Research Article, J Clin Nutr Metab Vol: 2 Issue: 1
Quality of Life in HPN Patients Measured By EQ5D-3L Including VAS
Holst M*, Ryttergaard L, Frandsen L S, Vinter-Jensen L and Rasmussen HH
Centre for Nutrition and Bowel Disease, Department of Gastroenterology, Aalborg University Hospital, Aalborg, Denmark
*Corresponding Author : Mette Holst
Centre for Nutrition and Bowel Disease, Department of Medical Gastroenterology, Aalborg Hospital, Aarhus University Hospital, Moelleparkvej 4, Reception 3, 9000 Aalborg, Denmark
Tel: +45 27113236
Fax: +45 99326107
E-mail: mette.holst@rn.dk
Received: December 14, 2017 Accepted: January 02, 2018 Published: January 09, 2018
Citation: Holst M, Ryttergaard L, Frandsen L S, Vinter-Jensen L, Rasmussen HH (2018) Quality of Life in HPN Patients Measured By EQ5D-3L including VAS. J Clin Nutr Metab 2:1.
Abstract
Rationale: According to literature, HPN (home parenteral nutrition) patients experience reduced quality of life (QOL). QOL questionnaires are however often long and may not seem relevant for the population in question. As a basis for this study, 10 HPN patients were asked to choose the QOL questionnaire, which seemed most relevant to them out of three. Thus, this study aimed to explore quality of life and the internal validity for measuring quality of life by EQ5D-3L including VAS in a Danish population of HPN patients.
Methods: All patients receiving HPN for >one year (N=88) at Center for Nutrition and Bowel Disease, Aalborg University Hospital, were included in the investigation of quality of life using EQ-5D-3L including the EQ VAS (visual analogue scale), which was sent to patients by mail, with a reply envelope.
Results: A total of 50 (57%) patients mean age 63(SD 12.4) responded. Of these, 68% were female. The majority were cohabiting 31 (62%), 40% had a medium high education, and 53% were retired. Home care nurse was involved in 26 (53%) for care around HPN. For the EQ5D dimensions, most patients indicated “no problems” to mobility, personal care and anxiety/depression, while for usual activities 30% and pain/discomfort, 36% reported “difficulties”. The mean value of EQ-5D index score (0.694) was higher than the mean VAS score (0.587) (p<0.001), and highest in women besides the age group 78-80 years. Overall EQ5D VAS score for QOL was 58.73. A numerically lower VAS score was found in Female (56.44) than male (63.59). Lowest VAS-QOL was found in patients aged 30-50 years.
Conclusions: An overall decreased QOL was seen in HPN patients especially in age below 50, and in dimensions of usual activities and pain/discomfort. A significant difference was seen between the EQ5D-3L QOL- index score and VAS. Patients found the method feasible and relevant for them.
Keywords: Nutrition; Personal care; Depression; Age
Introduction
Home parenteral nutrition (HPN) is an increasing life-sustaining therapy in intestinal failure, which is defined as the reduction of gut function below the minimum necessary for the absorption of macronutrients and/or water and electrolytes, such that intravenous supplementation is required to maintain health and/or growth [1]. Type III intestinal failure is a chronic condition, in metabolically stable patients, requiring intravenous supplementation over months to years or even life long, when it is based on a benign condition, such as Crohns disease, chronic intestinal pseudo-obstruction, or systemic sclerosis [1].
According to literature, HPN is associated with decreased physical health due to recurrent events from underlying disease, catheter related complications, parenteral nutrition-associated liver disease, and metabolic bone disease [2-10]. Pain, fatigue, gastrointestinal discomfort and dehydration are physiological factors that together with increased occurrence of depression and social isolation contribute to a lower Quality of life (QOL) in HPNdependent patients [10-12].
Measuring quality of life provides the possibility to assess changes in quality of life, and to see quality of life as a target or an outcome parameter to measure the effect of an intervention. The measuring instruments are used to assess changes in the patient’s health status and are divided into disease-specific and generic. Diseasespecific instruments are developed to assess aspects of quality of life specifically, to a particular disease. There is therefore most often a greater sensitivity in relation to changes due to treatment. The generic instruments are universal and capture the most general aspects of quality of life that are considered relevant to both sick and healthy. Therefore, they can be used in all patient groups, enabling a broader comparison across diseases, age and treatments [4,7,13-15]. The choice of instrument in clinical practice is however not only dependent on sensitivity and specificity, as suggested in a vast amount of studies which have developed and compared QOL instruments in selected populations [7,13-16]. A recent review looked the implications of home parenteral nutrition (HPN) on quality of life, as experienced by patients [6], and a qualitative study on what is actually important to the patient [17]. This study among other things found that it was of great importance to be seen as a person and not primarily as a patient suffering from a disease. A consideration using QOL measurements as an outcome parameter in clinical practice, is that the majority of QOL instruments include many questions [7,13,14,16]. In our practice with Type III intestinal failure patients, we find incentive to evaluate quality of life in all our patients, including also those who are older and may have difficulties in filling out a long questionnaire. In order to find an instrument which was found relevant by our patients and easy to use, we presented three different questionnaires, one disease specific and two generic to the first 10 HPN patients suffering from benign underlying diseases, who came to our outpatient clinic. This pilot investigation showed full consensus as nine out of ten preferred EQ-5D-3L, due to being most relevant and understandable, and less exhausting for patients to use.
Subjects and Methods
Aims
The study aimed to explore QOL by EQ5D, and the internal validity for measuring quality of life by EQ5D-3L including VAS in our population of out-patients receiving HPN.
Subjects and methods
All patients who received (N=88) at Center for Nutrition and Bowel Disease, Aalborg University Hospital, Denmark, were included in the investigation.
Inclusion criteria: HPN for more than one year, and able to read Danish. Age > 18 years.
Exclusion criteria: Current malignant disease.
An invitation letter was sent to patients at home by mail. The letter included a questionnaire with nine questions regarding demographic information, the EQ5D-3L questionnaire and VAS scale and a reply envelope. The invitation letter informed patients to fill in the questionnaires and send the closed envelope, back, either by mail, or with the weekly HPN-delivery. Patients were informed to not write their name on the form or envelope, in order to keep the investigation anonymous.
Material: EQ-5D is a standardized measure of health status developed by the EuroQol Group in order to provide a simple, generic measure of health for clinical and economic appraisal. The EQ- 5D consists of a simple and short questionnaire, and a VAS scale, which patients are asked to fill in themselves. With EQ5D-3L patients are asked to reply to the 5 questions on a three point scale, regarding mobility, self-care, usual activities, pain-discomfort and anxiety/depression. To help people say how good or bad they feel their health state in general is, they are asked to drawn a line on a VAS scale.
Ethical considerations
In the invitation letter, patients were given information about the study. The study was conducted according to the Helsinki Declaration of 2002. The study was put forward to the local ethic committee, which had no objections.
Results
Demographic information
A total of 50 (57%) patients, mean age 63(SD 12.4) responded to the questionnaire. Of these, 68% were female. The majority 31 (62%) were cohabitant, 40% had a medium high education, and 53% were retired due to health impact or age. Home care nurse was involved in 26 (53%) for care around HPN. Table 1 shows further demographic information regarding the included population.
| Study population | |
|---|---|
| Sex | N (%) |
| Female | 34 (68,0) |
| Male | 16 (32,0) |
| Age, Mean years (SD) = 63 (12,4) | |
| 30-50 | 5 (10,0) |
| 51-60 | 15 (30,0) |
| 61-70 | 16 (32,0) |
| 71-80 | 11 (22,0) |
| 80 | 3 (6,0) |
| Civil state | |
| Living alone | 19 (38,0) |
| Cohabitant | 31 (62,0) |
| Education, missing=2 | |
| Basic school | 6 (12,5) |
| Training | 1 (2,1) |
| Short higher education | 11 (22,9) |
| Bachelor degree/ medium higher education | 19 (39,6) |
| Master degree/ higher education | 4 (8,3) |
| No education | 7 (14,6) |
| Employment, missing=14 | |
| Full time employment | 2 (5,6) |
| Part time employment | 4 (11,1) |
| Early retirement due to health | 10 (27,8) |
| Pension | 19 (52,8) |
| Sick leave | 1 (2,8) |
| Home care nurse for HPN care, missing=1 | |
| Yes | 23 (46,9) |
| No | 26 (53,1) |
| Relatives help with HPN care, missing=2 | |
| Self managing | 21 (43,8) |
| Help from relatives | 27 (56,3) |
| Transportation | |
| Drives a car | 32 (64,0) |
| Help for transportation needed | 18 (36,0) |
| Time with HPN | |
| Less than 2 years | 29 (58,0) |
| More than 2 years | 21 (42,0) |
Table 1: Demographic information.
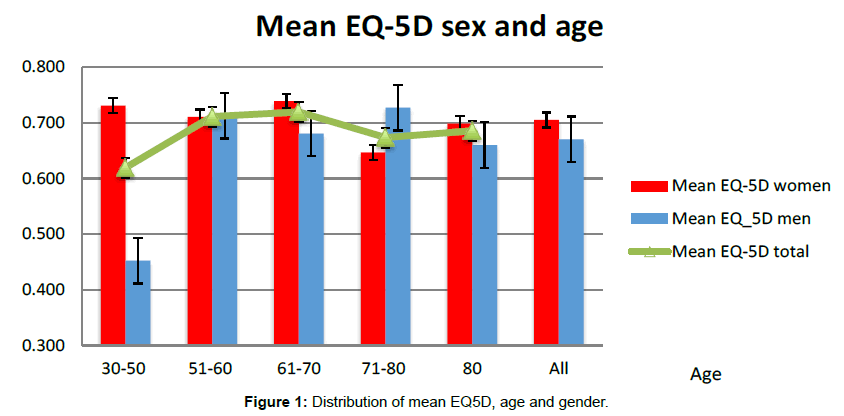
All patients included showed an extent of impaired quality of life. Most impairment in EQ-5D index score was seen in patients <50 years, where women in general reported a higher average EQ-5D index score than men, implicating a better quality of life. Figure 1 shows the distribution of mean EQ5D, age and gender.
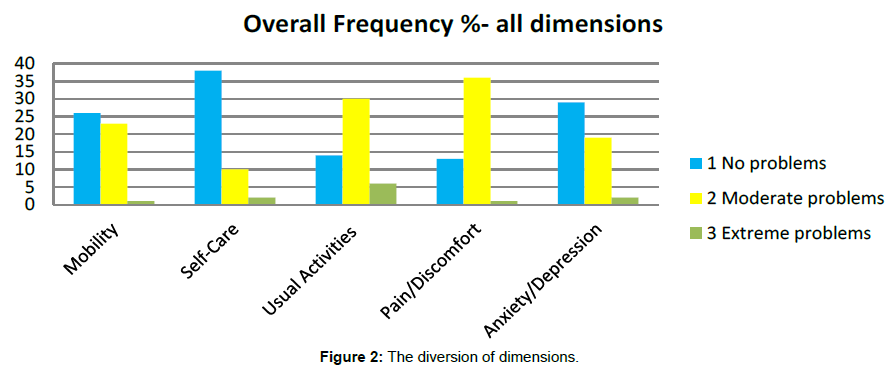
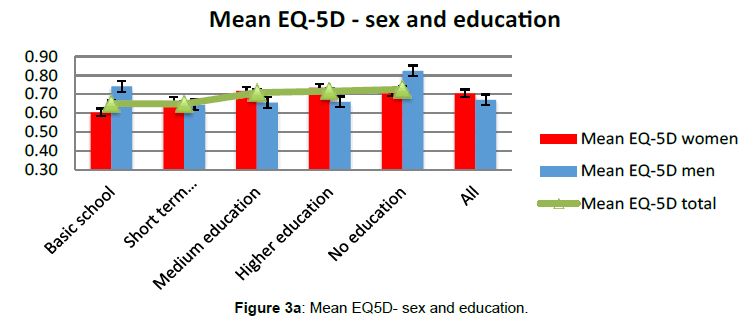
For the EQ5D dimensions, most patients indicated “no problems” to mobility, self-care and anxiety/depression, while for usual activities 30% and pain/discomfort, 36% reported “Moderate problems”. Three patients claimed having extreme problems maintaining “Usual Activities” (Figures 2 and 3a, 3b).
While time experience with HPN +/- 2 years made no difference to quality of life by EQ5D, male patients (N=16) with low or no education seemed to have improved quality of life compared to those with longer education. This tendency was unclear for women.
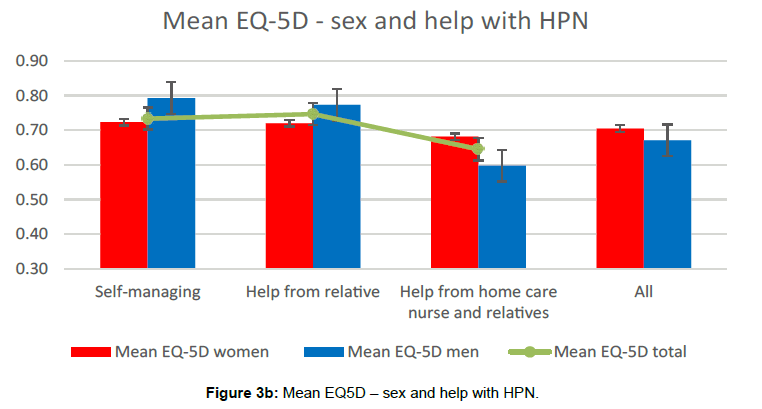
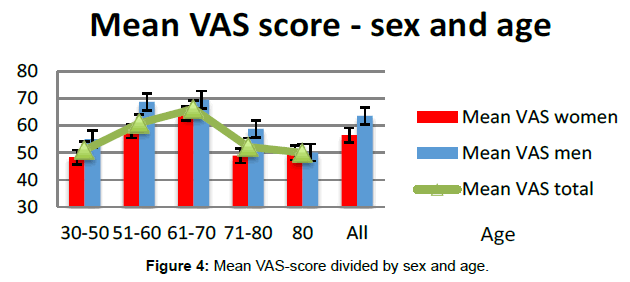
Self-managing ability seemed to contribute to improve to health related quality of life, however only significant in the male population (Figure 4).
The mean value of EQ-5D index score (0.694) was higher than the mean VAS score (0.587); T=5.172 (p <0.001). Separating gender, the paired T-test showed that the difference was not significant in men p=0.378, while women (n=34) scored significantly lower on the VAS scale, compared to the EQ-5D index score p<0.001. Female VAS: 56.44; Male VAS: 63.59. Lowest VAS-QOL was found in patients aged 30-50 years (Female: 48 and Male: 55).
Discussion
In the questionnaire survey, both an EQ-5D index score and a VAS score were performed by each of the 50 participating HPN patients. The average EQ-5D index score of 0.694 shows a reduction in full health of approximately 30%. EQ-5D measurements are most often used in studies where scores are either compared over time, thus being used as an effect assessment of a given treatment or effort, or compared to a control group. There is therefore no cut-off point for a good health status. Thus, it is not possible to give a clear answer to the whether the results of our patient’s health status should be considered fair, as this baseline study was the basis for a subsequent follow-up in clinical practice, from which it will then be possible to evaluate the impact of individual interventions. A recent review attempted to compare their EQ5D findings in patients with psoriasis to groups of other chronic diseases, and found that the ranges of disutility among psoriasis patients are within the ranges of other chronic diseases. The reported EQ-5D for other diseases ranged from 0.20 (Type 2 diabetes mellitus) to 0.66 and 0.79(liver diseases), up to 0.93 (cancer patients) [18].
In our study 42% of patients have received HPN treatment for more than two years, and therefore allegedly assess their health status and quality of life based on an adaption to their new existence. The above-mentioned study on chronic patients does not describe how long the patients in this study have been chronically ill, so we cannot compare adaption to chronic disease by this review [18]. However, a qualitative study addresses coping to disease with time, as they found that because patients had lived with the disease for many years, they were used to managing and had adjusted to many aspects of life [17]. This might be one of many explanations that our younger patients are doing less good, however this is shown in a very small sample.
Our results also showed a statistically significant (p <0.001) difference in the measurements between EQ-5D and VAS, as patients had a higher health status on EQ-5D (0.694) than on VAS (0.587). As the EQ-5D index score and VAS score are based on different methods of determining utility value, respectively, in the form of TTO (Time Trade Off) and VAS, methodological conditions can justify this difference. Most often, values based on VAS scores are lower than values based on TTO [19]. Conversely, the dimensions of the EQ- 5D may not adequately capture all the conditions that affect quality of life of the patient group. This can be substantiated by the female sub-analysis, where it is seen that they score significantly lower on the VAS score than on the EQ-5D index score. In a study from 1999, using the non-disease specific sickness impact profile (SIP) and the disease specific inflammatory bowel disease questionnaire (IBDQ) the analysis of the physical dimension showed that the female HPN patients had worse SIP scores (higher score) with regard to both functional parameters, compared to male. In the psychosocial dimension no significant difference was seen between sexes with regard to social interaction, but the female patients scored worse on emotion [20].
In the analysis of the EQ-5D index score, it is moreover seen that pain/discomfort and usual activities are the dimensions where most of the patients report problems. In line with existing literature, physical pain and discomfort in the form of headaches and nausea, are factors that significantly affect the quality of life of the patient group [7,21]. In addition, it should be pointed out that the dimensions of the EQ-5D are not weighted, indicating that although the patient indicates the same level of two dimensions, these may well be weighted differently by the patient, which can, for example, result in a difference between the EQ-5D index score and the VAS score of the individual patient.
The difference between the EQ5D-QOL index and the VAS-score as well as between the gender and age may furthermore indicate that the five dimensions do not meet all areas of what is important to HPN patients, for maintaining health related quality of life.
Further follow-up will show how EQ5D-3L works with follow-up on intervention in individual HPN-patients.
Study limitations
The response rate in our study was 57%, which we find fair, compared to other studies. One review found a variation of response rate between 30 and 100% in the 14 of 26 studies where respond rate was given [6]. The great variation in response rate might be explained by the approach to patients. For instance, in a study in an outpatient setting, the questionnaires were undertaken in the presence of a physician or dietitians who were able to help patients if they needed for the 30 questions in SF-30 [16]. In another study, giving a response rate of 61%, patients were contacted by phone to complete the questionnaires, in case of missing response [11]. The limited population of 50 included patients is comparable to many other studies, but yet a smaller sample. We chose to include only stable patients with and experience > one year, and not include patients with current cancer, as our patients with active cancer are already measured for quality of life with disease-specific tools.
Conclusions
• Decreased QOL in HPN patients measured by EQ5D-3L was seen especially in age below 50, and in dimensions of usual activities and pain/discomfort.
• Highest reduction in EQ-5D index score in patients <50 years, however the sample is small.
• Women showed a higher average EQ-5D index score than men (better quality of life).
• When the EQ-5D index score is compared to the VAS score, men had better quality of life than women.
• There was a significant difference between EQ5D-QOL index and VAS.
• EQ5D-3L was feasible and preferred by patients as relevant and understandable, and less exhausting for patients to use.
Acknowledgements
L S Frandsen, L Ryttergaard and M Holst were responsible for the study design data collection and analysis. L Vinter-Jensen and HH Rasmussen supervised the process. Mette Holst drafted the manuscript and wrote the final edition.
References
- Pironi L, Arends J, Baxter J, Bozzetti F, Peláez RB, et al. (2015) ESPEN endorsed recommendations: Definition and classification of intestinal failure in adults. Clin Nutr 34: 171-180.
- Bech LF, Drustrup L, Nygaard L, Skallerup A, Christensen LD, et al. (2016) Environmental Risk Factors for Developing Catheter-Related Bloodstream Infection in Home Parenteral Nutrition Patients. J Parenter Enter Nutr 40: 989-994.
- Christensen LD, Holst M, Bech LF, Drustrup L, Nygaard L, et al. (2016) Comparison of complications associated with peripherally inserted central catheters and HickmanTM catheters in patients with intestinal failure receiving home parenteral nutrition. Six-year follow up study. Clin Nutr 34: S84-85.
- Dreesen M, Foulon V, Vanhaecht K, Hiele M, De Pourcq L, et al. (2013) Development of quality of care interventions for adult patients on home parenteral nutrition (HPN) with a benign underlying disease using a two-round Delphi approach. Clin Nutr 32: 59-64.
- Klek S, Forbes A, Gabe S, Holst M, Wanten G, et al. (2016) Management of acute intestinal failure: A position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 35: 1209-1218.
- Schoonhoven L, Jansen J, Wanten G, van Achterberg T (2007) The impact of home parenteral nutrition on daily life-A review. Clin Nutr 26: 275-288.
- Kalaitzakis E, Carlsson E, Josefsson A, Bosaeus I (2008) Quality of life in short-bowel syndrome: Impact of fatigue and gastrointestinal symptoms. Scand J Gastroenterol 43: 1057-1065.
- Nygaard L, Skallerup A, Olesen SS, Køhler M, Vinter-Jensen L, et al. (2017) Osteoporosis in patients with intestinal insufficiency and intestinal failure: Prevalence and clinical risk factors. doi:10.1177/0148607117704812
- Skallerup A, Nygaard L, Olesen SS, Køhler M, Vinter-Jensen L, et al. (2017) The prevalence of sarcopenia is markedly increased in patients with intestinal failure and associates with several risk factors. doi:10.1016/j.clnu.2017.09.010
- Winkler MF, Smith CE (2014) Clinical, Social, and Economic Impacts of Home Parenteral Nutrition Dependence in Short Bowel Syndrome. J Parenter Enter Nutr 38: 32S-37S.
- Bazelmans E, Van Achterberg T, Jansen J, Sauerwein H, Wanten G, et al. (2011) Predicting fatigue in patients using home parenteral nutrition: A longitudinal study. Int J Behav Med 18: 268-276.
- Mueller M, Lohmann S, Thul P, Weimann A, Grill E (2010) Functioning and health in patients with cancer on home-parenteral nutrition: a qualitative study. Health Qual Life Outcomes 8: 41.
- Berghöfer P, Fragkos KC, Baxter JP, Forbes A, Joly F, et al. (2013) Development and validation of the disease-specific Short Bowel Syndrome-Quality of Life (SBS-QoL???) scale. Clin Nutr 32: 789-796.
- Miller TL (2017) Content Validation of a Home Parenteral Nutrition-Patient-Reported Outcome Questionnaire. Nutr Clin Pract 32: 806-813.
- Theilla M, Kagan I, Chernov K, Cohen J, Kagan I, et al. (2017) Self-Evaluation of Quality of Life Among Patients Receiving Home Parenteral Nutrition: A Validation Study. doi:10.1177/0148607117704812
- Cotogni P, De Carli L, Passera R, Amerio ML, Agnello E, et al. (2017) Longitudinal study of quality of life in advanced cancer patients on home parenteral nutrition. Cancer Med 6: 1799-1806.
- Carlsson E, Persson E (2015) Living with intestinal failure caused by Crohn disease: not letting the disease conquer life. Gastroenterol Nurs 38: 12-20.
- Møller AH, Erntoft S, Vinding GR, Jemec GB (2015) A systematic literature review to compare quality of life in psoriasis with other chronic diseases using EQ-5D-derived utility values. Patient Relat. Outcome Meas 6: 167.
- Happich M, Moock J, Von Lengerke T (2009) Health state valuation methods and reference points: The case of Tinnitus. Value Heal 12: 88-95.
- Jeppesen PB, Langholz E, Mortensen PB (1999) Quality of life in patients receiving home parenteral nutrition 44: 844-852.
- Carlsson E, Persson E (2015) Living with Intestinal Failure Caused by Crohn Disease. Gastroenterol Nurs 38: 12-20.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi