Case Report, J Food Nutr Disor Vol: 7 Issue: 1
Superior Mesenteric Artery Syndrome with: Gastric Emphysema, Gas in the Portal Vein and Pneumoperitoneum Due to Anorexia Nervosa
Klaudia Korecka1*, Grzegorz Kudela1, Magdalena Lucyga1, Małgorzata Janas-Kozik2, Ireneusz Jelonek2, Agnieszka Pastuszka3 and Tomasz Koszutski1
1Department of Pediatric Surgery, Medical University of Silesia, Upper Silesia Child Health Center, Katowice, Poland
2Department of Psychiatry and Psychotherapy of Developmental Age, Medical University of Silesia, John Paul II Pediatric Center, Sosnowiec, Poland
3Department of Descriptive and Topographic Anatomy, Medical University of Silesia School of Medicine with Division of Dentistry in Zabrze, Poland
*Corresponding Author : Klaudia Korecka
Department of Pediatric Surgery, The Upper Silesia Child Health Center, ul. Medyków 16, 40-572 Katowice, Poland
Tel: +48-792-717-551,+48-32-207-17-50
Fax: +48-32-207-15-46
E-mail: kkorecka@poczta.onet.pl
Received: December 01, 2017 Accepted: January 02, 2018 Published: January 05, 2018
Citation: Korecka K, Kudela G, Lucyga M, Kozik MJ, Jelonek I, et al. (2018) Superior Mesenteric Artery Syndrome with: Gastric Emphysema, Gas in the Portal Vein and Pneumoperitoneum Due to Anorexia Nervosa. J Food Nutr Disor 7:1. doi: 10.4172/2324-9323.1000240
Abstract
12- year- old patient suffering from anorexia nervosa feeding implementation after a period of prolonged fasting cause a refeeding syndrome, which manifests itself as acute electrolytes deficiency resulting in dysfunction of the entire organism, including bowel transit time disorders. Gastric antral electrical dysarhythmias which develop in this mechanism promote dilatation of the stomach. Concomitant compression and obstruction of the third portion of the duodenum due to superior mesenteric artery syndrome (Superior Mesenteric Artery syndrome) results in stomach dilatation, which can lead to gastric emphysema and pneumoperitoneum. The pathomechanisms described above create a vicious circle mechanism general symptom in the young patient.Gastric emphysema with gas in the portal vein and Superior mesenteric artery syndrome are potentially threatening complications of chronic malnutrition and anorexia. Intensive conservative treatment with a control CT scan after 24 to 48 hours may be useful when making the decision to withdraw from surgical procedure. Releasing the duodenum from the compression gives the opportunity to eliminate one element of the vicous circle mechanism as far as the treatment of eating disorders is concerned.
Keywords: Superior mesenteric artery syndrome; Gastric emphysema; Portal vein gas; Anorexia nervosa
Introduction
Medical symptoms associated with chronic malnutrition have long been observed. These include: superior mesenteric artery syndrome (Superior mesenteric artery syndrome), pneumatosis intestinalis (PI) as well as the refeeding syndrome symptoms. Superior mesenteric artery syndrome was first described by Rokitansky in 1861 with a frequency estimated at 0.3% of the population [1,2,3]. Symptoms of pnemuatosis intestinalis have been reported by DuVeroni in 1754. In terms of frequency of PI occurrence in the gastrointestinal tract, the stomach location is the most uncommon one. Until now 18 cases in 15 years with stomach localization have been described [4].
Case Report
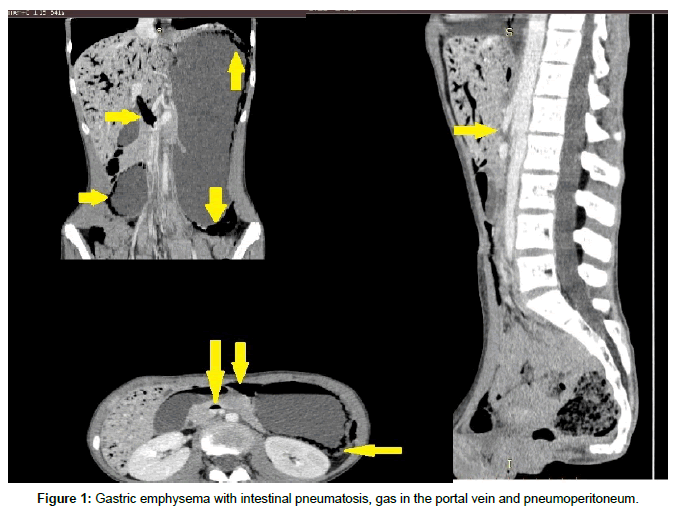
A 12-year-old patient suffering from anorexia (family complete, brother suffering autism) had lost 15 kg of body weight (from 43 kg to 28 kg) with a BMI of 12.1 last four months period was admitted to the Pediatric Surgery Department. Before the child was treated in the Pediatric and Childrens’ Psychiatric Departments where in addition to pharmacological treatment an attempt to feed by a nasogastric tube was essayed. During the second of the day naso-gastric tube nutrition supply, symptoms such as vomiting, abdominal pain and deterioration appeared. Due to presented clinical symptoms diagnostic imaging was performed (an X-ray of the abdominal cavity, as well as a CT scan of the abdomen). The diagnostic imaging depicted gastric emphysema with intestinal pneumatosis, gas in the portal vein and pneumoperitoneum (Figure 1).
Due to the pneumoperitoneum, suspecting a gastrointestinal tract perforation, the patient was qualified for a diagnostic laparoscopy. Gas in the omentum and a non-inflammated Meckel’s diverticulum were observed intraoperatively whereas the external wall of the stomach presented no pathology. No evident area of perforation was observed. In view of an obstruction in the third part of the duodenum, the need to re-examine the posterior wall of the stomach, as well as the necessity to resect the Meckel’s diverticulum a decision to switch to laparotomy was made. During laparotomy the entire gastrointestinal tract was examined (including the anterior and posterior wall of the stomach), a wedge resection of the Meckel’s diverticulum was performed and the duodenum was released from the compression made by the superior mesenteric artery. There were no surgical complications during the postoperative period.
On 5th day after the surgery, a control ultrasound of the abdomen presented no pathology (the gastric wall was free from pneumatosis and no gas in the portal vein was observed). After the surgery, a broad spectrum antibiotic therapy and parenteral nutritional treatment were introducted. The electrolytes levels (including phosphorus level) were monitored and their deficiencies were balanced. The patient was discharged from the Pediatric Surgery Department on the 5th day after surgery with plans for further nutritional and psychiatric treatment.
Discussion
Superior mesenteric artery syndrome is described as an exogenous compression of the third portion of the duodenum by narrowing of the angle between the abdominal aorta and the overlying superior mesenteric artery (<25°C). This pathology is caused by involution of retroperitoneal and mesenteric fat which is physiologically present in this area. Compression and obstruction of the third portion of the duodenum results in stomach dilatation, which can further lead to gastric emphysema. Massive distension of the stomach causes hypoperfusion and ischemia with gas penetration into the gastric wall [4,5]. Feeding implementation after a period of prolonged fasting cause a refeeding syndrome as well, which manifests itself as acute electrolytes deficiency resulting in disfunction of the entire organism, including bowel transit time disorders [1,6]. Gastric antral electrical dysarhythmias which develop in this mechanism promote dilatation of the stomach and lead to further consequences described previously.
Treatment of superior mesenteric artery syndrome may be conservative or surgical. The latter is connected with releasing the third portion of the duodenum by performing a duodenojejunal bypass anastomosis above the superior mesenteric artery (also known as Strong’s procedure) [2,5,7]. Norris proves that 73% patients suffering from anorexia-related superior mesenteric artery syndrome can be successfully treated conservatively [8]. In this presented case, the decision of surgical intervention was made not strictly because of the superior mesenteric artery syndrome but due to the presence of concomitant symptoms such as pneumoperitoneum and the co-occurence of PVG with PI which could cause possible further serious consequences. Sooby quotes a 44% mortality rate due to the presence of PI and a 2% mortality rate for idiopathic PVG. However, the co-occurrence of PVG with PI increases the mortality rate up to 75-90% [9]. Additionally, the presence of free gas in the peritoneal cavity, which suggested a gastrointestinal tract perforation, determined the decision of surgical intervention (as statistical data presents an 80% mortality rate in patients with stomach dilatation and additional perforation in patients suffering from anorexia [8]. Mularski quotes that the rupture of the intramural emphysematous bulla (which creates PI) is not synonymous with a full thickness gastrointestinal wall perofration, as the majority of emphysematous bullas are located in the submucosal or subserosal layers of the bowel and they do not communicate with its lumen [9,10].
When analyzing the presented case report and the literature data, intensive conservative treatment (as well as monitoring the patient with a control CT scan of the abdominal cavity after 24-48 hour) provides a tempting alternative to urgent surgical treatment. The presented patient is one of the youngest patients suffering from anorexia (12 years old) with such severe general symptoms. Norris quotes 12 patients under 18 years of age, in whom, in course of anorexia, gastric complications have been observed [8]. However none of the patients have presented gastric PI, nor gas in the portal vein or pneumoperitoneum.
Conclusion
• Gastric emphysema with gas in the portal vein and superior mesenteric artery syndrome are potentially threatening complications of anorexia and chronic malnutrition.
• Despite distressful radilogical signs, an intensive conservative treatment with a control CT scan after 24-48 hours may be useful when making the decision to withdraw from surgical procedure.
• Releasing the duodenum from the compression gives the opportunity to eliminate one element of the “vicous circle” mechanism as far as the treatment of eating disorders is concerned.
Conflict of Interest
The authors have no disclosures of funding or financial support to disclose with regards to the preparation of this manuscript. Additional informed consent was obtained from participant for whom identifying information is included in this article.
References
- Moscolo M, Dee E, Townsend R, Brinton JT, Mehler PS (2015) Severe gastric dilatation due to superior mesenteric artery syndrome in anorexia nervosa. Int J Eat Disord. 48: 532-544.
- Zaraket V, Deeb L (2015) Wilkie's syndrome or superior mesenteric artery syndrome: fact or fantasy? Case Rep Gastroenterol 9: 194-199.
- Welsch T, Buchler MW, Kienle P (2007) Recalling superior mesenteric artery syndrome. Dig Surg 24: 149-156.
- Lopez-Medina G, Castillo Diaz de Leon R, Heredia-Salazar AC, Hernandez-Salcedo DR (2014) Gastric emphysema a spectrum of pneumatosis intestinalis: a case report and literature review. Case Rep Gastrointest Med.
- Merrett ND, Wilson RB, Cosman P, Biankin AV (2009) Superior mesenteric artery syndrome: diagnosis and treatment strategies. J Gastrointest Surg 13: 287-292.
- Adson DE, Mitchell JE, Trenkner SW (1997) The superior mesenteric artery syndrome and acute gastric dilatation in eating disorders: A report of two cases and a review of the literature. Int J Eat Disord 21: 103-114.
- Mandarry M, Zhao L, Zhang C, Wei Z (2010) A comprehensive review of superior mesenteric artery syndrome. Eur Surg 42: 229-236.
- Norris ML, Harrison ME, Isserlin L, Robinson A, Feder S, et al. (2016) Gastrointestinal complications associated with anorexia nervosa: A systematic review. Int J Eat Disord 49: 216-237.
- Sooby P, Harshen R, Joarder R (2015) An unusual triad of pneumatosis intestinalis, portal venous gas and pneumoperitoneum in an asymptomatic patient. J Surg Case Rep.
- Mularski RA, Sippel JM, Osborne ML (2000) Pneumoperitoneum: a review of nonsurgical causes. Crit Care Med 28: 2638-2644.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi