Research Article, J Clin Nutr Metab Vol: 1 Issue: 2
Nutritional Risk and Risk of Mucositis in Patients Treated with HDT Prior to Stem Cell Transplantation
Lotte Drustrup1 and Mette Holst2*
1Department of Gastroenterology, Aalborg University Hospital, Demark
2Department of Clinical Medicine, Aalborg University, Denmark
*Corresponding Author : Mette Holst
Centre for Nutrition and Bowel Disease, Department of Medical Gastroenterology, Aalborg Hospital, Aarhus University Hospital, Moelleparkvej 4, Reception 3, 9000 Aalborg, Denmark
Tel: +45 27113236
Fax: +45 99326107
E-mail: mette.holst@rn.dk
Received: September 26, 2017 Accepted: October 20, 2017 Published: October 27, 2017
Citation: Drustrup L, Holst M (2017) Nutritional Risk and Risk of Mucositis in Patients Treated with HDT Prior to Stem Cell Transplantation. J Clin Nutr Metab 1:2.
Abstract
Mucositis is one of the most significant side effects reported in patients receiving high-dose chemotherapy (HDT), either BEAM (a combination therapy) or Melphalal prior to stem cell transplantation due to hematology disease. Mucositis induces pain, diarrhea and reduced food intake in different degrees. This study investigated incidence of mucositis, nutritional risk by NRS (2002 screening), and artificial nutritional therapy in HDT patients. Methods: A retrospective observational cohort included all adult patients treated with HDT prior to stem cell transplantation due to lymphoma or multiple myeloma at Aalborg University Hospital during 20 months. Data was extracted from patient records, and followed patients during the 21-day treatment. Results: A high incidence of mucositis was seen (66%), with highest occurrence in the BEAM population (43%) (p=0.02). The prevalence of nutritional risk increased in both groups from overall 48% before treatment, to overall 92% during treatment (p=0.47), and 41% were treated with EN or PN. An elevation of sodium (p<0.001) as well as potassium (K) (p=0.02) at any given level, and not just above the normal before upstart of treatment, increased the duration of mucositis. Furthermore elevation of sodium (Na) (p=0.03) at any given level, decrease the time to mucositis. Conclusion: Mucositis and nutritional risk is common in HDT, with high prevalence of the need for Enteral and Parenteral Nutrition. Attention should be given to prevention of mucositis and timing of nutritional therapy, as well as studies looking into the importance of focusing on the levels of K and Na prior to HDT treatment.
Keywords: Mucositis; High-dose chemotherapy; Risk factors; Nutritional risk; Under nutrition; Hospitalized patients
Introduction
High-dose-chemotherapy (HDT) is the treatment prior to stemcell transplantation in patients suffering from some Hematological diseases. Several complications, including mucositis, have been reported. Mucositis is one of the most serious and common complications in patients undergoing cancer therapy and occurs in as much as 80% of patients receiving HDT prior to hematopoietic stem cell transplant [1-3]. Mucositis is a breakdown of the mucosa lining the gastrointestinal tract, especially the oral and oropharyngeal mucosa, resulting in erythema, ulcerations, necrosis and bleeding. In addition the breakdown of the mucosa results in a simple access through the barrier and entails an increased risk of bacteria passing into the systemic circulation [4-7].
The pathophysiology of mucositis is believed to be a complex process, however not yet fully understood. Currently, mucositis is seen as a five-phase process consisting of initiation, primary damage response, signal amplification, ulceration, and healing [4-7].
The initiation stage occurs almost immediately after the introduction of cancer treatment, leading to both epithelial and submucosal damage, including DNA and tissue damage. In addition, reactive oxygen species are generated resulting in oxidative stress. At this point, the mucosa seems normal, but underlying downstream biological events have been initiated. Following the initiating stage, primary damage response develops initiating a complex cascade of intracellular events including activation of a number of transcription factors. One of the most significant transcription factors is nuclear factor-kappa B (NF-κB). When activated, NF-κB is capable of inducing an expression of up to 200 genes, and production of proinflammatory cytokines. The result of NF-κB activation, in normal cells, is apoptosis. Simultaneous, several other contributing pathways are activated [4-7].
The third stage results in an amplification of the signal due to the ability of both positive and negative feedback, by the molecules already induced in the first and second stage, thus leading to an expansion of downstream processes [4-7]. As a result of the downstream biological processes, destruction of the cells and tissue occur, leading to deep mucosal ulceration affecting the full epithelial thickness. When developed, the ulcerations may be colonized by bacteria which can induce additional tissue damage. Thus, this stage is characterized by being the most symptomatic and results in most clinical complications such as infections, need of opioid analgesics and malnutrition, due to reduced food intake and diarrhea.
Mucositis induces pain, diarrhea, dehydration, malnutrition, and may thus in severe form result in treatment breaks or therapy dose reduction and thereby compromising survival of the patients [1-7].
The aim of this study was to investigate the incidence of mucositis, time to appearance, duration, association and statistical correlation to selected possible risk factors and risk of under nutrition for mucositis during the cause of disease and HDT therapy.
Methods
A 2 year observational cohort study was conducted. All adult patients receiving high-dose chemotherapy, either BEAM (a combination therapy consisting of BiCNU ® – carmustine, Etoposide, Ara-C – cytarabine and Melphalan), or. + Melphalan prior to stem cell transplantation due to lymphoma or myelomatosis at department of hematology between December 2014 and august 2016 at Aalborg University Hospital were included. Data were obtained by retrospectively reviewing medical records. Exclusions: Patients, who underwent HDT twice in one year, were only included the first time. Patients who had undergone HDT earlier were included in the study.
Data extracted from medical records were: Gender, age, height, weight, nutritional risk by NRS- 2002, weight loss, HDT start day, transplantation day, comorbidity, smoking habits, treatment type, diagnosis, C - reactive protein, albumin, sodium, potassium and calcium, artificial nutrition as enteral nutrition (EN) or parenteral nutrition (PN). Degree of mucositis was evaluated by pain severity and pain treatment given. For every day in the 21 days follow up period the following registrations were included: If the patient suffered from mucositis, nutritional risk by NRS-2002(10), need of artificial nutrition as either enteral nutrition (EN) or parenteral nutrition (PN), infection estimated on signs, symptoms, and positive microbiology culture, and pain severity classified as: No pain, mild pain, or severe pain based on the amount of analgesics [8]. Pain was classified as “mild” if treated with Caphosol, Benzydanine mouthwash, Lidokain viscose, or Paracetamol. Pain was classified as “severe” if eased by means of Morphine-containing analgesics.
All patients were informed of importance of oral hygiene, keeping the mouth hydrated, and brushing teeth four times a day. Supplementary all patients were trained in the use of Caphosol mouthwash 4 times a day by department staff and all patients received Palifermin day 4, 3, and 2 before chemotherapy start, at the transplantation day and the following two days [8-12].
All myelomatosis patients were instructed in cryopreservation of the oral cavity, by sucking ice cubes, under Melphalan and stem cell induction [11-15].
Statistics
Comparison was made using the independent student’s t-tests, Mann-Whitney or â–¡2-tests. Environmental risk factors were analyzed using the Cox proportional hazards.
All statistical analyses were performed using IBM® SPSS® Statistics (version 24.0.0.0, 2016, USA) or StataSE® 14. Baseline characteristics were analyzed with the use of descriptive statistics and expressed as mean ± standard deviation (SD) unless otherwise stated. Independent student’s t-test was used to compare continuous baseline variables in the myelomatosis and lymphoma cohort, whereas an X2 test was used for categorical variables. A univariate Cox proportional hazards model was used to determine whether environmental risk factors and blood samples including BMI, smoking habits, comorbidity, CRP, albumin, calcium, potassium and sodium influenced the risk of mucositis, always corrected by sex, age and treatment type.
A two-tailed p value<0.05 was considered statistically significant.
Results
In total, 66 HDT patients were included in the study, of which 23 patients were treated with BEAM and 43 patients were treated with Melphalan. Only 2 patients were excluded due to exclusion criteria. A mucositis incidence of 73% was observed. The mean age in all HDT patients was 59.11 ± 10.91 but mean of the Melphalan cohort was 6.64 years younger compared to the BEAM cohort. In both cohorts the majority were men. Of all HDT patients, 20% had undergone HDT before, all of which pertained the Melphalan cohort. Baseline characteristics are shown in Table 1. In general, baseline demographic showed some differences between the two cohorts (Table 2). The odds of mucositis was 5.63 times greater in the BEAM cohort compared to the Melphalan cohort (p=0.03). Nutritional risk was found in 92% throughout the 21 follow up period (p=0.024) and increased during treatment in both groups (p=0.47), (Table 3). Artificial nutritional therapy was prescribed as EN or PN in 41% of the patients. Weight loss was found in 66% of the patients, with a mean weight loss of 0.6 kg. No difference with regard to weight loss was found between patients suffering from mucositis compared to patients who avoided mucositis (p=0.06).
| All HDT population | BEAM cohort | Melphalan cohort | P-value comparison between groups |
|
|---|---|---|---|---|
| Number of patients (n) | 66 | 23 | 43 | |
| Mean age of the patient, at the time of treatment ± SD (Range) | 59.11 ± 10.91 (22-71) | 54.78 ± 13.21 (22-71) | 61.42 ± 8.79 (37-71) | 0.07a |
| Gender(n) - Male - Female |
43(65%) 23(35%) |
13(57%) 10(43%) |
30(70%) 13(30%) |
0.28b |
| Cause of HDCT(n) - Myelomytosis - Lymphoma |
43(65%) 23(35%) |
Lymphoma | Myelomatosis | |
| HDCT before(n) - Yes |
13(20%) | 0(0%) | 13(30%) | |
| Comorbidity(n) - Yes |
29(44%) | 12(52%) | 17(40%) | 0.32b |
| Mean habitual weight (Kg) (SD) | 79.45 ± 16.83 SD (43.4-118) |
83.24 ± 14.05 SD (59.9-107) |
77.42 ± 17.96 SD (43.4-118) |
0.18b |
| Mean BMI (Range) | 26.22 ± 4.08 SD (17.4-37) |
26.83 ± 3.6 SD (20.9-37) |
25.90 ± 4.32 (17.4-35.8) |
0.38b |
Table 1: Baseline characteristics.
| All HDT population | BEAM cohort | Melphalan cohort | |
|---|---|---|---|
| N= (%Female) | 66 (35) | 23(43) | 43(30) |
| Mucositis N (%) | 48(73) | 21(91) | 27(63) |
| NRS-2002 risk prior to treatment N (%) | 32(48) | 9(39) |
23(47) |
| NRS-2002 risk during treatment N (%) | 61(92) | 22(96%) | 39(91%) |
Table 2: The incidence of mucositis and nutritional risk.
| Duration of mucositis | Time to start of mucositis | |||||
|---|---|---|---|---|---|---|
| N | HR | P-value | N | HR | P-value | |
| Smoking Habits | 66 | 0.50 | 0.13 | 66 | 1.35 | 0.51 |
| Body Mass Index | 66 | 0.97 | 0.44 | 66 | 1.03 | 0.53 |
| Comorbidity | 66 | 0.62 | 0.19 | 66 | 1.24 | 0.51 |
| CRP | 64 | 1.00 | 0.99 | 64 | 1.00 | 0.73 |
| Albumin | 64 | 0.92 | 0.23 | 64 | 0.99 | 0.84 |
| Potassium | 65 | 4.98 | 0.02* | 65 | 0.37 | 0.09 |
| Sodium | 65 | 1.24 | 0.00* | 65 | 0.84 | 0.03* |
| Calcium | 64 | 0.85 | 0.84 | 64 | 1.38 | 0.67 |
Table 3: Environmental Risk Factors and blood samples prior to treatment influencing time to mucositis and mucositis duration.
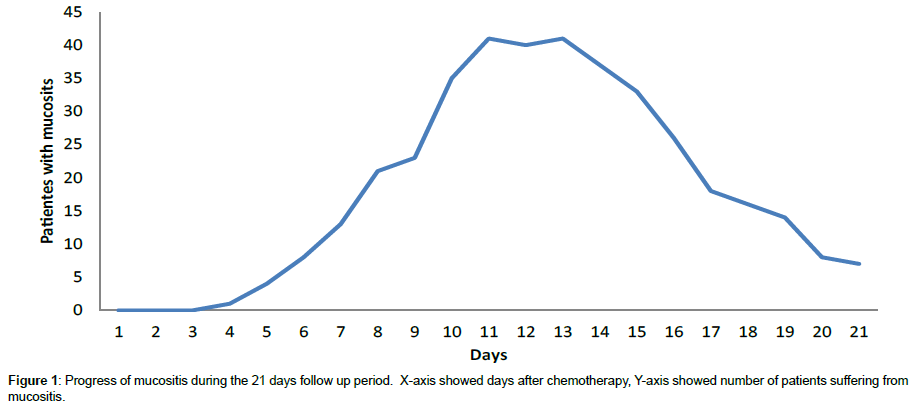
Most patients suffered from mucostis at 11th and 13th day (Figure 1). The median duration of mucositis was 5 days. The median day of mucositis start was 10 days after HDT treatment start. Of patients, who developed mucositis 60%, experienced severe pain? In the BEAM cohort and Melphalan cohort, respectively 66.7% and 55.6% experienced severe pain due to mucositis. In patients who developed mucositis, 100% suffered from mild pain. The pain progress during the 21 days follow up period showed that most patients suffered from severe pain at day 12 after HDT (Figure 1).
The odds of mucositis in the entire group of HDT patients was found to be 2.67, indicating that mucositis was 2.67 more likely to happen than not in all HDT patients. Divided into groups, the risk of mucositis was 10.5 and 1.69 in the BEAM cohort and Melphalan cohort respectively. The odds ratio of mucositis between the BEAM and Melphalan cohort was 5.63, indicating that the odds of getting mucositis was 5.63 times greater in the BEAM cohort compared to the Melphal ancohort (p=0.03). Of the patients suffering from mucositis, 60 % experienced severe pain (Figure 2).
Risk Factors
An elevation of sodium (p<0.001) as well as potassium (K) (p=0.02) above any prior range before upstart of treatment, increased the duration of mucositis and an elevation of sodium (Na) (p=0.03) above the prior range, decreased the time to appearance of mucositis.
Infection was seen in 39%of the patients, but no difference was found between patients suffering from mucositis compared to patients who avoided mucositis (p=0.08).
No environmental risk factors influenced neither the time to mucositis nor the mucositis duration. An elevation of both sodium and potassium increased the duration of mucositis and an elevation in sodium also decreased time to mucositis.
Discussion
In the present study a persistent high incidence of HDT inducedmucositis was observed despite of current mucositis prophylaxis. As much as 73% of all HDT patients developed mucositis with a median duration of 5.5 days and up to 60% experienced pain only eased by morphine-containing analgesics. The duration of mucositis and the time to mucositis, were influenced by the potassium and sodium level in serum prior to HDT.
When evaluating baseline characteristics it was found that the majority of the patients were men appropriate to the relatively high mean weight. The mean age of 59.11 years was relatively high when compared to other studies of chemotherapy induced mucositis. This may be explained by the differences in the study population regarding included patients, in which the majority of the patients in the present study suffered from myelomatosis, which differed from the other studies [2,3].
Despite current prophylaxis, HTD induced mucositis was a relatively big problem with an incidence of 73%, which was almost equal to the incidence reported by Vera-Llonch, but somewhat higher than reported in other studies [2,3,9]. Most incidences of mucositis developed during the second week after HDT, which corresponded to mucositis pathophysiology [4-7,9]. Concerning mucositis duration, the present study found a median duration of 5.5 days which was short compared to some studies [3]. The longer duration of mucositis in the BEAM cohort compared to the Melphalan cohort, may be explained by the differences in treatment intensity and in addition by the differences in prophylaxis between the two cohorts. The melphalan cohort was, in addition to oral hygiene, Caphosol mouthwash, and Palifermin, receiving cryopreservation of the oral cavity as prophylaxis, which was recommended by MASCC/ISOOguidelines as mucositis prophylaxis [14,15]. Cryopreservation was not recommended for patients in the BEAM cohort due to their lymphoma diagnosis, in which cryopreservation may protect potential tumor cells. Regarding pain caused by mucositis, 60% of patients who developed mucositis suffered from severe pain and most patients experienced severe pain 12 days following HDT. This result combined with the fact that the present study found that most patents suffered from mucositis at day 11 or 13 and the median start day of mucositis was 10 days after HDT, showed that the second week after HDT, was the period where most patients suffered from this severer complication to HDT. This period was also the period where an elevation of EN- and PN-therapy was seen. Thus, determining the fact that an increase in mucositis and the concomitant pain may result in discomfort when eating. When evaluating the severity of pain in the present study, it should be considered that determining pain severity by the selected analgesics may have some inaccuracies, since not all patients have the same pain tolerance or the same opinions regarding the consumption of analgesics. This is comparable to those in other retrospective studies evaluating mucositis, where a mucositis score was not amended during treatment [7]. Thus, no other method could eliminate this bias, but if a daily mucositis score was obtained a correlation between the mucositis score and pain severity could be made.
Weight loss was observed in 66% of the patients, with a mean weight loss of 0.6 kg, however no difference was found between patients suffering from mucositis compared to patients who avoided mucositis when evaluating whether the patients had a weight loss or not (p=0.06). The weight loss was smaller than expected when looking at severity of discomfort and eating problems. Many possible explanations for this could be applicable and the fact that the patients are often overhydrated or infected, which may increase weight. Another reason may be the extra focus on patients’ nutrition intake, and that the staff interceded when a problem was observed. This argument was supported by the result showing that 92% of the patients developed nutritional risk (NRS 2002) [10] during the 21 day follow up period and 41% received either EN or PN, thus taking action on the patients’ needs. Infection during the 21 day follow up period was seen in 39% of the patients. No difference was found between patients suffering from mucositis compared to patients who avoided mucositis when evaluating whether the patients were infected or not (p=0.08). This result was different than the expected due to that the impaired mucosa barira in mucositis patients simplify the passing for bacteria into the systemic circulation [1-7]. It has to be considered that all patients, due to the HDT, were in a high risk of infection, as HDT induces neutropenia. Also all patients received infection prophylaxis, which may mask the reality. The investigated risk factors were BMI, comorbidity and smoking habits. The reason why comorbidity had no influence may be explained by the fact that the HDT population is a selected population, where only the patients considered capable of completing the treatment without high risk are offered treatment due to guidelines. Regarding smoking habits only 13 patients were smokers which were a rather small part of the whole population, why the possible influence may be too small to be detected. Regarding BMI no influence was found in spite of the wide range. Regarding the influence of blood samples prior to HDT CRP, albumin potassium, sodium and calcium was selected as investigation parameters for the patients’ general condition. It was chosen not to investigate hematological blood samples as neutrophil granulocytes, hemoglobin, platelets and leucocytes, due to the fact that the patient’s disease would influence these parameters. The results showed that potassium and sodium both influenced mucositis duration. When the potassium level increases the mucositis duration increased almost by a factor 5 and regarding sodium, when sodium elevates the mucositis duration was prolonged by a factor 1.24. Sodium was the only significant factor influencing the time to mucositis by reducing the time to mucositis by a factor 1.2 when serum sodium increases. These results should be taken into account regarding mucositis and may predict which patients would be at high risk of an early and long lasting mucositis and permit early action, such as implementing EN before mucositis develops.
Conclusion
Despite of current mucositis prophylaxis a high incidence of HDT induced mucositis was observed. Almost all patients became at nutritional risk and as much as 41% needed either EN or PN. Only the sodium and potassium level in serum prior to HDT influenced the duration and time to mucositis, which indicated that these parameters may be considered before starting HDT.
No environmental risk factors influenced the duration of mucositis. Results showed that when the serum level of sodium and potassium were elevated before initiating treatment, mucositis started earlier, and the duration of mucositis was prolonged.
References
- Rzepecki P, Barzal J, Oborska S (2010) Blood and marrow transplantation and nutritional support. Support Care Cancer 2: 57-65.
- Vera-Llonch M, Oster G, Ford CM, Lu J, Sonis S (2007) Oral mucositis and outcomes of allogeneic hematopoietic stem-cell transplantation in patients with hematologic malignancies. Support Care Cancer 15: 491-496.
- Cutler C, Li S, Kim HT, Laglenne P, Szeto KC, Hoffmeister L, et al. (2005) Mucositis after Allogeneic Hematopoietic Stem Cell Transplantation: A Cohort Study of Methotrexate and Non–Methotrexate-Containing Graft-versus-Host Disease Prophylaxis Regimens. Biol Blood Marrow Transplant 11: 383-388.
- Al-Dasooqi N, Sonis ST, Bowen JM, Bateman E, Blijlevens N, et al. (2013) Emerging evidence on the pathobiology of mucositis. Support Care Cancer 21: 3233-3241.
- Sonis ST (2009) Mucositis: The impact, biology and therapeutic opportunities of oral mucositis. Oral Oncol 45: 1015-1020.
- Sonis ST (2004) Pathobiology of mucositis. Nat Rev Cancer 20: 277-284.
- Sonis ST, Elting LS, Keefe D, Peterson DE, Schubert M, et al. (2004) Perspectives on cancer therapy-induced mucosal injury: pathogenesis, measurement, epidemiology, and consequences for patients. Cancer 100: 1995-2025.
- Kramer IR, Pindborg JJ, Bezroukov V, Infirri JS (1980) Guide to epidemiology and diagnosis of oral mucosal diseases and conditions. World Health Organization. Community Dent Oral Epidemiol 8: 1-26.
- Chaudhry HM, Bruce AJ, Wolf RC, Litzow MR, Hogan WJ, et al. (2016) The Incidence and Severity of Oral Mucositis among Allogeneic Hematopoietic Stem Cell Transplantation Patients: A Systematic Review. Biol Blood Marrow Transplant 22: 605-616.
- Kondrup J, Rasmussen HH, Hamberg O, Stanga Z (2003) Nutritional risk screening (NRS 2002): a new method based on an analysis of controlled clinical trials. Clin Nutr 22: 321-336.
- Sebille YZ Van, Stansborough R, Wardill HR, Bateman E, Gibson RJ, et al. (2015) Management of Mucositis During Chemotherapy: From Pathophysiology to Pragmatic Therapeutics. Curr Oncol Rep 17: 50-59.
- Clarkson JE, Worthington HV, Furness S, McCabe M, Khalid T, et al. (2010) Interventions for treating oral mucositis for patients with cancer receiving treatment. Cochrane Database Syst Rev 4: CD001973.
- Chaveli-López B, Bagán-Sebastián J V (2016) Treatment of oral mucositis due to chemotherapy. J Clin Exp Dent 8: e201-209.
- Lalla R V, Bowen J, Barasch A, Elting L, Epstein J, Keefe DM, et al. (2014) MASCC/ISOO clinical practice guidelines for the management of mucositis secondary to cancer therapy. Cancer 120: 1453-1461.
- Lalla RV (2014) Alleviating mucositis: Are we on track for a novel therapeutic? Expert Rev Gastroenterol Hepatol 9: 127-128.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi