Research Article, J Sleep Disor Treat Care Vol: 6 Issue: 4
Sleep Apnea and Neck Circumference in Japanese Rugby Union Athletes
Hiroshi Suzuki1*, Arisa Ebato1, Yoshihiro Iwata1, Akihiro Yasuda1, Tatsuo Yagi2, Hiroki Takeuchi1, Osamu Komiyama1 and Chin Moi Chow3
1Department of Oral Function and Rehabilitation, Nihon University School of Dentistry at Matsudo, Japan
2Faculty of Law, Seiwa University, Chiba, Japan
3Discipline of Exercise and Sport Science, Faculty of Health Sciences, The University of Sydney, Australia
*Corresponding Author : Hiroshi Suzuki, DDS, PhD
Department of Oral Function and Rehabilitation, Nihon University School of Dentistry at Matsudo, 870-1 Sakaecho, Nishi-2, Matsudo, Chiba 271-8587, Japan
Tel: +81-47-360-9641
Fax +81-47-360-9615
E-mail:suzuki.hiroshi91@nihon-u.ac.jp
Received: August 29, 2017 Accepted: September 18, 2017 Published: September 25, 2017
Citation: Suzuki H, Iwata Y, Yasuda A, Yagi T, Takeuchi H (2017) Sleep Apnea and Neck Circumference in Japanese Rugby Union Athletes. J Sleep Disor: Treat Care 6:4. doi: 10.4172/2325-9639.1000200
Abstract
Objective: The body size of football players may potentially influence high-level performance. However, increased body mass may increase sleep apnea risks. This study investigated the severity of obstructive sleep apnea (OSA) and body composition among Japanese rugby union players.
Methods: Subjects were 52 Japanese male rugby union players. The team received routine dental support at the Nihon University School of Dentistry in Matsudo, Japan. Dental services included dental checkups and treatment, and provision of custom-made mouthguards. Outcome measures were the respiratory disturbance index (RDI) recorded from a sleep apnea test and body mass index (BMI), neck circumference (NC) measurements, and the Epworth Sleepiness Scale (ESS). All players were informed of the outcome of the sleep apnea test following completion of assessments, after which eight players desired and received treatment with a monoblock mandibular advancement device (MAD).
Results: OSA was seen in 86.5% of players (29 mild, 14 moderate, 2 severe), with only seven players free of OSA. All players were obese according to BMI, with a large NC (mean, 42.5±3.7 cm). Players with moderate and severe OSA exhibited significantly higher BMI and NC than the normal group (p=0.05 and p=0.02, respectively). NC and BMI correlated positively with RDI and snoring episodes, but negatively with minimum and mean peripheral oxygen saturation. The Youden index (NC cut-off, 40.75 cm) indicated increased OSA risk in 32.7%. Daytime ESS score was high (mean, 11±3.9). MAD treatment in eight of the players with OSA significantly improved RDI.
Conclusion: OSA was identified in 86.5% of rugby players, with potential contributions from the large NC and characteristic facial morphology of Japanese individuals. During dental care for athletes, dentists may be able to identify sleep-related disorders.
Keywords: Sports athlete; Rugby union player; Obstructive sleep apnea; Respiratory disturbance index; Body mass index; Neck circumference; Dental treatment; Mandibular advancement device
Introduction
The body size of football athletes has reportedly been increasing over the last century [1]. Given the general effects on the outcomes of physical performance tests, body size is commonly believed to matter [2]. Body size increases career length, and athletes with this physical asset stand to gain greater financial rewards [1]. Anding and Oliver emphasized that while football athletes have continued to gain size, height has remained relatively constant [3]. The increase in body mass often includes both lean and fat mass. In particular, offensive linemen have recorded higher body fat mass than other player positions [4]. Increased fat mass has been linked to metabolic syndrome and cardiovascular risks in football players [5]. Furthermore, large body size, expressed as body mass index (BMI), correlates significantly with neck circumference (NC) (men, r=0.83; women, r=0.71) [6], which in turn represents a significant predictor of obstructive sleep apnea syndrome (OSAS) and central obesity [7]. NC>43 cm was also reportedly related to the severity of obstructive sleep apnea (OSA) in American patients, with 67% sensitivity and 83% specificity [8]. Given that many rugby athletes have thick necks that may be due to training and the nature of the game, it may not be surprising that many players may experience disturbed sleep linked to OSAS.
Competitive sports have become increasingly sophisticated, and the training of athletes to improve competitive strength has gained in both intensity and frequency. Even outstanding athletes who are unable to follow training as planned or fail to reach optimal fitness can experience difficulty in achieving desired results in a competition. Sleep is believed to play important roles in the physical and psychological recovery of athletes [9], and inadequate sleep would be expected to impact negatively on physical and psychological performance. For example, insufficient sleep has been reported to cause muscular weakness [10] and increases in heart rate, ventilation, and lactic acid concentration [11] at specific exercise intensities. In addition, insufficient sleep is reported to lead to increases in perceived exercise intensity [10], slowed reaction time, and lowered attentiveness [12], as well as reductions in movement precision [13].
Sleep as a primary means of recovery is widely accepted and has been recognized as the most important recovery modality by a large number of elite team sport athletes, including rugby union players [14], as well as being an important consideration for cricket players [15]. Sleep may also play an important role in physical adaptation from a training stimulus, with resultant improvements in skill acquisition, physical performance and mood variables [16]. The consequences of inadequate sleep are numerous and well-documented. Those pertinent to athletes include negative mood and cognitive impacts [17], immune system impairment, increased inflammation [18], metabolic dysfunction [19] and decreased pain tolerance [17,20], and conditions such as OSAS.
To date, no research has investigating the sleep concerns of Japan’s top rugby union athletes. Rugby union is a game in which muscular strength is a prerequisite, and neck muscle strength is also a requirement. The present study aimed to investigate the presence and severity of OSA, associations with BMI and NC, and subjective daytime sleepiness in 52 rugby union players.
Methods
Subjects
Subjects were 52 Japanese male rugby union players. The team received routine dental support at the Nihon University School of Dentistry in Matsudo, Japan. Dental services included dental checkups and treatment, and provision of custom-made mouthguards. At the time of a checkup, consent was obtained for participation in the study. Table 1 shows mean values and standard deviations (SDs) for age, height, weight, BMI, and NC, which was measured at the midway of the neck between the mid-cervical spine and mid-anterior neck to 10 mm, and, if palpable, just below the laryngeal prominence [6]. The team was in general good health and no subjects were on any medications. In addition, dental assessments in all participants indicated normal occlusions without subjective or objective abnormalities in the stomatognathic system, and no past or present disorders of the maxillomandibular joint or abnormalities of the motor function of the trunk or limbs.
| Normal (n=7) | Mild (n=29) | Moderate (n=14) | Severe (n=2) | P | Multiple Comparision | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | Mean | SD | Mean | SD | Bonferroni | ||
| Height | 176.71 | 7.68 | 178.1 | 5.03 | 179.47 | 6.15 | 184 | 5.66 | 0.394 | N.S. |
| Weight | 86.13 | 19.87 | 91.3 | 14.52 | 99.96 | 14.08 | 119.65 | 10.39 | 0.02 | normal < Severe |
| BMI | 27.34 | 4.28 | 28.7 | 3.77 | 31.09 | 3.8 | 33.85 | 2.9 | 0.05 | normal < moderate,Severe |
| Neck Circumference | 39.64 | 1.84 | 41.98 | 3.57 | 44.44 | 3.28 | 43 | 0 | 0.02 | normal < moderate,Severe |
Table 1: RDI severity and Sleep apnea characteristics.
Sleep apnea test
Respiratory disturbance index (RDI), minimum and mean peripheral oxygen saturation (SpO2), total number of snoring episodes and number of snoring episodes per hour during sleep were recorded using the SAS-2100 sleep disorder diagnostic system (Teijin Home Healthcare, Tokyo, Japan). This device is simple and easy to use, and is classified as a type 3 monitor [21]. Nasal airflow, heart rate and SpO2 were continuously monitored for about 6 h, then downloaded and analyzed using QP-021W version 01-10 software (Nihon Kohden, Tokyo, Japan). Players were grouped by RDI score as used in other studies [22] for comparison between groups, as follows: 0-4.9, normal; 5-14.9, mild OSA; 15-29.9, moderate OSA; and ≥ 30, severe OSA.
Daytime sleepiness evaluation
Subjective sleepiness was assessed using the Japanese version of the Epworth Sleepiness Scale (ESS), a simple questionnaire measuring the general level of daytime sleepiness or average sleep propensity experienced by the individual [23]. The questionnaire yields a global score ranging from 0 to 24. The ESS measure is comparable to other daytime tests such as the multiple sleep latency test, which is a valid and reliable measure of objective sleepiness. The ESS is a practical evaluative tool that has been applied to athletes [24].
Dental treatment
All players were informed of the outcome of the sleep apnea test following completion of assessments, of which eight players (mean, ± SD) age, 27.8 ± 4.1 years; height, 178.1 ± 5.8 cm; weight, 92.6 ± 15.6 kg; BMI, 29.2 ± 4.1 kg/m2; and NC, 42.5 ± 3.7 cm) desired and received treatment with a monoblock mandibular advancement device (MAD) at the outpatient Snore Clinic, Nihon University School of Dentistry at Matsudo Hospital. One month after treatment, when participants were accustomed to wearing the MAD, the sleep apnea test and ESS were re-administered to evaluate the effects of MAD.
Data analyses
One-way analysis of variance was used to compare OSA severity groups with respect to body composition (body weight, height, BMI, NC) and sleep apnea characteristics (subjective sleepiness, minimum SpO2, mean SpO2, total number of snoring episodes, and number of snoring episodes per hour). Bonferroni post-hoc analysis was applied when a significant difference was identified between group means. Spearman's rank-correlation coefficient was used to assess relationships between body composition data (BMI and NC) and sleep apnea characteristics (RDI, minimum and mean SpO2, and total and mean snoring episodes). The sensitivity and specificity of wellclassified observations and the Youden index (sensitivity+specificity-1) [25] were calculated for different NCs. The receiver operating characteristics (ROC) curve was plotted and the area under the curve (AUC) was calculated according to the trapezoid method. A paired t-test was applied as the test for significance of the effect of dental treatment using the MAD.
For all analyses, we presented 95% confidence intervals and considered values of p<0.05 as significant. All statistical analyses were performed using SPSS for Windows version 20 software (SPSS, Chicago, IL).
Ethical Considerations
All participants provided written informed consent prior to enrolment. All procedures performed in studies involving human participants were in accordance with the ethical standards of institutional and/or national research committees and the 1964 Helsinki Declaration including its subsequent amendments, or comparable ethical standards. This study was approved by the Ethics Committee of Nihon University School of Dentistry at Matsudo (EC 17-12-012-1).
Results
OSA
OSA was diagnosed in 86.5% of players, classified according to the RDI severity as mild in 29 players (55.8%), moderate in 14 (26.9%), and severe in two (3.8%). Seven players (13.5%) had no OSA. No significant differences in age were apparent between groups. On the other hand, significant differences were observed in minimum or mean SpO2, total number of snoring episodes or number of snoring episodes per hour between RDI severity groups (Table 1). Players with moderate and severe OSA displayed significantly lower mean SpO2 than players with normal RDI (p=0.000). All players with mild, moderate or severe RDI showed significantly reduced minimum SpO2, and si gnificantly greater total number of snoring episodes (p=0.003) and number of snoring episodes per hour (p=0.005) (Table 1).
Severity of OSA and body composition
Table 2 shows a comparison of body weight, BMI and NC between RDI groups. Players with severe OSA were significantly heavier than players in the normal group (p=0.02). Players with moderate or severe OSA showed significantly higher BMI and NC than the normal group (p=0.05 and p=0.02, respectively) (Table 2). NC, BMI, body weight and height all correlated positively with the sleep apnea variables of RDI and number of snoring episodes (total and average per hour), but negatively with SpO2 (minimum and mean), with the exception of a lack of correlation between height and mean SpO2 (Table 3).
| Normal (n=7) | Mild (n=7) | Moderate (n=7) | Severe (n=7) | P | Multiple Comparision | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | Mean | SD | Mean | SD | Bonferroni | ||
| Age | 26.29 | 1.5 | 27.86 | 3.98 | 27.71 | 4.73 | 32.5 | 0.71 | 0.281 | N.S. |
| RDI | 2.14 | 1.39 | 9.42 | 2.69 | 21.86 | 4.19 | 33.95 | 0.92 | 0 | Normal<mild<moderate<severe |
| Minimum SpO2 | 93.86 | 2.41 | 90.52 | 3.48 | 88.5 | 2.59 | 87.5 | 0.71 | 0.003 | Normal>mild<moderate, severe |
| Mean SpO2 | 95.71 | 0.95 | 94.69 | 1 | 93.64 | 1.34 | 92.5 | 0.71 | 0 | Normal>moderate, severe |
| Total Snore Events | 13.14 | 12.19 | 341021 | 482 | 861.59 | 781.8 | 1071.3 | 120.21 | 0.003 | Normal, mild<moderate, severe |
| Snore Events per hour | 10.86 | 19.35 | 60.97 | 79.3 | 181.44 | 182.15 | 83.35 | 103.17 | 0.005 | Normal, mild<moderate, severe |
| ESS | 11.14 | 3.8 | 9.72 | 4.34 | 12.71 | 4.94 | 14.5 | 2.12 | 0.138 | N.S. |
Table 2: RDI severity and body composition.
| RDI | Minimum SpO2 | Mean SpO2 | Total Snore Events | Snore Events per hour | ||
|---|---|---|---|---|---|---|
| Height | ρ | 0.225 | -0.293 | -0.25 | 0.452 | 0.417 |
| P | 0.119 | 0.035 | 0.073 | 0.001 | 0.002 | |
| Weight | ρ | 0.413 | -0.361 | -0.405 | 0.561 | 0.516 |
| P | 0.002 | 0.009 | 0.003 | <.001 | <.001 | |
| BMI | ρ | 0.401 | -0.361 | -0.418 | 0.505 | 0.476 |
| P | 0.003 | 0.009 | 0.002 | <.001 | <.001 | |
| Neck Circumference | ρ | 0.466 | -0.491 | -0.453 | 0.582 | 0.548 |
| P | 0.001 | <.001 | 0.001 | <.001 | <.001 |
Table 3: Spearman’s rank-correlation coefficient between body composition and sleep apnea characteristics.
NC as a predictor of OSA
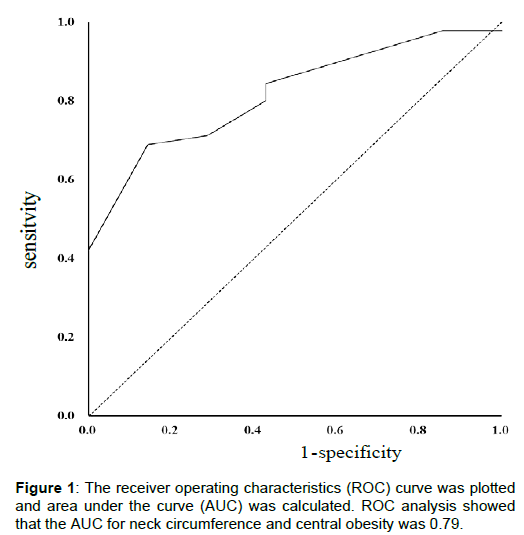
Mean NC was 42.5 ± 3.7 cm. ROC analysis showed that the AUC for NC and central obesity was 0.79. The optimal NC cut-off, as determined using the Youden index, was 40.75 cm; 32.7% of players exceeded this value (Figure 1 and Table 4).
| Neck circumference | Sensitivity | Specificity | Youden index 0.00 |
|---|---|---|---|
| 35.0 | 1.00 | 0.00 | 0.00 |
| 36.5 | 0.98 | 0 | -0.02 |
| 37.25 | 0.98 | 0. 14 | 0.12 |
| 37.75 | 0.96 | 0. 14 | 0.1 |
| 38.5 | 0.89 | 0.14 | 0.03 |
| 39.25 | 0.84 | 0.57 | 0.42 |
| 39.75 | 0.8 | 0.57 | 0.37 |
| 40.25 | 0.71 | 0.71 | 0.43 |
| 40.75 | 0.69 | 0.86 | 0.55* |
| 4 1.25 | 0.64 | 0.86 | 0.5 |
| 41.75 | 0.56 | 0.86 | 0.41 |
| 42.3 | 0.53 | 0.86 | 0.39 |
| 42.8 | 0.51 | 0.86 | 0.37 |
| 43.25 | 0.42 | 1 | 0.42 |
| 43.75 | 0.38 | 1 | 0.38 |
| 44 .5 | 0.29 | 1 | 0.29 |
| 45.5 | 0.2 | 1 | 0.2 |
| 46.25 | 0.18 | 1 | 0.18 |
| 46.75 | 0.16 | 1 | 0. 16 |
| 47.25 | 0.11 | 1 | 0.11 |
| 47.75 | 0.09 | 1 | 0.09 |
| 48.5 | 0.07 | 1 | 0.07 |
| 49.5 | 0.04 | 1 | 0.04 |
| 51 | 0.02 | 1 | 0.02 |
| 53 | 0 | 1 | 0 |
Table 4: Sensitivity, specificity and Youden index for neck circumference.
ESS
A high prevalence of clinically borderline excessive daytime sleepiness was observed. In total, 32 participants (61.5%) reported excessive sleepiness during the day (ESS ≥ 10). Nevertheless, ESS score did not differ significantly between RDI severity groups (Table 1).
Sleep apnea status after dental treatment
In the eight players who accepted treatment (RDI range, 7.6- 33.4 times/h), the MAD significantly decreased RDI, minimum and mean SpO2, total number of snoring episodes and number of snoring episodes per hour, but did not alter the ESS score (Table 5).
| Before Treatment | After Treatment | ||||
|---|---|---|---|---|---|
| Mean | SD | Mean | SD | P | |
| ESS | 11.5 | 3.63 | 10.13 | 1.81 | 0.156 |
| RDI | 21.28 | 11.16 | 7.16 | 2.5 | .003* |
| Minimum SpO2 | 88.63 | 1.85 | 94 | 1.51 | <.001* |
| Mean SpO2 | 93.38 | 0.92 | 95.45 | 1.06 | <.001* |
| Total Snore Events | 658.1 | 442.23 | 11.58 | 4.23 | .004* |
| Snore Events per hour | 73.7 | 63.41 | 2.79 | 1.63 | .015* |
| N=8 | |||||
Table 5: Sleep apnea status before and after mandibular advancement device (MAD) treatment.
Discussion
The key findings showed that, among the 52 Japanese rugby players assessed, 86% had OSA to varying degrees of severity and associated with high NC and BMI. These players experienced excessive daytime sleepiness. The NC cut-off according to the Youden index indicated increased OSA risk in 32.7%. Eight players who accepted OSA treatment with MAD showed improvements in RDI, SpO2 and snoring behaviors.
A high proportion of players displaying OSA is often seen despite the strong physique of rugby players, who are exposed to high-impact physical collisions on the field. This dominance may be linked to certain genetic traits and/or body dimensions. Japanese individuals in general have been reported to have long faces, a racial characteristic that is associated with susceptibility to OSA [26]. In addition, players with moderate to severe RDI were overweight/obese according to the BMI, with mean BMI >31 kg/m2 (Table 2). These observations differed from those reported by Ong and Clerk, in that sleep breathing disorders among Asians tended to be more severe [27] despite a lower BMI than Caucasians.
The players showed a mean NC exceeding 44 cm (Table 2). Players with moderate or severe OSA showed significantly higher BMI and NC than those without OSA (Table 2). BMI and NC predicted RDI and snoring (Table 3). The NC cutoff above which OSA risk began to rise was determined to be 40.75 cm, and the Youden index predicted OSA risk. Our data thus showed that risk associated with NC began 2.25 cm lower than the results reported by of Dixon et al. [8]. NC >43 cm is related to severity of OSA in American patients, with 67% sensitivity and 83% specificity [28]. The thick necks observed in our players may be explained by the facial morphology distinctive to Japanese and the size and position of the lower jaw [29], and also by increased muscle or fat mass in the neck region. However, we are unable to differentiate lean mass from fat mass without, for example, dual-energy X-ray absorptiometry (DXA) screening. The incidence of obesity among Japanese is reportedly 28.7% [30], generally lower than that reported for Westerners, although it is believed that there is no difference in this measure among individuals who snore [28]. In sports like rugby or American football, where body size reduction is not an option and players must also build up strength in the neck, increased player physique increases the risk of obstruction of the pharynx and the risk of OSA. The Japanese rugby players assessed in this study clearly carried an extremely high risk of OSA.
In the present study, 61.5% of players showed ESS score >10, indicating that Japanese players experienced high levels of daytime sleepiness. ESS score was higher than that reported for American football players (mean ESS score, 7.3; score >10 in >20% of players; N=302) [31] or Australian Rules football players (mean ESS score, 8.1; score >10 in 34% of players; N=40) [23], but similar to that reported for college basketball players (mean ESS score, 9.64 ± 3.8) [16]. Almost all players in this study believed that sleepiness was attributable to strenuous training and that their sleep recovery from fatigue was inadequate. This reflection suggests that neither players nor team staff recognized the presence of disordered breathing during sleep. Our view is that increased awareness of sleep apnea is essential, and that players should be provided with options for sleep apnea treatment and advice on nutritional intake to adjust dietary intake and ultimately body fat mass.
OSA is associated with various complications, from hypoxemia to hypertension, ischemic heart disease, and cerebrovascular disorders. Although nasal continuous positive airway pressure (nCPAP) is the most common method of treatment for OSA. However, in nCPAP treatmanet, the national health insurance is covered for OSA patients more than RDI ≥ 40 in Japan. None of the players in this study were eligible for the scheme. Thus, among players who were diagnosed with OSA, only eight players accepted treatment with the MAD at the outpatient snoring clinic of our university hospital. The MAD was a viable option, since these players had no dental problems. Players could elect to receive treatment elsewhere. MAD treatment resulted in significantly improved RDI and arterial oxygen saturation, and reduced total number and the number of snoring episodes per hour. The players reported experiencing an exhilarating feeling on waking and reduced drowsiness during the day, and remarked how much happier their wives and children were at being liberated from the noise of their snoring. However, subjective reports of reduced drowsiness were inconsistent with the recorded ESS score, which did not differ significantly from that before treatment (Table 5). Although the ESS is easy to use, some reports claimed that this tool has a tendency to produce incongruous results [32].
In terms of the therapeutic effects of oral appliance treatment, the MAD is believed to be particularly effective in expanding not only the airway at the root of the tongue, but also the pharyngeal airway during sleep [33]. During preparation of the MAD, orientation of the lower jaw at about 60-70% of the maximum anterior position is desirable. Expansion of the pharyngeal airway is reportedly observed from 67% of the maximum anterior position, and reductions in nasal resistance are also seen [34,35]. However, associated symptoms such as discomfort due to the device, temporomandibular joint symptoms, dry mouth, and changes in occlusion may also reportedly develop, after anterior placement of the lower jaw to ≥50% of the maximum anterior position. Use of the appliance itself as a factor that may disturb sleep must be considered. Any expressions of dissatisfaction or problems reported by players would thus require ongoing management.
Conclusion
Investigation of sleep breathing disorders among top rugby players in Japan indicated that a large proportion of the players had OSA that may be attributable to an increased NC linked to increased lean or fat mass or both, and potentially the characteristic facial morphology of Japanese. The fact that the OSA of players went unnoticed may represent a significant issue. Educational programs to increase awareness of sleep apnea, factors that may influence sleep recovery, and nutritional advice for athletes may be warranted. Through the dental care of athletes, dentists may have a contributory role to play in identifying sleep-related issues that may hinder performance or increase cardiovascular risks.
Conflicts of Interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest.
Funding
The Japanese Ministry of Education, Culture, Sports, Science and Technology provided financial support in the form of Grant–in-Aid for Scientific Research (15K11200) funding. The sponsor played no role in the design or conduct of this research.
Acknowledgements
This study was supported by a Grant-in-Aid for Scientific Research (15K11200) from the Ministry of Education, Culture, Sports, Science and Technology, Japan.
References
- Norton K, Olds T (2001) Morphological evolution of athletes over the 20th century: causes and consequences. Sports Med 31: 763-783.
- Jaric S (2003) Role of body size in the relation between muscle strength and movement performance. Exerc Sport Sci Rev 31: 8-12.
- Anding R, Oliver JM (2015) Football player body composition: importance of monitoring for performance and health. Sports Science Exchange 25: 1-8.
- Kraemer WJ, Torine JC, Silvestre R, French DN, Ratamess NA, et al. (2005) Body size and composition of National Football League players. J Strength Cond Res 19: 485-489.
- Borchers JR, Clem KL, Habash DL, Nagaraja HN, Stokley LM, et al. (2009) Metabolic syndrome and insulin resistance in Division 1 collegiate football players. Med Sci Sports Exerc 41: 2105-2110.
- Ben-Noun L, Sohar E, Laor A (2001) Neck circumference as a simple screening measure for identifying overweight and obese patients. Obes Res 9: 470-477.
- Onat A, Hergenç G, Yüksel H, Can G, Ayhan E, et al. (2009) Neck circumference as a measure of central obesity: associations with metabolic syndrome and obstructive sleep apnea syndrome beyond waist circumference. Clin Nutr 28: 46-51.
- Dixon JB, Schachter LM, O Brien PE (2003) Predicting sleep apnea and excessive day sleepiness in the severity obese: Indicators for polysomnography. Chest 123: 1134-1141.
- Leeder J, Glaister M, Pizzoferro K, Dawson J, Pedlar C (2012) Sleep duration and quality in elite athletes measured using wristwatch actigraphy. J Sports Sci 30: 542-545.
- Reilly T, Piercy M (1994) The effect of partial sleep deprivation on weight-lifting performance. Ergonomics 37: 107-115.
- Mougin F, Simon-Rigaud ML, Davenne D, Renaud A, Garnier A, et al. (1991) Effects of sleep disturbances on subsequent physical performance. Eur J Appl Physiol 63: 77-82.
- Jarraya M, Jarraya S, Chtourou H, Souissi N (2013) The effect of partial sleep deprivation on the reaction time and the attentional capacities of the handball goalkeeper. Biol Rhythm Res 44: 503-510.
- Edwards BJ, Waterhouse J (2009) Effects of one night of partial sleep deprivation upon diurnal rhythms of accuracy and consistency in throwing darts. Chronobiol Int 26: 756-768.
- Venter R (2008) Sleep for performance and recovery in athletes. Continuing Medical Education 26: 331-333.
- Reddan G (2010) The use of the total quality recovery model in determining optimal training loads and recovery periods. Conference of Science, Medicine & Coaching in Cricket 2010. Brisbane, Melbourne, Australia.
- Mah CD, Mah KE, Kezirian EJ, Dement WC (2011) The effects of sleep extension on the athletic performance of collegiate basketball players. Sleep 34: 943-950.
- Venter RE (2014) Perceptions of team athletes on the importance of recovery modalities. Eur J Sport Sci 14 Suppl 1: S69-76.
- Motivala SJ, Irwin MR (2007) Sleep and immunity. Cytokine pathways linking sleep and health outcomes. Curr Dir Psychol Sci 16: 21-25.
- Halson SL (2014) Sleep in elite athletes and nutritional interventions to enhance sleep. Sports Med 44: 13-23.
- Haack M, Mullington JM (2005) Sustained sleep restriction reduces emotional and physical well-being. Pain 119: 56-64.
- Nakayama-Ashida Y, Takegami M, Chin K, Sumi K, Nakamura T, et al. (2008) Sleep-disordered breathing in the usual lifestyle setting as detected with home monitoring in a Japanese male working population. Sleep 31: 419-425.
- Zaghi S, Holty JE, Certal V, Abdullatif J, Guilleminault C, et al. (2016) Maxillomandibular advancement for treatment of obstructive sleep apnea: A meta-analysis. JAMA Otolaryngol Head Neck Surg 142: 58-66.
- Takegami M, Suzukamo Y, Wakita T, Noguchi H, Chin K, et al. (2009) Development of a Japanese version of the Epworth Sleepiness Scale (JESS) based on item response theory. Sleep Med 10: 556-565.
- Antic NA, Weeks R, McEvoy D, Sargent C, Jarema L, et al. (2013) Prevalence of sleep disorders and excessive daytime sleepiness in an elite Australian Rules football team. Am J Respir Crit Care Med 187: A3455.
- Taube A (1986) Sensitivity, specificity and predictive values: a graphical approach. Stat Med 5: 585-591.
- Nezu H, Nagata K, Yoshida Y, Kosaka H, Kikuchi M (1982) Cephalometric comparison of clinical norms between the Japanese and Caucasians. J Jpn Orthod Soc 4: 450-465.
- Ong KC, Clerk AA (1998) Comparison of the severity of sleep-disordered breathing in Asian and Caucasian patients seen at a sleep disorders center. Respir Med 92: 843-848.
- Stierer T, Punjabi NM (2005) Demographics and diagnosis of obstructive sleep apnea. Anesthesiol Clin N Am 23: 405-420.
- Kikuchi M, Higurashi N, Miyazaki S, Itasaka Y (2000) Facial patterns of obstructive sleep apnea patients using Ricketts' method. Psychiatry Clin Neurosci 54: 336-337.
- National Health and Nutrition Examination Survey in Japan. Japan Ministry of Health, Labour and Welfare.
- George CF, Kab V, Kab P, Villa JJ, Levy AM (2003) Sleep and breathing in professional football players. Sleep Medicine 4: 317-325.
- Chervin RD, Aldrich MS (1999) The Epworth Sleepiness Scale may not reflect objective measures of sleepiness or sleep apnea. Neurol 52: 125-131.
- Tsuiki S, Lowe AA, Almeida FR, Kawahata N, Fleetham JA (2004) Effects of mandibular advancement on airway curvature and obstructive sleep apnoea severity. Eur Respir J 23: 263-268.
- Tsuiki S, Hiyama S, Ono T, Imamura N, Ishiwata Y, et al. (2001) Effects of a titratable oral appliance on supine airway size in awake non-apneic individuals. Sleep 24: 554-560.
- Okawara Y, Tsuiki S, Hiyama S, Hashimoto K, Ono T, et al. (2004) Oral appliance titration and nasal resistance in nonapneic subjects. Am J Orthod Dentofacial Orthop 26: 620-622.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi