Research Article, J Food Nutr Disor Vol: 8 Issue: 3
Millet Intake and Risk Factors of Type 2 Diabetes: A Systematic Review
Ameerah Almaski1,2*, Shelly COE1, Helen Lightowler1 and Sangeetha Thondre1
1Oxford Brookes Centre for Nutrition and Health (OxBCNH), Department of Sport, Health Sciences and Social Work, Oxford Brookes University, Gipsy Lane, Oxford, OX3 0BP, U.K
2Taibah University, KSA, Medina, Universities Road, 344, Saudi Arabia
*Corresponding Author : Ameerah Almaski, Ph.D. Researcher
Oxford Brookes Centre for Nutrition and Health, Department of Sport, Health Sciences and Social Work, Oxford Brookes University, Oxford, OX3 0BP, U.K.
E-mail: am.almiske@gmail.com
Received: July 30, 2019 Accepted: August 16, 2019 Published: August 16, 2019
Citation: Almaski A, Shelly COE, Lightowler H, Thondre S (2019) Millet Intake and Risk Factors of Type 2 Diabetes: A Systematic Review. J Food Nutr Disor 8:3.
Abstract
Daily consumption of millet-based foods is associated with a reduced risk of type-2 diabetes. The aim of the present study was to systematically review the literature describing intervention studies that have investigated the effects of consuming different types and forms of millet on the risk factors for type-2 diabetes. A literature search was conducted, using five databases, from May 2016 to January 2017, which identified 57 articles. Search terms included ‘millet’ AND healthy, pre-diabetic or type-2 diabetes AND fasting blood glucose or glycaemic or glycemic response or insulin response or glucose tolerance or insulin sensitivity. Nineteen studies met the inclusion criteria. Although glycemic and insulin responses differ depending on the millet type and cooking method used, overall, millet has a beneficial effect on fasting and post-prandial blood glucose and the plasma-insulin response in healthy individuals and those with type-2 diabetes. It can be concluded that millets do have the potential to play a protective role in the management of type-2 diabetes.
Keywords: Glycemic response; Insulin response; Glucose tolerance; Insulin sensitivity
Introduction
Type-2 diabetes is the most common chronic metabolic condition around the world that is associated with long-term complications, such as stroke, cardiovascular disease, kidney failure, retinopathy and neuropathy [1]. The prevalence of diabetes in the UK was 4.05 million in 2016-an astounding 65% increase over the past decade [2]. Preventing acute complications and reducing risk of the disease can be accomplished with medical support and education in patient selfmanagement, as well as promoting beneficial lifestyle modifications, a healthy diet, physical activity and weight loss [3].
Dietary interventions are an easy and cost-effective way to provide health benefits to people at risk and those who have been diagnosed with type-2 diabetes, in addition to improving their quality of life [1]. Current guidelines for those with type-2 diabetes are to follow a healthy, balanced diet-notably including starchy carbohydrates with a low GI (Glycaemic index) and higher dietary fiber, both of which can help regulate post-prandial hyperglycemia and reduce body weight [4]. It has been shown that a low glycaemic carbohydrate/high-fiber diet safely reduces plasma cholesterol levels and improves blood glucose control in people with type-2 diabetes [5].
Millet is an important crop for populations in Africa, Asia and parts of Europe [6]. Nutritionally, millet is superior to other major cereals, such as wheat and rice, and its high content of many essential nutrients makes it an attractive ingredient for incorporation into healthy foods [7]. Millet grains have been successfully used to produce adult foods, beverages and weaning foods, such as porridge, bread (fermented and unfermented) and snacks, in African and Asian areas, where they provide the main component of traditional meals [7,8].
Recently, millet has been found to be nutritionally superior compared to other traditional food grains due to the higher proportions of fibre, polyphenols and antioxidants [8]. This has drawn more attention to millet as a dietary option for helping manage diabetes by reducing blood glucose levels [9], which is of clinical importance for individuals with type-2 diabetes. Several studies have addressed the beneficial effects of millet on the risk markers for type-2 diabetes [10-12]. However, the results of randomized trials investigating the effects of millet on the GR (Glycaemic response) have been inconsistent, with some using short intervention periods or small sample sizes that could reduce the quality of the results. Therefore, this systematic review aims to evaluate the literature on intervention studies investigating the effects of consuming different types and forms of millet on markers of type-2 diabetes and highlight the need for future adequately powered trials in this important area of research.
Methods
Data extraction
Search engines, including Scopus, Web of Science, Academic Research Complete, PubMed and CAB abstract (Centre for Agriculture and Biosciences International), were used to search for studies in English, between 1990 and 2017, involving healthy, prediabetic and type-2 diabetic participants. The search terms used were: ‘Millet AND healthy’ or ‘pre-diabetic’ or ‘type-2 diabetes and fasting blood glucose’ or ‘glycaemic’ or ‘glycaemic response’ or ‘insulin response’ or ‘glucose tolerance’ or ‘insulin sensitivity’. We followed standard (PRISMA) criteria for reporting literature in this systematic review. Data extraction was conducted using a standardized table for all studies and all data was extracted for author, year, country, study design, intervention meals and control used, millets types and forms used, and individual’s characteristics (e.g. gender, age, BMI, height, weight, health condition).
Study selection
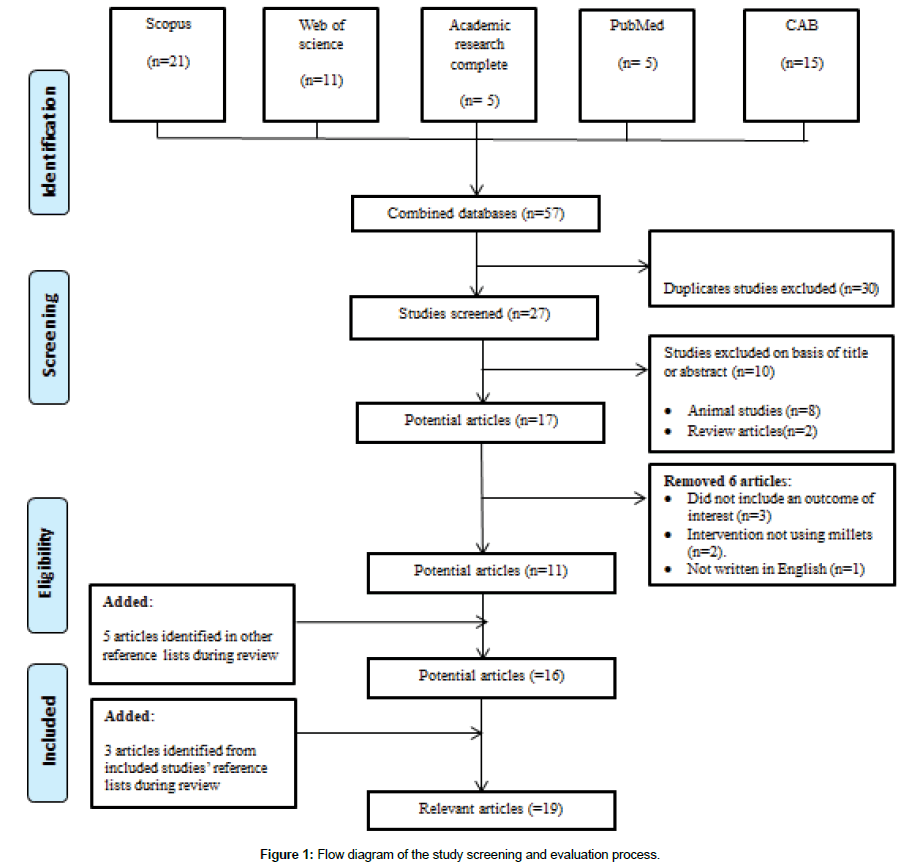
Data were extracted by one reviewer, as shown in the flow diagram for article selection (Figure 1) and all selected studies were confirmed by a second reviewer. The reference lists of all included studies were also searched to identify additional studies of interest. Studies were excluded if their titles or abstracts did not mention millet (any type or form), human participants (healthy and/or pre-diabetics and/or type-2 diabetes) or outcome (fasting blood glucose or glycaemic or glycaemic response or insulin response or glucose tolerance or insulin sensitivity). A total of 57 abstracts were included for review; from these, 30 were excluded on the basis of being duplicate studies, eight were animal studies and two were review papers. Three studies were not relevant (lacking the outcome of interest), two did not include millet as an intervention food and one was not written in English. Three more studies were identified from the reference lists of the included studies and, from these; five more studies were identified from in the reference list. In total, 19 studies met the criteria for inclusion in this review.
Quality assessment
The methodological quality of the 19 selected studies was independently evaluated by two reviewers using the Consolidated Standards of Reporting Trials (CONSORT) 2010 checklist for intervention studies [13,14]. Studies were assigned a quality rating of positive, negative or neutral, based on a set of quality questions, including intervention details, outcome measures, subject criteria and statistical analysis using the checklist for primary research from the Academy of Nutrition and Dietetics [15,16].
Results
Characteristics of included studies
A total of 19 studies were included in this review (Table 1). All studies examined an adult population, totalling 130 healthy adults (71 female and 59 male) and 482 type-2 diabetes adults (174 female and 308 male) with a mean age of 41.4 ± 12.4 years. The mean Body Mass Index (BMI) of participants in 12 studies was 24.4 ± 2.7kg/m2, the mean weight of participants in six studies was 59.3 ± 5.5 kg and the mean height of participants in one study was 162.3 ± 8.6 cm. The remaining included studies did not provide BMI, weight or height details.
| Reference | Subject characteristics | Study design/length | Millet types and forms | Intervention | Study outcomes | Quality rating |
|---|---|---|---|---|---|---|
| Abdelgadir M et al. [17] | 10 type 2 diabetic adults (4 females), 50.2 ± 5.3 years, BMI 27.5 ± 4.0 kg/m2 | Crossover study Study length: 6 days |
Proso millet | Each participant consumed 60 g of available carbohydrate id different occasions: 1: wheat gorasa (pancakes) 2: sorghum kisra (flat bread) 3: sorghum acida (porridge) 4: millet kisra 5: millet acida 6: maize acida *Control (NA) |
The AUCs of the meals showed that millet acida (porridge) followed by wheat gorasa (pancakes) displayed significantly ↓ post-prandial glucose and insulin responses, whereas maize acida induced a higher post-prandial glucose and insulin response | Positive |
| Arora S and Srivastava S [27] | 10 healthy adults (10 female), 23.5 ± 4.95 years, BMI 21.74 ± 3.08kg/m2 | Not known Study length: 6 days |
Finger millet Barnyard millet |
Each participant consumed 50 g ofavailable carbohydrate in different occasions: 1: Khichdi (millet, whole green gram and fenugreek seeds) 2: Laddu (millet, roasted soybean, malted fenugreek seeds, and amaranth) 3: Baati (fenugreek seed and roasted Bengal gram flour) *Control (Standard glucose solution (50 g)) |
Consumption of low GI millets based products (finger and barnyard millet) resulted in significantly ↓ GR (AUC) auc for different food products ranged from 1675.23 mg min/100 ml (finger millet based khichdi)to 2377.80 mg min/100 ml (barnyard millet-based laddu) | Positive |
| Ayuo PO andEttyang GA [18] | 15 type 2 diabetes adults, (6 female), 51 ± 3.9 years, BMI 24.2 ± 1.2 kg/m2 | Not known Study length: 2 months |
Not known | Each participant consumed 50 gofavailable carbohydrate in different occasions, 4 to 8 test meals: 1: Brown bread, 2: White rice (boiled in water+salt) 3: English potatoes (boiled in water+salt) 4: Maize meal (porridge) 5: Millet (porridge) 6: Cassava (boiled in water+salt) *Control (white bread) |
The mean blood sugars at 0,60 and 120 minutes were comparable for each food, and the peak rise occurred at 60 minutes. The highest rise (4.0 mmol/I) was seen with millet porridge | Neutral |
| Itagi S et al. [9] | Group 1:15 diabetic adults (5 female) and 6 diabetic adults (4 female) as control 50.78 ± 51 years, weight 69.40 ± 74.83 kgs, BMI 27.79 ± 29.14 kg/m2 Group 2:15 healthy adults (5 female) and 6 healthy adults (2 female) as control, 43.17 ± 43.67 years, weight 64.33 ± 66.00 kgs, BMI 24.07 ± 26.10 kg/m2 |
Not known Study length: 4 weeks |
Foxtail millet | Each participant consumed 87 g of diabetic mix per day in breakfast/lunch and dinner (50 g of available carbohydrate). Diabetic meal mix made with 80%foxtail millet and along with with 10% both wheat semolina, black gram dal and selected spices *Control(Healthy adult group) |
Consumption of diabetic mix foxtail millet-based resulted in ↓ fasting plasma glucose (up to 16-19%) after 4 weeks | Neutral |
| Jayasinghe MA et al. [20] | 11 healthy adults (6 female), 25 ± 7.07 years, BMI 21 ± 3.54kg/m2 | Crossover study Study length: 3 days | Finger millet/A bulk finger millet (halfwas milled using a rubber roller and mill, another half by a domestic stone grinder) | Each participant consumed 50 g of available carbohydrate in different occasions: Roti and Pittu occasions made with industrially milled finger millet flour or stone-ground flour. *Control (Standard glucose solution) | Foods prepared with finger millet (kurakkan) flour with a larger particle size distribution resulted in a ↓ GR |
Neutral |
| Lakshmikumri P and Sumathi S [30] | 6 type 2 diabetes adults (male) 47.5 ± 10.61years, weight 57 ± 3.54 kg |
Not knownStudy length: 7 days | Finger millet (Germinated) | Each participant consumed 75 g of available carbohydrate: Dosa and roti made with finger millet compared with control breakfast wheat roti and rice dosa (breakfast meet one-third of daily calorie requirement) *Control (wheat roti and rice dosa) |
Consumption of finger millet-based diets resulted in significantly ↓ plasma glucose levels, mean peak rise, and area under curve | Neutral |
| Nambiar V and Patwardhan T [25] | 6 healthy female, 20.5 ± 3.54 years, 23.0 ± 24.9 kg/m2 | Not knownStudy length: 9 days | Pearl millet | Each participant consumed 6 test meals /50 gof available carbohydrate in different occasions each meal served with curd (dairy product/50 g of available carbohydrate) 1: Pearl millet bhakri 2: Jowar bhakri 3: Cheela 4: Khichadi 5: Thalipeeth 6: Wheat roti *Control (Standard glucose solution (50 g)) |
Consumption of pearl millet-based meals resulted in ↓ GR (IAUC) | Neutral |
| Narayanan J et al. [12] | 105 type 2 diabetes adults (36 female), 49.26 ± 9.903 years, weight 72.157 ± 10.417, height 162.295 ± 8.636,BMI 27.436 ± 3.7396kg/m2 | Not knownStudy length: 2 days | Foxtail millet | All participants are divided into two groups/each participant consumed 50 gof available carbohydrate in different occasions of: 1: Millet based dosa 2: Rice based dosa *Control (White bread) |
Consumption of millet-based dosa resulted in significantly ↓ in the postprandial glucose level | Neutral |
| Pathak P et al. [23] | 5 healthy adults (female) and 5 types 2diabetes adults (male), 46 ± 33.94 years, BMI 25.5 ± 4.24 kg/m2 | Not knownStudy length: 4 days | Foxtail millet Barnyard millet |
Each participant consumed 50 g of available carbohydrate in different occasions of: Laddu made with amaranth, foxtail millet, roasted legumes, a paste of fenugreek seeds and jaggery syrup. Uppuma made with foxtail, barnyard millet, legumes, fenugreek seeds and defatted coconut powder each Dhokla made with foxtail, barnyard millet, legumes, and fenugreek seeds. *Control (NA) |
Consumption of foxtail-millet-based meals resulted in a ↓ GR |
Neutral |
| Ren X et al. [19] | 10 healthy adults (7 female), (mean) 26.0 years, (mean) BMI 20.8 kg/m2 | Not known Study length: 6 days |
Foxtail millet (flour) | Each participant consumed 50 g of available carbohydrate in different occasionsof Steamed bread, pancake or porridge made with foxtail millet flour *Control (Standard glucose solution (50 g)) | Consumption of foxtail-millet-based meals resulted in a ↓ GR |
Positive |
| Shobana et al. [24] | 8 healthy adults (3 female), 39 ± 19.80 years | Not knownStudy length: 5 days | Finger millet | Each participant consumed 50 gof available carbohydrate in different occasions: Porridge made with wheat or millet or rice *Control (White bread) |
Consumption of finger millet-based and wheat meals resulted in a ↓ GR |
Negative |
| Shukla K and Srivastava S [29] |
10 healthy female adults, 25.5 ± 2.12 years | Not known Study length: 2 days | Finger millet | Each participant consumed 50 gof available carbohydrate in different occasions: 1: Noodles made with finger millet flour 2: Noodles made refined wheat flour *Control (Refined wheat flour noodles) |
Consumption of low GI finger millet flour incorporated noodles improved blood glucose control | Positive |
| Shukla, Ket al. [22] | 18 healthy adults, 14 type 2diabetes adults 49.25 years, weight 55.625 ± 14.286 BMI 24.575 ± kg/m2 | Not known Study length: 2 days | Pearl millet (bajra) | Each participant consumed 50 gof available carbohydrate in different occasions: 1: Maize (chapattis) 2: Bajra (chapattis) 3: Barley (chapattis) *Control (White bread (50 g of available carbohydrate) |
GR to pearl millet was significant ↓ than that to white bread in healthy subjects, but the two responses were indistinguishable in T2D subjects. The IR to pearl millet and white break were not significantly different in either group of subjects | Neutral |
| ThakkarR and Kapoor R[28] | 42 type 2diabetes adults, 42.5 ± 3.54years, weight 50 to 58 kg | Not knownStudy length: 1 day | Finger millet | All participants were randomly assigned to 7 groups (6 test groups and 1 control group). Each group consists of 6 participants. Each test meal product provided of 50 g of available carbohydrate: 1: Finger millet (roti, idli, upma) 2: Rice (roti, idli, upma) *Control (Healthy adults group) |
Consumption of low GI finger millet based meals resulted in significantly ↓ GR | Neutral |
| Thathola A et al. [32] | 30 type 2 diabeticsadults(14 female), 57 ± 29.70 years, BMI 24.9 ± 10.47kg/m2 | 2 experiments: 1/Case control clinical trial. Study length: 30 days 2/Crossover study (4 weeks), this trail was an extension of the case-control clinical trial. Study length: 30 days |
Foxtail millet (flour) | Each participant consumed 100 g of biscuit and burfi made with foxtail millet *Control (Type 2 diabetes adults group) | Consumption of low GI biscuits or burfi made with foxtail millet resulted in significantly ↓ serum glucose by 23% from the baseline value | Neutral |
| Ugare R et al. [21] | 9 diabetic adults, 6 healthy adults (3 female), 37 ± 40years | Not known Study length: 28 days |
Barnyard millet | Each participant consumed 73 g of test meals/50 g of available carbohydrate in breakfast/lunch or dinner: Upma (dehulled and roasted barnyard millet) *Control (Standard glucose solution (50 g)) |
Consumption of barnyard millet based meals resulted in significantly ↓GR (139.2 to 131.1 mg/dl) | Positive |
| Urooj A et al. [31] | 7 type 2diabetes adults (3 female) , 27 ± 60 years, BMI 24.5 ± 3.32 kg/m2 7 healthy adults (4 female), 22 ± 45 years, BMI 22.3 ± 2.0 kg/m2 |
Not known Study length: 4 days | Finger millet (ragi) | Each participant consumed4 test meals/50g of available carbohydratein different occasions: 1: Finger millet roti 2: Rice roti 3: Finger millet dumpling 4: Jowar dumpling *Control (Standard glucose solution (50 g)) |
Consumption of finger millet based meals resulted in significantly ↓ GR (IAUC) | Positive |
| Thilakavathy S and Muthuselvi S [26] | 200 type 2 diabetes adults, (100 female), 50 ± 14.14 years | Not known Study length: 2 days | Pearl millet (bajra) Kodo millet (varagu/paspalum scrobiculatum) Foxtail millet(Thenai/Setaria italica) |
Each participant consumed test meals on different occasions: 1: Chappati made with whole wheat flour 2: 100 g white bread 3: 75 g of chappati made with millet 4: 75 gchappati made with millet and 30 fenugreek leaves *Control (50 g available carbs of white bread) |
Consumption of millet based meals resulted in ↓ GR | Neutral |
| TorangattiG and Rama K[33] | 18 type 2 diabetes adults (2 females), 54.8 ± 3.25years, weight 65.3 ± 1.70 18 healthy adults(10 female) 53.2 ± 4.10years, weight 45.45 ± 14.78 |
Not known Study length: 2 days | Pearl millet (bajra) Finger millet (ragi) Foxtail millet (Navani/Setaria italica) |
Each participant consumed 50 g of available carbohydrate: the selected diabetic subjects were then randomly divided into six groups consisting of three types 2 diabetics and three normal subjects. Test meals: Group 1: Jowar (Sorghum) roti and green gram Group 2: Riceand red gram dhalcurry Group 3: Chapatiand cabbagebhaji Group 4: Ragi balls and red gram dhal with amaranthuscurry Group 5: Navanirice and curds with milk Group 6: Bajraroti and brinjal bhaji *Control (Standard glucose solution (50 g)) |
Consumption of millets based meals (foxtail. Finger and pearl millet) resulted ↓ in GR | Neutral |
Table 1: Characteristics of the 19 studies included in this review.
The majority of trials (n=15) were carried out on participants in India, with one study based in Sudan [17], one in Kenya [18], one in China [19] and one in Sri Lanka [20]; none were based in the UK. The methodologies of the studies were similar to some extent, in that a baseline period was generally followed by participants before being instructed to consume a millet-based test product or glucose (control). Five of the studies collected venous blood from volunteers [9,19,21,22]; ten used a finger-prick blood draw [12,18,20,23-29]; and four studies did not stipulate on how blood was collected. In the studies that used the finger prick draw (capillary blood), blood samples were taken at the baseline and every 15 and 30 min for 2 to 3h. From those studies collecting venous blood, three [19,22] took blood every 15, 30 or 60 min, while others conducted long term feeding and took blood before and after the intervention periods [9,21] (4 weeks and 28 days, respectively). In the studies that had no defined blood collection methods, three [17,30,31] had blood samples taken every 30 or 60 min and only one study [32] had blood taken at the baseline, after a month and after two months.
Study quality and outcomes
All 19 studies were rated for quality using the checklist for primary research from the Academy of Nutrition and Dietetics; six studies received a positive rating [17,19,21,27,29,31], 12 studies were recorded as neutral [9,12,18,20,22,23,25,26,28,30,32] and only one study had a negative rating [24].
All studies investigated the impact of millet consumption on blood glucose levels as the as primary or secondary outcomes. Postprandial IR (Insulinaemic response) was also measured in three of the studies [17,19,22]. 12 of the studies measured the GI of meals prepared from millet [12,20,21,23-27,29,31,32], three of the studies measured the sensory characteristics of test meals [23,27,29] and the rest reported in vitro and in vivo starch digestion, protein and lipid profiles, glycosylated haemoglobin, lipemic response, serum cholesterol and glycaemic load as the outcomes [9,19,21,24,25,32].
Millet as intervention
The most common types of millet were used in the studies (finger, foxtail, pearl, proso, Kodo and barnyard millet). Eight studies used finger millet (six studies used finger millet alone and two studies used finger millet as a mixture with another millet type) [20,24,28-31], two studies used finger millet mixed with pearl and foxtail millet or barnyard millet [27] and only one study used proso millet [17]. Five used foxtail millet [9,12,19,23,32], three used pearl millet [22,25,26], one used barnyard millet [21] and one study used barnyard millet mixed with foxtail millet [23]. One study used pearl millet, kodo millet and foxtail millet [26] and one did not mention the type of millet used [18].
The majority of studies added millet to traditional meals, either alone or mixed with other grains, seeds or other ingredients. Common Indian dishes were prepared from these millets: roti , pittu, dosa, dhokla, upma, laddu, dal, mudde, cheela, bhakri, khichdi, thalipeeth, chapati, bati and idli [9,12,17,18,20-23,25-28,30,31]. Several studies prepared meals in the form of bread, pancake, porridge, biscuit or noodles [19,24,29,32].
Fasting and post-prandial blood glucose
All 19 studies in this review assessed the effects of different millet types and forms on the GR. Of these, eight used finger millet; one study used 50 g of available carbohydrates (from finger-millet flour) as an intervention in two different meals (roti and pittu), stoneground or industrially prepared. Meals prepared with finger-millet flour that was stoneground displayed a lower GR when compared to rubber rolling (industrial method). The GR curves indicated a lower and delayed peak (after 15 min) in individuals’ samples after eating both pittu and roti made with stoneground flour. However, the peak glucose concentrations in roti samples were relatively lower than in pittu samples, even when the same milling method was used [20]. This finding was corroborated by a second study, where the GR to finger-millet dosa was compared with finger-millet roti (both whole and germinated); finger-millet roti samples were found to have a lower GR than finger-millet dosa [30]. Other studies also revealed a lower GR following consumption of finger-millet-based roti in comparison to dumplings, idli or upma made from finger millet [28,31]. Four studies found that blood glucose levels after ingestion of millet-based meals peaked at 30 min [24,29] and then fell.
Seven studies showed reductions in the GR after consumption of foxtail-millet-based meals, including steamed bread, pancakes, porridge, dosa with foxtail-millet biscuits, burfi made with foxtail millet and foxtail millet rice with curds and milk [9,12,19,23,26,32].
Four studies [22,25,26] showed the same positive effect of consuming traditional Indian meals including pearl millet on lowering GR. These meals included roti, dhal, chapati [22,26] cheela and bhakri [25].
Three studies tested the GR after ingestion of barnyard millet and showed a significant reduction in fasting plasma glucose level [21]. One tested a mix of barnyard millet with finger millet, which elicited a peak rise in blood glucose 60min after the meal, before returning to baseline levels after 150 min [27]. Another study showed the same dampening effect of barnyard and foxtail millet (mixed) on the GR [23].
One study found that porridge made from proso millet significantly reduced postprandial GR-more so than wheat pancakes and maize porridge [17]. Another study reported that chappati made from kodo millet mixed with fenugreek leaves also reduced the GR [26].
As mentioned, one study did not clarify the type of millet added to meals [18]. The authors showed that the mean blood glucose increments differed between all the test foods, the highest reported for millet porridge (4.0 mmol/l) and the lowest for English potatoes boiled in water with salt (1.1 mmol/l).
Fasting and postprandial plasma insulin
Of all the studies in this review, only three assessed the IR after millet consumption. Plasma insulin levels changed significantly in response to millet porridge in one out of three studies (p=0.01). The AUC for plasma insulin showed a significant reduction in IR after the consumption of millet porridge, compared to sorghum porridge or flatbread, wheat pancakes, maize porridge or millet flatbread [17]. One of the studies showed that the peak insulin concentration in blood insulin reaction curves was slightly higher after millet porridge than after a standard glucose solution, compared to other millet meals in the study [19]. The third study in this group found that the IRs to pearl millet-based chapati and white bread were not significantly different between healthy and type-2 diabetic individuals [22].
Discussion
Fasting and post-prandial blood glucose
This systematic review has revealed a beneficial effect of consuming different types of millet on fasting and post-prandial blood glucose and the plasma IR in healthy and type-2 diabetic individuals. Finger millet is considered to be suitable food for people with type-2 diabetes and other non-communicable diseases [8]. Generally, in the review by Saleh et al. [8], all dishes made with finger millet were shown to be beneficial to reduce GR in both healthy individuals and those with type-2 diabetes. In fact, some studies that have tested the GI, might not in line with the recommendations by Brouns et al. [33] such as calculating the available CHO and the study sample size, however, considering the limited literature, these earlier studies are the only to compare to despite the limitations that they have slightly different methodology. Lower GI values were measured in meals made with stoneground millet flour, in comparison with those made through the use of industrially milled millets. This was due to the large particle size of the flour produced in stoneground flour [20]. Roti meals made from finger millet elicited a lower GR (alone or mixed with gum acacia (5 g)) compared with other meal types such as pittu, idli, upma, and dumplings in both healthy individuals and those with type-2 diabetes [28,30,31]. Many researchers have shown that meals with low and medium GI values can be protective for people with type-2 diabetes [34]. Moreover, some experiments have shown significantly lower peak levels of plasma glucose and a decreased AUC after consumption of whole-finger millet, compared with the same dishes made from germinated-finger millet [30]. Notably, however, removal of the seed coat from finger millet was shown to impede finger millet’s ability to lower the GR, as reported by Shobana et al. [24].
The variations in the GR of different products made prepared from finger millet may be due to differences in the extent of gelatinization, which significantly increases the GR [35]. The lower GR of wholefinger millet meals is also likely evidence of the physiological benefits of anti-nutritional factors, such as polyphenols, enzyme inhibitors, phytic acid and tannins [30]. Moreover, different processing methods, such as cooking, fermentation and the removal of seed covers may all alter the impact of finger millet on blood glucose.
Numerous studies have shown that millet consumption elicits a reduction in blood glucose due to its high content of unavailable carbohydrates. It has been reported that dehulled and dehulled and heated barnyard millet possess low GI values of 50% and 42%, respectively, making them highly beneficial for individuals with type- 2 diabetes. The average reductions in fasting plasma glucose in diabetic and non-diabetic individuals after barnyard millet intervention were 6% and 7%, respectively Ugare et al. [21], which may be owed to the higher dietary fibre and low carbohydrate content [36]. Although a high proportion of unavailable carbohydrates in millet may be the major contributing factor to the reduction in blood glucose, different cooking methods (pressure cooking, roasting and baking) used by Arora and Srivastava [27] were not shown to have any significant effect on the GI of certain traditional Indian meals (khichdi, luddu and baati).
Pearl millet (bajra) is one of the most popular millet types used in Indian dishes. It has been determined that the effect of bajra consumption on the GR depends on the cooking method used (shallow frying, roasting or steaming). It has also been shown that millet-based meals (pearl, foxtail, and finger) are associated with low GIs both in healthy individuals and those with type-2 diabetes, due to the high protein content [26]. Shukla et al. [22] showed that the GR of chapati made with bajra was significantly lower than that of white bread in healthy individuals. Moreover, the addition of 30g of fenugreek to millet chapati reduced the GI further, resulting in a lower GR than that observed through consumption of millet chapati without fenugreek. The reduction in the GR, in this case, may have been due to the nature and viscosity of fenugreek fibre in the leaves, which may have delayed GE [26].
It has been well established that there is a positive link between proso millet consumption in type-2 diabetic participants and a significant reduction in the glucose impact [17]. According to Colling [37], the method and time taken for the preparation of a meal may affect both the glycaemic and insulinemic responses. In particular, the degree of milling and duration of fermentation affected these outcomes. However, Ayuo and Ettyang [18] found that the highest peak rise in blood glucose level was recorded after consumption of millet porridge compared with root vegetables, probably due to the higher GIs of cereals (millet, maize, and rice) compared with those of root vegetables, such as cassava and English potatoes. This, along with the nature of the foods and the preparation methods, may explain the differences observed in the GRs between millet porridge and root vegetables; however, this study does not mention the type of millet used for porridge preparation, which reduces the reliability of the findings when comparing them with findings of studies that have tested other cereals and root vegetables, as each species of millet exerts different influences on the GRs and IRs.
An intervention study reported an association between foxtail millet intake and glucose reduction [23]. Consumption over four weeks of a ready-made mix that contained 80% foxtail millet and 10% each of wheat semolina and black gram dal with selected spices led to reductions of 16% to 19% in the plasma glucose levels of the type-2 diabetic intervention group. In addition, the carbohydrate tolerance of the intervention group improved, as shown by a reduction in the GR after four weeks. The cereal-pulse composite was concluded to be a healthy meal combination that helped to maintain normal concentrations of blood glucose. Notably, large portions of uppuma and dhokla (Indian dishes) made with foxtail millet did not induce sharp rises in blood glucose levels, indicating that they offered a healthy choice for type-2 diabetics [23].
Foxtail-millet dosa caused a significant reduction (p<0.001) in postprandial glucose values compared to individuals who consumed rice dosa [12]. This finding corroborates that by Thathola et al. [32], who reported that biscuits and burfi made from foxtail millet significantly reduced serum glucose levels from baseline by 23% after a long intervention period (30 days). According to Ren et al. [19], cooked foxtail millet elicited the lowest post-prandial blood glucose concentration, followed by millet pancakes (without extrusion flour), foxtail millet porridge, millet pancakes (75% millet flour and 25% extrusion flour), foxtail-millet steamed bread and standard glucose solution. It has been noted that the processing methods significantly affected the GR of foxtail millet. Ren et al. [19] found that cooked millet was found to be the best choice and preparation of millet for individuals with type-2 diabetes.
Fasting and post-prandial plasma insulin
It has been confirmed that there is a strong association between millet intake and reduced insulin response. A study by Abdelgadir et al. [17], indicated that the AUC for plasma insulin after consumption of proso-millet porridge showed a significantly reduced insulin response compared with findings after consumption of sorghum (flatbread and porridge), millet (flatbread), maize (porridge) and wheat (pancake) (p=0.0001 for all comparisons). The degree of milling and duration of fermentation was suggested to play an important role in the insulinemic response [37]. Also, a reduction of insulin levels was observed 2h after consumption of cooked foxtail millet and foxtail-millet pancakes (which comprised 75% millet flour and 25% extrusion flour) compared with consumption of a standard glucose solution. However, Shukla et al. [22], found no significant differences in the IRs after consumption of pearl millet compared with white bread in healthy and type-2 diabetic individuals, although the white bread produced a somewhat lower insulin response in type-2 diabetics 1h after intervention. In healthy individuals, pearl millet was shown to exhibit a low GI and a high insulinemic index; however, the opposite was true for those with type-2 diabetes, in whom the GI of pearl millet was high and the insulinemic index was low. The authors found that pearl millet evoked insulin secretion in healthy individuals, and this reduced the GR, whereas in type-2 diabetics there may have been an insufficient insulin reserve, leading to insufficient mobilization of insulin on ingestion of pearl millet.
Millet is a functional grain known for its significant health benefits, attributed in large part to its high content of polyphenols and antioxidants, as evidenced by substantial research regarding their effects on type-2 diabetes, among other fields [8]. The present systematic review of 19 studies has demonstrated a beneficial effect of different types and forms of millet on fasting and post-prandial blood glucose and plasma insulin levels in healthy adults and patients with type-2 diabetes. To our knowledge, this is the first systematic review to examine the effect of millet consumption on glucose and insulin sensitivity in healthy adults and those with type-2 diabetes. Overall, this review has shown that consumption of different types and forms of millet can lead to an improvement in glucose and insulin sensitivity compared with the levels of these markers after different control meals (e.g. glucose, sorghum, and wheat).
Limitations
The quality ratings of the 19 eligible studies, assigned using CONSORT and the checklist for primary research from the Academy of Nutrition and Dietetics, indicated that, despite strong criteria that limited the number of studies that could be included (n=19), only a few were rated positively (n=6), while 12 were rated neutral and only one study received a negative rating.
There were a few limitations to the systematic review in this work. First, the 19 studies were mostly reports not of randomized clinical trials but of primary pilot trials, which did not provide reliable causality inferences or achieve sufficient statistical power to detect a significant effect of millet consumption on postprandial blood glucose and plasma insulin responses. These shortcomings were compounded by the small sample sizes and short-duration interventions in some studies. One study, as previously mentioned, did not specify the millet type (e.g. finger, pearl) or the form (e.g. grain, flour or flakes) used, which impaired the quality of the study results. Some studies mixed millet with other grains or spices, which made it hard to determine whether the millet and its components or the other ingredients were responsible for the observed reductions in the GR in participants. It should also be noted that portion size of test meals, or the millet proportions (either added to a meal or as a replacement), were not sufficiently explained in some studies. Separate investigations across the various millet-grain foods produced from different crops may be useful to decrease heterogeneity and to obtain more robust scientific evidence of the impact of millets from specific sources on glycaemic and insulinemic responses. This is because each millet type has a different source, type, and colour, and has been shown to produce a different effect on blood glucose and insulin responses dependent on the polyphenol compound and starch content.
Conclusion
This systematic review has revealed a beneficial effect of consuming different types of millet on fasting and post-prandial blood glucose and the plasma IR in healthy and type-2 diabetic individuals. The effect of millet consumption on pre-diabetic trials with an adequate sample size should be investigated in the future. Also, it is worth exploring the potential benefits of different types of millet in managing type-2 diabetes through long-term feeding interventions.
Acknowledgment
The authors would like to thank Taibah University, KSA for funding the study and Oxford Brookes University, the UK for providing all support and resources to conduct the study.
Funding
This work was supported by Taibah University, KSA, Medina (grant number TAU211).
Conflict of Interests
The authors report no conflict of interests.
References
- Asif M (2014) The prevention and control the type-2 diabetes by changing lifestyle and dietary pattern. J Educ Health Promot3: 1.
- Diabetes UK-global diabetes community (2016) NHS diet advice for diabetes. Diabetes, UK 2016.
- American Diabetes Association (2016) Comprehensive, annual guide includes new and updated recommendations to safeguard the physical and psychological health of people with diabetes. American Diabetes Association 2016.
- Diabetes UK (2016) Number of people with diabetes reaches over 4 million. Diabetes, UK 2017.
- Willett W, Manson J, Liu S (2002) Glycemic index, glycemic load, and risk of type 2 diabetes. Am J Clin Nutr 76: 274S-80S.
- Bull C, Hazeltine B (2003) Field guide to appropriate technology. Elsevier, Amsterdam, Academic Press.
- Amadou I, Gounga ME, Le GW (2013) Millets: nutritional composition, some health benefits and processing-A review. Emir J Food Agric 1: 501-508.
- Saleh AS, Zhang Q, Chen J, Shen Q (2013) Millet grains: nutritional quality, processing, and potential health benefits. Compr Rev Food Sci Food Saf 12: 281-295.
- Itagi S, Naik R, Bharati P, Sharma P (2012) Readymade foxtail millet mix for diabetics. Int J Sci Nat 3: 47-50.
- Naoyuki N, Tubasa T, Kyung O, Daiki S, Yo M, et al. (2009) Dietary japanese millet protein ameliorates plasma levels of adiponectin, glucose, and lipids in type 2 diabetic mice. Biosci, Biotechnol, Biochem 73: 351-360.
- Choi YY, Osada K, Ito Y, Nagasawa T, Choi MR, et al. (2005) Effects of dietary protein of korean foxtail millet on plasma adiponectin, HDL-cholesterol, and insulin levels in genetically type 2 diabetic mice. Biosci, Biotechnol, Biochem 69: 31-37.
- Narayanan J, Sanjeevi V, Rohini U, Trueman P, Viswanathan V (2016) Postprandial glycaemic response of foxtail millet dosa in comparison to a rice dosa in patients with type 2 diabetes. Indian J Medical Res 144: 712-717
- Consort (2010) The CONSORT Statement. Consort 2017.
- Visser E, Gosens T, Den Oudsten BL, De Vries J (2017) The course, prediction, and treatment of acute and posttraumatic stress in trauma patients: A systematic review. J Trauma Acute Care Surg 82: 1158-1183.
- Academy of Nutrition and Dietetics (2016) Quality criteria checklist: Primary research. Academy of Nutrition and Dietetics 2016.
- Coe S, Ryan L (2016) Impact of polyphenol-rich sources on acute postprandial glycaemia: A systematic review. J Nutr Sci 5: 1-11.
- Abdelgadir M, Abbas M, Järvi A, Elbagir M, Eltom M, et al. (2005) Glycaemic and insulin responses of six traditional sudanese carbohydrateâ€Ârich meals in subjects with type 2 diabetes mellitus. Diabet Med 22: 213-217.
- Ayuo P, Ettyang GA (1996) Glycaemic responses after ingestion of some local foods by non-insulin dependent diabetic subjects. East Afr Med J 73: 782-785.
- Ren X, Chen J, Molla MM, Wang C, Diao X, et al. (2016) In vitro starch digestibility and in vivo glycemic response of foxtail millet and its products. Food Funct 7: 372-379.
- Jayasinghe MA, Ekanayake S, Nugegoda DB (2013) Effect of different milling methods on glycaemic response of foods made with finger millet (Eucenea coracana) flour. Ceylon Med J 58: 148-152.
- Ugare R, Chimmad B, Naik R, Bharati P, Itagi S (2014) Glycemic index and significance of barnyard millet (Echinochloa frumentacae) in type II diabetics. J Food Sci Technol 51: 392-395.
- Shukla K, Narain P, Puri P, Gupta A, Bijlani R, et al. (1991) Glycaemic response to maize, bajra and barley. Indian J Physiol Pharmacol 35: 249-254.
- Pathak P, Srivastava S, Grover S (2000) Development of food products based on millets, legumes and fenugreek seeds and their suitability in the diabetic diet. Int J Food Sci Nutr 51: 409-414.
- Shobana S, Usha Kumari SR, Malleshi NG, Ali SZ (2007) Glycemic response of rice, wheat and finger millet based diabetic food formulations in normoglycemic subjects. Int J Food Sci Nutr 58: 363-372.
- Nambiar VS, Patwardhan T (2015) Assessment of glycemic index (GI) and glycemic load (GL) for selected traditional millet-based Indian recipes. Int J Diabetes in Dev Ctries 35: 157-162.
- Thilakavathy S, Muthuselvi S (2010) Development and evaluation of millets incorporated chappathi on glycemic response in type II diabetics. Indian J Nutr Diet 47: 42-50.
- Arora S, Srivastava S (2002) Suitability of millet-based food products for diabetics. J Food Sci Technol 39: 423-426.
- Thakkar R, Kapoor R (2007) Enrichment of rice and finger millet based preparations with gum acacia and their effects on glycemic response in non-insulin dependent diabetic subjects. J Food Sci Technol 44: 183-185.
- Shukla K, Srivastava S (2014) Evaluation of finger millet incorporated noodles for nutritive value and glycemic index. J Food Sci Technol 51: 527-534.
- Kumari PL, Sumathi S (2002) Effect of consumption of finger millet on hyperglycemia in non-insulin dependent diabetes mellitus (NIDDM) subjects. Plant Foods Hum Nutr 57: 205-213.
- Urooj A, Rupashri K, Puttaraj S (2006) Glycaemic responses to finger millet based Indian preparations in non-insulin dependent diabetic and healthy subjects. J Food Sci Technol 43: 620-625.
- Thathola A, Srivastava S, Singh G (2010) Effect of foxtail millet (Setaria italica) supplementation on serum glucose, serum lipids and glycosylated hemoglobin in type 2 diabetics. Diabetol Croat 40: 23-28.
- Brouns F, Bjorck I, Frayn KN, Gibbs AL, Lang V, et al. (2005) Glycaemic index methodology. Nutr Res Rev 18: 145-171.
- Potter JG, Coffman KP, Reid RL, Krall JM, Albrink MJ (1981) Effect of test meals of varying dietary fiber content on plasma insulin and glucose response. Am J Clin Nutr 34: 328-334.
- Wolever TM, Jenkins DJ, Jenkins AL, Josse RG (1991) The glycemic index: Methodology and clinical implications. Am J Clin Nutr 54: 846-854.
- Veena B, Chimmad B, Naik R, Shantakumar G (2005) Physico-chemical and nutritional studies in barnyard millet. Karnataka J Agric Sci 18: 101-105.
- Collings P, Williams C, MacDonald I (1981) Effects of cooking on serum glucose and insulin responses to starch. Br Med J (Clin Res Ed) 282: 1032.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi