, Buddhist Tzu Chi Medical Foundation, School of Medicine, Buddhist Tzu Chi University, Hualien, Taiwan
*Corresponding Author : Ru-Wen Liao
MSN, RN, Vice Director, Department of Nursing, Taipei Tzu Chi Hospital, Buddhist Tzu Chi Medical Foundation
Graduated school of National Taipei University of Nursing and Health Sciences, No. 289, Jianguo Rd., Xindian Dist., New Taipei City 23142, Taiwan
Tel: 886-2-6628-9779; Ext. 8600
E-mail: ruwen@tzuchi.com.tw
Received: September 28, 2017 Accepted: May 24, 2018 Published: June 01, 2018
Citation: Liao RW, Huang CW, Hung PS, Luan JW, Chen YC (2018) Modified Transcendental Meditation Intervention for Nurses via an Application User Group Accessed on Smartphones: Effects of Anxiety and Depression on Sleep Quality. J Sleep Disor: Treat Care 7:2. doi: 10.4172/2325-9639.1000210
Abstract
Background: Sleep quality plays an important role in the overall health of nurses, which may influence the quality of patient care provided by nurses. The LINE messaging app is a commonly used tool for sending messages easily and quickly. Therefore, in this study, to improve sleep quality among nurses, we designed and implemented an intervention with modified transcendent meditation (MTM), which is religious form of meditation, through a LINE user group.
Objective: This study evaluated whether the MTM intervention delivered through a LINE user group effectively improved sleep quality and lessened anxiety and depression in nurses.
Methods: A sample of 84 nurses with poor sleep quality (Chinese version of Pittsburgh Sleep Quality Index (CPSQI) > 5) and psychological problems (Chinese version of Hospital Anxiety and Depression Scale (CHADS) ≥ 8) were randomly assigned to the MTM intervention group (IG) and control group (CG; no MTM intervention). Self-report data were collected at baseline and at intervals of 2 weeks continually to 12 weeks and then naturalistic extension 12-week follow-up using smartphones. Generalized estimating equations and regression analysis was used to evaluate the effects of anxiety and depression in the Chinese version of Pittsburgh Sleep Quality (CPSQI) score.
Results: The anxiety and depression scores of the IG were significantly different at 6 weeks. However, the CPSQI scores of the IG had not changed significantly until 8 weeks of MTM
intervention had been completed. Changes in scores of CPSQI were nonsignificant in the CG. The effects of MTM for improving sleep quality, anxiety and depression were maintained for 12 weeks under naturalistic extension. MTM improves sleep quality which may modulate through the reduction of depression.
Conclusions: MTM exerts positive effects on anxiety, depression, and sleep quality among nurses. Nurses can use this safe, cheap and easy-to-learn method to improve their sleep quality and psychological detachment.
Keywords: Modified transcendental meditation; LINE-used group; Smartphone; Intervention
Introduction
Mason et al. [1] reported that meditation enables slow wave sleep and background delta activity and subsequently reduces electromyogram activity, which is beneficial for sleep. Travis et al. [2] reported that meditation practice increases frontal midline theta activity. Such effects can enhance network synchronization and the neural functions of the brain during sleep. These results show that meditation exerts positive modulatory effects on sleep through autonomic neurons. Pattanashetty et al. [3] reported that poor sleep quality is associated with depression and may be a risk factor for the development of depression or depression relapse. Meditation can promote a beneficial phase of neurological activity that may reset metabolic action, even under fluctuating stress levels [4]. Moreover, meditation may produce physiological and psychological global regulatory changes, which may produce favorable sleep [5].
Koenig et al. [6] observed that religious belief involvement may mitigate the effects of stress, thus decreasing the likelihood of negative health outcomes. Williams et al. [7] found that religious belief involvement buffers the effects of stress on anxiety and depression. The aforementioned results indicate that meditation can influence sleep and its functions. Meditation can regulate the activity of different brain regions through its global effects, thus establishing a state of harmony during sleep. Transcendental meditation (TM), a religious form of meditation, has been discovered to decrease worry rumination and creates a state of deep rest in the body and mind [8].
As a part of their job, nurses manage complex aspects of daily medical care, need to constantly update their professional knowledge, exercise job autonomy to a certain extent, and obtain organization support to ensure and improve the health care of patients. Performing the aforementioned multiple tasks may lead to stress in nurses unavoidably, conflict between nurses and physicians or the central hospital authority may occasionally occur. In such situations, nurses are accountable for their actions, placing extra burden on themselves [9]. For these reasons, nursing is considered the fourth most stressful profession by health education authorities [10]. Nurses with poor sleep quality are more likely than well-rested nurses to make inappropriate decisions and errors in clinical judgment and medication administration and fail to intercept errors made by others [11]. Because many nurses are women, nurses are disproportionately affected by family commitments (e.g., household chores and childcare) and work strain, which often cause difficulties in falling asleep, frequent awakening, and premature awakening [11]. Nurses who cope with daily stressors can improve their mental health, particularly if they can efficiently manage or eliminate poor sleep quality. Hence, identifying suitable coping strategies for improving their sleep quality and promoting their mental health is crucial.
In this study, we incorporated an element of religious belief into meditation—called modified TM (MTM). The feature of MTM is voicelessly speaking the Holy Name of God in the mind. Although previous studies have reported that meditation has positive effects on anxiety, depression and sleep quality [12,13], Moritz et al. [14] found some evidence of no effect and insufficient evidence of any effect of mindful meditation on emotional symptoms. Goyal et al. [15] found no evidence that meditation programs are more favorable than any active treatment (e.g., drugs or behavioral therapies). Based on the aforementioned results, whether MTM exerts effects on nurses working in shifts is our concern. Therefore, this study aimed to confirm the positive effects of MTM on sleep quality and psychological detachment. We established a user group on the smartphone application LINE and encouraged the participants in the LINE group to achieve intervention targets. Previous studies have assessed the effect of meditation interventions at only two points of time (the start and end) [15]. By contrast, we performed assessments of the MTM intervention among nurses at multiple time points to identify the mechanism underlying the association of sleep quality with anxiety and depression.
Design
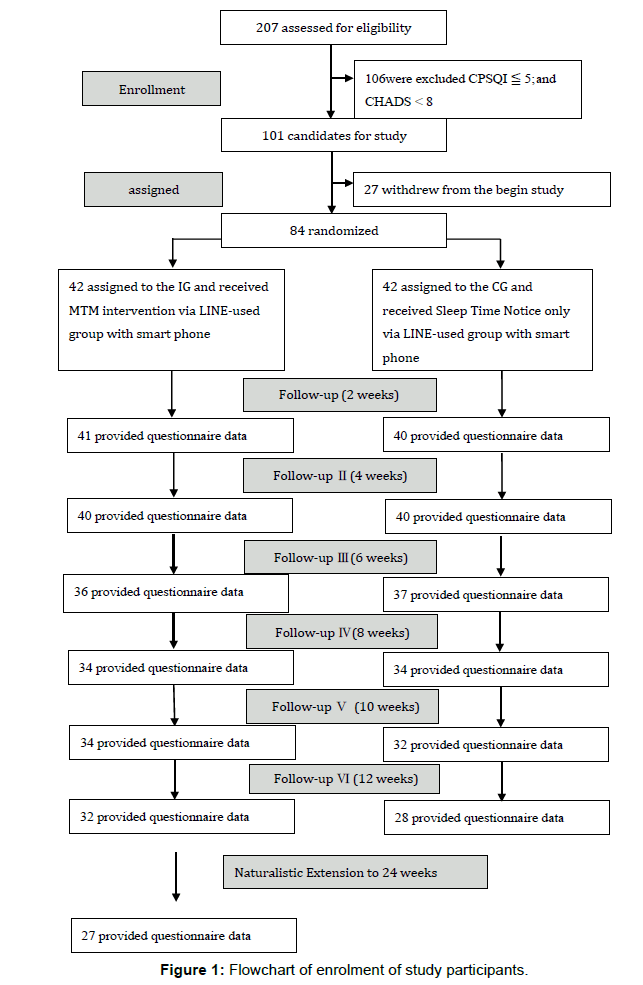
A two-arm randomized controlled trial was conducted in which the MTM intervention group (IG; participants received messages through a LINE user group on their smartphone) was compared with the control group (CG; no MTM intervention). All participants downloaded the iOS or Android LINE app onto their smartphone and joined the study’s private LINE group. The participant members of the private LINE privileged group were anonymous and represented using Arabic numbers only. The intervention was evaluated in a sample of nurses because (a) nurses are often considered to be highly affected by work-related stress [16] and (b) nurses usually have weak boundaries between work life and private life and thus face death and life situations with insufficient psychological support from work. Assessments were conducted at baseline and during and after the MTM intervention (at an interval of approximately 2 weeks, continued to 12 weeks). A naturally extended 12-week follow-up was conducted for the IG only. The flow chart of study is showed in Figure 1.
This study was approved by the Institutional Review Board of the Taipei Tzu Chi Hospital, Buddhist Tzu Chi Medical Foundation.
Meditation
Many types of meditation exist, including TM and mindful meditation (MM). TM emphasizes the mantra to transcend the self to an effortless state without attention being focused; MM emphasizes training to focus on awareness and mindfulness [17]. As for TM and MM, most techniques of meditation require a quiet environment, comfortable posture, focus on a target, and open mind or attitude. Individuals practicing TM constantly utter the mantra in a low voice to synchronize their heart beats and number of breaths. Therefore, in TM, the constant uttering of the mantra may cause individuals feel thirsty and uncomfortable. MM emphasizes thinking about inner and deep thoughts and putting aside external affairs. MTM is a meditation technique intermediate between MM and TM. In this study, we suggested that participants practice MTM not only by concentrating on the Holy Name of God or words in their mind but also by not uttering any words. The object of concentration, namely the Holy Name of God or other words, is more important than the skill of concentration itself and varies with individuals and situations. According to their religious belief, participants practiced MTM by uttering the Holy Names of Buddha for Buddhists, Jesus for Christians, or Zikr for Muslims. Therefore, MTM is a religious form of meditation. If participants did not hold any type of religious belief, we suggested that they should adopt the Holy Name of Buddha, Jesus, or Zikr when practicing meditation. By practicing MTM by focusing on the Holy Name of God or other words, the participants could feel closer to God and obtain more blessings from God. After practicing MTM, an individual may obtain the belief that “Wherever I am and whatever I do, I am accompanied always by God, even when I fall asleep, I am not lonely.” This meditation practice results in tranquility, and the ultimate goal is to promote psychological detachment among nurses, facilitating their sleep.
Participants and intervention connectors
To recruit participants, the nursing department of the hospital sent e-mails to the nurses it employed. Nurses who applied for participation received an online message containing detailed information about the study procedures. They downloaded the LINE messaging app on their mobile phone and were subsequently asked to join the LINE group. The inclusion criteria of participants were (a) all sex, (b) worked full-time for at least 6 months, (c) age more than 20 years, (d) poor sleep quality as measured by a score of >5 on the Chinese version of Pittsburgh Sleep Quality Index (CPSQI) [18], and (e) low levels of psychological detachment from work (i.e., workrelated rumination) as measured by a score of ≥8 on the Chinese version of the Hospital Anxiety and Depression Scale (CHADS) [19]. The exclusion criteria of participants were pregnancy, lactation, working in the administration department and sleep medication use. We chose a score of >5 on the CPSQI because this score indicates poor sleep quality. We chose a score of ≥8 on the CHADS because this score indicates an above-average level of anxiety/depression. A total of 68 nurses meeting all of the inclusion criteria and none of the exclusion criteria were randomly allocated to the study groups by computer. In addition, we chose three individuals to serve as intervention connectors (ICs) who sent messages to participants during the day (8 a.m.–16 p.m.; DIC), evening (16 p.m.–24 p.m.; EIC), and night (0 a.m.–8 a.m.; NIC). These three ICs had worked in psychiatric wards for at least 4 years. They were responsible for sending messages of MTM through LINE according to the different working schedules of the participants; that is, the DIC messaged night shift nurses, EIC messaged day shift nurses, and the NIC messaged evening shift nurses.
Intervention
The three ICs would send messages to the participants of the private LINE group using their smartphone. Through these messages, participants were educated about the appropriate method of starting and stopping meditation practice when they experienced problems such as a concerning image running through their mind continually or health problems. We suggested that all participants in the IG should perform the sitting type of MTM. Before participating in this study, the participants in the IG were educated about the sitting type of MTM through messages sent by the IC through the LINE user group. These participants performed the sitting type of MTM for 30 min over 12 consecutive weeks [20] before going to sleep. To avoid the Hawthorne effect [21], a naturalistic extension to 24-week followup was performed for the IG only.
The MTM intervention consisted of seven steps. First, the participants in the IG practiced MTM for 1 week; their MTM practice was then confirmed by an IC before beginning the study process. Second, all participants were divided into three groups according to their working schedule, with one IC responsible for conveying messages “it’s high time to sleep and execute MTM” to one such group. Third, the DIC would send messages to the night shift nurses in the IG; the NIC would send messages to the evening shift nurses in the IG. These messages reminded the night and evening shift nurses, who left the hospital ward after 3 hours; and evening IC would remind the day shift nurses in the IG at 10 p.m., respectively, to practice MTM and then prepare to sleep. During the same period, the three ICs also sent the message “it’s high time to sleep” only to the participants in the CG. Fourth, when they received the message from their IC, the participants were required to send confirmation messages through the LINE user group. In addition to the IC, the confirmation message sent by a participant could be seen by the other members of the same LINE user group. Fifth, the IC would send the messages of the MTM intervention or the sleep-related message three times (at intervals of 20 min) if the participants did not send a confirmation message on that day. The IC would not send the sleep-related message to participants again if they did not answer and confirm receipt of the messages more than three times during 1 week. If this occurred, the participant’s record would not be entered into analysis and the IC would not send any more messages. Sixt, if participants changed their working schedule, they were required to send their original IC a message about whether they would continue their participation in the project. If their answer was positive, they would be changed to a new LINE group. Finally, these three ICs were not permitted to actively communicate with participants unless participants individually sent a poor health message through the LINE group. In this situation, the IC should suggest that participants consult a physician immediately.
Hypotheses of poor sleep quality affected by anxiety or depression
To determine the effects of the MTM intervention on participants, anxiety and depression were included in analysis as covariates. By investigating changes in sleep quality, we could determine the possible mechanism through which the MTM intervention reduced anxiety or depression. Therefore, we presented the following five hypotheses: Hypothesis 1 (H1): The MTM intervention directly affects CPSQI in nurses (MTM→CPSQI). Hypothesis 2 (H2): The MTM intervention directly affects anxiety in nurses (MTM→Anxiety). Hypothesis 3 (H3): The MTM intervention directly affects depression in nurses (MTM→Depression). Hypothesis 4 (H4): The effect of the MTM intervention on CPSQI in nurses is moderated by change in anxiety (MTM→Anxiety→CPSQI). Hypothesis 5 (H5): The effect of the MTM intervention on CPSQI in nurses is moderated by change in depression (MTM→Depression→CPSQI).
To compare the effect of the intervention on anxiety and depression in the aforementioned five hypotheses, we used multiple repeated measures generalized estimating equations (GEEs) to evaluate the change in CPSQI and CHADS scores between the IG and CG. Regression analysis was used to predict the effects of anxiety and depression on change in the CPSQI score in the IG.
Measurements
Demographic characteristics collected were age, work performance, education level, religious belief, and marital status. Sleep quality was measured using the CPSQI [18]. The 19-item CPSQI is a self-evaluation questionnaire that is used to examine a subject’s sleep patterns during the preceding week. The CPSQI has seven components: sleep latency, sleep duration, subjective sleep quality, sleep efficiency, sleep disturbance, use of sleep medication, and daytime dysfunction. Scores for each item range from 0 to 3, and the overall score ranges from 0 to 21. CPSQI scores greater than 5 indicate the presence of a sleep disorder. The Cronbach’s α of the CPSQI was found to be .87.
When religion-related elements were incorporated into MTM, psychological assessments were conducted using the CHADS [19]. The CHADS is a 14-item self-report instrument that contains seven items related to anxiety and seven items related to depression. The CHADS uses a 4-point Likert scale, with 0 for never, 1 for low frequency, 2 for usually, and 3 for always. CHADS scores indicate the prevalence of anxiety and depression: 0–7, normal; 8–10, mild; 11–14, moderate; and 15–21, severe. Higher scores indicate higher degrees of anxiety and depression. The Cronbach’s α of the CHADS was .81 for anxiety and .82 for depression in the present study.
Statistical analysis
Descriptive statistics for age, gender, marital status, education level, working performance, and religious belief were computed. Multiple repeated measures GEEs were used to evaluate the change in CPSQI and CHADS scores between baseline and different intervals, and scores recorded over the extended 12-week follow-up were evaluated from pre to post intervention between the IG and CG. Regression analysis was used to predict the effects of anxiety and depression on the change in CPSQI score. All analyses were conducted using SPSS for Windows, version 20.0 (SPSS Inc., Chicago, IL, USA).
Results
Demographic characteristics and baseline CPSQI and CHADS scores of participants
Figure 1 shows the flowchart for the enrolment of study participants. A total of 84 participants were divided into the IG (N=42) and CG (N=42) at baseline. Only 32 IG and 28 CG participants completed the study after MTM intervention of the study to 12 weeks (Figure 1). Regarding demographic characteristics, no significant differences were observed in age, working performance, educational level, marital status, sex, and religious belief between the IG and CG (Table 1). Furthermore, no significant differences were identified in the baseline scores on the CPSQI and baseline anxiety and depression scores on the CHADS between the IG and CG (Table 1).
| Variables | IG (n=42) n (%) |
CG (n=42) n (%) |
F / Chi-square |
|---|---|---|---|
| Sex | .11 | ||
| Male | 3(7.1) | 3(7.1) | |
| Female | 39(92.9) | 39(92.9) | |
| Age(years) | 27.97 ± 4.28 | 28.14 ± 4.22 | .01 |
| Working performance (years) | 5.28 ± 3.34 | 5.47 ± 3.45 | .04 |
| Education level | .25 | ||
| Junior collage | 14(33.3) | 13(31.0) | |
| University | 28(66.7) | 29(69.0) | |
| Martial status | .58 | ||
| Unmarried | 30(71.4) | 28(66.7) | |
| Married | 12(28.6) | 14(33.3) | |
| Religious belief | .25 | ||
| Have | 16(38.1) | 15(35.7) | |
| None | 26(61.9) | 27(64.3) | |
| Baseline PSQI | 7.93 ± 2.38 | 8.07 ± 2.27 | .01 |
| Baseline Anxiety | 10.20 ± 2.19 | 10.33 ± 2.02 | .08 |
| Baseline Depression | 13.63 ± 2.20 | 13.57 ± 2.29 | .10 |
Table 1: Demographic characteristics (means/counts, standard deviations/percentages) and baseline CPSQI and CHADS scores between IG and CG.
Change in CPSQI score after MTM intervention
Compared with the baseline score, the IG presented the first, but nonsignificant change in CPSQI score after 6 weeks of MTM intervention (B=0.43, Wald χ2=3.05, confidence interval [CI]: -0.92 to 0.05). The CPSQI scores of the IG were significantly lower after 8 weeks of MTM intervention (B=-1.50, Wald χ2=34.03, CI: -2.00 to -1.00) compared with baseline (Table 2). Thus, the MTM intervention directly changed the CPSQI score until 12 weeks and the naturalistic extended 12-week period. The CPSQI scores changed insignificantly in the CG during the 12-week study period.
| Variables | CPSQI | Anxiety | Depression | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Variables | B | Wald χ2 | 95% CI | B | Wald χ2 | 95% CI | B | Wald χ2 | 95% CI |
| (Constant) | 8.59** | 190.30 | (7.37, 9.81) | 9.63** | 420.83 | (8.72, 10.55) | 12.99** | 662.99 | (12.00, 13.98) |
| Baseline | |||||||||
| 2 weeks | 0.07 | 0.33 | (-0.16, 0.30) | 0.13 | 0.61 | (-0.20, 0.47) | -0.33 | 1.59 | (-0.85, 0.19) |
| 4 weeks | -0.23 | 1.76 | (-0.58, 0.11) | -0.10 | 0.20 | (-0.53, 0.33) | -0.37 | 1.62 | (-0.85, 0.18) |
| 6 weeks | -0.43 | 3.05 | (-0.92, 0.05) | -1.13** | 28.80 | (-1.55, -0.72) | -1.57** | 23.90 | (-2.20, -0.94) |
| 8 weeks | -1.50** | 34.03 | (-2.00, -1.00) | -2.03** | 93.89 | (-2.51, -1.56) | -2.27** | 66.37 | (-2.81, -1.72) |
| 10 weeks | -1.37** | 28.74 | (-1.91, -0.82) | -1.97** | 89.33 | (-2.37, -1.56) | -2.03** | 40.37 | (-2.66, -1.41) |
| 12 weeks | -1.33** | 23.96 | (-1.82, -0.85) | -1.93** | 83.76 | (-2.34, -1.52) | -1.80** | 29.72 | (-2.45, -1.15) |
| Extend to 24 weeks | -1.27** | 23.04 | (-1.78, -0.75) | -1.80** | 75.16 | (-2.21, -1.39) | -1.53** | 24.29 | (-2.14, -0.92) |
Table 2: Repeated measures GEE analysis of changes in CPSQI score and anxiety and depression scores on CHADS at different time points during MTM intervention in IG.
Change in anxiety and depression scores after MTM intervention
Compared with the baseline score, the IG presented significant changes in anxiety scores after 6 weeks of MTM intervention (Table 2) (B=-1.13, Wald χ2=28.80, CI: -1.55 to -0.72). The anxiety scores of the IG were statistically significantly lower after 8 weeks of MTM intervention (B=-2.03, Wald χ2=93.89, CI: -2.51 to -1.56) compared with baseline. These scores were maintained until 12 weeks. Similarly, compared with the baseline score, the IG presented significant changes in depression scores after 6 weeks of MTM intervention (B=- 1.57, Wald χ2=23.90, CI: -2.20 to -0.94). The depression scores of the IG were significantly lower after 8 weeks of MTM intervention (B=- 2.27, Wald χ2=66.37, CI: -2.81 to -1.72) compared with baseline. These scores were maintained until 12 weeks (Table 2). Thus, the MTM intervention directly reduced anxiety and depression. The anxiety and depression scores on the CHADS changed non-significantly in the CG during the 12-week study period.
Effects of MTM intervention maintained during extended 12-week follow-up
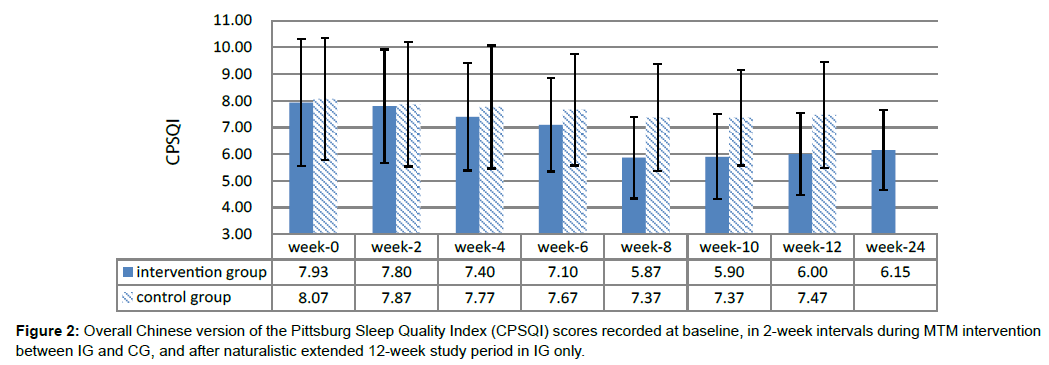
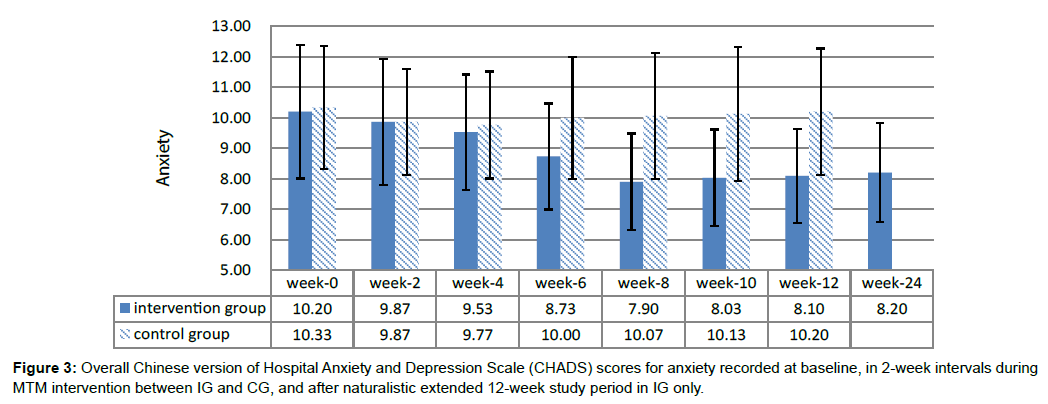
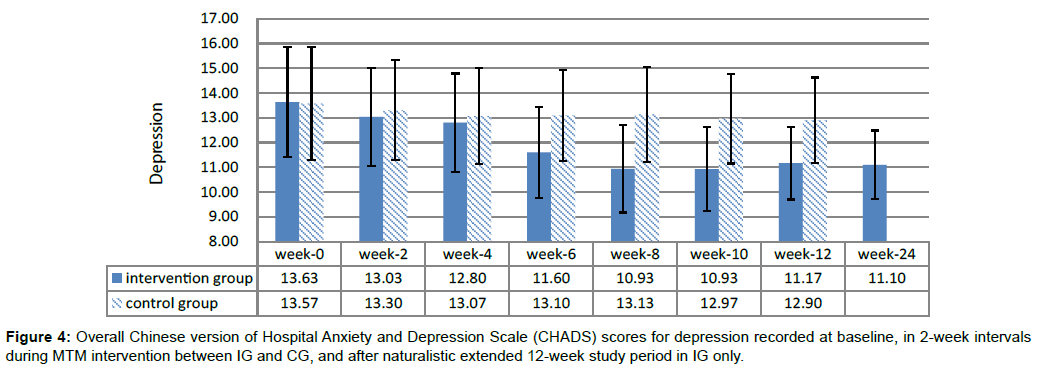
After the study period’s naturalistic extension to 12 weeks, the IG presented significant changes in CPSQI score (B=-1.27, Wald χ2=23.04, CI: -1.78 to -0.75), anxiety score (B=-1.80, Wald χ2=75.16, CI: -2.21 to -1.39), and depression score (B=-1.53, Wald χ2=24.29, CI: -2.14 to -0.92) (Table 2) compared with the baseline. The intervention exerted positive effects in reducing CPSQI (Figure 2), anxiety (Figure 3), and depression (Figure 4) score in the IG during the naturalistic extended 12-week study period. This finding indicated that the effects of the MTM intervention were stable in the IG.
Responders versus non-responders
We divided the participants of the IG into responders and nonresponders after the MTM intervention was complete. Participants were considered responders when their CPSQI scores were less than 5 and their anxiety and depression scores were less than 8 after naturalistic extension of the study to 12 weeks. By the end of the naturalistic extension to 12-week study period, 9 of the 27 participants in the IG (33.0%) were responders (data not shown), whereas the remaining 18 participants of the IG were non-responders. The responders were confirmed with CPSQI and CHADS by a psychiatric physician through reassessment of their LINE messages.
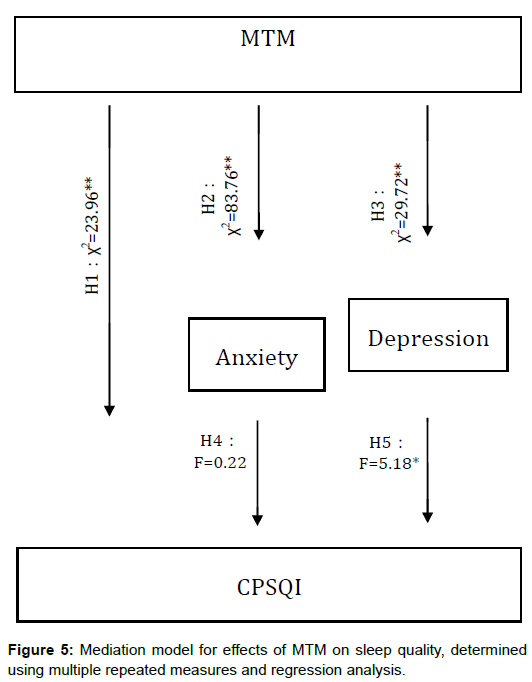
Mechanisms of CPSQI change during MTM intervention
Figure 5 displays the mediation model for the MTM intervention. At 6 weeks, the direct effect was significant, supporting H2 (B=- 1.13) and H3 (B=-1.57) (Table 2). Furthermore, the mediation effect was nonsignificant regarding CPSQI in line with H1 (B=-0.43), H4 (F=0.14, B=-0.07, SE=0.19, ß=-0.07, T=-0.38) and H5 (F=3.91, B=-0.33, SE=0.16, ß=-0.35, T=-1.98) (Table 3). As indicated by the hypothetical model at 6 weeks, no mediation effects were found for anxiety and depression (Table 3). At 8 weeks, the direct effects were significant, supporting H1 (B=-1.50), H2 (B=-2.03), and H3 (B=- 2.27). The mediation effect was significant, supporting H5 (F=7.01, B=-0.40, SE=0.15, ß=-0.45, T=-2.65) but disproving H4 (F=0.66, B=-0.15, SE=0.19, ß=-0.15, T=-0.81) (Table 3). As indicated by the hypothetical model in Figure 5, in the IG, the MTM intervention began to directly reduce anxiety and depression significantly at 6 weeks and then reduced the CPSQI score significantly until 12 weeks. The MTM intervention thus changed anxiety and depression scores before changing the CPSQI score (Figures 2-4). At 24 weeks, the MTM intervention significantly mediated poor sleep quality by reducing depression in the IG, supporting H5 (Tables 2 and 3).
| Variable | F | B | SE | β | t |
|---|---|---|---|---|---|
| 6 weeks | |||||
| Anxiety | 0.14 | -0.07 | 0.19 | -0.07 | -0.38 |
| Depression | 3.91 | -0.33 | 0.16 | -0.35 | -1.98 |
| 8 weeks | |||||
| Anxiety | 0.66 | -0.15 | 0.19 | -0.15 | -0.81 |
| Depression | 7.01* | -0.40 | 0.15 | -0.45 | -2.65* |
| 10 weeks | |||||
| Anxiety | 0.38 | -0.08 | 0.19 | -0.08 | -0.43 |
| Depression | 4.83* | -0.38 | 0.17 | -0.38 | -2.20* |
| 12 weeks | |||||
| Anxiety | 0.22 | -0.03 | 0.19 | -0.03 | -0.15 |
| Depression | 5.18* | -0.41 | 0.18 | -0.40 | -2.28* |
| 24 weeks | |||||
| Anxiety | 0.02 | -0.02 | 0.17 | -0.02 | -0.12 |
| Depression | 4.51* | -0.39 | 0.18 | -0.37 | -2.12* |
Table 3: Regression analysis of anxiety and depression score versus CPSQI score during MTM intervention in IG.
Discussion
This randomized controlled study investigated whether an intervention through a LINE user group improved sleep quality and psychological detachment among nurses. Previous studies have shown that mindful or mantra meditation exerts a moderate effect for reducing psychological symptoms (e.g., stress, depression, and anxiety) [22] and for improving physical symptoms (e.g., sleep disorders) [13]. Wolever et al. [23] found moderate evidence that 8 weeks of mindfulness meditation improved anxiety and depression and some evidence that mindfulness meditation improved stress and mental-health-related quality of life (e.g., sleep). By contrast, Moritz et al. [14] reported evidence of no or only slight effect of MM on emotional symptoms. Goyal et al. [15] found no evidence that meditation programs are more favorable than any active treatment (e.g., drugs, exercise, and other behavioral therapies). We discovered that the MTM intervention effectively improved anxiety, depression (psychological detachment), and sleep quality. During the period of naturalistic extension study to 24-week, the CPSQI scores of 33% (9/27) of participants in the IG decreased to less than 5. This result showed that the effect of the MTM intervention remained stable and that the intervention improved upon poor sleep quality.
Previous studies have discovered that the effect of different self-help MM interventions tended to be less than that of expect in meditation programs for improving sleep, anxiety and depression [15]. The effects of the intervention implemented through the LINE user group in this study may indicate that intervention at a fixed time daily is necessary to achieve significant meaningful results for nurses. Many studies have been conducted in which interventions for poor sleep quality were applied without intensive guidance; these studies discovered weak or nonsignificant effects [24,25]. This result may be because people are perhaps less willing to participate in an intervention if extra support is not provided. In addition, the MTM intervention in the present study produced strong effects for participants in the same LINE user group, as membership of this group may have resulted in higher motivation to achieve intervention targets than expected. Its potential effect may be greater in nurses, because the intervention through LINE user groups is a wider reach and more participants can use it because of its low cost [26]. Thus, future studies should evaluate the effectiveness and convenience of intervention through LINE user groups.
Reduced sleep effort has been suggested to be one of the core mechanisms of psychological interventions for sleep [27,28]. Cuijpers et al. [29] reported that meditation intervention exerted significant effects on psychological detachment and sleep. In the present study, we also found that the intervention increased sleep quality by reducing depression. This finding shows that MTM intervention may improve poor mental health resulting from job-related rumination and poor sleep quality in people with comorbid psychological detachment and sleep problems. The present study results indicated that MTM intervention improved anxiety and depression before improving poor sleep quality. Thus, MTM may be a valuable intervention for improving sleep. The present study showed that the MTM intervention positively and directly improved anxiety, depression, and sleep quality and that depression played a mediation role. This trial is the first to provide empirical evidence for this hypothesis. Additional studies should investigate whether the effect of the MTM intervention on sleep is mediated through reduction of depression or through other mechanisms and it needs more studies in the future.
Conclusion
Our data suggest that the MTM intervention, implemented through a LINE user group, exerts a positive effect on sleep quality, anxiety, and depression, which can be a substantial benefit for nurses. Nurses should use MTM, which is simple and easy to learn, as a coping strategy because it is a safe and cheap method that can be used to improve sleep quality and increase psychological detachment. In addition, this study demonstrated that LINE user groups may be highly useful tools for delivering self-help intervention in health care.
Study Limitations
First, this study enrolled nurses, who are well-trained professional staff. The study results may only be valid for professionals working in shifts who exhibit similar attributes and work-related stress, such as firemen, policemen, and medical staff who experience high professional stress and a blurring of the line between work and offduty life.
Second, the sample size was insufficient; thus, more underlying mechanisms could not be investigated in this study. Although serial multiple analyses confirmed the core hypothesis that MTM intervention affects anxiety, depression, and poor sleep quality, the other mechanisms of the intervention remain unclear. It was hypothesized that MTM reduces anxiety and depression and increases sleep quality both directly and indirectly. To present a clear conclusion on the mechanisms underlying the effects of the MTM intervention on anxiety, depression, and poor sleep quality, more longitudinal and long terms research are required.
What this study adds
• The MTM intervention directly exerted positive effects on poor sleep quality, anxiety, and depression.
• The MTM intervention changed anxiety and depression scores before changing CPSQI scores.
• MTM improved poor sleep quality by reducing depression.
• MTM is a cheap, safe, and easy-to-learn method that can be used by nurses to cope with poor sleep quality, anxiety, and depression.
• This study demonstrated that a LINE user group may be a highly useful tool for delivering self-help intervention in health care.
References
- Mason LI, Alexander CN, Travis FT, Marsh G, Orme-Johnson DW, et al. (1997) Electrophysiological correlates of higher states of consciousness during sleep in long-term practitioners of the transcendental meditation program. Sleep 20: 102-110.
- Travis F, Shear J (2010) Focused attention, open monitoring and automatic self-transcending: categories to organize meditations from Vedic, Buddhist and Chinese traditions. Conscious Cogn 19: 1110-1118.
- Pattanashetty R, Sathiamma S, Talakkad S, Nityananda P, Trichur R, et al. (2010) Practitioners of vipassana meditation exhibit enhanced slow wave sleep and REM sleep states across different age groups. Sleep Biol Rhyth 8: 34-41.
- Sibinga EM, Kerrigan D, Stewart M, Johnson K, Magyari T, et al. (2011) Mindfulness-based stress reduction for Urban youth.J Altern Complement Med 17: 213–218.
- Ong JC, Manber R, Segal Z, Xia Y, Shapiro S, et al. (2014) A randomized controlled trial of mindfulness meditation for chronic insomnia. Sleep 37: 1553-1563.
- Koenig HG (2009) Research on religion, spirituality, and mental health: A review. Can J Psychiatry 54: 285-291.
- Williams DR, Larson DB, Buckler RE, Heckmann RC, Pyle CM (1991) Religion and psychological distress in a community sample. Soc Sci Med 32: 1257-1262.
- Schneider RH, Alexander C, Staggers F, Orme-Johnson DW, Rainforth M, et al. (2005) A randomized controlled trial of stress reduction in African Americans treated for hypertension for over one year. Am J Hypertens 18: 88-98.
- Gasparino R C, Guirardello EB (2015) Professional practice environment and occupational burnout among nurses. Rev Rene 16: 90-96.
- Jodas D A, Haddad MCL (2009) Burnout syndrome among nursing staff from an emergency department of a hniversity hospital. Acta paul enferm 22: 192-197.
- Lin SH, Liao WC, Chen MY, Fan JY (2014) The impact of shift work on nurses job stress, sleep quality and self-perceived health status. J Nurs Manag 22: 604-612.
- Hofmann SG, Sawyer AT, Witt AA, Oh D (2010) The effect of mindfulness-based therapy on anxiety and depression: a meta-analytic review. J Consult Clin Psychol 78: 169-183.
- Winbush NY, Gross CR, Kreitzer MJ (2007) The effects of mindfulness-based stress reduction on sleep disturbance: a systematic review. Explore (NY) 3: 585-591.
- Moritz S, Quan H, Rickhi B, Liu M, Angen M, et al. (2006) A home study-based spirituality education program decreases emotional distress and increases quality of life--a randomized, controlled trial.Altern Ther Health Med 12: 26-35.
- Goyal M, Singh S, Sibinga EM, Gould NF, Rowland-Seymour A, et al. (2014) Meditation programs for psychological stress and well-being: a systematic review and meta-analysis. JAMA Intern Med 174: 357-368.
- Rocha MCP, Martino MMF (2009) Stress and sleep quality among registered nurses who use sleeping pills. Acta Paul Enferm 22: 658-665.
- Rapgay L, Bystrisky A (2009) Classical mindfulness: an introduction to its theory and practice for clinical application. Ann N Y Acad Sci 1172: 148–162.
- Tsai PS, Wang SY, Wang MY, Su C T, Yang TT, et al. (2005) Psychometric evaluation of the Chinese version of the Pittsburgh Sleep Quality Index (CPSQI) in primary insomnia and control subjects. Qual Life Res 14: 1943-1952.
- Liang CC (2004) Stress reaction, emotional effects and posttraumatic stress disorder in sever acute respiratory syndrome patients: a follow-up study. Master’s Thesis.
- Carmody J, Baer RA (2009) How long does a mindfulness-based stress reduction program need to be? A review of class contact hours and effect sizes for psychological distress. J Clin Psychol 65: 627-638.
- McCambridge J, Witton J, Elbourne DR (2014) Systematic review of the Hawthorne effect: new concepts are needed to study research participation effects. J Clin Epidemiol 67: 267-277.
- Chambers R, Gullone E, Allen NB (2009) Mindful emotion regulation: An integrative review. Clin Psychol Rev 29: 560-572.
- Wolever RQ, Bobinet KJ, McCabe K, Mackenzie ER, Fekete E, et al. (2012) Effective and viable mind-body stress reduction in the workplace: a randomized controlled trial. J Occup Health Psychol 17: 246-58.
- Riley WT, Mihm P, Behar A, Morin CM (2010) A computer device to deliver behavioral interventions for insomnia. Behav Sleep Med 8:2-15.
- Suzuki E, Tsuchiya M, Hirokawa K, Taniguchi T, Mitsuhashi T, et al. (2008) Evaluation of an Internet-based self-help program for better quality of sleep among Japanese workers: A randomized controlled trial. J Occup Health 50: 387-399.
- Ebert DD, Lehr D, Smit F, Zarski AC, Riper H, et al. (2014) Efficacy and cost-effectiveness of minimal guided and unguided internet-based mobile supported stress-management in employees with occupational stress: A three-armed randomised controlled trial. BMC Public Health 14: 807.
- Espie CA, Broomfield NM, MacMahon KMA, Macphee LM, Taylor LM (2006) The attention-intention-effort pathway in the development of psychophysiologic insomnia: A theoretical review. Sleep Med Rev 10: 215-245.
- Schwartz DR, Carney CE (2012) Mediators of cognitive–behavioral therapy for insomnia: A review of randomized controlled trials and secondary analysis studies. Clin Psychol Rev 32:664-675.
- Cuijpers P, Huibers M, Ebert DD, Koole S L, Andersson G (2013) How much psychotherapy is needed to treat depression? A metaregression analysis. Journal of Affective Disorders 149:1-13.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi