Research Article, Dent Health Curr Res Vol: 9 Issue: 3
Evaluation and Comparision of Molar Incisor Hypomineralisation-Treatment Need: Index and Molar Hypomineralisation Severity Index in Patients with MIH
Alpana Kumari*, Abi M Thomas, Namita Singh, Shaila Masih, Ruchika Kundra and Joe Mathew Cherian
1Department of Pedodontics and Preventive Dentistry, Christian Dental College, CMC, Brown road Ludhiana, Punjab, India
*Corresponding Author: Alpana Kumari,
Department of Pedodontics and Preventive
Dentistry, Ludhiana, Punjab, India
E-mail: alpanakumari01@gmail.com
Received date: 08 June, 2023, Manuscript No. DHCR-23-101823;
Editor assigned date: 12 June, 2023, PreQC No. DHCR-23-101823 (PQ);
Reviewed date: 27 June, 2023, QC No. DHCR-23-101823;
Revised date: 04 July, 2023, Manuscript No. DHCR-23-101823 (R);
Published date: 11 July, 2023 DOI: 10.4172/2470-0886.1000154.
Citation: Kumari A, Thomas AM, Singh N, Masih S, Kundra R, et al. (2023) Evaluation and Comparision of Molar Incisor Hypomineralisation-Treatment Need: Index and Molar Hypomineralisation Severity Index in Patients with MIH. Dent Health Curr Res 9:3.
Abstract
Objective: A wide variation in the prevalence of Molar Incisor Hypomineralisation (MIH) could be due to lack of standardized system for recording it. Hence, the need of the hour is to test the applicability of the MIH-TNI, which is developed by an international MIH working group for epidemiological screening procedure. Till date Molar Incisor Hypomineralisation-Treatment Need Index (MIH-TNI) has not been used in any study. On the other hand, Molar Hypomineralisation Severity Index (MHSI) was developed to address deficiencies in indices concerning hypomineralisation severity. So, the aim of this study was to evaluate and compare MIH-TNI and MHSI.
Methods: 20 patients of age group 6-12 year with MIH were included in the study. Visual inspection of teeth without drying them was done using sterilized instruments. MIH TNI and MHSI was used simultaneously to measure the defect of MIH and the scores was recorded separately in the examination chart.
Results: Data were compared and results were statistically analyzed. According to MHSI, brown colored defect was more common in mandibular molars whereas in maxillary molars it was cream and white colored discoloration. By using MIH-TNI, the extent of defect could also be analyzed. Maxillary molars and maxillary incisors were more commonly involved as compared to mandibular molars and mandibular incisors.
Conclusion: MIH-TNI being a simple-indices to use and reproduce, can play a significant role in maintaining the standardized criteria while recording MIH cases. Early diagnosis and prevention of MIH can thereby lead to prolonging the life of the affected teeth.
Keywords: Molar Incisor Hypomineralisation (MIH); Qualitative defect; Molar Incisor Hypomineralisation-Treatment Need Index (MIH-TNI); Molar Hypomineralisation Severity Index (MHSI)
Introduction
Weerheijm et al. first introduced the term Molar-Incisor Hypomineralisation (MIH) and defined it as “hypomineralisation of systemic origin, presenting as demarcated qualitative defects of enamel of one to four permanent molars frequently associated with affected incisors”. But according to recent studies these defects could affect any primary or permanent teeth.
Clinical presentation of MIH teeth has discrete opaque enamel defects varying from white to yellow or brownish discoloration. The enamel of such teeth can be soft and porous and have the presentation of chalk or old dutch cheese [1-3].
There is a rapid development of dental caries as the hypomineralized enamel gets chipped off easily under the masticatory forces leading to exposure of dentine. Since molars are under the masticatory forces these defects are more severe in the molar region as compared to the incisors. Another reason for the fast progression of caries could be hypersensitivity from air, heat and cold. The child would avoid properly brushing their teeth leading to increased accumulation of plaque.
As per the literature, there is presence of histological difference between the appearance of post eruptive enamel breakdown and hypoplasia.
The localised and asymmetrical pattern of MIH molars suggests it to be of systemic origin and the ameloblasts are probably affected either during early maturation or late secretory stage of amelogenesis. Prenatal, perinatal and post-natal condition of the child also play the utmost role in the etiology of MIH [4]. Though the exact mechanism is still unclear, the literature suggests various causative mechanism such as environmental changes, prolonged breast feeding leading to increased exposure of dioxins, respiratory problems, low birth weight, metabolic disorders associated with calcium-phosphate metabolism, frequent childhood diseases with fever and use of antibiotics [5-8].
There has been association between MIH and hypomineralised second primary molars as quoted in various literatures [9-11]. Schmalfuss et al. in his study concluded that one in every four participants with MIH had at least one canine affected.
Several conditions such as fluorosis, enamel hypoplasia, traumatic hypomineralisation, white spot lesion and amelogenesis imperfecta can be present with hypomineralised defect and thus should be distinguished from MIH.
For managing MIH a six-step management approach has been proposed that is identification of risk factor, early diagnosis, remineralisation and desensitization ,prevention of dental caries and post eruptive enamel breakdown, restorations or extractions and followed by maintenance [12].
Teeth affected with MIH require more dental treatment as compared to those without it. Treatment option for molars are resin infiltration, restoration using Resin-modified Glass Ionomer Cement (RMGIC) or composite, full or partial coverage metal crown. Extraction has to be done for the severely affected first molars after orthodontic consideration and the radiographic evaluation of calcification of bifurcation of second permanent molar.
Treatment for incisors are mainly to achieve better aesthetic result. This involves micro-abrasion, bleaching, resin infiltration and composite restorations or veneers.
The huge variation in prevalence ranging from 2.4% to 40.2% is due to lack of standardised system for recording MIH [13]. Hence, the need of the hour is to test the applicability of Molar Incisor Hypomineralisation-Treatment Need Index (MIH-TNI) which is developed by an international MIH working group for epidemiological screening and monitoring of individuals with MIH by dental practitioners. Till date, MIH-TNI has not been used in any study. On the other hand, Molar Hypomineralisation Severity Index (MHSI) was developed to address deficiencies in indices concerning hypomineralisation severity.
Hence, the aim of this study is to evaluate and compare MIH-TNI and MHSI in patients with molar incisor hypomineralisation.
Methodology
Before conducting the study, ethical clearance was obtained from the Research and Ethics Committee of the college.
Inclusion and exclusion criteria
Inclusion criteria: Children between age group 6-12 years who were affected with Molar incisors hypomineralisation and reported to the Department Of Pedodontia And Preventive Dentistry were included in the study. A total of twenty children were enrolled.
Exclusion criteria:
• Children having enamel defects other than MIH
• If molars and incisors were not fully erupted
• Undergoing any fixed orthodontic therapy
• Medically compromised
Procedure
Before starting the examination written consent was obtained from patient’s parents. Visual inspection of teeth without drying them was done using sterilized mouth mirror and probe.
Both the indices that is MHSI and MIH TNI were used simultaneously and the scores were recorded separately in the examination chart as per the scoring criteria given by Oliver et al, and Steffen.
The author was trained in diagnosing hypomineralized defects using photographs from a previous published study.
Statistical analysis
The data collected was tabulated and Statistical Package for Social Science (SPSS 20, SPSS Inc., Chicago, IL, USA) statistical analysis software was used for statistical analysis. Chi square tests was used to analyze the data.
Results
A total of twenty children affected with MIH were recorded. First, the result was compiled for molar hypomineralisation severity index and then for the molar incisor hypomineralisation-treatment need index.
Molar hypomineralisation severity index
In the present study, Brown colored defects were more in mandibular molars as compared to maxillary molars. Similarly, white and yellow colored discoloration was observed more in maxillary molars than mandibular molars. Cuspal involvement was mainly associated with maxillary molars whereas in case of mandibular molars occlusal surface was involved (Table 1).
| Maxillary | Mandibular | |
|---|---|---|
| Colour of defect | ||
| Brown | 45 | 65 |
| Yellow | 60 | 45 |
| White | 60 | 55 |
| Location of defect | ||
| Cuspal involvement | 70 | 60 |
| Occlusal surface | 50 | 65 |
Table 1: Colour and location of defect.
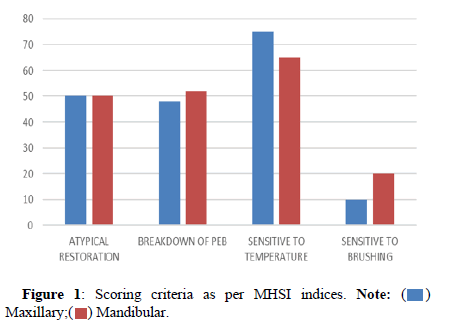
There was no difference between the mandibular and maxillary molars with atypical restorations. There was slight difference between maxillary and mandibular molars in term of post eruptive enamel breakdown. Maxillary molars were more prone in having sensitivity to temperature. It was more common on left side as compared to right side. The difference was statistically insignificant. Mandibular molars had more sensitivity while brushing as compared to maxillary molars (Figure 1).
Molar incisor hypomineralisation-treatment need index
Maxillary molars had more severe defect than mandibular molars. Most common defect present in maxillary molar had 2/3 defect extension or/and presence of defect close to the pulp along with hypersensitivity. Less number of defects were close to pulp or had 2/3 defect extension in case of mandibular molars (Figure 2).
Defects were mainly seen in maxillary incisors than mandibular incisors. Mostly the defects were present without hypersensitivity (Figure 3).
Discussion
Molar Incisor Hypomineralisation (MIH) is a qualitatitive defect of enamel which is distinct from other developmental defects involving enamel. Clinically, affected teeth is present with demarcated enamel opacities of different colour. The soft and porous enamel of such teeth are prone to post eruptive enamel breakdown leading to atypical cavitation or complete distortion of coronal portion [14].
Atleast one first permanent molar should be present with hypomineralisation to be diagnosed as MIH. The defect is more severe if more molars and incisors are affected [15]. The clinical management of MIH is challenging due to the presence of hypersensitivity, rapid development of dental caries in affected teeth, lack of cooperation of a young child, lack of optimum anesthesia and the repeated marginal breakdown of restorations [16].
As there are many different criteria used to define cases of MIH along with lack of standardised tool there is difficulty in comparing the prevalence data reported in different studies [17]. Therefore, in the current study, evaluation of hypomineralisation defects was performed using the Molar Hypomineralisation Severity Index (MHSI) and Molar Incisor Hypomineralisation-Treatment Need Index (MIH-TNI) [18,19].
In the present study, using MHSI index, it was found that brown colour of defect was mostly seen in mandibular molars as compared to the maxillary molars. However, the less severe color defect that is yellow and white was more in maxillary molars than mandibular molars. Occlusal surface involvement as well as post eruptive enamel breakdown was also more common in mandibular molars. Thus, mandibular molars had more severe color defect, occlusal surface involvement and post eruptive enamel breakdown. This result was in accordance with the result of Mittal et al. Bhaskar and hedge and Jasulaityte et al. [20,21].
Maxillary molars were more sensitive to temperature whereas it was mandibular molar which was more sensitive to brushing. This result was in agreement with the study of oliver et al. However, all these results were statistically insignificant.
Second index that was used in the study was MIH-TNI. As per our knowledge and the literature search, this indices has not been used in any study till date. MIH-TNI is based on the model of Community Periodontal Index of Treatment Needs (CPITN).
Using this indices, the extent of defect could also be analysed .The result of the present study revealed that maxillary molars had more chances of being present with hypersensitivity and defect with 2/3 extension and close to the pulp. Similarly, score 2a which is 1/3 defect extension and score 2b which is greater than 1/3 and less than 2/3 defect extension was also seen more in maxillary molars as compared to mandibular molars. Leppaniemi, Ghanim also reported similar results in their study [22,23].
In incisors, there was no defect approaching pulp. The main defect present were with score 2b followed by score 2a. Chances of hypersensitivity was more in posterior teeth as compared to the anterior teeth.
The main advantages of using MIH-TNI is that it is simple to use, can be used both for epidemiological as well as individual assessment, for both primary and permanent dentition, can allow consistent classification of the MIH condition and reproducible finding for each affected patient can be obtained.
Limitation
Major limitation of using MIH-TNI is that training and calibration programme for examiners needs to be developed, validation and verification of applicability in epidemiological studies and individual treatment planning and therapy approach based on MIH TNI needs to be developed. Second limitation was the small sample size so the results obtained cannot be generalized.
Conclusion
Hypomineralisation and the problem associated with it vary from patient to patient. So, it becomes imperative to diagnose patient with molar incisor hypomineralisation during early stages. With early identification, remineralization and preventive measures can be instituted for such teeth as soon as their affected surfaces are accessible.
References
- Weerheijm KL (2003) Molar incisor hypomineralisation (MIH). Eur J Paediatr Dent 4:115-120.
- Weerheijm KL (2004) Molar incisor hypomineralization (MIH): clinical presentation, aetiology and management. Dent Update. 31(1):9-12.
- Almuallem Z, Busuttil-Naudi A (2018) Molar incisor hypomineralisation (MIH)–an overview. Br Dent J. 225(7):601-609.
- Alaluusua S, Lukinmaa PL, Vartiainen T, Partanen M, Torppa J, et al. (1996) Polychlorinated dibenzo-p-dioxins and dibenzofurans via mother's milk may cause developmental defects in the child's teeth. Environ Toxicol Pharmacol. 1(3):193-197.
- Alaluusua S, Lukinmaa PL, Koskimies M, Pirinen S, Hölttä P, et al. (1996) Developmental dental defects associated with long breast feeding. Eur J Pharm Sci 104(5‐6):493-497.
- Beentjes VE, Weerheijm KL, Groen HJ (2002) Factors involved in the aetiology of molar-incisor hypomineralisation (MIH). Eur J Paediatr Dent. 3:9-13.
- Pagaria S, Singh BD, Dubey A, Avinash A (2019) Molar Incisor Hypomineralisation: A Review. Kathmandu. Univ Med J.;20.
- Koch G, Hallonsten AL, Ludvigsson N, Hansson BO, Hoist A, et al. (1987) Epidemiologic study of idiopathic enamel hypomineralization in permanent teeth of Swedish children. Community Dent Oral Epidemiol. 15(5):279-85.
- Elfrink ME, Schuller AA, Weerheijm KL, Veerkamp JS (2008) Hypomineralized second primary molars: prevalence data in Dutch 5-year-olds. Caries Res 42(4):282-5.
- Mittal R, Chandak S, Chandwani M, Singh P, Pimpale J (2016) Assessment of association between molar incisor hypomineralization and hypomineralized second primary molar. Journal of International Society of Preventive & Community Dentistry. 6(1):34.
- Negre-Barber A, Montiel-Company JM, Boronat-Catalá M, Catalá-Pizarro M, Almerich-Silla JM (2016) Hypomineralized second primary molars as predictor of molar incisor hypomineralization. Sci Rep. 25;6(1):31929.
- Willmott NS, Bryan RA, Duggal MS (2008) Molar-incisor-hypomineralisation: a literature review. Eur Arch Paediatr Dent. 9:172-9.
- Silva MJ, Alhowaish L, Ghanim A, Manton DJ (2016) Knowledge and attitudes regarding molar incisor hypomineralisation amongst Saudi Arabian dental practitioners and dental students. Eur Arch Paediatr Dent. 17:215-22.
- Lygidakis NA, Dimou G, Briseniou E (2008) Molar-incisor-hypomineralisation (MIH). Retrospective clinical study in Greek children. I. Prevalence and defect characteristics. Eur Arch Paediatr Dent. 9:200-6.
- Lygidakis NA, Wong F, Jälevik B, Vierrou AM, Alaluusua S, et al. (2010) Best clinical practice guidance for clinicians dealing with children presenting with molar-incisor-hypomineralisation (MIH) an EAPD policy document. Eur Arch Paediatr Dent. 11:75-81.
- William V, Messer LB, Burrow MF (2006) Molar incisor hypomineralization: review and recommendations for clinical management. Pediatr Dent. 28(3):224-32.
- Ghanim A, Silva MJ, Elfrink ME, Lygidakis NA, Mariño RJ, et al. (2017) Molar incisor hypomineralisation (MIH) training manual for clinical field surveys and practice. Eur Arch Paediatr Dent. 18:225-42.
- Oliver K, Messer LB, Manton DJ, Kan K, Ng F, et al. (2014) Distribution and severity of molar hypomineralisation: trial of a new severity index. Int J Paediatr Dent. 24(2):131-51.
- Steffen R, Krämer N, Bekes K (2017) The Würzburg MIH concept: the MIH treatment need index (MIH TNI) a new index to assess and plan treatment in patients with molar incisior hypomineralisation (MIH). Eur Arch Paediatr Dent. 18:355-61.
- Bhaskar SA, Hegde S (2014) Molar-incisor hypomineralization: Prevalence, severity and clinical characteristics in 8-to 13-year-old children of Udaipur, India. Journal of J Indian Soc Pedod Prev Dent. 32(4):322-9.
- Jasulaityte L, Veerkamp JS, Weerheijm KL (2007) Molar incisor hypomineralization: review and prevalence data from a study of primary school children in Kaunas (Lithuania). Eur Arch Paediatr Dent. 8:87-94.
- Leppaniemi A, Lukinmaa PL, Alaluusua S (2001) Nonfluoride hypomineralizations in the permanent first molars and their impact on the treatment need. Caries Res. 35(1):36-40.
- Ghanim A, Morgan M, Marino R, Bailey D, Manton D (2011) Molar‐incisor hypomineralisation: prevalence and defect characteristics in Iraqi children. Int J Paediatr Dent. 21(6):413-21.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 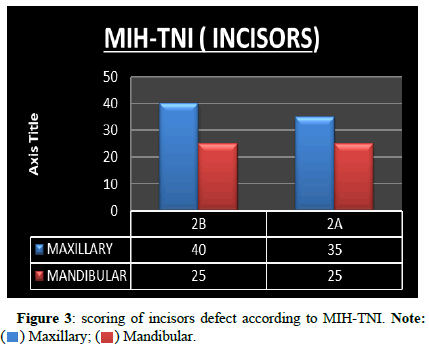
 )
Maxillary;(
)
Maxillary;( ) Mandibular.
) Mandibular.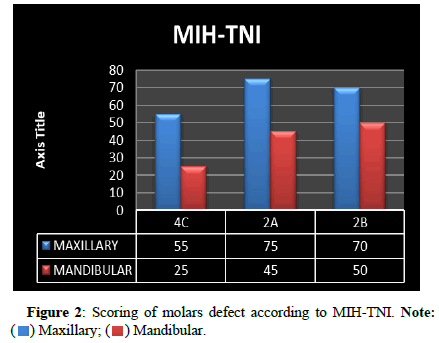
 ) Maxillary; (
) Maxillary; (