Research Article, J Sleep Disor Vol: 9 Issue: 3
Development of an Unobtrusive Sleep Monitoring System using a Depth Sensor
Jangwoon Park1, Jungyoon Kim2, Jaehyun Park3*, DeJeanne Adams4, Celeste Branstrom5
1Department of Engineering, Texas A&M University-Corpus Christi, USA
2Department of Computer Science, Kent State University, USA
3Department of Industrial & Management Engineering, Incheon National University, South Korea
4Department of Kinesiology, Texas A&M University-Corpus Christi, USA
5Department of Biological & Agricultural Engineering, Texas A&M University, College Station, USA
*Corresponding Author: Jaehyun Park
Department of Industrial & Management Engineering, Incheon National University, South Korea
Tel: 82-32-835-8867
E-mail: jaehpark@inu.ac.kr
Received: May 10, 2020 Accepted: July 20, 2020 Published: July 24, 2020
Citation: Park J, Kim J, Park J, Adams D, Branstrom C (2020) Development of an Unobtrusive Sleep Monitoring System using a Depth Sensor. J Sleep Disor: Treat Care 9:3. doi: 10.37532/jsdtc.2020.9(3).231
Abstract
The elderly, who are isolated and neglected, can experience to an increased likelihood of age-related sleep disorders. Early detection, proper diagnosis, and treatments for sleep disorders can be achieved by identifying sleep behaviours through long-term monitoring. Although many studies developed sleep monitoring systems by using non-invasive measures, research is still limited to detect sleep behaviours using an infrared 3D depth camera. The present study has two main goals: a) identifying design characteristics on the existing sleep monitoring systems based on the extensive literature review; b) developing a non-invasive sleep monitoring system using a 3D depth camera. For the literature review, several journal papers have been reviewed to identify the design features, classification accuracy, and embedded algorithms of the existing sleep monitoring systems. For the system development, a sleep posture monitoring system was developed, using a Microsoft Kinect II depth sensor. For the validation of the developed system, the differences of sleep behaviours between the two participants were investigated. The developed system used an unobtrusive measure and it would be useful for long-term monitoring on sleep behaviours for the senior population.
Keywords: Sleep Quality; Sleep Monitoring System; Sleep Pattern; Kinect II Depth Sensor
Introduction
Improper sleep quality of senior people can make negative physiological, psychological, and social impacts (e.g., decreased social activities and social isolation), causing a range of health problems, which including coronary heart disease, depression, anxiety, and loneliness on the senior population. Dickerson (2011) reported that sleep apnea, restless leg syndrome, the use of medications, and psychiatric disorders, such as anxiety and depression, are all examples of sleep disorders diagnosed in senior populations. Corman and Leger (2004) identified an increase in sleep latency in the senior group by using polysomnography (PSG) and reported that the sleep latency in the senior population may result from the circadian changes by age. Moreover, the seniors were getting a decreased amount of slow-wave sleep, which results in fragmented sleep, early awakening, and even the progression of Alzheimer’s disease [1-3]. Therefore, to resolve the sleep issues for the senior population, early detection and diagnoses of various sleep disturbances are needed by using sleep monitoring systems to mitigate age-related sleep issues.
There are three different types of sleep monitoring system are being developed and they have pros and cons. The first method is using PSG, which is the most popular and adopted as a medical standard. The PSG can measure various bio-signals during the sleep, such as heart rate, brain activities, and airflow, and the measurements are the most accurate to diagnose sleep quality [4]. However, in order to measure the PSG measurements, many sensors need be attached on a patient’s skin, which may hinder the patient’s sleep quality. In addition, the examination fee is relatively high (e.g., $150 - $500 USD per patient) and it can only be measured in a lab environment (e.g., sleep lab).
The second method is the autography, which monitors the physiological signals including body movements to classify sleep stages. The autography was used to evaluate sleep patterns with insomnia in the research of sleep and circadian rhythms [5]. The wearable autography-recording device was proposed to assess sleep quality by using the body movement signals [6]. The autography commonly used wearable devices, such as smart phone [7], smart watch [8], and fitness tracker [9]. These wearable devices use builtin accelerometers to track the body movement, which is known as one of significant measures for evaluating sleep quality [10]. Some autography tools reach good performances compared with the gold standard (PSG) [11,12]. The third group uses Wi-Fi signals to detect sleep movement, such as DoppleSleep [13] and Wi-Sleep systems [14]. These devices are particularly useful to accurately detect sleep movements without attaching any sensors on the skin. The one drawback is that the devices do not obtain as many measurements as the PSG.
There are two main goals in this study. The first goal is to understand the characteristics of the existing sleep monitoring systems. In the literature review section, we have summarized currently-available systems to monitor sleep quality. The second goal is to develop an unobtrusive sleep monitoring system that can measure sleep behaviours of elderly people by using an unobtrusive sensor. The novel sleep monitoring system is developed by incorporating wireless and a nonintrusive 3D motion sensing technology. The developed system utilizes a touchless sensor technology (i.e. Microsoft Kinect II depth sensor) that can unobtrusively and precisely collect a person’s sleep postures during the sleep. Specifically, the sensor can record 3D distances (depths) between a sleeper and a camera on a millimetre level. The developed system is validated in this study with two participants. The system would be useful to detect age-related sleep behaviours (e.g., restless leg syndrome) of the senior population.
Literature Review
The primary review sources were conference proceedings and journal articles found on various online databases (medical journal search engines including PubMed, Ovid, Web of Science, Science Direct, Scopus, Cochrane Library, and Google Scholar). The review results in this paper were not just limited to academic papers, but websites and news were also taken into consideration. The National Center for Biotechnology Information (NCBI) was a website that leads to an abundance of resources. All the search keywords were “sleeping conditions,” “sleep position,” and “quality.” Other phrases and words that were included in this search were “sleep monitoring systems” or “devices.” Selection of a review article was dependent on two main factors, the published date and the information contained in the sources.
Many researchers have defined the definition of good sleep quality in terms of subjective measures or objective judgments. Chaput and Team defined sleep quality as a subjective assessment of how each participant felt after a night of sleep. For example, multiple self-reported questionnaires are important to determine the quality of sleep and the subjective assessment. Chaput also defined highquality sleep as a means of having the efficiency of staying asleep, since the amount of a participant’s sleep is crucial to sleep quality. Pittsburgh Sleep Quality Index (PSQI) is a simple and widely used instrument for evaluating/diagnosing the quality and patterns of sleep in adults [15]. An evaluation score of PSQI is given, based upon seven components: (1) subjective sleep quality, (2) sleep latency, (3) sleep duration, (4) habitual sleep efficiency, (5) sleep disturbances, (6) use of sleep medications, and (7) daytime dysfunction. The assessment can be done by the participant, and a healthcare provider should be consulted if a score is five or more. Similarly, the Insomnia Severity Index (ISI) is also a well adopted instrument, due to its simplicity. It has seven questions that can serve as guidelines for scoring/ interpreting sleep quality [16].
On the other hand, the National Sleep Foundation in 2017 determined objective measures defining good sleep quality, such as not waking up more than once at night, falling asleep in 30 minutes or less, and sleeping 85% of the total time designated for sleep. Furthermore, there are objective measurements for obstructive sleep apnea (OSA), such as the apnea-hypopnea index (AHI) and respiratory disturbance index (RDI). The AHI is the number of apneas and hypopneas recorded during the sleep study within each hour of sleep [17]. RDI is similar, but the number is usually greater, due to the inclusion of other breathing irregularities, as well as apneas and hypopneas [18].
Sleep quality and OSA can also be diagnosed by a sleeper’s brain activities in each sleep stage. Sleep stage is broken into two groups based on eye movement patterns, rapid eye movement (REM) and non-rapid eye movement (NREM). NREM is divided into four stages that are dependently unique. The subcategories of NREM are monitored by electroencephalography (EEG) activity. In the first stage (called stage I), the EEG shows low voltage with mixed frequency waves. This stage is the easiest to disturb and usually counts for a maximum of 5% of the total sleep cycle. In the second stage (stage II), the EEG shows low voltage with mixed frequency waves, along with sleep spindles and K-Complexes. Stage II is where 45-55% of sleep is spent. In stage III, where 3-8% of all sleep is spent, an EEG shows high voltage with slow wave activity. While stage IV is similar concerning slow wave activity, it shows a higher voltage and counts for 10-15% of the time spent sleeping. Both stage III and IV are considered slow wave systems. The final portion of the sleep cycle is when REM sleep and dreams occur [19].
One popular sleep monitoring device is the Fitbit. The Fitbit is a small, more affordable, wrist-worn, minimally invasive way to improve the quality of sleep. Kahn and Kinsolving described their methods of monitoring a user’s movements and determining when the user is falling asleep by using Fitbit. The Fitbit has the ability to track activities, which can improve sleep pattern. The Fitbit can set the alarm for a specific time or wake the user at the proper time during a sleep cycle before drifting into a deeper stage of sleep. This allows users to wake at an appropriate time without feeling sluggish, rather than being abruptly woken up in the middle of NREM sleep stage II, the longest stage in the NREM cycle.
Various noninvasive sleep monitoring systems, such as smartphone apps, vision-based, frequency signal-based, and pressure-based sleep monitoring systems, are being developed. Alqassim et al. created a smartphone application named Sleep Apnea Monitor (SAM) to monitor and detect symptoms of sleep apnea, using built-in sensors that smartphones have: built-in microphone, accelerometer, GPS receiver, and WiFi capabilities. Movements and breathing rates were recorded while the user slept. The data was stored on a database management server. Since a user can show results to a physician, there is potential within this software that could be useful. Off-the-shelf WiFi devices can make sleep monitoring technologies more accessible and less invasive. Liu et al. in 2014 created a WiFi device, using line-of-sight interference to observe breathing rates by observing changing interference levels. Respiratory data was able to be accurately monitored when the participants were sleeping, either on their sides or backs, though not when the participants were on their stomachs. Liu et al. in 2016 used the system to determine both breathing rates and position changes. The study showed that determining the sleep position can accurately determine respiration rate, even when the participant slept on their stomachs. The 30-second pauses in breathing were accurately diagnosed with an accuracy of 82.1%. The studies show how breathing rates can be noninvasively measured and used to determine the time spent in the different sleep stages. Liu and Ostadabbas strived to make a tracking system of inbed postures while sleeping. They used a vision-based method, due to low cost and easy maintenance, compared to a pressure sensor mat. They found that the supine position shows more frequency than the stomach or side position. Liu et al. also analyzed sleeping posture using pressure sensors. Each posture was distinguished with physical meanings, using the data collected from the dense pressure sensitive bed sheet and a statistical equation.
Various in-home based sleep monitoring systems have been developed. Mack et al. studied a non-invasive analysis of physiological signals (NAPS) and found it to be useful as a home health tool for assessing patients’ sleeping habits in an assisted living environment. NAPS has four temperature sensors and two compliant forcecoupling pads that can track body movements from the respiratory effort and postural changes. Cardiac contraction and relaxation can also be measured. Preliminary validation results show a sensitivity of 89.2% and a specificity of 94.6%, compared to traditional PSG. Mack et al. used a ballistocardiography (BCG) system to monitor the heart rate and the breathing rate while sleeping. Due to the system’s accuracy when compared with ECG results, the BCG system is a potential candidate for a non-invasive home sleep monitoring system. Kortelainen et al. used a BCG sensor developed by the researchers that accurately determined breathing rate data when compared to data from a respiration belt. These studies show how BCG systems can be used to develop non-invasive accurate sleep monitoring systems that can be used in locations outside of a laboratory or hospital.
There are also some other products that help with sleep control, such as SleepMate, YuMe Hi-Tech Mattress, and NightWave. The SleepMate 980A White Noise Sound Conditioner helps with improving sleep by masking unwanted sounds, which leads to a more restful sleep. The YuMe Hi-Tech Mattress controls the temperature specifically to an individual’s needs and delivers top-notch comfort. The NightWave sleep assistant can emit a soft, slow oscillating blue light. This device is used to help relax the user enough to aid in falling asleep. The literature review results for the existing sleep monitoring systems are summarized in (Table 1).
| Monitored Data | Type of System | Device Studied | Collection/ | Performance | Commercial Use |
|---|---|---|---|---|---|
| data method | |||||
| Respiration | Force sensing resistors | Lokavee et al. [29] | Sensor Pillow and bed sheet | - | Yes |
| Non-Invasive Analysis of Physiological Signals (NAPS system) | Mack et al. | Passive BCG. Heart Rate and Breathing rate were also recorded | Sensitivity 89.2% | No | |
| [27] | Specificity 94.6% | ||||
| Nasal/Oral Airflow, respiratory effort, blood oxygen levels | Chest system, nasal sensors, finger clip | At home PSG system | PSG | - | No, but it can be used at home |
| Heart Rate/ Movement | wearable watch | Fitbit | Accelerometer | - | Yes |
| Smartwatch | Sun et al. [8] |
Accelerometer | Movement 87% | Yes | |
| Doppler Technology | Rahman et al. [13] |
Off the shelf K-band 24GHz radar module. Electromagnetic waves | Breathing 89.2% | Not yet—still needs improvement | |
| H.R. 91.9% | |||||
| Self-powered Triboelectric Nanogenerator | Song et al. [30] |
A sensor attached to shoulder & leg to monitor body movement | - | No | |
| Position | Off the shelf device | Liu et al. [14] |
Wi-Fi | Detection error | No |
| < 20% | |||||
| Pressure sensitive textile bed sheet sensor | Liu et al. [14] |
Pressure image analysis for recognition | - | No | |
| Pulse rate and oxygen saturation | Wearable watch and finger clip | PC 68B - Smart Home Sleep Monitor | - | - | Yes - at home use |
| ECG Monitoring on bed | Indirect contact ECG | Lim et al. [31] |
High input impedance active electrodes fixed on the mattress. | - | Yes |
| Nightcap: A Home-Based Sleep Monitoring System | Nightcap: A Home-Based Sleep Monitoring System | Time-lapse photography and electromyography (EMG) | - | Yes |
Table 1: Summary of the studies regarding sleep monitoring systems.
Sleep Monitoyring System using a 3D Depth Camera
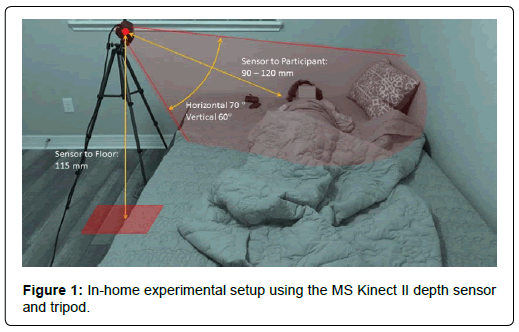
The present study utilized Microsoft Kinect II depth sensor, that can unobtrusively measure sleep movement. Note that the price of MS Kinect II sensor is around USD 200, which is relatively cheaper than other high-resolution bio-signal measurement devices. As shown in (Figure 1), the sensor can be located right next to the bed, and the sensor can capture the participant’s body movements based on the depth changes. The resolution of the depth data is 512 × 424 pixels, and each pixel contains a distance (unit: millimeters) between the sensor and the participant. Therefore, because the camera location is fixed, if there are any body movements, then the depth value of each pixel will then be changed due to the distance changes between the depth camera and a participant’ body. The sampling rate we used in this study was 30 frames per second. The detailed specifications of the proposed sleep monitoring system including MS Kinect II depth sensor and the tripod are shown in (Table 2) and (Figure 1), respectively. (Table 2) shows the detailed specification of the MS Kinect II depth sensor in terms of camera resolution and field of view (degrees). According to the Lachat et al., Kinect II depth sensor can measure a depth with a consistent accuracy (less than 3 mm error). In addition, Wasenmüller & Stricker (2016), Butkiewicz (2014), Giancola et al. (2018) highlighted the accuracy, robustness, and stability of the MS Kinect II depth sensor. (Figure 1) also shows the dimensions of the proposed sleep monitoring system.
| Feature | Specification |
|---|---|
| Depth | Camera Resolution: 512 × 424 pixels |
| Frame rate: 30 frames per second | |
| Measurement rage: from 0.5 m to 4.5 m | |
| Field of view | Horizontal: 70 degrees |
| Vertical: 60 degrees |
Table 2: The specification of the MS Kinect II depth sensor by Jiao et al.
As shown in (Figure 2), a computerized system was developed to collect depth data. In addition, the system calculated an averaged depth data. This single value would be particularly useful to identify whether there is a sleep movement or not. This experimental protocol was approved by Texas A&M University-Corpus Christi Institutional Review Board (IRB) (IRB ID: NHS 13-19). We presumed that there would be a substantial age effect on body movement during sleep [1,2]. Therefore, we recruited two adults, one is a male who is 33 years old (YO) and the other one is an older female who is 84 YO who has a restless leg symptom, which is one of age-related sleep disorders.
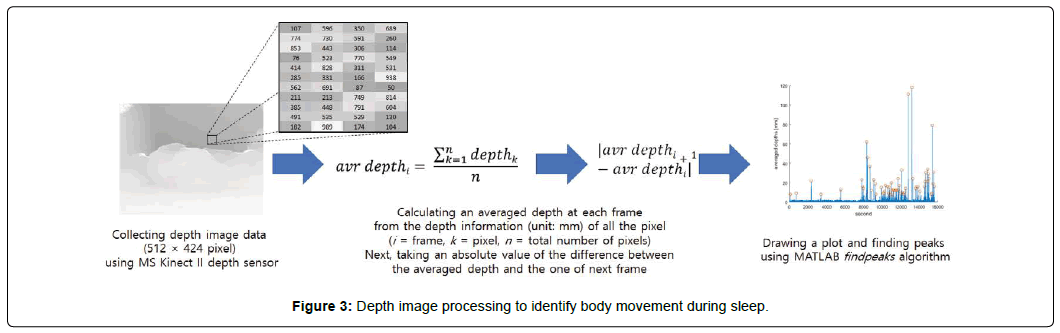
The data processing procedure consists of four steps as shown in (Figure 3): 1) Measuring depth images (512 x 424 pixel) using the MS Kinect II 3D depth sensor with an infrared feature at a sampling rate of 1 Hz (one frame per second), 2) calculating an average depth of all the pixels at each frame, 3) calculating the difference at each frame by subtracting the averaged depth from the one of the next frame, 4) plotting the absolute values of the differences along the time frame (See (Figure 4A and 4B); x-axis indicates measuring time in second and y-axis indicates the absolute difference), and then finding peaks using the MATLAB function (find peaks algorithm: It is the builtin MATLAB function finding local minimum values of the input signal vector. The local peak is a data sample that is larger than its two neighbouring samples). After finding peaks, several features (e.g., number of peaks, peak interval) can be extracted from the plot to analyse how many body movements occurred during sleep.
To find the true signals of sleep movements for both participants, we set the two parameters (minimum peak height and minimum peak distance), which are options of the MATLAB find peak function. First, we wanted to find peaks that have an amplitude of at least 7 mm to ignore small-scale movements (e.g., breathing) by adjusting the minpeakheight parameter. The amplitude was determined based on the Groote et al. (1997)’s study (averaged chest movement during breathing = 3 – 5 mm). Second, we restricted the acceptable peak-topeak separations using the values greater than 35 second by adjusting the minpeakdistance parameter, which was determined by the visual observations on the peak data. This time span enables us to improve the accurate detection of the sleep movements by ignoring the local peaks that are too small or very close to each other. However, these parameters can be slightly adjusted depending on an experimental setup such as position or angle of a camera which might affect an averaged depth. Since the depth sensor can detect human motion with an acceptable accuracy, and the MATLAB minimum peak height and interval are adjustable, we can detect sleep movements even in a second. However, based on our visual observations on the collected data, 35 seconds would be appropriate as a peak-to-peak interval for detecting meaningful body movements (e.g., body, head, or leg rolling). If the peak interval is shorter than 35 seconds, the system would yield too high sensitivity, but poor specificity. Likewise, the 7 mm peak height would be appropriate in the proposed system in terms of acceptable sensitivity and specificity.
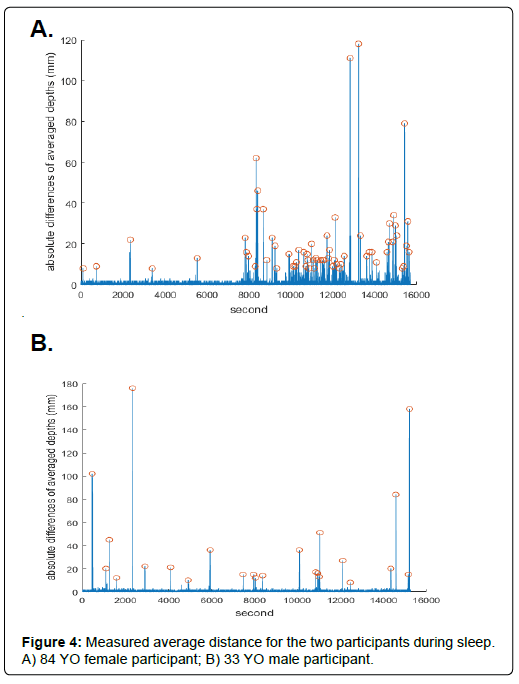
(Figure 4A) shows the averaged depth of the female participant for around four hours sleep. By using the MATLAB findpeaks function, we accurately identified the peak values (circled in red), which indicate body movements. It is expected that the first movement occurred at the beginning of the recording, and the participant well maintained the sleep positions until 8,000 s (2.2 hours). However, after around 8,500 s, the female participant started to move the body frequently, ultimately causing poor sleep quality. Because the participant went a rest room, there are two big spikes between 12,000 s and 14,000 s in (Figure 4A), which means that we can use the magnitude of the averaged depth to determine how much body movement occurred. Also, if there is no spike (flat height in the graph), then we can anticipate that the participant does not change the sleep position over a certain amount of time. On the other hand, as shown in (Figure 4B), the male participant showed relatively stable sleep position throughout the experiment compared to the older female participant. The male participant changed the sleep posture less frequently compared to the female participant, also once the body movement was occurred, then the younger male participant could maintain the changed sleep position steadily. Therefore, we can conclude that the male participant well maintained the sleeping posture or position compared to the senior female participant based on the collected depth data.
Table 3 summarizes the computational results generated by the body movement detection algorithm that we evaluated with video recorded annotations; we list sensitivity, specificity, positive- predictivity and accuracy. Overall, our method afforded an accuracy of 99.56%, sensitivity of 86.18%, specificity of 99.78% and positivepredictivity of 86.18%, which are the commonly used performance metrics. We also evaluated the proposed movement detection algorithm about the two participants. The overall performance of the 33 YO male participant shows better performance than the 84 YO female participant’s performance.
| % | Sensitivity | Specificity | Positive-Predictivity | Accuracy |
|---|---|---|---|---|
| 84 YO female participant | 84.83 | 99.69 | 84.83 | 99.38 |
| 33 YO male participant | 89.44 | 99.89 | 89.44 | 99.78 |
| All | 86.18 | 99.78 | 86.18 | 99.56 |
Table 3: Comparison of the detection performance for the two participants.
Discussion
The present paper is completely different from the previous proceeding [20-37] in two major aspects. First reason is that the present work includes extensive literature reviews for the sleep monitoring systems and more finding are summarized at the section “Literature Review”. Although the previous work showed some literature reviews on the sleep monitoring system, the review was limited to PSG, wearable devices, and WiFi methods. On the other hand, the present literature review encompasses not just previous works, but also PSQI, ISI, RDI, and bio-signals (e.g., respiration rate, heart rate, airflow, and pulse), which are never published elsewhere. The second reason is that the proposed detection method for sleep movement is done by MATLAB findpeaks algorithm, which is never shown in the previous work. The proposed algorithm is more useful to accurately and automatically find the sleep movements from the depth data than the previous method, which was relying on visual observations.
The present paper introduces the existing methods to monitor sleep quality based on extensive reviews. The review results would be particularly useful for researchers and engineers to understand or inform the existing technology, metrics, performance, and research trend. The research we collected aimed to provide information on existing sensing technologies that accurately and consistently produced results on determining sleeping disorders. This paper provides the knowledge of specific testing aspects used by each technology. As stated before, PSG produces the most accurate metrics but is very costly. PSG consists of monitoring and analyzing airflow, respiratory movement, oxygen saturation, brain activity, eye/jaw movement, and heart activity. While PSG is the number one sensing technology, other technologies can be developed based on the PSG testing parameters. For example, one study showed that simply by attaching a wristwatch on the patient's arm could analyze changes in heart rate and position from back to the left or right side. In addition, we can find that the technology in sleep monitoring system has been changed toward a more non-invasive and accurate detecting method with advanced machine learning algorithms on non-invasive measurements (e.g., WiFi signal).
Non-invasive measures can also be substituted for PSG to allow for more natural and positive sleep analysis, rather than attaching sensors, watches, head gear, to analyze possible sleep disorders. Recently, more apps have been created and available to use on smartphones to analyze changes in breathing, detecting snoring, and being able to differentiate between the person sleeping or waking up throughout the night. The optimal approach we gathered towards the end of our research concluded that the non-invasive tests allowed for more accurate predictions because the patient was able to sleep as normal as possible.
Mathematical approaches can be incorporated to predict changes in breathing, heart rate, or oxygen saturation. Many existing studies used PSG measurements as a gold standard to compare with a new sleep monitoring device developed by themselves. PSG measurements are known as the most accurate metrics, and currently, they are widely accepted in a medical field to identify a patient’s sleep stage or OSA symptoms. However, in the real world, collecting or accessing patients’ PSG data is not easy for general engineering researchers in terms of cost or regulation issues, respectively. Therefore, it would be beneficial to a sleep researcher, if there is a generalizable model developed by using a large cohort of PSG datasets, which can identify the sleep patterns of patients. For example, mathematical equations do exist that can suggest possible sleep disorders. The NAMES assessment (neck circumference, airway classification, comorbidities, Epworth scale, and snoring) was developed for a better screening tool for OSA with up to 99% of classification sensitivity [38-40].
The effectiveness of the developed unobtrusive-sleep-monitoringsystem has been validated by collecting data from the human-subject experiment. As shown in the (Figure 3), different body movement patterns between two different age people were clearly identified by a visual observation on the sleep movement charts (Figure 3A and 3B). Since the measurement is in millimeter level scale, the collected data would be useful to precisely identify abnormal sleep patterns of the senior personnel in terms of early detection. However, the usefulness of the proposed system in the medical field needs to be validated with the PSG measurements (gold standard) or a sleep experts, nurses, and physicians’ opinions.
The developed system can be seamlessly connected with a healthcare provider, so that an isolated elderly can be monitored and healed in real time. This is particularly important to care a vulnerable older person living alone, often in isolated circumstances, from undesirable age-related sleep disorders, since the circumstances of people dying alone were often the result of a degree of social isolation [41]. In addition, because the developed system can unobtrusively detect sleep movements, the system could be ideal to monitoring even patients in a hospital setting, who do not like to attach sensors to the skin. Since the current study is a pilot study to validate the developed sleep monitoring system, we may need to recruit more participants to collect sleep data, so that an accurate sleep classification models can be developed.
Conclusion
Based on the literature review, we understand the pros and cons of the three types sleep monitoring systems (PSG, wearable device, and Wi-Fi device), and there is a consensus that an accurate, nonobtrusive, and cost-effective sleep monitoring system needs to be developed. In this study, we present the sleep monitoring system using MS Kinect II 3D depth sensor, which can measure body movement non-invasively and cost-effectively. The system shows acceptable accuracy to identify and quantify the body movement during sleep. Since senior people resist to attach any sensor on the skin during sleep, the developed system would be useful to monitor sleep quality in senior care facilities or any home-based environment.
As a future study, it is necessary to develop a sleep position classification model after collecting data from various people. Analysing the statistical effects of age on sleep position is important, but monitoring and early diagnosis of sleep disorders is more important, which requires the development of mathematical classification models that can determine normal and abnormalities. Subsequent research will collect averaged 3D depth patterns for people of various ages and then develop sleep position classification models by incorporating human dimensions, such as demographic information as well as anthropometric dimensions. The models would be particularly useful to detect sleep disorders for the older population, so that they will eventually contribute to reduce medical costs and improve sleep quality. Also, the classification models need to be validated with other medical level devices and sleep experts’ opinions.
Acknowledgement
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIP) (No. 2018R1C1B6008848).
References
- Dickerson RF, Gorlin EI, Stankovic JA (2011) Empath: A continuous remote emotional health monitoring system for depressive illness. In Proceedings of the 2nd Conference on Wireless Health 5: 1-10.
- Corman B, Léger D (2004) Sleep disorders in the elderly. La revue du praticien, 54: 1281-1285.
- Varga AW, Wohlleber ME, Giménez S, Romero S, Alonso JF et.al., (2016) Reduced slow-wave sleep is associated with high cerebrospinal fluid Aβ42 levels in cognitively normal elderly. Sleep 39: 2041-2048.
- Douglas NJ, Thomas S, Jan, MA (1992) Clinical value of polysomnography. Lancet 339: 347-350.
- Israel S A, Cole R, Alessi C, Chambers M, Moorcroft W et.al., (2003) The role of actigraphy in the study of sleep and circadian rhythms. Sleep 26: 342-392.
- Abeyratne UR, Wakwella AS, Hukins C (2005) Pitch jump probability measures for the analysis of snoring sounds in apnea. Physiol Meas 26: 779-798.
- Chen Z, Lin M., Chen, F, Lane ND, Cardone G et.al.,(2013) Unobtrusive sleep monitoring using smartphones. In Proceedings of the 7th International Conference on Pervasive Computing Technologies for Healthcare. ICST 145-152
- Sun X, Qiu L, Wu Y, Tang Y, Cao G (2017). Sleepmonitor: Monitoring respiratory rate and body position during sleep using smartwatch. Proceedings of the ACM on Interactive, Mobile, Wearable and Ubiquitous Technologies 1: 104.
- Mansukhani MP, Kolla BP (2017) Apps and fitness trackers that measure sleep: Are they useful. Cleve Clin J Med 84: 451-456.
- Seneviratne S, Hu Y, Nguyen T, Lan G, Khalifa S (2017) A survey of wearable devices and challenges. IEEE Communications Surveys & Tutorials 19: 2573-2620.
- Ibáñez V, Silva J, Cauli O (2018). A survey on sleep assessment methods. PeerJ 6: 4849.
- Crivello A, Barsocchi P, Girolami M, Palumbo F (2019) The Meaning of Sleep Quality: A Survey of Available Technologies. IEEE Access 7: 167374-167390.
- Rahman T, Adams AT, Ravichandran RV, Zhang M, Patel, SN et.al., (2015) Dopplesleep: A contactless unobtrusive sleep sensing system using short-range Doppler radar.ACM International Joint Conference on Pervasive and Ubiquitous Computing 39-50.
- Liu X, Cao J, Tang S, Wen J, Guo P (2016) Contactless Respiration Monitoring Via Off-the-Shelf WiFi Devices. IEEE Transactions on Mobile Computing 15: 2466-2479.
- Chaput JP, Gray CE, Poitras VJ, Carson V, Gruber R et.al., (2016) Systematic review of the relationships between sleep duration and health indicators in school-aged children and youth. Appl Physiol Nutr Metab41: S266-S282.
- Buysse DJ, Reynolds III CF, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28: 193-213.
- Bastien CH, Vallières A, Morin CM (2001). Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med 2: 297-307.
- National Sleep Foundation (2017) What is Good Quality Sleep? Retrieved March 21, 2018, from https://sleepfoundation.org/press-release/what-good-quality-sleep
- Division of Sleep Medicine at Harvard Medical School (2011). Retrieved January 31, 2019, from http://healthysleep.med.harvard.edu/sleep-apnea/diagnosing-osa/understanding-results
- De Groote A, Wantier M, Chéron G, Estenne M, Paiva M (1997) Chest wall motion during tidal breathing. J App Physiol83: 1531-1537.
- Westbrook PR, Levendowski DJ, Cvetinovic M, Zavora T, Velimirovic V et.al., (2005) Description and validation of the apnea risk evaluation system: A novel method to diagnose sleep apnea-hypopnea in the home. Chest 128: 2166-2175.
- Colten HR, Altevogt BM (2006) Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. National Academies Press.
- Kahn P R, Kinsolving A (2015). Sleep Monitoring System. United States Patent 1-28.
- Alqassim S, Ganesh M, Khoja S, Zaidi M, Aloul F et.al., (2012) Sleep Apnea Monitoring Using Mobile Phones. International Conference on e-Health Networking, Applications, and Services. 443-446.
- Liu, JJ, Huang MC, Xu W, Zhang X, Stevens L et.al., (2015) Breathsens: A continuous on-bed respiratory monitoring system with torso localization using an unobtrusive pressure sensing array. IEEE J Biomed Health Inform19: 1682-1688.
- Liu S, Ostadabbas S (2017) A vision-based system for in-bed posture tracking. In Proceedings of the IEEE International Conference on Computer Vision 1373-1382.
- Mack DC, Patrie JT, Suratt PM, Felder RA, Alwan M (2008) Development and preliminary validation of heart rate and breathing rate detection using a passive, ballistocardiography-based sleep monitoring system. IEEE Trans Inf Technol Biomed 13: 111-120.
- Kortelainen JM, Van Gils M, Pärkkä J (2012) Multichannel bed pressure sensor for sleep monitoring. In 2012 Computing in Cardiology 313-316.
- Lokavee S, Puntheeranurak T, Kerdcharoen T, Watthanwisuth N, Tuantranont A (2012) Sensor pillow and bed sheet system: Unconstrained monitoring of respiration rate and posture movements during sleep. In 2012 IEEE International Conference on Systems, Man, and Cybernetics (SMC) 1564-1568
- Song W, Gan B, Jiang T, Zhang Y, Yu A et.al. (2016) Nanopillar arrayed triboelectric nanogenerator as a self-powered sensitive sensor for a sleep monitoring system. ACS nano 10: 8097-8103.
- Lim YG, Kim KK, Park KS (2007) ECG recording on a bed during sleep without direct skin-contact. IEEE Transactions on Biomedical Engineering 54: 718-725.
- Lachat E, Macher H, Mittet MA, Landes T, Grussenmeyer P (2015) First experiences with Kinect v2 sensor for close range 3D modelling. The International Archives of Photogrammetry, Remote Sensing and Spatial Information Sciences 40: 93.
- Jiao J, Yuan L, Tang W, Deng Z, Wu Q (2017) A post-rectification approach of depth images of Kinect v2 for 3D reconstruction of indoor scenes. ISPRS Int. J. Geo-Inf 6: 349.
- Wasenmüller O, Stricker D (2016) Comparison of kinect v1 and v2 depth images in terms of accuracy and precision. In Asian Conference on Computer Vision 34-45.
- Butkiewicz, T (2014). Low-cost coastal mapping using Kinect v2 time-of-flight cameras. Oceans-St. John's 1-9.
- Giancola S, Valenti M., Sala R. (2018) Metrological Qualification of the Kinect V2™ Time-of-Flight Camera. In A Survey on 3D Cameras: Metrological Comparison of Time-of-Flight, Structured-Light and Active Stereoscopy Technologies 41-60.
- Park J, Kim J, Park J, Sheta A, Murphey C et.al., (2019) Development of a sleep monitoring system by using a depth sensor: A pilot study. In International Conference on Applied Human Factors and Ergonomics ,191-196.
- Subramanian S, Hesselbacher S, Aguilar R., Surani S (2011) The NAMES assessment: a novel combined-modality screening tool for obstructive sleep apnea. Sleep Breath 15: 819-826.
- Park J, Sheta A, Surani S (2019) Statistical models for predicting a patient’s respiratory disturbance index. Chest 156: 138.
- Surani S, Sheta A, Turabieh H, Park J, Mathur S (2019) Diagnosis of sleep apnea using artificial neural network and binary particle swarm optimization for feature selection. Chest 156: 136.
- Seale C (1995) Dying alone. Sociology of Health & Illness 17: 376-392.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi